Anal Disorders: Causes, Symptoms, and Treatment
Complete guide to understanding anal disorders, their symptoms, and effective treatment options.
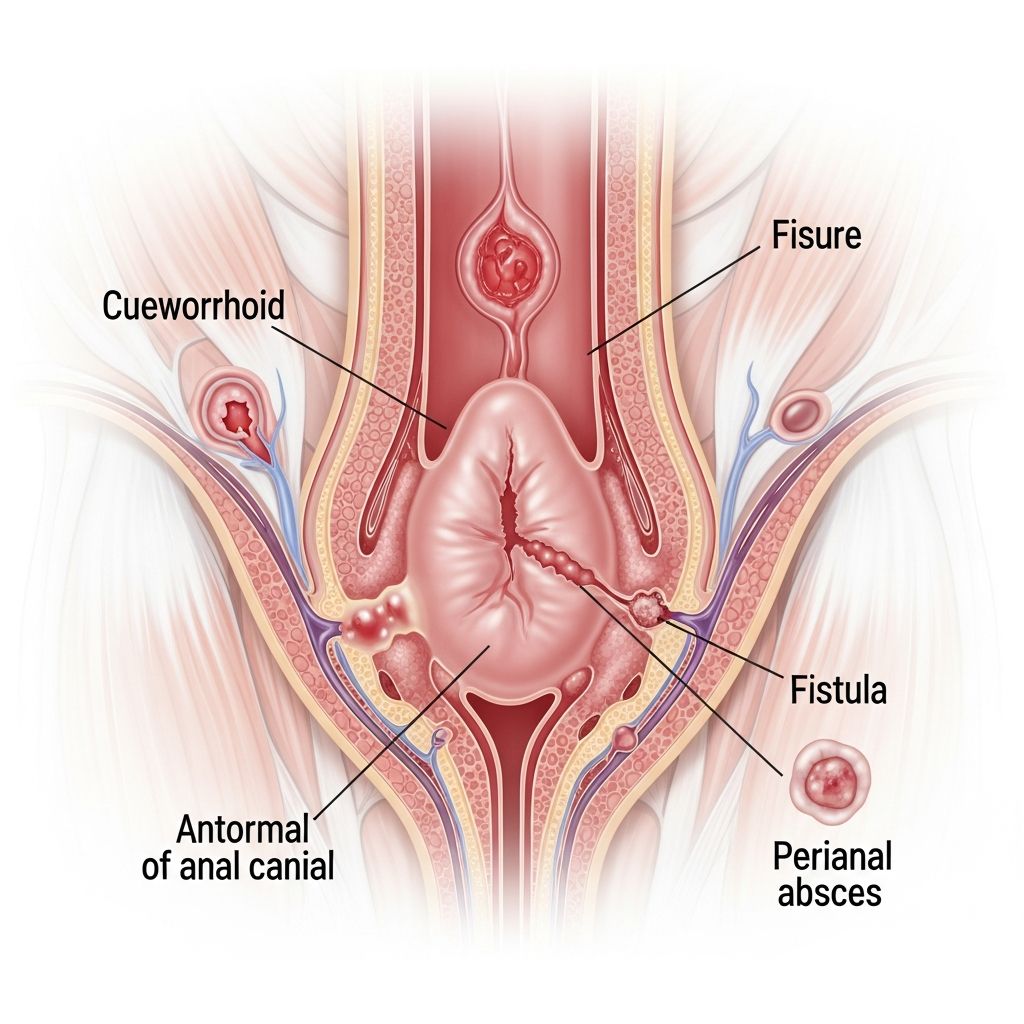
Anal Disorders: A Comprehensive Guide
Anal disorders are common health conditions that affect millions of people worldwide. While often considered a sensitive topic, understanding these conditions is essential for recognizing symptoms and seeking appropriate treatment. Many anal disorders are benign and manageable with proper care, though some may require medical intervention. This guide covers the most prevalent anal disorders, their causes, symptoms, and available treatment options.
Understanding the Anatomy
The anus is the opening at the end of the digestive tract where stool exits the body. It consists of specialized muscles called sphincters that control bowel movements. The anal canal is lined with sensitive tissue, making it susceptible to various conditions. Understanding the basic anatomy helps in recognizing when something may be wrong and when professional medical evaluation is necessary.
Common Anal Disorders
Hemorrhoids (Piles)
Hemorrhoids are among the most common anal disorders, affecting approximately 3 out of 4 adults at some point in their lives. They are swollen blood vessels in the anal area that can develop internally or externally.
Types and Causes: External hemorrhoids occur in the tissue surrounding the anus, while internal hemorrhoids develop inside the rectum. Common causes include straining during bowel movements, low-fiber diets, chronic constipation or diarrhea, prolonged sitting, and pregnancy. Hemorrhoidal tissue becomes engorged with blood, causing the characteristic swelling.
