Alpha-1-Antitrypsin Deficiency Panniculitis
Rare skin inflammation linked to genetic AAT deficiency: causes, symptoms, diagnosis, and targeted treatments explored.
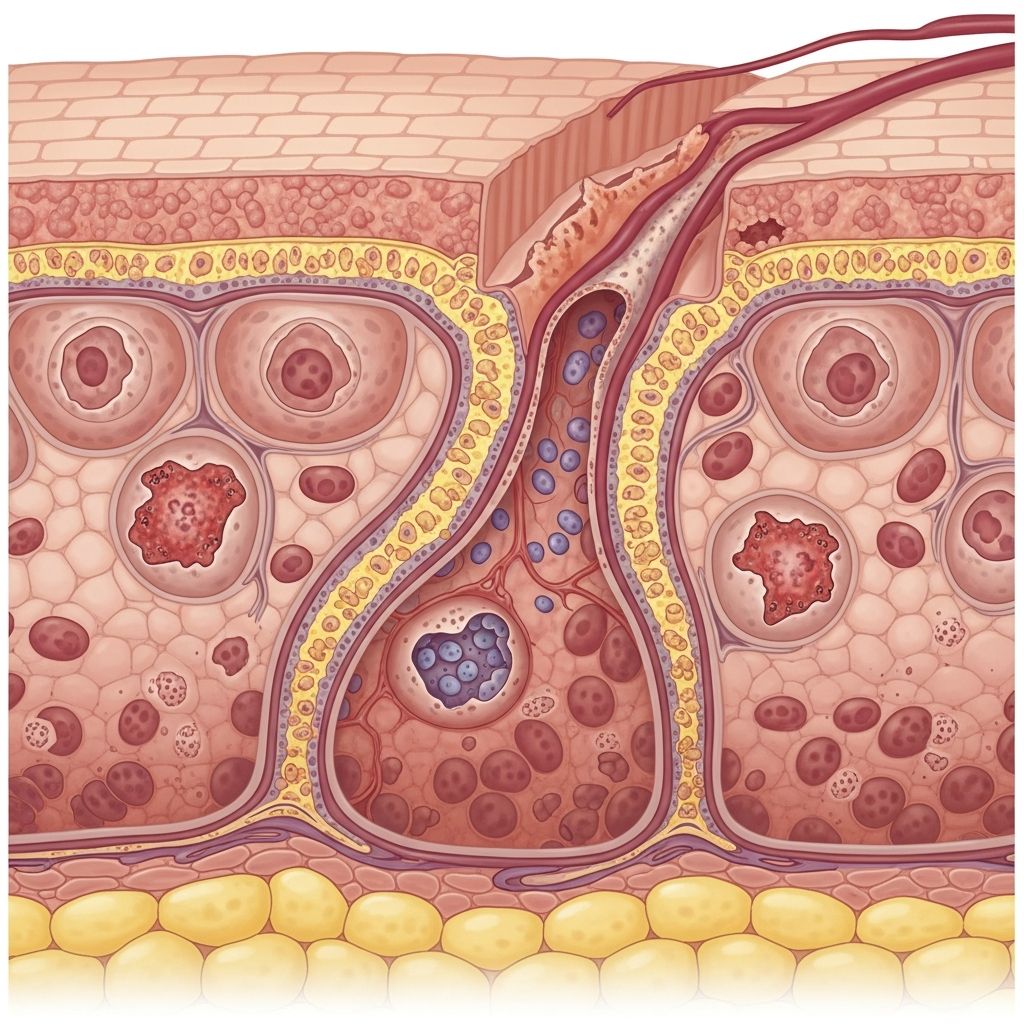
Alpha-1-antitrypsin deficiency is a rare dermatological manifestation of alpha-1-antitrypsin (AAT) deficiency, characterized by inflammation of subcutaneous fat leading to painful, ulcerating nodules that may drain oily fluid. This condition arises from unchecked proteolytic enzyme activity due to low AAT levels, primarily affecting the skin but linked to broader AAT deficiency impacts on lungs and liver.
What is alpha-1-antitrypsin deficiency panniculitis?
Alpha-1-antitrypsin deficiency (AATD or A1AT deficiency) is a genetic disorder causing reduced production or dysfunctional AAT, a key protease inhibitor produced mainly in the liver. Panniculitis refers to inflammation of the subcutaneous adipose tissue beneath the skin. In AATD panniculitis, low AAT levels fail to neutralize enzymes like neutrophil elastase, leading to fat tissue destruction, nodule formation, ulceration, and potential systemic symptoms like fever.
This form is neutrophilic panniculitis, often triggered by trauma, and occurs in a small fraction of AATD patients, not exclusively severe cases. Lesions typically present as tender, erythematous, indurated subcutaneous nodules with irregular borders, progressing to ulceration and serosanguineous or oily discharge.
Who gets alpha-1-antitrypsin deficiency panniculitis?
AATD panniculitis affects males and females equally across all ages, including rare pediatric cases, though average onset is around 40 years. It is most prevalent in Caucasians of Northern European descent due to higher AATD carrier rates. True incidence is underreported as AATD is often undiagnosed; one study found panniculitis in 0.9% of ZZ homozygotes, but up to 15% of biopsy-proven panniculitis cases in some series had AATD.
Risk is higher in severe deficiency genotypes like ZZ (Pi*ZZ), but moderate phenotypes (e.g., MZ, SZ) can also manifest. Trauma often precedes lesions, as injury activates proteases that AAT normally curbs. Patients may have coexisting emphysema, liver disease, or be asymptomatic systemically until skin involvement.
