Back Pain: Causes, Symptoms, and Treatment Options
Comprehensive guide to understanding back pain, its causes, and effective treatment strategies.
Understanding Back Pain: A Comprehensive Guide
Back pain is one of the most common reasons people seek medical attention, ranking as the number two reason for physician visits in ambulatory settings. Whether acute or chronic, back pain can significantly impact quality of life and daily functioning. This comprehensive guide explores the causes, symptoms, diagnostic approaches, and evidence-based treatment strategies for managing back pain effectively.
What is Back Pain?
Back pain is discomfort or pain that originates in the back region, which can vary in intensity from mild to severe. It can be acute, lasting a few days to weeks, or chronic, persisting for months or longer. The back is a complex structure composed of bones, muscles, ligaments, and nerves, making it susceptible to various injuries and conditions that can cause pain and discomfort.
Common Causes of Back Pain
Understanding the underlying causes of back pain is essential for developing an effective treatment plan. The back contains several major structures that can be sources of pain:
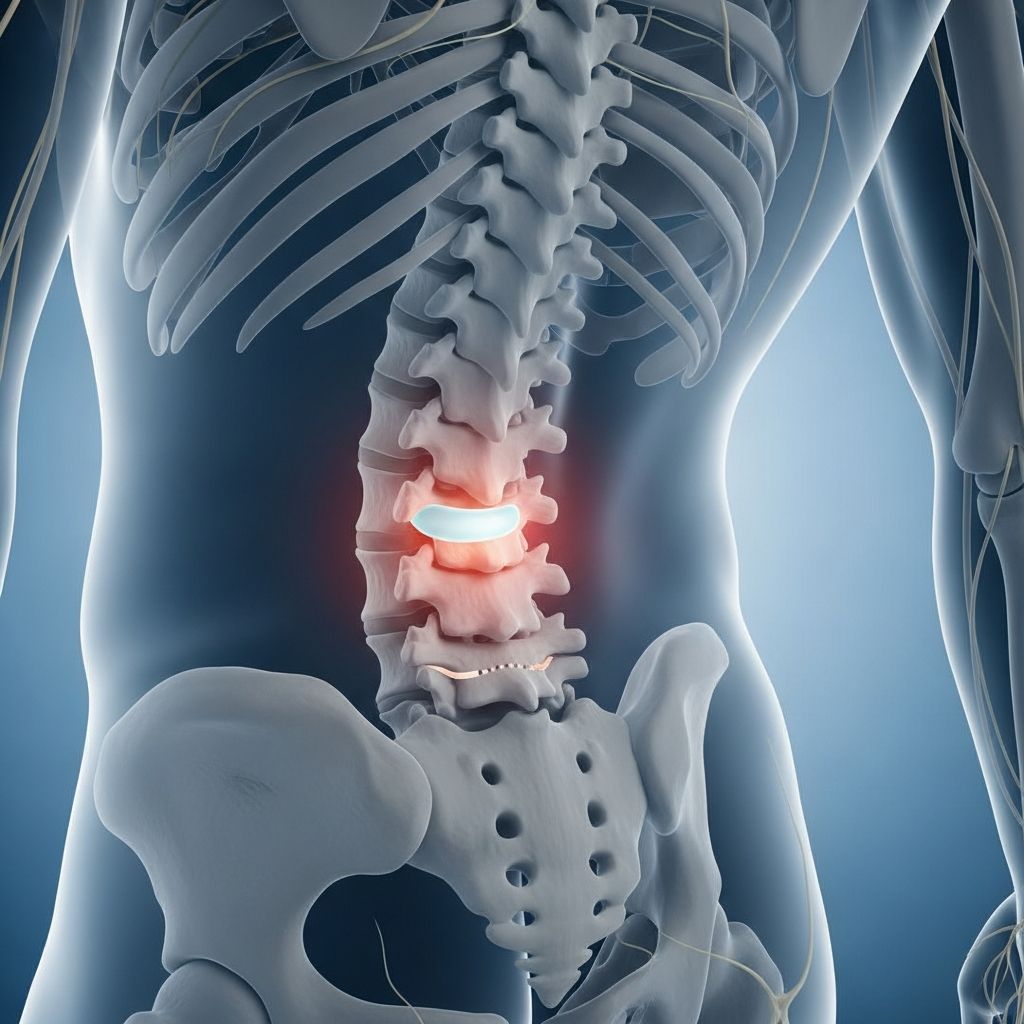
Lumbar Disc Herniation
One of the most common sources of lower back pain is lumbar disc herniation. This occurs when the soft inner core of a spinal disc protrudes through the tough outer layer, potentially irritating nearby nerves. When a herniated disc presses on a nerve root, it can cause pain that radiates down the leg, a condition known as sciatica. Research indicates that approximately eight out of ten people with disc herniation experience improvement within about ten weeks through conservative treatment, as the body naturally reabsorbs the protruding disc material through inflammatory processes.
