Atherosclerosis: Symptoms, Causes & Treatment
Understanding atherosclerosis: Learn about plaque buildup, risk factors, and comprehensive treatment options for arterial disease.
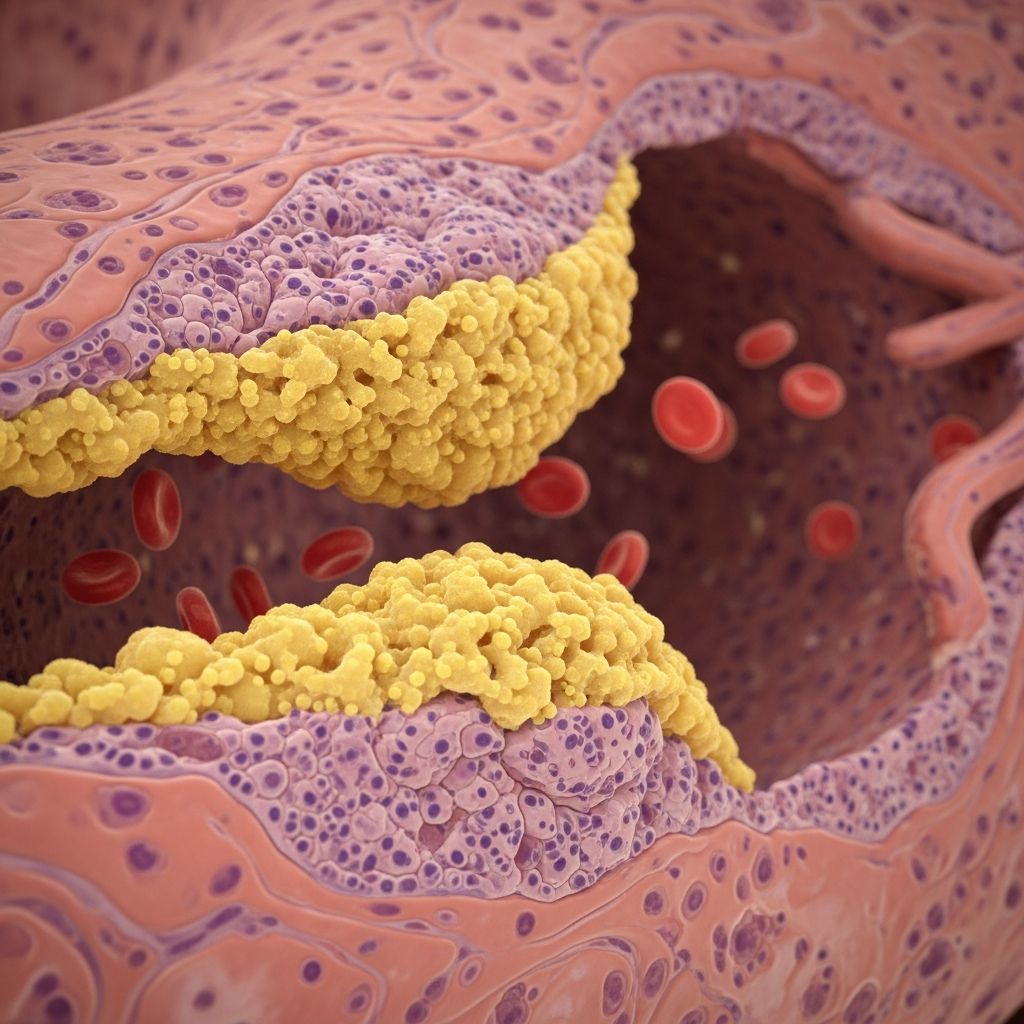
Atherosclerosis: Understanding Arterial Disease, Symptoms, and Treatment Options
What Is Atherosclerosis?
Atherosclerosis is a progressive disease characterized by the hardening of your arteries from plaque buildup gradually accumulating inside them. This plaque consists of fat, cholesterol, and other substances that accumulate along the inner walls of blood vessels.[10] As plaque deposits form and expand, they narrow the arterial passages, significantly limiting blood flow throughout your body. The condition develops silently over many years, and you may not experience any symptoms until serious complications develop, such as a heart attack or stroke.
The plaque in atherosclerosis is composed of cholesterol, waste products from cells, calcium deposits, and fibrin—a protein that aids in blood clotting. Over time, these deposits harden your arteries, making them less flexible and more prone to rupture or become completely blocked. This condition is remarkably common worldwide, and the complications resulting from plaque buildup, including heart attacks and strokes, represent the leading causes of death globally.
How Common Is Atherosclerosis?
