Angioplasty and Stent Placement for the Heart
Complete guide to heart angioplasty and stent placement procedures, recovery, and outcomes.
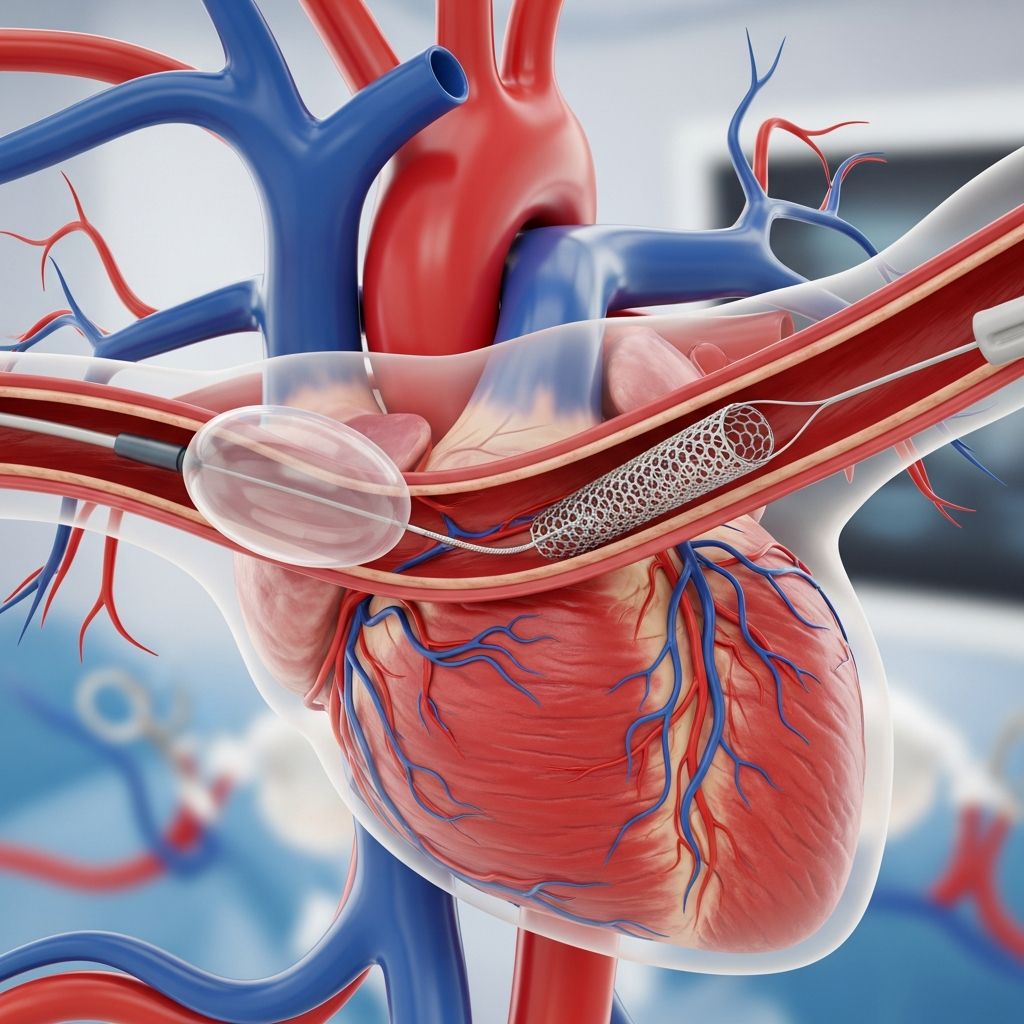
Angioplasty and stent placement are minimally invasive procedures used to treat narrowed or blocked coronary arteries that supply blood to the heart muscle. These procedures are among the most common interventions performed to restore blood flow and relieve symptoms of coronary artery disease. Whether performed as a planned procedure or emergency treatment during a heart attack, angioplasty and stent placement offer patients a less invasive alternative to open-heart surgery while providing effective relief from chest pain and improving heart function.
