Allergy To Ethylenediamine: Symptoms, Diagnosis, Treatment
Understanding ethylenediamine contact allergy: causes, symptoms, diagnosis, and management strategies for this potent skin sensitizer.
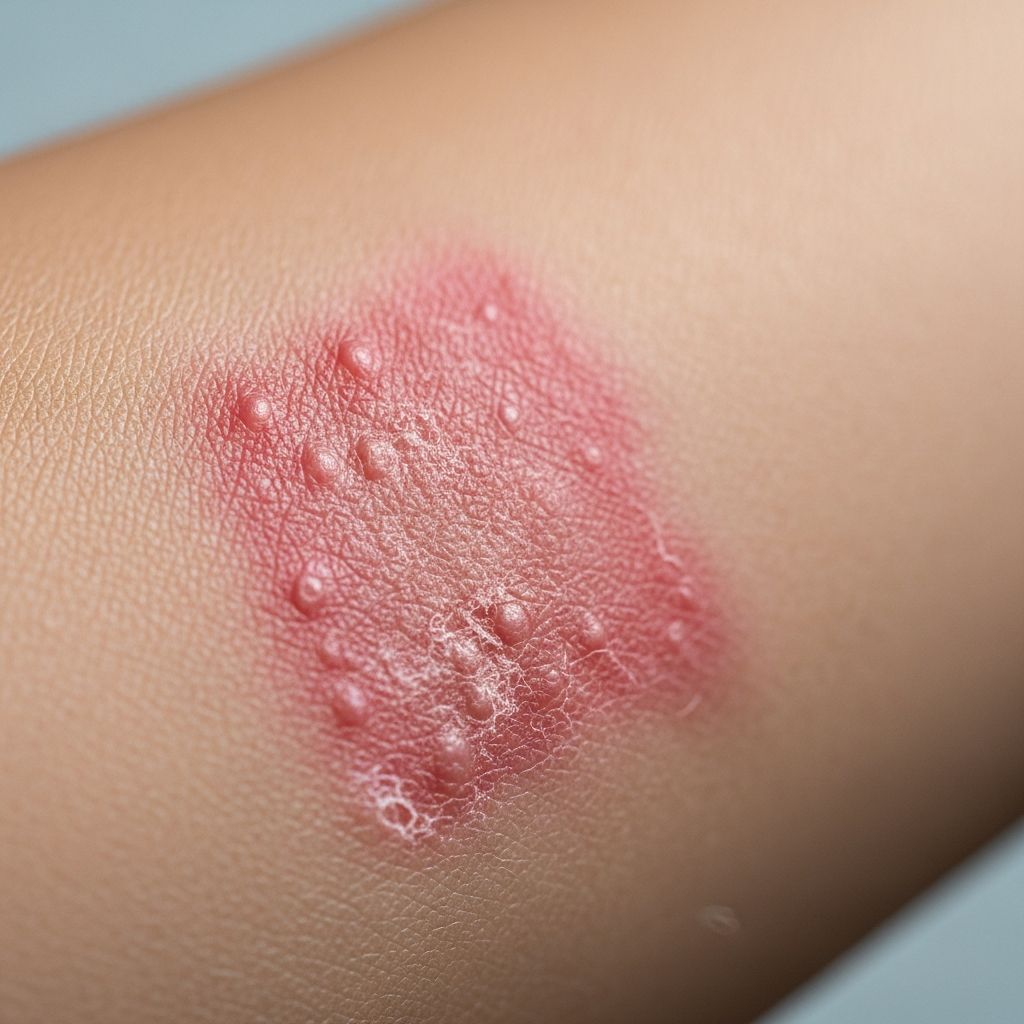
Allergy to Ethylenediamine
Ethylenediamine is a synthetic chemical compound widely used as a stabilizer in topical medications, particularly antibiotic and steroid creams, and in various industrial products. It is a potent skin sensitizer that can trigger
allergic contact dermatitis
in susceptible individuals. This type of allergy manifests as an inflammatory skin reaction upon contact with the substance, often worsening pre-existing skin conditions.What is Ethylenediamine?
Ethylenediamine (EDA), chemically known as H2NCH2CH2NH2, is a colorless liquid with an ammonia-like odor. It serves as a building block in manufacturing dyes, resins, waxes, pesticides, antifreeze, and chelating agents like EDTA. In medicine, it stabilizes emulsions in creams combining antifungals, antibiotics, and corticosteroids, such as nystatin-neomycin-gramicidin-triamcinolone (e.g., Kenacomb, Mycolog).
Its role as a stabilizer prevents ingredient separation, but this utility comes at a cost: EDA is highly allergenic, with damaged or eczematous skin being particularly vulnerable to sensitization. Historically, it was a top contact allergen, ranking fifth in some studies, even surpassing nickel.
Who Gets Ethylenediamine Allergy? (Epidemiology)
Ethylenediamine allergy primarily affects individuals using EDA-containing topical treatments for skin infections or eczema. Patients treating fungal or bacterial skin issues with combination creams like Kenacomb are at highest risk. Occupational exposure occurs in chemical, pharmaceutical, and manufacturing workers handling solvents, adhesives, or coolants.
- Prevalence has declined since the 1970s-1980s due to reformulation of many creams, removing EDA. However, generic versions and industrial uses persist.
- Studies from the 1970s reported it as the fifth most common allergen in patch-tested patients.
- Co-sensitization is frequent; up to 30-50% of EDA-allergic patients react to neomycin, another common cream ingredient.