Atherosclerosis affects millions of people worldwide. In America alone, approximately half of all people between the ages of 45 and 84 have atherosclerosis but are completely unaware of their condition, according to the U.S. National Institutes of Health. This widespread prevalence demonstrates why understanding the disease, its risk factors, and available treatments is essential for public health.
Understanding Atherosclerosis Symptoms
One of the most challenging aspects of atherosclerosis is that symptoms often don’t appear until an artery becomes significantly narrowed or blocked—typically when blockage exceeds 70%. Many individuals remain unaware they have plaque buildup until they experience a medical emergency such as a heart attack or stroke. This delayed symptom presentation makes regular health screenings and risk factor management crucial for early detection and prevention.
Symptoms by Location of Blockage
Atherosclerosis can affect different parts of your body, and symptoms vary depending on where the plaque buildup occurs.
Heart Involvement: When atherosclerosis affects the coronary arteries that supply blood to your heart, it causes coronary artery disease (CAD). Symptoms may include chest pain or discomfort (angina), shortness of breath, fatigue, and in severe cases, a heart attack. Sometimes, the first symptom of coronary artery disease is a heart attack itself.
Brain Involvement: Atherosclerosis in the carotid arteries that supply blood to your brain can lead to carotid artery disease. The first symptoms are typically a transient ischemic attack (TIA) or stroke. You may experience sudden weakness, numbness, difficulty speaking, or vision problems.
Kidney Involvement: With renal artery stenosis, which involves narrowing of the arteries that deliver blood to your kidneys, you may experience high blood pressure that’s difficult to control and declining kidney function.
Limb Involvement: When atherosclerosis affects the arteries in your arms and legs, it causes peripheral artery disease (PAD). Symptoms include leg pain or cramping during activity, weakness, numbness, or coldness in the affected limbs.
Understanding the Causes of Atherosclerosis
Researchers believe multiple factors contribute to the development of atherosclerosis. These causative factors typically damage the inner lining of your arteries, called the endothelium, and this damage usually occurs slowly and progressively over time. Understanding these contributing factors is essential for prevention and management.
Risk Factors You Cannot Change
Certain risk factors for atherosclerosis are fixed and cannot be modified through lifestyle changes or medications:
- Age (risk increases as you get older)
- Sex (men face higher risk at younger ages; women’s risk increases after menopause)
- Family history of heart disease or stroke
- Genetic predisposition to high cholesterol
Risk Factors You Can Manage
While you cannot change certain risk factors, many others can be managed through lifestyle modifications or medications:
- High cholesterol levels
- High blood pressure
- Smoking and tobacco use
- Diabetes or prediabetes
- Obesity or overweight status
- Physical inactivity and sedentary lifestyle
- Unhealthy diet high in saturated fats and sodium
- Excessive alcohol consumption
- Chronic stress
- Inflammation and certain inflammatory conditions
How Atherosclerosis Affects Your Body
Atherosclerosis doesn’t exclusively affect your heart—it can harm arteries throughout your entire body, leading to various symptoms from head to toe. When plaque accumulates in the coronary arteries that supply blood to your heart, you develop coronary artery disease, which causes most heart attacks. However, atherosclerosis can simultaneously develop in multiple locations, affecting your brain, kidneys, and limbs, creating a cascade of potential health complications.
As plaque grows along artery walls, it gradually narrows the opening (lumen) of the vessel, leaving less room for blood to flow. Additionally, plaque buildup raises your risk for blood clots. These clots can form on the plaque surface and block blood flow entirely, triggering medical emergencies including heart attacks or strokes. Research has also identified sex-based differences in how atherosclerosis develops—studies show that females may develop larger plaques in the aorta under similar conditions and are more likely to develop problems with how blood vessels expand and constrict.
Serious Complications of Atherosclerosis
The primary complication of atherosclerosis is a heart attack, which constitutes a medical emergency that can be fatal. During a heart attack, your heart muscle begins to die because it cannot receive sufficient blood flow and oxygen. Immediate medical attention is necessary to restore blood flow and preserve life.
Beyond heart attacks, atherosclerosis can cause several life-threatening complications:
- Stroke or transient ischemic attack (TIA)
- Sudden loss of blood flow to organs and tissues
- Aortic aneurysm (when plaque weakens artery walls)
- Aneurysm rupture and dissection (potentially fatal)
- Embolism (when plaque breaks away and blocks blood flow elsewhere)
Diagnosis and Treatment Approaches
When atherosclerosis is identified, healthcare providers typically employ a multi-faceted approach combining lifestyle modifications and medical interventions tailored to individual circumstances. Treatment focuses on improving blood flow, lowering the risk of serious complications, and managing symptoms effectively.
