Acne Agminata: Complete Guide to Diagnosis & Treatment
Uncommon facial skin disorder with red-brown papules, granulomatous inflammation, and potential for scarring if untreated.
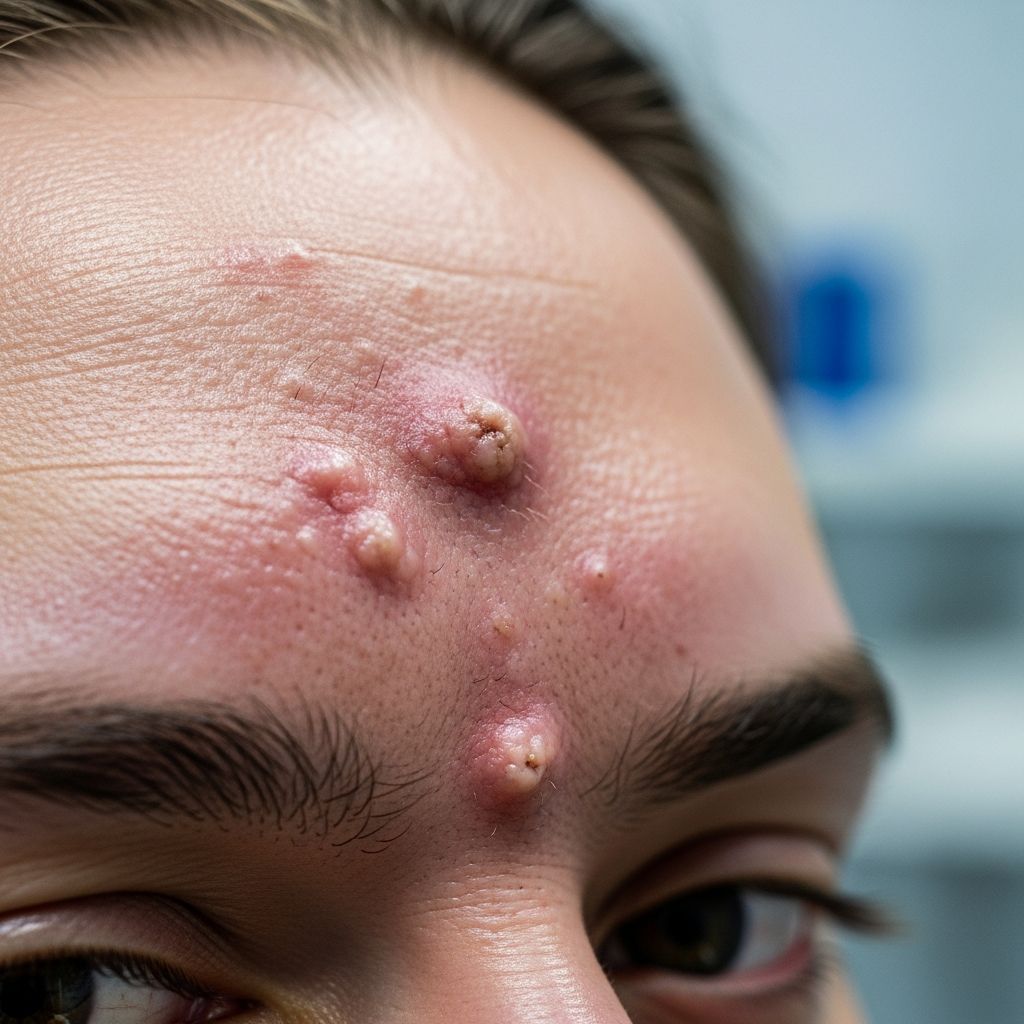
Acne Agminata
Acne agminata, also known as lupus miliaris disseminatus faciei (LMDF), is a rare inflammatory dermatosis characterized by clusters of small, red-brown papules primarily on the central face. These lesions often heal with atrophic scarring, making early recognition and intervention crucial.
What is acne agminata?
Acne agminata manifests as multiple monomorphic, dome-shaped papules, typically 1-2 mm in diameter, with a reddish-brown hue and yellowish centers due to caseation. The condition predominantly affects the malar cheeks, eyelids, forehead, glabella, and chin, though it can extend to perioral areas, neck, or rarely armpits. First described by Tilbury Fox in 1878 as disseminated folliculitis, it earned the name ‘acne agminata’ from Ernest Gaucher in 1889 due to its acne-like grouped (agminate) appearance.
Histopathologically, it shows perifollicular epithelioid granulomas with central caseous necrosis, lacking acid-fast bacilli or other infectious agents, distinguishing it from true granulomatous infections. The disease evolves in crops over 2-3 years, starting acutely and stabilizing before spontaneous regression, but residual pitted scars are common in 70-90% of cases without treatment.
Who gets acne agminata?
Acne agminata primarily affects young adults aged 20-40 years, with a slight female predominance (2:1 ratio), though cases occur across all ages. No strong ethnic predisposition exists, but reports are more common in Asian and Caucasian populations. Risk factors remain unidentified, as it is non-contagious and unrelated to hygiene or diet. Genetic factors are not established, and it does not cluster in families.
What causes acne agminata?
The etiology of acne agminata is unknown, with no infectious agent consistently identified despite granulomatous histology suggesting prior folliculitis. Hypotheses include:
- Abnormal immune response to follicular contents like keratin, sebum, or commensal bacteria, leading to granuloma formation.
- Possible hypersensitivity to unidentified antigens, akin to idiopathic granulomatous reactions.
- Exclusion of Mycobacterium tuberculosis via negative Ziehl-Neelsen stains and cultures.
