Adenoid Cystic Carcinoma Pathology: A Comprehensive Guide
Detailed pathology of adenoid cystic carcinoma, including clinical features, histopathology, and differential diagnosis for accurate recognition.
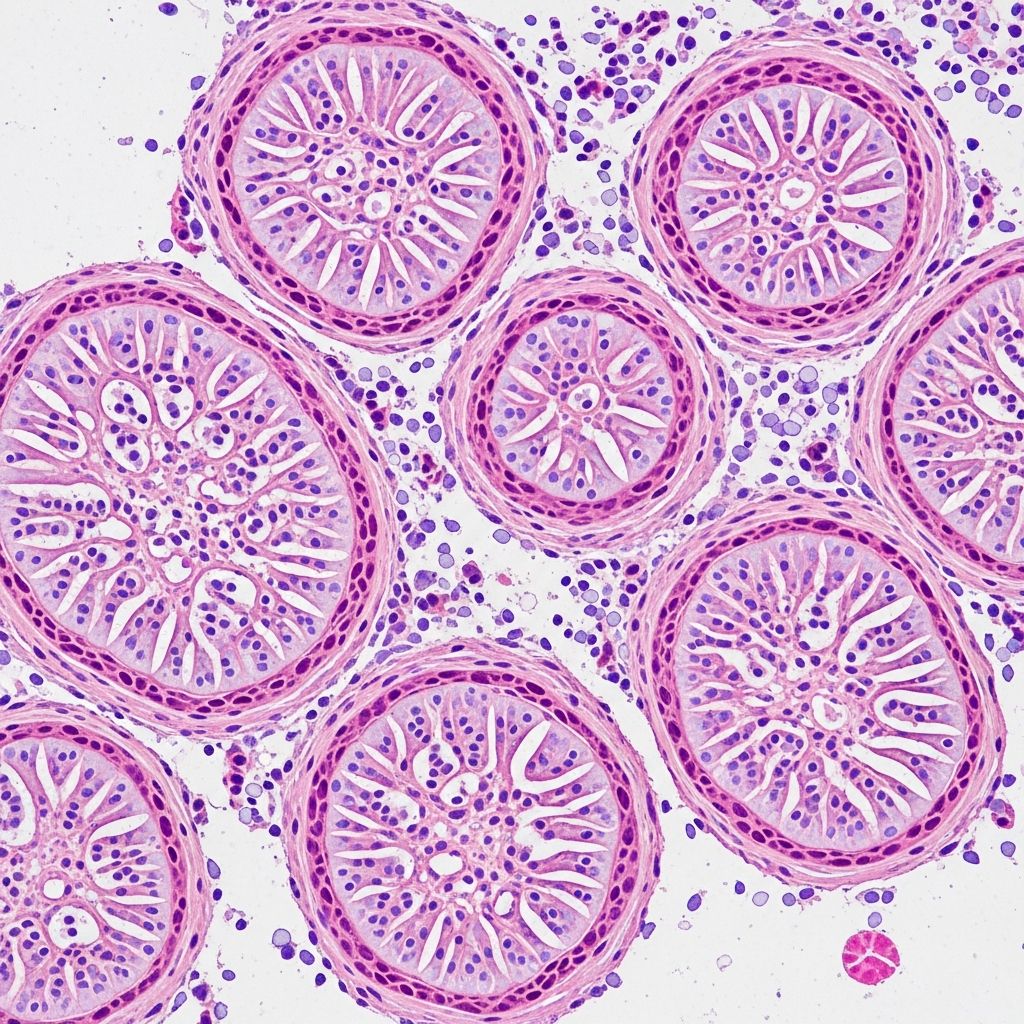
Adenoid cystic carcinoma pathology
Adenoid cystic carcinoma (ACC) represents a distinctive basaloid malignancy characterised by its cribriform, tubular, and solid growth patterns. While most commonly arising in salivary glands, primary cutaneous ACC is a rare entity that poses diagnostic challenges due to its overlap with adnexal tumours. This article details the pathological features, aiding accurate diagnosis and management.