Symptoms: External hemorrhoids may appear as lumps around the anus and can be painful or itchy. They may bleed, particularly during bowel movements. Some hemorrhoids produce no discomfort at all. Internal hemorrhoids may cause bleeding during defecation, though they are often painless. Patients might notice bright red blood on toilet paper or in the stool.
Treatment Options: Most hemorrhoids resolve without treatment. Conservative approaches include increasing fiber intake, drinking adequate water, using stool softeners, and taking warm baths. Over-the-counter creams and ointments can provide relief from itching and discomfort. Ice packs wrapped in clean towels can help reduce swelling when applied for 30 minutes at a time. For persistent or severe hemorrhoids, medical procedures such as rubber band ligation, sclerotherapy, or surgical removal may be necessary.
Anal Fissures
An anal fissure is a small tear in the lining of the anal canal. These painful conditions are often mistaken for hemorrhoids but have distinct characteristics and causes.
Causes: Anal fissures commonly result from passing hard stools, chronic diarrhea, irritable bowel syndrome, or a tight anal sphincter muscle. They can also occur following vaginal childbirth, anal sex, or in rare cases, anal tumors or infections. The trauma to the sensitive anal tissue creates a tear that can become chronic if not properly treated.
Symptoms: Patients experience sharp, burning pain during and after bowel movements, often lasting several hours. Bleeding may occur, and a visible lump or skin tag may develop near the fissure. The pain can be severe enough to cause anxiety about subsequent bowel movements, potentially leading to constipation and worsening of the condition.
Treatment: Initial management includes dietary modifications to prevent constipation, increased water intake, and topical anesthetics for pain relief. Warm baths can soothe the area and promote healing. In a significant study, approximately 89 percent of people with uncomplicated anal fissures were successfully treated with Botox injections, which relax the anal sphincter and allow healing. Surgical intervention may be considered for chronic fissures that don’t respond to conservative treatment.
Anal Abscesses
An anal abscess is a collection of pus around inflamed tissue caused by bacterial infection. This condition requires prompt medical attention.
Formation and Risk Factors: Anal abscesses develop when a gland in the anus becomes clogged and subsequently infected. The infection occurs when bacteria, fecal matter, or foreign material enters through tiny cracks in the tissue. Certain conditions, such as colitis, increase the risk of abscess development. More than half of anal abscesses occur in people between ages 20 to 40, with men being more commonly affected than women.
Symptoms: Patients experience pain, swelling, and a noticeable lump around the anus. Fever may accompany the infection. The pain can be severe and progressively worsen without treatment.
Treatment: Surgical drainage is considered the most effective treatment for anal abscesses. The procedure involves making an incision to allow the accumulated pus to drain. Antibiotics may be recommended, particularly for patients with underlying conditions such as diabetes or compromised immune systems. Prompt treatment prevents the development of complications, including anal fistulas.
Anal Fistulas
An anal fistula is an abnormal tunnel that forms inside the anus and exits through the skin on the buttocks. This condition often develops as a complication of anal abscesses.
Development: Approximately half of individuals who have experienced an anal abscess will develop a fistula. The tunnel forms when an abscess doesn’t fully resolve or when the drainage site doesn’t close properly. Fistulas can be simple or complex, depending on their path and depth.
Symptoms: Common symptoms include anal swelling, irritation, pain, and itching. Patients may experience stool leakage or a discharge from the opening on the skin. Recurrent infection and drainage are common problems associated with untreated fistulas.
Treatment: Surgical intervention is typically necessary to treat anal fistulas. The treatment approach depends on the fistula’s complexity. Surgical options include opening the tunnel, plugging it with special material, or tying it off. Complex fistulas may require staged procedures to minimize the risk of fecal incontinence.
Perianal Crohn’s Disease
Crohn’s disease is a chronic inflammatory bowel condition that can affect the entire digestive tract, including the anus and rectum. When it affects the perianal area, it presents unique management challenges.
Prevalence and Manifestations: Up to 43 percent of people with Crohn’s disease develop perianal involvement. This manifestation can include anal fissures, fistulas, and abscesses. The inflammation associated with Crohn’s disease makes these complications more prone to recurrence and more difficult to treat.
Treatment Approach: Management of perianal Crohn’s disease is multifaceted. Antibiotic therapy is often employed to control infection. Surgical intervention may be necessary for fistulas and abscesses, though surgery in Crohn’s patients requires careful planning. Additional supportive measures include periodic icing, warm baths, and over-the-counter pain relievers and anti-inflammatory medications. Systemic treatment of the underlying Crohn’s disease is essential for managing perianal complications.
Other Anal Conditions
Anal Sex and Injury
Anal swelling can occur following anal sexual activity, particularly if inadequate lubrication is used or if the activity is rough. Proper precautions include using plenty of water-based lubricant, employing barrier protection such as condoms or dams, and ensuring partners remove rings and trim fingernails to prevent tissue damage. These measures significantly reduce the risk of tears, infections, and sexually transmitted infections.