Triggers like topical steroids, sunlight, alcohol, or spicy foods may exacerbate lesions, but causation is unproven. Hormonal influences are speculative, without acne vulgaris-like comedonal pathology.
What are the clinical features of acne agminata?
Lesions appear as symmetrical, asymptomatic or mildly pruritic red-brown papules in malar and periorbital distributions. Key features include:
- Monomorphic 1-4 mm dome-shaped papules with central dell or crust.
- Grouped in ‘agminate’ clusters, sparing nasolabial folds.
- Evolution: New crops every few weeks; older lesions flatten and scar.
- Rare systemic symptoms; occasional mild itch or tenderness.
Without intervention, the disease persists 12-36 months, resolving spontaneously but with disfiguring atrophic scars. Images typically show periorbital and cheek involvement with characteristic scarring.
How is acne agminata diagnosed?
Diagnosis is primarily clinical, supported by histopathology. Key diagnostic steps:
- Clinical exam: Monomorphic facial papules with granulomatous suspicion.
- Skin biopsy: Essential; reveals mid-dermal perifollicular granulomas with caseous necrosis, multinucleated giants, and lymphohistiocytic infiltrate. No organisms on special stains.
- Additional tests: If tuberculosis/sarcoidosis suspected: Quantiferon-TB Gold, chest X-ray, serum ACE, or PCR for mycobacteria. Negative in confirmed cases.
Diagnosis requires clinicopathologic correlation to exclude mimics.
What are the differential diagnoses for acne agminata?
| Condition | Key Distinguishing Features |
|---|---|
| Granulomatous rosacea | Telangiectasia, flushing, eye involvement; responds to tetracyclines |
| Nodulocystic acne | Polymorphic lesions (comedones, cysts); antibiotic-responsive |
| Perioral dermatitis | Periorificial; scale-crust; female predominance, steroid history |
| Histoid leprosy | Spindle cells, acid-fast bacilli on Fite stain |
| Sarcoidosis | Non-caseating granulomas; systemic involvement, high ACE |
| Tuberculosis (lupus vulgaris) | Irregular ‘apple-jelly’ nodules; positive TB tests |
| Syringomas | Flesh-colored, translucent; no inflammation |
Differentials emphasize biopsy necessity for granulomatous papules.
What is the treatment for acne agminata?
No standardized protocol exists; treatments aim to shorten duration and prevent scarring via early anti-inflammatory intervention. Untreated resolution occurs in 2-3 years with scarring.
First-line options:
- Oral tetracyclines (doxycycline 100mg daily): Variable success; anti-inflammatory effect.
- Dapsone 50-100mg daily: Excellent response in case series, especially combined with topicals.
- Systemic corticosteroids (prednisolone 0.5mg/kg): Rapid clearance without scars if early; taper over weeks.
Other therapies:
- Topical tacrolimus 0.1% ointment: Reduces inflammation; synergistic with dapsone.
- Isotretinoin: Mixed results; avoid if scarring predominant.
- Clofazimine 100mg daily: For refractory cases.
- Tranilast 150mg TID: Inhibits fibrosis; emerging option.
- Laser (1450nm diode, CO2 + peel): Adjunctive for scars.
Combination dapsone + tacrolimus yields high efficacy. Monitor for side effects: G6PD for dapsone, glucose for steroids. Early treatment halves disease duration and minimizes scars.
What is the outcome for acne agminata?
Spontaneous resolution in 1-3 years, but 70% develop atrophic ‘chicken-pox’ scars, worse centrally. Prompt therapy prevents disfigurement; post-inflammatory hyperpigmentation fades. Recurrence is rare post-resolution. Regular follow-up ensures clearance.
Self-care for acne agminata
- Gently cleanse with mild soap; avoid scrubbing.
- Apply warm compresses to soften crusts.
- Use non-comedogenic moisturizers; sunscreen daily.
- Avoid triggers: harsh cosmetics, alcohol, spicy foods.
- Do not squeeze papules to prevent worsening scars.
Prevention of acne agminata
Impossible due to unknown etiology; early dermatology consultation for facial granulomas prevents complications.
Frequently Asked Questions (FAQs)
Is acne agminata contagious?
No, it is non-infectious despite granulomas.
Does acne agminata scar permanently?
Yes, untreated cases scar in most; early treatment prevents this.
How long does acne agminata last?
2-3 years untreated; shorter with therapy.
Is acne agminata a form of acne vulgaris?
No, lacks comedones; granulomatous not comedonal.
What is the best treatment for acne agminata?
Dapsone ± topical tacrolimus or early oral steroids show best results.
References
- Lupus Miliaris Disseminatus Faciei: A Report of a Rare Case and Its … — PMC/NCBI. 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC11281938/
- Acne agminata – DermNet — DermNet NZ. 2023. https://dermnetnz.org/topics/acne-agminata
- Acne Agminata – DoveMed — DoveMed. 2024. https://www.dovemed.com/diseases-conditions/acne-agminata
- Oral prednisone in the treatment of acne agminata — British Journal of Dermatology/Oxford Academic. 1996-06-01. https://academic.oup.com/bjd/article-abstract/134/6/1098/6681972
- Lupus Miliaris Disseminatus Faciei — MD Searchlight. 2024. https://mdsearchlight.com/skin-problems-and-treatments/lupus-miliaris-disseminatus-faciei/
- Lupus miliaris disseminatus faciei — Wikipedia (references primary sources). 2024. https://en.wikipedia.org/wiki/Lupus_miliaris_disseminatus_faciei
Read full bio of Sneha Tete