Lifestyle Modifications
The foundation of atherosclerosis treatment involves adopting sustainable lifestyle changes:
- Quit smoking and avoid tobacco products
- Follow a heart-healthy diet low in saturated fats and cholesterol
- Maintain regular physical activity and exercise
- Achieve and maintain a healthy weight
- Manage stress through relaxation techniques
- Limit alcohol consumption
- Control blood pressure and blood sugar levels
Medical Therapies
Healthcare providers often prescribe medications to manage atherosclerosis risk factors and prevent complications:
- Cholesterol-lowering medications (statins)
- Blood pressure medications
- Antithrombotic agents (blood thinners or antiplatelet drugs) to prevent clot formation
- Medications to manage diabetes or prediabetes
- Anti-inflammatory medications when appropriate
Advanced Interventions
In cases where blockages are severe, interventional procedures may be necessary to restore blood flow and prevent medical emergencies.
Prevention and Management Strategies
While you cannot always prevent atherosclerosis entirely, you can significantly slow disease progression and reduce your risk of serious complications through proactive management. Healthcare providers recommend working closely with your medical team to adopt manageable lifestyle changes and follow treatment plans.
For individuals diagnosed with atherosclerosis, especially aortic atherosclerosis, maintaining overall cardiovascular health becomes even more critical, as these patients face increased risk for developing additional conditions like coronary artery disease. Your provider can offer guidance on blood pressure control, cholesterol management, physical activity, dietary choices, and medication adherence.
Living with Atherosclerosis
While atherosclerosis is a serious condition, the encouraging news is that healthcare providers can identify risk factors and help manage the disease effectively. Early diagnosis combined with appropriate treatment makes it possible to manage your condition and maintain a long, healthy life. Working with your healthcare team to understand your individual risk factors, implementing recommended lifestyle changes, and maintaining medication compliance are essential components of successful atherosclerosis management.
Managing atherosclerosis is a personal journey that doesn’t require facing alone. By partnering with healthcare providers, telling family and friends about your health goals, and asking for their support, you create a comprehensive approach to protecting your cardiovascular health and preventing serious complications.
Frequently Asked Questions
Q: How quickly does atherosclerosis develop?
A: Atherosclerosis develops silently over many years. The process is typically gradual, and you may not notice any symptoms until an artery becomes significantly narrowed (typically over 70% blocked) or blocked entirely. This is why regular health screenings are important for early detection.
Q: Can atherosclerosis be reversed?
A: While plaque buildup cannot be completely reversed, appropriate treatment can slow disease progression, stabilize plaques, and reduce your risk of complications. Aggressive management of risk factors through lifestyle changes and medications has been shown to improve outcomes.
Q: What’s the difference between atherosclerosis and arteriosclerosis?
A: Arteriosclerosis is a general term for hardening of the arteries, which includes three types. Atherosclerosis is one specific type characterized by plaque buildup inside arteries. Other types involve thickening of artery walls and calcification.
Q: Are there differences in how atherosclerosis affects men and women?
A: Yes, research shows sex-based differences. Females may develop larger plaques in the aorta under similar conditions and are more likely to experience problems with blood vessel expansion and constriction. Women typically face increased atherosclerosis risk after menopause.
Q: What should I do if I have symptoms suggesting atherosclerosis?
A: Contact your healthcare provider immediately. If you experience symptoms of a heart attack (chest pain), stroke (sudden weakness or speech difficulties), or other severe symptoms, call 911 or your local emergency number. Early intervention can be life-saving.
Q: How is atherosclerosis diagnosed?
A: Diagnosis typically involves medical history evaluation, physical examination, and imaging tests such as ultrasound, CT scans, angiography, or ankle-brachial index testing for peripheral artery disease. Your provider will recommend appropriate testing based on your symptoms and risk factors.
References
- Coronary Artery Disease (CAD): Symptoms & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/16898-coronary-artery-disease
- Atherosclerosis of the Aorta: Causes, Symptoms & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/23431-atherosclerosis-of-aorta
- How Atherosclerosis Affects Your Body — Cleveland Clinic. 2025. https://my.clevelandclinic.org/watch/where-atherosclerosis-symptoms-can-appear
- Atherosclerosis: Symptoms, Causes & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/16753-atherosclerosis-arterial-disease
- Arteriosclerosis: Symptoms, Causes & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/24870-arteriosclerosis
- Cleveland Clinic researchers identify sex-based differences in blood vessel cells that contribute to heart disease — Cleveland Clinic Lerner Research Institute. 2025. https://www.lerner.ccf.org/news/article/?title=Cleveland+Clinic+researchers+identify+sex-based+differences+in+blood+vessel+cells+that+contribute+to+heart+disease
- New treatments for peripheral artery disease — Cleveland Clinic Journal of Medicine, 2020. https://www.ccjm.org/content/87/5_suppl_1/21
Read full bio of medha deb