Introduction
Adenoid cystic carcinoma typically originates within salivary glands, accounting for approximately 10% of all salivary gland tumours and being the most common malignancy of minor salivary glands. Primary cutaneous adenoid cystic carcinoma and ACC of the breast are rare but well-recognised variants. In the skin, it manifests as a dermal-based tumour that may extend into the subcutis, often presenting as a slow-growing, painless nodule.
Authoritative sources highlight ACC’s rarity, with an incidence of about 1% of head and neck malignancies, predominantly affecting individuals over 50 years. Its insidious growth and propensity for perineural invasion contribute to delayed diagnosis and potential for distant metastasis, primarily to lungs.
Clinical features
Clinically, primary cutaneous ACC presents as a firm, painless subcutaneous nodule, typically on the scalp, trunk, or proximal extremities. Lesions range from 0.5 to 3 cm in diameter at diagnosis and grow slowly over months to years. Pain or paraesthesia may emerge due to perineural involvement, a hallmark feature reported in over 50% of cases.
- Slow-growing, hard, painless swelling in dermis/subcutis.
- Predilection for head and neck, scalp, chest.
- Perineural invasion common, leading to neuropathic symptoms.
- Low rate of regional lymph node metastasis; hematogenous spread to lungs predominant.
Histologically aggressive despite benign clinical course; 5-year survival exceeds 75%, but 10-year drops to ~20% due to late recurrences.
Histopathology
In primary cutaneous adenoid cystic carcinoma, the tumour involves the dermis and may invade the subcutis. It is composed of uniform basaloid cells arranged in ductal or cribriform patterns. Key features include eosinophilic hyaline membranes lining pseudolumina, creating a ‘Swiss cheese’ appearance.
Three classic histological patterns exist, often intermixed:
- Cribriform (most common): Islands of basaloid cells with round pseudocysts filled with basophilic, PAS-positive mucoid material contiguous with stroma.
- Tubular: Bilayered ductal structures with inner luminal cells and outer myoepithelial cells embedded in hyalinised stroma.
- Solid: Sheets of basaloid cells with high mitotic activity, necrosis; portends worse prognosis.
Tumour cells exhibit scant cytoplasm, hyperchromatic angulated nuclei (carrot-shaped in myoepithelial cells), and perineural invasion is frequent. Hyaline basement membrane material surrounds nests, highlighted by PAS stain.
| Pattern | Key Features | Prognostic Implication |
|---|---|---|
| Cribriform | Pseudocysts with hyaline rims, basaloid cells | Favourable |
| Tubular | Bilayered ducts in stroma | Intermediate |
| Solid | Sheets, mitoses, necrosis | Poor (>30% solid = grade III) |
Histopathology images
- Figure 1. Scanning magnification of primary cutaneous adenoid cystic carcinoma showing a dermal nodule invading subcutis (H&E).
- Figure 2. Cribriform pattern with eosinophilic hyaline membranes lining pseudolumina (arrows; H&E).
- Figure 3. Higher power showing basaloid cells with scant cytoplasm and angular nuclei.
- Figure 4. PAS stain highlights magenta hyaline basement membrane material.
- Figure 5. Perineural invasion by tumour nests.
- Figure 6. Solid pattern with central necrosis (higher grade).
Immunohistochemistry
ACC shows a dual population: ductal (CK7+, S100 focal) and myoepithelial (p63+, calponin+, SMA+) cells. Characteristic markers include:
- CD117 (c-KIT) diffusely positive in basaloid cells.
- p63 strong nuclear positivity in myoepithelial component.
- CK7/CK5/6 positive; ER/PR/HER2 negative.
- S100, calponin, actin highlight myoepithelium.
- MYB overexpression (IHC surrogate for fusion).