What Is Angioplasty?
Angioplasty, also known as percutaneous coronary intervention (PCI), is a procedure designed to open narrowed or blocked blood vessels that supply blood to the heart. The term “angioplasty” refers to the reshaping of blood vessels using a balloon-tipped catheter. During this minimally invasive procedure, a cardiologist uses specialized imaging techniques to guide a thin, flexible tube called a catheter through the blood vessels to reach the blockage in the coronary arteries.
The procedure works by inflating a small balloon at the tip of the catheter, which compresses the plaque buildup against the artery walls and widens the vessel. This restores proper blood flow to the heart muscle, relieving symptoms such as chest pain and shortness of breath. In most cases, a stent—a small metal mesh tube—is placed during or immediately after angioplasty to help keep the artery open and prevent it from closing again.
Understanding Coronary Artery Stents
A coronary artery stent is a small, metal mesh tube that expands inside a coronary artery to maintain its patency following angioplasty. Stents serve as scaffolding within the artery, providing structural support and preventing restenosis, which is the re-narrowing of the vessel. Modern stents are typically drug-eluting stents, meaning they are coated with medication that is gradually released over time to prevent scar tissue formation and further narrowing of the artery.
Drug-eluting stents have become the gold standard in interventional cardiology because they significantly reduce the risk of the artery closing back up compared to bare-metal stents. The medication embedded in these stents helps suppress the body’s natural healing response that can lead to excessive scar tissue formation within the stent, which would otherwise narrow the artery again.
Why the Procedure Is Performed
Angioplasty and stent placement are performed to treat coronary artery disease, a condition characterized by the buildup of plaque—made up of fat, cholesterol, and other substances—on the inside of artery walls. This buildup, known as atherosclerosis, narrows the arteries and restricts blood flow to the heart muscle. Several specific conditions warrant this intervention:
Acute Coronary Syndromes
During or immediately after a heart attack, emergency angioplasty with stent placement can restore blood flow through blocked coronary arteries, minimizing damage to the heart muscle and improving survival outcomes.
Chronic Stable Angina
Persistent chest pain caused by narrowed coronary arteries that does not respond adequately to medications can be relieved through angioplasty and stent placement, restoring blood flow and reducing symptoms.
Heart Failure
Blockage or narrowing of one or more coronary arteries that impair heart function and lead to heart failure may be treated with angioplasty and stenting to improve cardiac performance.
Silent Ischemia
In some patients, significant coronary artery narrowing exists without causing noticeable symptoms. When detected, these blockages may be treated prophylactically to prevent future heart attacks.
How the Procedure Works
Pre-Procedure Preparation
Before the angioplasty procedure begins, patients receive pain medication and sedation to ensure comfort throughout the intervention. Blood-thinning medications are administered intravenously to prevent blood clots from forming during the procedure. The area where the catheter will be inserted is cleaned and numbed with local anesthetic. Sticky patches called electrodes are placed on the chest to continuously monitor heart rate and rhythm throughout the procedure.
Catheter Insertion and Navigation
The cardiologist makes a small incision to access a blood vessel, typically in the wrist (radial artery) or groin (femoral artery). A sheath is first inserted into the blood vessel to provide a pathway. A flexible guide wire is then inserted through the sheath and carefully advanced through the blood vessels toward the heart. The balloon-tipped catheter is threaded over this guide wire and guided toward the area of blockage using real-time x-ray imaging.
Angiography and Blockage Identification
Once the catheter is positioned near the coronary artery, contrast material (sometimes referred to as “dye”) is injected through the catheter. This contrast makes the blood vessels visible on x-ray images, allowing the cardiologist to identify the exact location and severity of the blockage. This angiographic imaging is crucial for determining the appropriate treatment strategy.
