Acromegaly: Causes, Symptoms, Diagnosis And Treatment Guide
Understanding acromegaly: causes, skin changes, systemic effects, diagnosis, and comprehensive treatment strategies for this rare hormonal disorder.
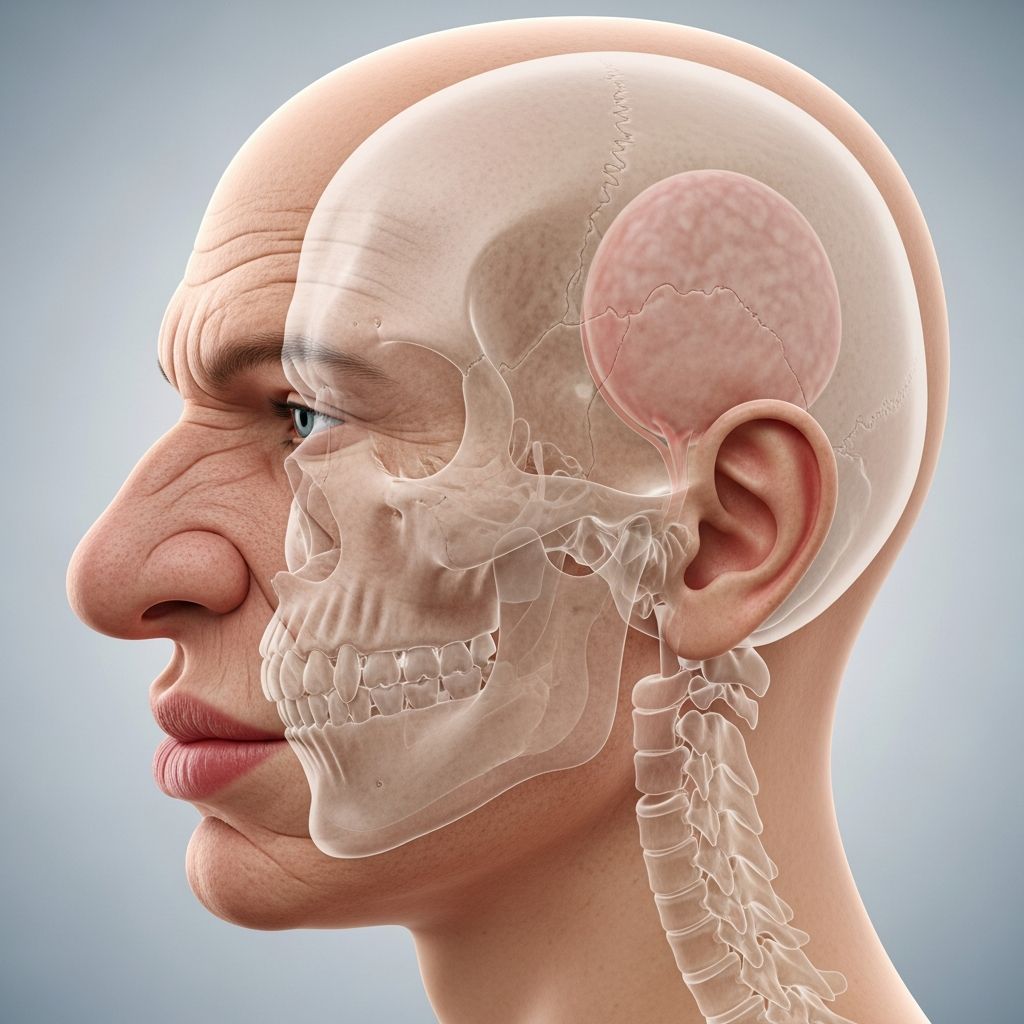
Acromegaly
Acromegaly is a rare chronic disorder characterised by
excessive growth hormone (GH)
production in adults, typically due to apituitary adenoma
. This leads to insidious enlargement of bones and soft tissues, particularly in the hands, feet, face, and skin, resulting in distinctive physical changes and multisystem complications if untreated.What is acromegaly?
Acromegaly arises from
hypersecretion of GH
after epiphyseal closure in adulthood, distinguishing it from gigantism which occurs pre-puberty. The excess GH stimulatesinsulin-like growth factor-1 (IGF-1)
production in the liver, driving acral and facial bone overgrowth, visceromegaly, and metabolic derangements. Approximately 95% of cases stem from benignpituitary adenomas
(somatotrophinomas), with rare causes including ectopic GH-releasing hormone (GHRH) secretion or pituitary hyperplasia.The condition affects 3-4 individuals per million annually, with mean diagnosis age around 45 years and slight male predominance. Untreated acromegaly reduces life expectancy by 10 years due to cardiovascular disease, respiratory failure, and malignancy.
Who gets acromegaly?
Acromegaly typically manifests in
middle-aged adults
(30-60 years), with equal male-female distribution in some cohorts but male predominance noted in others. No strong ethnic or geographic predisposition exists, though delayed diagnosis (average 7-10 years) occurs due to subtle progression.Risk factors include:
- Underlying
pituitary adenoma
(most common). - Genetic syndromes like
multiple endocrine neoplasia type 1 (MEN1)
,carney complex
, orfamilial isolated pituitary adenoma
(5-10% of cases). - Rare ectopic GHRH production from pancreatic/bronchial tumours.
What causes acromegaly?
Over 95% of acromegaly results from
monoclonal pituitary somatotroph adenomas
. These tumours autonomously secrete GH independent of hypothalamic regulation. Microadenomas (<10mm) cause ~15% of cases; macroadenomas (>10mm) cause 85%, often with mass effects like visual field defects.Pathophysiology involves:
- GH hypersecretion → elevated IGF-1 → bone/soft tissue hypertrophy.
