Acquired Elastotic Haemangioma Pathology
Detailed pathology of acquired elastotic haemangioma, a benign vascular lesion linked to chronic sun exposure in sun-damaged skin.
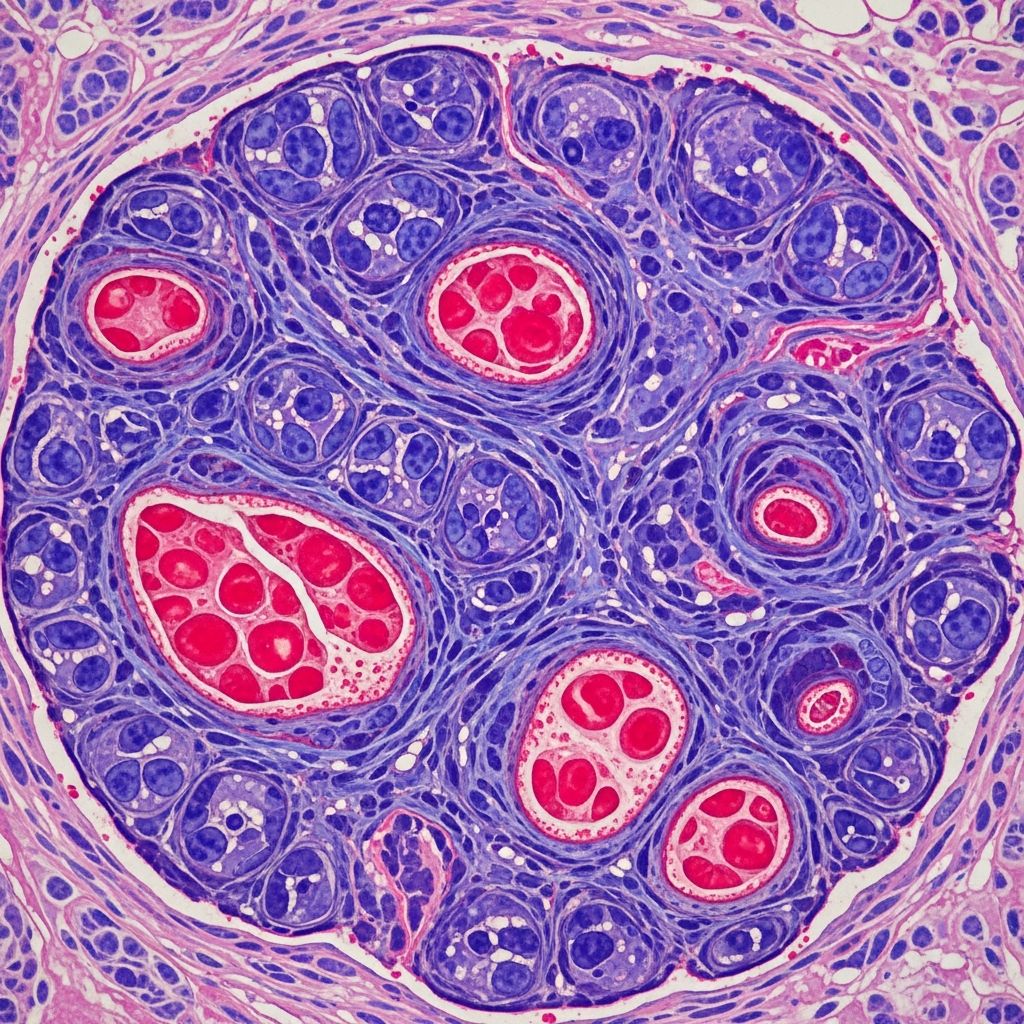
Acquired elastotic haemangioma is a benign endothelial proliferation typically presenting as a flat or raised erythematous plaque on sun-exposed skin of middle-aged to elderly individuals. It is strongly associated with chronic solar damage, characterized histologically by a band-like vascular proliferation in the superficial dermis amid prominent elastosis.
Introduction
Acquired elastotic haemangioma (AEH), first described by Requena et al. in 2002, represents a distinctive variant of cutaneous vascular proliferation. This lesion arises almost exclusively in actinically damaged skin, most commonly on the forearms, V-neck area, and other sun-exposed sites in fair-skinned adults over 50 years of age. Clinically, it manifests as a solitary, well-circumscribed, erythematous to violaceous plaque, often irregular in shape and measuring 0.5–8 cm in diameter. The lesion is usually asymptomatic, though occasional tenderness or cosmetic concern may prompt evaluation.
AEH predominantly affects middle-aged to elderly women (female-to-male ratio approximately 3:1), though male cases are reported. Its pathogenesis is linked to long-term ultraviolet (UV) exposure, which induces dermal solar elastosis—a hallmark degenerative change in the extracellular matrix. While initially considered a true hemangioma, recent studies suggest possible lymphatic differentiation based on variable D2-40 expression, though it remains classified as a benign capillary proliferation reactive to photodamage. Importantly, AEH follows an indolent course with no malignant potential; complete excision, if desired, yields no recurrences.
Histology
Microscopic examination reveals the pathognomonic features of AEH. Low-power view demonstrates a well-demarcated, band-like proliferation of dilated, thin-walled capillary-sized vessels confined to the upper dermis, oriented parallel to the dermoepidermal junction. A key diagnostic clue is the presence of a thin, uninvolved papillary dermis (Grenz zone) separating the vascular proliferation from the epidermis.
- Superficial dermis: Dense horizontal array of closely packed, capillary-sized vessels forming a superficial band-like pattern amid abundant solar elastosis.