Balloon Inflation and Plaque Compression
A guide wire is carefully advanced across the blockage, creating a pathway for the balloon catheter. Once positioned correctly, the balloon is inflated with controlled pressure. As the balloon expands, it compresses the plaque against the artery wall and widens the vessel lumen. Sometimes the balloon may need to be inflated more than once to achieve optimal widening of the artery.
Stent Placement
In most cases, a stent is deployed at the site of the blockage. The stent is mounted on the balloon catheter and expands as the balloon inflates, embedding itself into the vessel wall. Once the stent is properly positioned and expanded, the balloon is deflated and removed, leaving the stent in place to maintain arterial patency.
Procedure Completion
After successful stent placement and confirmation of adequate blood flow through angiography, the catheters and guide wires are carefully removed. The small incision site is then closed, typically with a pressure dressing or closure device, and the patient is transferred to the recovery area.
Types of Stents
| Stent Type | Description | Advantages | Considerations |
|---|---|---|---|
| Drug-Eluting Stents (DES) | Metal mesh coated with medication that prevents restenosis | Reduced restenosis rates; improved long-term outcomes; most commonly used | Requires longer dual antiplatelet therapy; higher initial cost |
| Bare-Metal Stents (BMS) | Uncoated metal mesh stent | Lower cost; shorter dual therapy duration needed | Higher restenosis rates; less commonly used today |
| Bioresorbable Vascular Scaffolds | Stent that gradually dissolves after healing | Theoretical restoration of normal vessel function; research ongoing | Limited clinical data; not widely available |
Risks and Complications
While angioplasty and stent placement are generally safe procedures, they carry potential risks that patients should understand before undergoing the intervention.
Common Risks
Bleeding at the catheter insertion site is the most frequent complication, though usually minor and easily managed with pressure dressing. Some patients experience bruising or minor infections at the puncture site. Allergic reactions to contrast material or medications used during the procedure can occur, though serious reactions are rare.
Procedural Complications
Coronary artery dissection, where the artery wall develops a small tear, can occur during catheter manipulation. Vasospasm, a temporary constriction of the coronary artery, may reduce blood flow temporarily but usually responds well to medication. Perforation of a coronary artery is a rare but serious complication requiring emergency intervention.
Post-Procedure Complications
Restenosis, the re-narrowing of the treated artery, can occur even with drug-eluting stents, though at much lower rates than with bare-metal stents. Stent thrombosis, blood clot formation within the stent, is a rare but potentially serious complication that highlights the importance of taking prescribed antiplatelet medications. Contrast-induced nephropathy, temporary kidney function impairment from contrast material exposure, can occur in patients with pre-existing kidney disease.
Recovery and Post-Procedure Care
Immediate Recovery
After the procedure, patients are transferred to a recovery area where vital signs are monitored closely. The catheter insertion site is kept immobilized and monitored for bleeding. Most patients can return home the same day or after an overnight stay, depending on procedural complexity and overall health status.
Activity Restrictions
Patients are advised to limit strenuous activity and heavy lifting for several days following the procedure. Gradual return to normal activities is encouraged, with most patients resuming routine activities within 3-7 days. Your cardiologist will provide specific activity guidelines based on individual circumstances.
Medication Management
Dual antiplatelet therapy (DAPT), typically aspirin combined with a P2Y12 inhibitor such as clopidogrel, ticagrelor, or prasugrel, is essential after stent placement. These medications prevent blood clots from forming within the stent. The duration of DAPT varies depending on stent type and clinical circumstances, typically ranging from one month to one year or longer.
Incision Site Care
The catheter insertion site should be kept clean and dry. Patients are advised to avoid soaking the wound in baths or swimming until it is fully healed. Any signs of infection, including increased redness, swelling, warmth, drainage, or fever, should be reported to the healthcare provider immediately.
Follow-Up Appointments
Regular follow-up visits with the cardiologist are scheduled to assess recovery progress, review medications, and evaluate heart function. These appointments allow early detection and management of any complications that may arise.