- Local tumour expansion → compression of optic chiasm, cavernous sinus invasion.
- Cosecretion of prolactin (25-50% of tumours) or rarely TSH/ACTH.
Rare causes (<1%):
- Ectopic GHRH
- Genetic mutations (AIP gene, GNAS mutations).
from neuroendocrine tumours → pituitary hyperplasia.
What are the clinical features of acromegaly?
Skin features
Characteristic
cutaneous manifestations
often precede systemic symptoms:- Coarse facial features: frontal bossing, deepened nasolabial folds, macroglossia, prognathism, widened dental spaces.
- Acral enlargement: increased ring/shoe size, thickened digits.
- Skin changes: thickened, oily skin; hyperhidrosis (80%); malodorous sweat; acanthosis nigricans; skin tags (75%).
- Acrochordons and
dermal hyperplasia
common.
Systemic features
| System | Manifestations |
|---|---|
| Cardiovascular | Left ventricular hypertrophy, hypertension (35%), cardiomyopathy, arrhythmias |
| Endocrine | Diabetes mellitus (25-50%), insulin resistance, menstrual irregularities, hypopituitarism (30%) |
| Musculoskeletal | Osteoarthritis, joint pain, carpal tunnel syndrome (30-60%), vertebral fractures |
| Respiratory | Sleep apnoea (60%), upper airway obstruction from macroglossia |
| Neoplastic | Colon polyps/cancer risk ↑2-7x, thyroid nodules |
How is acromegaly diagnosed?
Diagnosis combines
clinical suspicion
withbiochemical confirmation
andimaging
:- Biochemical testing:
- Age-adjusted
IGF-1
(gold standard screening). - **Oral glucose tolerance test (OGTT)**: failure of GH suppression <1μg/L diagnostic.
- Random GH unreliable due to pulsatility.
- Age-adjusted
- Imaging: pituitary MRI (95% sensitivity).
- Visual fields if macroadenoma suspected.
Normal ranges: IGF-1 varies by age/sex; OGTT nadir <0.4μg/L excludes diagnosis.
What is the treatment for acromegaly?
Treatment aims to normalise
GH/IGF-1
, reduce tumour volume, preserve pituitary function, and reverse complications.Multimodal therapy
combines surgery, medical therapy, and radiotherapy. No single approach suffices for all patients.Surgery
**Transsphenoidal adenomectomy** is first-line, achieving biochemical remission in 50-80% microadenomas and 20-50% macroadenomas. Endoscopic techniques improve outcomes. Rapid symptom relief occurs within days.
Medical therapy
Three classes used as primary, adjuvant, or salvage therapy:
- Somatostatin receptor ligands (SRLs) (first-line medical): Octreotide LAR, lanreotide autogel (monthly IM), pasireotide. Normalise IGF-1 in 50-65%; tumour shrinkage 20-50%. FDA-approved oral octreotide (Mycapssa) for responders.
- GH receptor antagonist: Pegvisomant (Somavert®) daily SC. Normalises IGF-1 in 90%+ but no antitumour effect. New oral paltusotine approved.
- Dopamine agonists: Cabergoline (licensed off-label). Effective in 10-20%, useful for mild disease/prolactin cosecretion.
Radiotherapy
Reserved for surgical/medical failure. Fractionated external beam (4-6 weeks) achieves control in 50-70% over 5-10 years but risks hypopituitarism (50-80%). Stereotactic radiosurgery for residuals.
Acromegaly in skin of colour
Skin findings remain consistent across ethnicities, though
hyperpigmentation
from acanthosis nigricans may be more prominent in darker skin types. Hyperhidrosis and skin tags universally prevalent. Diagnostic delays similar across groups.Related conditions
- Pseudocromegaly: Ectopic acromegaly, McCune-Albright syndrome.
- Gigantism: Prepubertal GH excess.
- Cushing disease,
primary hypogonadism
(overlapping features).
Frequently asked questions in acromegaly
What is the most common cause of acromegaly?
Pituitary adenoma (95%+), specifically somatotroph adenomas secreting excess GH.
How do you diagnose acromegaly?
Elevated age-matched IGF-1 plus failure of GH suppression <1μg/L on OGTT, confirmed by pituitary MRI.
What does the face look like in acromegaly?
Coarse features: prominent supraorbital ridges, broad nose, prognathism, macroglossia, widened teeth spacing.
Is acromegaly curable?
Biochemical control achievable in 60-80% with multimodal therapy; surgical cure in ~50% microadenomas.
What is the prognosis for treated acromegaly?
Normalised GH/IGF-1 restores life expectancy; untreated mortality increased 2-3x from cardiovascular/respiratory disease.
Activity
Monitor GH/IGF-1 every 3-6 months initially, then annually. Colonoscopy screening q5-10y. Cardiovascular risk management essential.
References
- Acromegaly – Symptoms, Causes, Treatment — National Organization for Rare Disorders (NORD). 2023. https://rarediseases.org/rare-diseases/acromegaly/
- Treatment of Acromegaly — Pituitary Foundation. 2024. https://www.pituitary.org.uk/information/acromegaly-treatment/
- Acromegaly – Symptoms and causes — Mayo Clinic. 2024-01-15. https://www.mayoclinic.org/diseases-conditions/acromegaly/symptoms-causes/syc-20351222
- Acromegaly — National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). 2023-10-23. https://www.niddk.nih.gov/health-information/endocrine-diseases/acromegaly
Read full bio of medha deb