Facet Joint Dysfunction
The facet joints are small joints located at the back of the spine that allow for movement and flexibility. These joints can become arthritic, inflamed, or misaligned, leading to localized back pain. Facet joint pain typically feels like pain in the lower back and may worsen with certain movements or positions.
Muscle Strain and Tension
Muscle strains are among the most common causes of acute back pain. Poor posture, sudden movements, lifting heavy objects incorrectly, or overuse can cause the muscles and ligaments in the back to become strained and inflamed. This type of pain is often characterized by muscle tenderness and stiffness.
Lifestyle Factors
Several lifestyle factors contribute to back pain development. Excess weight, particularly around the waist, puts additional strain on the lower back and spine. Sedentary lifestyles with inadequate physical activity weaken the supportive muscles around the spine, increasing vulnerability to injury. Poor ergonomics at work, improper sleeping positions, and high stress levels can also contribute to back pain.
Symptoms and When to Seek Help
Back pain can present with various symptoms depending on the underlying cause. Common symptoms include localized pain in the lower or upper back, stiffness, reduced range of motion, and muscle spasms. In cases of nerve involvement, pain may radiate to the legs or arms. Some individuals experience numbness, tingling, or weakness in the extremities.
You should contact a healthcare provider if back pain persists beyond a few days, worsens despite self-care measures, is accompanied by numbness or weakness in the legs, or follows an injury or accident. Immediate medical attention is warranted if pain is accompanied by loss of bowel or bladder control, severe weakness, or fever.
Diagnosis of Back Pain
Medical History and Physical Examination
A proper diagnosis begins with a detailed medical history where your healthcare provider will ask about the onset of pain, what activities make it worse, and what measures provide relief. The physician will perform a comprehensive physical examination, checking your strength and sensation, typically in the legs and arms. They will palpate structures in your lower back and spine, applying special maneuvers to reproduce your pain and identify its source.
Special diagnostic tests may be employed during the physical examination. The slump test and straight leg raise are commonly used to evaluate nerve involvement. These tests involve specific movements designed to stretch nerves exiting the lower back, helping to reproduce nerve or sciatica pain patterns.
Imaging Studies
Imaging tests such as X-rays, MRI scans, or CT scans may be ordered to visualize the spine’s structures and identify specific abnormalities. MRI is particularly useful for evaluating soft tissue structures, including discs, ligaments, and nerve roots. These imaging studies provide valuable information to confirm the diagnosis and guide treatment planning.
Treatment Options for Back Pain
Conservative Management
For most cases of back pain, conservative treatment measures are effective and should be tried first. Initial management typically involves short-term rest for a day or two, combined with over-the-counter anti-inflammatory medications such as ibuprofen or naproxen, or acetaminophen for pain relief. These medications can help reduce inflammation and provide pain relief.
Physical Therapy and Exercise
Physical therapy is a cornerstone of back pain treatment. A physical therapist will teach you specific back exercises designed to strengthen the supporting muscles around the spine and improve flexibility. Regular exercise helps restore normal function and prevents future episodes of pain. Back strengthening and stretching exercises should be performed consistently, ideally multiple times per week. Exercises focus on core strengthening, which provides crucial support for the spine and helps maintain proper posture.
Medications
Several types of medications can be used to manage back pain. Non-steroidal anti-inflammatory drugs (NSAIDs) reduce both inflammation and pain. Prescription medications may be recommended for more severe pain, including stronger analgesics or muscle relaxants to reduce muscle spasms and tension. These medications should be used under medical supervision and in conjunction with other treatment modalities.
Stress Reduction Techniques
Stress and emotional tension often exacerbate back pain by increasing muscle tension and reducing pain tolerance. Implementing stress reduction techniques such as deep breathing exercises, meditation, mindfulness, progressive muscle relaxation, and yoga can help improve pain control. These complementary approaches support overall well-being and enhance the effectiveness of other treatment strategies.
Injection Therapies
When conservative measures provide insufficient relief, injection therapies offer targeted treatment options:
Trigger Point Injections: These are among the least invasive injection options and are typically used for tight, sore muscles. Medications are injected directly into trigger points to reduce muscle tension and pain.
Facet Joint Blocks and Ablations: These injections target pain originating from the spinal facet joints. Facet blocks provide diagnostic and therapeutic benefits by reducing joint-related pain, while radiofrequency ablation can provide longer-lasting relief by disrupting pain signals from these joints.