- At-risk groups: those with chronic eczema, as broken skin facilitates penetration and sensitization.
Sources of Exposure
Exposure occurs via topical medications or occupational/industrial contact. Common sources include:
- Topical medications: Antifungal/steroid creams (Kenacomb, Kenacort, Mycolog, generics with nystatin, neomycin, gramicidin, triamcinolone).
- Industrial products: Solvents, dyes, waxes, pesticides, antifreeze, rubber accelerators, epoxy resins, adhesives.
- Other: Chelating agents (EDTA in foods, soaps, cosmetics), some antihistamines, anti-nausea drugs (though less common now).
Systemic exposure via inhalation or ingestion can exacerbate skin symptoms, causing widespread dermatitis.
Clinical Features (Symptoms)
In sensitized individuals, contact with ethylenediamine provokes classic
allergic contact dermatitis
: red, itchy, inflamed skin that may blister or weep. Reactions often appear or worsen at treated sites, mimicking disease progression but actually allergy-driven.- Local reactions: Eczema-like rash, vesicles, scaling; delayed 24-72 hours post-exposure.
- Systemic contact dermatitis: Generalized eruption from inhaled/oral EDA.
- Associated risks: Asthma-like symptoms (wheezing, shortness of breath), eye irritation, potential liver/kidney effects with high exposure.
Symptoms: itching, redness, swelling, blisters. Severely damaged skin absorbs more, intensifying reactions.
Diagnosis (Patch Testing)
Diagnosis relies on
patch testing
with 1% ethylenediamine in petrolatum, applied under occlusion for 48 hours, read at 48 and 96 hours. This concentration (5x commercial levels) ensures sensitivity without false negatives.| Test Allergen | Concentration | Vehicle | Indication |
|---|---|---|---|
| Ethylenediamine dihydrochloride | 1% | Petrolatum | TRUE Test #11 or custom series |
Positive reaction: erythema, induration, vesicles. Confirm relevance by exposure history. Test for cross-reactants like neomycin, EDTA, antihistamines (e.g., hydroxyzine).
Differential Diagnosis
- Irritant dermatitis (non-immune).
- Other allergies (neomycin, preservatives, fragrances).
- Infection recurrence or steroid withdrawal.
- Endogenous eczema.
Cross-Reactions and Related Allergies
Ethylenediamine cross-reacts with:
- Aminophylline/theophylline: Bronchodilators (avoid).
- EDTA: In foods, cosmetics, cleaners.
- Neomycin: Common co-allergen in creams.
- Other amines: Piperazine, some antihistamines (e.g., hydroxyzine, cimetidine).
Avoid these as precaution.
Management and Treatment
Key principle: Strict avoidance of EDA and cross-reactants.
- Acute phase: Potent topical corticosteroids (non-EDA), emollients, wet wraps. Oral steroids for severe cases.
- Chronic: Barrier creams, protective clothing in occupational settings.
- Patient education: Read labels; alert doctors/pharmacists/dentists. Use Material Safety Data Sheets (MSDS) at work.
For respiratory exposure: Remove from source, supportive care; monitor for pulmonary edema.
Prevention
- Avoid EDA-containing products; choose EDA-free alternatives (e.g., mupirocin, clotrimazole alone).
- Workplace: Gloves, aprons, masks; ventilation; MSDS review.
- Pharmacists: Recommend non-EDA antihistamines/anti-nausea meds.
Outlook / Prognosis
With avoidance, symptoms resolve completely. Allergy may persist lifelong, but reactions lessen if exposure ceases. Prevalence dropped with cream reformulations.
Frequently Asked Questions (FAQs)
Is ethylenediamine allergy common?
Less common today due to reduced use in medications, but still relevant for those exposed industrially or to generics.
What creams contain ethylenediamine?
Primarily older combo creams like Kenacomb, Mycolog. Check labels or databases.
Can I use antihistamines if allergic?
Avoid those with EDA-related structures (e.g., hydroxyzine); opt for loratadine, cetirizine.
How do I protect myself at work?
Use PPE (gloves, masks), request MSDS, substitute if possible.
Does it affect internal organs?
High exposure may irritate lungs, liver, kidneys; skin allergy is primary concern.
Related Information
- Allergic contact dermatitis overview.
- Neomycin allergy.
- Patch testing guide.
References
- ETHYLENEDIAMINE HAZARD SUMMARY — New Jersey Department of Health. 2006. https://www.nj.gov/health/eoh/rtkweb/documents/fs/0875.pdf
- Ethylenediamine contact allergy — DermNet NZ. Accessed 2026. https://dermnetnz.org/topics/allergy-to-ethylenediamine
- NA35: Ethylenediamine Dihydrochloride — SmartPractice Canada. Accessed 2026. https://www.smartpracticecanada.com/spcanada/pdfs/all-allergens/NA35.pdf
- Allergy to Ethylenediamine — JAMA Dermatology (Arch Dermatol). 1975-06. https://jamanetwork.com/journals/jamadermatology/fullarticle/535065
- Allergy to Ethylenediamine — Cutaneous Allergy. Accessed 2026. https://cutaneousallergy.org/pils/ethylenediamine/
- TRUE Test Allergen #11: Ethylenediamine Dihydrochloride — HMP Global Learning Network. Accessed 2026. https://www.hmpgloballearningnetwork.com/site/thederm/article/6555
Read full bio of medha deb