Sexually Transmitted Infections
Various sexually transmitted infections can cause anal and rectal swelling. Common culprits include gonorrhea, herpes simplex virus, and human papillomavirus (HPV). Symptoms may include pain, discharge, swelling, and itching. Proper diagnosis and treatment with appropriate antibiotics or antivirals is essential. HPV is particularly significant as it significantly increases the risk of anal cancer. HPV vaccination can substantially reduce the risk of developing anal cancer.
Diagnostic Procedures
When anal symptoms persist or are particularly concerning, healthcare providers may recommend diagnostic procedures to identify the underlying cause:
Anoscopy: This procedure uses a tube with a light source that allows direct visualization of the anus and rectum. It’s useful for identifying hemorrhoids, fissures, and other visible lesions.
Flexible Sigmoidoscopy: This procedure employs a flexible tube with a light and camera to examine the rectum and lower intestinal tract. It’s particularly valuable when Crohn’s disease or other inflammatory conditions are suspected.
Colonoscopy: A long, flexible tube with a camera is inserted through the anus to visualize the entire colon. This procedure is typically used to rule out cancer and evaluate for inflammatory bowel disease or other serious conditions.
Prevention and Self-Care
Dietary and Lifestyle Measures
Preventing anal disorders often involves simple lifestyle modifications. Consuming a high-fiber diet rich in fruits, vegetables, and whole grains promotes healthy bowel movements and prevents constipation. Drinking 6 to 8 glasses of water daily maintains proper hydration and stool consistency. Regular exercise, maintaining a healthy body weight, and avoiding smoking or vaping all contribute to anal health.
Proper Toilet Habits
Appropriate toilet practices significantly impact anal health. Respond to the urge to defecate promptly rather than holding on, as this can lead to constipation. Proper sitting position is important: rest your elbows on your knees, lean forward, and consider using a footstool to elevate your knees higher than your hips. This positioning promotes easier, more natural bowel movements. Avoid straining, as excessive pressure increases pressure on anal tissues and can worsen existing conditions.
Personal Hygiene
Gentle anal hygiene is essential. After bowel movements and before bed, gently wash and dry the anus with wet toilet paper or a washcloth using plain water or unscented soap. Avoid scented soaps, bubble baths, perfumes, talcum powder, and deodorants, as these can irritate the sensitive tissue. Wear cotton underwear that isn’t tight. Do not use douches or enemas, as these can damage the rectum.
When to Seek Medical Attention
Seek immediate medical attention if you experience any of the following:
– Anal bleeding that won’t stop, particularly if accompanied by dizziness or lightheadedness- Severe pain- Anal pain with fever or chills- Increasing pain despite self-care measures- Anal discharge
Schedule a doctor’s appointment if you have:
– Changes in bowel movements- Rectal bleeding- Anal pain unrelieved by self-care techniques after several days- Any new or unusual lumps near the anus- Persistent itching not improving with over-the-counter treatments- Difficulty controlling bowel movements
Frequently Asked Questions
Q: Are hemorrhoids dangerous?
A: Most hemorrhoids are not dangerous, though they can be uncomfortable. However, significant or persistent bleeding should be evaluated by a healthcare provider to rule out other conditions.
Q: Can anal fissures heal on their own?
A: Many anal fissures heal with conservative treatment including dietary changes, increased water intake, and topical treatments. However, chronic fissures may require medical intervention such as Botox injections or surgery.
Q: Is anal abscess contagious?
A: Anal abscesses are not contagious to others. They result from bacterial infection within an individual’s own anal glands and tissues.
Q: Can anal fistulas be prevented?
A: While fistulas often develop from untreated or inadequately treated abscesses, prompt drainage and appropriate care of anal abscesses significantly reduces fistula development.
Q: What is the connection between HPV and anal cancer?
A: Most anal cancers are caused by human papillomavirus (HPV). HPV vaccination can lower the chance of developing anal cancer.
Q: How long does anal fissure pain last?
A: Pain from anal fissures can last from hours to days after bowel movements. With proper treatment, healing typically occurs within a few weeks.
Conclusion
Anal disorders are common health conditions that, while sometimes embarrassing to discuss, deserve appropriate medical attention when necessary. Most anal conditions are manageable with conservative treatment, lifestyle modifications, and proper hygiene. However, when symptoms persist or worsen, professional medical evaluation is essential to ensure proper diagnosis and treatment. By understanding these conditions and taking preventive measures, individuals can maintain better anal health and quality of life. Don’t hesitate to consult with a healthcare provider if you experience concerning anal symptoms—early intervention often leads to better outcomes and faster resolution.
References
- Swollen Anus: Causes, Symptoms, and Treatment — Healthline. 2024. https://www.healthline.com/health/swollen-anus
- Anal Care Guide — Health Direct Australia (Australian Department of Health). July 2025. https://www.healthdirect.gov.au/anal-care
- Anal Disorders Overview — Harvard Health Publishing. https://www.health.harvard.edu/a_to_z/anal-disorders-a-to-z
Read full bio of Sneha Tete