Epidural Steroid Injections: These injections deliver anti-inflammatory medication directly into the epidural space around irritated nerve roots. They are particularly effective for nerve-related pain such as sciatica and can help reduce inflammation when there is narrowing around a nerve root.
Complementary and Alternative Treatments
Various complementary approaches may provide benefit for back pain management. Physical modalities such as chiropractic care, massage therapy, and acupuncture have been used traditionally and are offered at many medical centers including Johns Hopkins. While evidence varies for different approaches, many patients report symptomatic relief. These options are often considered alongside conventional treatment strategies based on individual patient preferences and evidence-based medicine recommendations.
Surgical Intervention
Surgery is considered when conservative treatments have failed to provide relief, typically after several weeks to months of non-surgical management. The need for surgery is determined based on the specific diagnosis, severity of symptoms, and neurological findings. Common surgical procedures address structural problems such as severe disc herniations, spinal stenosis, or instability. Your spine specialist will discuss the risks and benefits of surgical options specific to your condition.
Prevention Strategies
Preventing back pain is often more effective than treating it after it occurs. Key prevention strategies include:
- Maintain a healthy weight, particularly avoiding excess weight around the waist, which puts strain on the lower back.
- Practice good posture throughout the day, especially when sitting at a desk or using computers.
- Use proper body mechanics when lifting, bending, or carrying objects.
- Perform regular back strengthening and stretching exercises to maintain muscular support for the spine.
- Stay physically active with regular cardiovascular exercise and strength training.
- Manage stress effectively through relaxation techniques, exercise, or counseling.
- Ensure proper ergonomics at your workplace and while sleeping, using supportive pillows and mattresses.
Working with Your Healthcare Team
A multidisciplinary approach to back pain management often provides the best outcomes. This may involve collaboration between primary care physicians, pain management specialists, physical medicine and rehabilitation doctors, physical therapists, and orthopedic or neurosurgeons when necessary. Johns Hopkins Medicine’s Musculoskeletal Center exemplifies this comprehensive approach, with specialists trained to identify correct diagnoses and develop personalized treatment plans for each patient.
When consulting with your healthcare provider about back pain, be specific about describing your symptoms, including when the pain started, what makes it worse, and what provides relief. This information helps your doctor understand what strategies you have already tried and what new interventions might be beneficial. A thorough physical examination is crucial for determining the underlying cause of your pain and directing appropriate treatment.
Frequently Asked Questions
Q: How long does back pain typically last?
A: Acute back pain often resolves within a few days to weeks with conservative treatment. Many people with disc herniations experience significant improvement within ten weeks as the body naturally heals. Chronic back pain lasting more than three months may require more comprehensive management strategies.
Q: Do I need imaging tests for back pain?
A: Not all cases of back pain require imaging. A thorough medical history and physical examination are often sufficient to initiate treatment. Imaging studies such as MRI or X-rays are typically ordered when symptoms persist, neurological findings are present, or the diagnosis is unclear.
Q: Is surgery necessary for back pain?
A: Most cases of back pain can be managed successfully with conservative treatments including physical therapy, medications, and lifestyle modifications. Surgery is reserved for cases that have not responded to conservative treatment over several weeks to months, or when there are specific indications such as progressive neurological deficits or severe structural abnormalities.
Q: Can exercise worsen back pain?
A: Improper exercise or too much activity too soon can exacerbate pain. However, appropriate physical therapy exercises specifically designed for your condition are beneficial and necessary for recovery. Always consult with a physical therapist or physician to ensure exercises are appropriate for your specific situation.
Q: What role does stress play in back pain?
A: Stress increases muscle tension and can lower pain tolerance, exacerbating back pain symptoms. Stress reduction techniques including relaxation exercises, meditation, and physical activity can help improve pain control and overall well-being.
References
- Get Your Lower Back Pain under Control—and Get on with Life — Johns Hopkins University Press. 2012. https://www.press.jhu.edu/books/title/10099/get-your-lower-back-pain-under-control-and-get-life
- Back Pain Causes and Treatments Webinar — Johns Hopkins Medicine. 2022-06-07. https://www.hopkinsmedicine.org/musculoskeletal-center/
- Treatment Options for Back and Neck Pain — Johns Hopkins Medicine. 2020-10-01. https://www.hopkinsmedicine.org/musculoskeletal-center/
- Back Pain Monday — Johns Hopkins Public Health. 2012-02-20. https://publichealth.jhu.edu/2012/healthy-monday-2012/02202012_back-pain
- Musculoskeletal Health and Spine Care — Johns Hopkins Medicine Department of Physical Medicine and Rehabilitation. 2024. https://www.hopkinsmedicine.org/
Read full bio of medha deb