What causes alpha-1-antitrypsin deficiency panniculitis?
AATD results from mutations in the SERPINA1 gene on chromosome 14, inherited autosomal codominantly. AAT normally inhibits serine proteases (e.g., elastase, trypsin, chymotrypsin) to prevent tissue damage. Deficiency leads to unopposed enzyme activity, causing inflammation and necrosis in lungs (emphysema), liver (cirrhosis), and skin (panniculitis).
In skin, neutrophil-derived elastase degrades subcutaneous fat post-trauma or spontaneously, forming liquefying nodules. Unlike typical panniculitis, AATD-related lesions resist antibiotics/steroids due to proteolytic dominance.
- Genetic basis: Pi*ZZ (homozygous severe), Pi*MZ/SZ (heterozygous moderate).
- Trigger: Trauma increases protease release.
- Pathophysiology: Protease-antiprotease imbalance → adipose necrosis → ulceration/drainage.
What are the clinical features of alpha-1-antitrypsin deficiency panniculitis?
Lesions start as tender, red, inflamed subcutaneous nodules (1-10 cm), often on trunk, extremities, thighs, buttocks, or pressure areas. They harden (indurated), develop irregular borders, and progress to ulceration with oily, serosanguineous drainage. Systemic signs include fever; severe cases cause extensive tissue damage.
| Feature | Description |
|---|---|
| Nodules | Tender, erythematous, subcutaneous, irregular borders |
| Ulceration | Breaks open, leaks oily/serous fluid, bleeds |
| Locations | Trunk, limbs, thighs, buttocks (pressure sites) |
| Systemic | Fever, potential liver/lung comorbidity |
Lesions may migrate or recur; trauma exacerbates. Unlike Weber-Christian panniculitis, AATD type is lobular, neutrophilic on biopsy.
Diagnosis
Suspect AATD panniculitis in liquefying/ulcerating panniculitis with emphysema/hepatitis history. Confirm via:
- Serum AAT levels: Low (<80 mg/dL); phenotype/genotyping (Pi*ZZ most severe).
- Biopsy: Lobular panniculitis with neutrophils, no vasculitis; AAT immunostaining negative in lesions.
- Liver/lung eval: For cirrhosis/emphysema.
Differential: Infections, autoimmune panniculitis, factitial; AAT testing essential.
Treatment
AATD panniculitis resists antibiotics/steroids, which may worsen via immunosuppression. Effective options:
- AAT augmentation therapy: IV purified AAT (e.g., Prolastin) raises levels, promotes healing; most efficacious, especially refractory cases.
- Dapsone: Inhibits neutrophil chemotaxis; cost-effective first-line, but remission failure common.
- Doxycycline: Anti-inflammatory, neutrophil-modulating.
- Supportive: Wound care, avoid trauma; rarely excision.
Glucocorticoids ineffective/high failure. Monitor for lung/liver progression; augmentation FDA-approved for emphysema, off-label for skin.
Frequently asked questions (FAQs) on alpha-1-antitrypsin deficiency panniculitis
Q: Is alpha-1-antitrypsin deficiency panniculitis contagious?
A: No, it is a genetic inflammatory condition, not infectious.
Q: Can children get AATD panniculitis?
A: Yes, rarely, though more common in adults around age 40.
Q: Does trauma cause AATD panniculitis?
A: It often precedes lesions by activating proteases.
Q: Is AAT augmentation therapy curative?
A: It controls symptoms effectively but requires ongoing infusions; not curative.
Q: How common is panniculitis in AATD patients?
A: Rare (<1% in ZZ), but AATD found in up to 15% of panniculitis biopsies.
Related topics
- Alpha-1 antitrypsin deficiency
- Erythema nodosum
- Idiopathic lobular panniculitis
- Liver diseases
- Neutrophilic dermatoses
References
- Alpha-1 Antitrypsin Deficiency – Symptoms, Causes — National Organization for Rare Disorders (rarediseases.org). Accessed 2026. https://rarediseases.org/rare-diseases/alpha-1-antitrypsin-deficiency/
- Alpha-1-antitrypsin deficiency panniculitis — DermNet NZ. Accessed 2026. https://dermnetnz.org/topics/alpha-1-antitrypsin-deficiency-panniculitis
- Alpha 1 Antitrypsin Deficiency Panniculitis — Perris Dermatology (perridermatology.com). 2013-03-23. https://perridermatology.com/dr-perris-blog/panniculitis-alpha-1-antitrypsin-deficiency-panniculitis/
- Alpha-1 and Panniculitis — Alpha-1 Foundation (alpha1.org). Accessed 2026. https://alpha1.org/panniculitis/
- Alpha-1 antitrypsin deficiency-associated panniculitis — PubMed (pubmed.ncbi.nlm.nih.gov/33516773). 2022. https://pubmed.ncbi.nlm.nih.gov/33516773/
- Alpha-1 Antitrypsin Deficiency: Causes, Symptoms — Cleveland Clinic (my.clevelandclinic.org). Accessed 2026. https://my.clevelandclinic.org/health/diseases/21175-alpha-1-antitrypsin-deficiency
- Alpha-1-antitrypsin deficiency – Symptoms and causes — Mayo Clinic (mayoclinic.org). Accessed 2026. https://www.mayoclinic.org/diseases-conditions/alpha-1-antitrypsin-deficiency/symptoms-causes/syc-20588790
Read full bio of Sneha Tete