Lifestyle Modifications
To maximize the benefits of angioplasty and stent placement and reduce the risk of future blockages, comprehensive lifestyle modifications are essential. A heart-healthy diet low in saturated fats, trans fats, and cholesterol, and rich in fruits, vegetables, whole grains, and lean proteins supports cardiovascular health. Regular physical activity, as recommended by your cardiologist, strengthens the heart and improves circulation. Smoking cessation is critical, as continued smoking significantly increases the risk of restenosis and future cardiac events. Stress management through relaxation techniques, meditation, or counseling helps reduce cardiovascular strain. Maintaining a healthy weight and managing conditions such as diabetes, hypertension, and high cholesterol through medications and lifestyle changes prevents further arterial damage.
Success Rates and Outcomes
Angioplasty and stent placement have excellent success rates, with immediate procedural success achieved in over 95 percent of cases. Modern drug-eluting stents significantly reduce restenosis rates to approximately 5-10 percent compared to 20-30 percent with bare-metal stents. Long-term outcomes depend on multiple factors including the severity of coronary disease, left ventricular function, presence of diabetes, and adherence to prescribed medications and lifestyle modifications.
Most patients experience significant symptom improvement, with relief of chest pain and improved exercise tolerance. Quality of life improvements are common, allowing patients to return to normal daily activities and pursue meaningful pursuits. However, angioplasty does not cure underlying atherosclerosis, and continued management of coronary risk factors remains necessary to prevent disease progression in untreated vessels.
Frequently Asked Questions
Q: How long does the angioplasty procedure take?
A: The procedure typically takes 30 minutes to two hours, depending on the complexity of the blockage and whether multiple vessels require treatment.
Q: Will I feel pain during the procedure?
A: Most patients do not experience significant pain during the procedure due to local anesthesia and sedation, though mild pressure sensation may be felt.
Q: How long does a stent last?
A: Modern drug-eluting stents are designed to be permanent fixtures within the artery. They continue to provide benefit indefinitely with proper medication adherence.
Q: Can I have another angioplasty if restenosis occurs?
A: Yes, repeat angioplasty with stent placement is possible if restenosis develops. Your cardiologist will determine the best treatment approach based on the pattern of restenosis.
Q: When can I return to normal activities after stent placement?
A: Most patients can resume light activities within several days and gradually increase activity levels over weeks. Your cardiologist will provide personalized recommendations.
Q: Do I need to take medications forever after stent placement?
A: Dual antiplatelet therapy is typically required for at least one month to one year after stent placement. Long-term medications for blood pressure control, cholesterol management, and other cardiac conditions are usually continued indefinitely.
Q: What is the difference between emergency and planned angioplasty?
A: Emergency angioplasty is performed during acute coronary syndromes to restore blood flow quickly, while planned angioplasty is scheduled for chronic coronary artery disease causing symptoms uncontrolled by medications.
References
- Angioplasty and Stent Placement – Heart — MedlinePlus, National Library of Medicine. Accessed 2025. https://medlineplus.gov/ency/article/007473.htm
- Angioplasty and Vascular Stenting — Radiological Society of North America. Accessed 2025. https://www.radiologyinfo.org/en/info/angioplasty
- Coronary Angioplasty and Stents — Mayo Clinic. Accessed 2025. https://www.mayoclinic.org/tests-procedures/coronary-angioplasty/about/pac-20384761
- Getting a Stent — National Heart, Lung, and Blood Institute, National Institutes of Health. Accessed 2025. https://www.nhlbi.nih.gov/health/stents/during
- Coronary Angioplasty and Stents — British Heart Foundation. Accessed 2025. https://www.bhf.org.uk/informationsupport/treatments/coronary-angioplasty-and-stents
- Angioplasty: Procedure, Types & Recovery — Cleveland Clinic. Accessed 2025. https://my.clevelandclinic.org/health/treatments/22060-angioplasty
Read full bio of medha deb