- Solar elastosis: Prominent basophilic degeneration of elastic fibers surrounding and intermingling with the vascular channels—constitutes the most distinctive feature.
- Endothelium: Flat, bland hobnail or flattened endothelial cells without multilayering, nuclear atypia, hyperchromasia, or mitoses.
- Deep margin: Sharp, well-defined lower border of the vascular proliferation, typically not extending into mid or deep dermis.
- Epidermis: Usually atrophic or unremarkable; no epidermal involvement.
- Stroma: Minimal scant lymphocytic infiltrate possible; absence of fibrosis, red cell extravasation, or hemosiderin deposition.
Higher magnification confirms the delicate, flattened endothelial lining and lack of atypical features. The vascular lumina contain red blood cells but no thrombi or papillary projections. This superficial, horizontally oriented ‘band-like’ pattern amid solar elastosis distinguishes AEH from other vascular lesions.
Special studies
Immunohistochemistry is rarely required for diagnosis but supports the vascular nature when performed.
- CD31 and CD34: Strong, diffuse positivity highlights the endothelial lining of all vascular channels.
- D2-40 (podoplanin): Variable expression reported (positive in some series, negative in others), raising questions about lymphatic differentiation.
- Ki-67: Low proliferative index (<5%), confined to few endothelial nuclei, confirming benignity.
- Alpha-SMA: Highlights pericytes surrounding vascular channels.
- HHV8: Negative, essential to exclude Kaposi sarcoma.
LYVE-1 and PROX-1 lymphatic markers show inconsistent results, supporting AEH as primarily a blood vascular (capillary hemangioma-like) lesion reactive to UV-induced stromal changes rather than a true lymphangioma. Elastic tissue stains (e.g., Verhoeff-van Gieson) accentuate the surrounding solar elastosis but add little diagnostic value.
Differential diagnoses
AEH enters the histopathological differential of superficial vascular proliferations in sun-damaged skin. Key distinguishing features include:
| Diagnosis | Key Distinguishing Features |
|---|---|
| Low-grade angiosarcoma | Infiltrative growth dissecting collagen; endothelial multilayering, atypia, mitoses; deep extension; lacks sharp borders and prominent elastosis |
| Early patch-stage Kaposi sarcoma | Jagged/anastomosing vessels; promontory sign; lymphoplasmacytic infiltrate; RBC extravasation; HHV8+; irregular dissection of dermis |
| Targetoid hemosiderotic haemangioma | Central dilated vessels with hobnail endothelium transitioning to peripheral ectatic channels; prominent hemosiderin; lacks band-like pattern and solar elastosis |
| Tufted angioma | Cannonball lobules of capillary tufts in dermis/subcutis; lacks superficial band and elastosis; may show lymphatic-like spaces |
| Capillary haemangioma (senile/cherry) | No/minimal solar elastosis; random dermal distribution, not band-like; often endophytic |
Clinical correlation aids differentiation: AEH’s characteristic location in sundamaged skin of older adults, asymptomatic plaque morphology, and lack of systemic associations (e.g., HIV for KS) provide context.
Frequently Asked Questions (FAQs)
What causes acquired elastotic haemangioma?
Chronic UV exposure leading to solar elastosis triggers reactive endothelial proliferation in the superficial dermis.
Is acquired elastotic haemangioma cancerous?
No, it is entirely benign with no risk of malignant transformation. Low Ki-67 confirms negligible proliferative activity.
How is it treated?
Observation suffices for asymptomatic lesions. Surgical excision for cosmesis yields excellent results without recurrence. Oral propranolol shows promise for facial lesions.
Who gets AEH?
Predominantly middle-aged/elderly fair-skinned women on sun-exposed areas like forearms and neck.
Does AEH itch or hurt?
Typically asymptomatic, though rare tenderness reported.
Clinical Significance and Management
Recognition of AEH prevents misdiagnosis as angiosarcoma, averting unnecessary aggressive therapy. Biopsy confirmation via punch or shave suffices diagnostically. Sun protection remains crucial given UV etiology. Multiple lesions are exceptional, potentially hormone-linked (e.g., progesterone). Emerging treatments like propranolol expand non-surgical options, particularly for visible sites. Ongoing research clarifies lymphatic vs. vascular origins via advanced markers.
References
- Acquired elastotic haemangioma pathology — DermNet NZ (Assoc Prof Patrick Emanuel). 2013 (updated). https://dermnetnz.org/topics/acquired-elastotic-haemangioma-pathology
- Acquired Elastotic Hemangioma; Cosmetic Surgery Forum Resident Winners — Practical Dermatology. 2023. https://practicaldermatology.com/youngmd-connect/resident-resource-center/case-report-acquired-elastoic-hemangioma-cosmetic-surgery-forum-resident-winners/21067/
- Acquired elastotic hemangioma, a little-known entity: report of 2 cases — NIH PMC (peer-reviewed). 2018-07-01. https://pmc.ncbi.nlm.nih.gov/articles/PMC6063116/
- Acquired elastotic hemangioma of the face: An effective treatment by oral propranolol — Journal of Pakistan Association of Dermatologists. 2023. https://www.jpad.com.pk/index.php/jpad/article/view/2535
- Acquired elastotic hemangioma: A diagnosis to keep in mind — Our Dermatology Online. 2017. https://www.odermatol.com/odermatology/20174/18.Acquired-RejebSB.pdf
Read full bio of Sneha Tete