IHC distinguishes ACC from mimics: diffuse p63 favours ACC over basaloid SCC (patchy); CD117+ excludes pleomorphic adenoma.
Genetics
The pathognomonic t(6;9)(q22-23;p23-24) MYB-NFIB fusion occurs in >85% of ACC, driving oncogenesis via MYB overexpression. This fusion is detectable by FISH and correlates with cribriform/tubular patterns; solid variants show additional alterations (e.g., 1p36 loss). MYB IHC serves as a diagnostic adjunct.
Differential diagnosis
ACC mimics include adnexal, salivary, and squamous tumours. Key differentials:
| Entity | Distinguishing Features |
|---|---|
| Cylindroma | Jigsaw puzzle architecture; no true atypia; dermal; MYB-. |
| Trichoadenoma/adenoma | Well-circumscribed; ductal differentiation; no perineural invasion. |
| Basaloid SCC | Surface connection; p63 patchy; HPV+; no MYB fusion. |
| Primary cutaneous cribriform carcinoma | Less basement membrane; CK20+ (Merkel cells); no perineural invasion. |
| Extramammary Paget/MCC | CK20+/neurofilament+; pagetoid spread; CK7+/CD117-. |
| Metastatic ACC (salivary) | Identical histology; clinical history key. |
Cylindroma — These tumours exhibit a typical “jigsaw puzzle” architecture rather than the irregular cribriform and tubular architecture of adenoid cystic carcinoma.
Basaloid squamous cell carcinoma – Can mimic adenoid cystic carcinoma. p63 immunohistochemistry can be helpful if this is a diagnostic consideration. Diffuse p63 positivity is more commonly seen with SCC.
Prognosis and management
ACC exhibits prolonged survival but high recurrence risk due to perineural spread. Solid pattern (>30%), size >4cm, bone invasion predict poor outcome. Treatment involves wide surgical excision with margins >1cm, often with adjuvant radiotherapy. Systemic therapy (tyrosine kinase inhibitors targeting c-KIT) for advanced disease.
Frequently asked questions
What is the most common site for adenoid cystic carcinoma?
Salivary glands, particularly minor glands; cutaneous ACC rare (<1% skin tumours).
How is adenoid cystic carcinoma diagnosed pathologically?
Morphology (cribriform/tubular with hyaline pseudolumina) + IHC (CD117+, p63+, MYB+) + genetics (MYB-NFIB fusion).
What is the hallmark genetic abnormality in ACC?
t(6;9) MYB-NFIB fusion in >85% cases, promoting tumorigenesis.
Does cutaneous ACC metastasise?
Less aggressive than salivary ACC; local recurrence common but distant mets rare (lungs if occur).
What stains distinguish ACC from cylindroma?
PAS+ hyaline in ACC; cylindroma shows jigsaw pattern without atypia/perineural invasion; MYB IHC positive in ACC.
References
- Adenoid Cystic Cancer – StatPearls — National Center for Biotechnology Information (NCBI). 2023-08-08. https://www.ncbi.nlm.nih.gov/books/NBK557855/
- Adenoid cystic carcinoma pathology – DermNet — DermNet NZ. 2023. https://dermnetnz.org/topics/adenoid-cystic-carcinoma-pathology
- Adenoid cystic carcinoma – Libre Pathology — Libre Pathology. 2024. https://librepathology.org/wiki/Adenoid_cystic_carcinoma
- Adenoid Cystic Carcinoma – MGH Learn Pathology — Massachusetts General Hospital Pathology. 2023. https://learn.mghpathology.org/index.php/Adenoid_Cystic_Carcinoma
- World Health Organization Classification of Head and Neck Tumours — International Agency for Research on Cancer (IARC). 2022. https://publications.iarc.who.int/Book-And-Report-Series/Who-Classification-Of-Tumours/Head-And-Neck-Tumours-5ed-2022
Read full bio of Sneha Tete










