Benign Prostatic Hyperplasia: Causes, Symptoms & Treatment
Understanding BPH: Comprehensive guide to enlarged prostate symptoms, diagnosis, and treatment options.
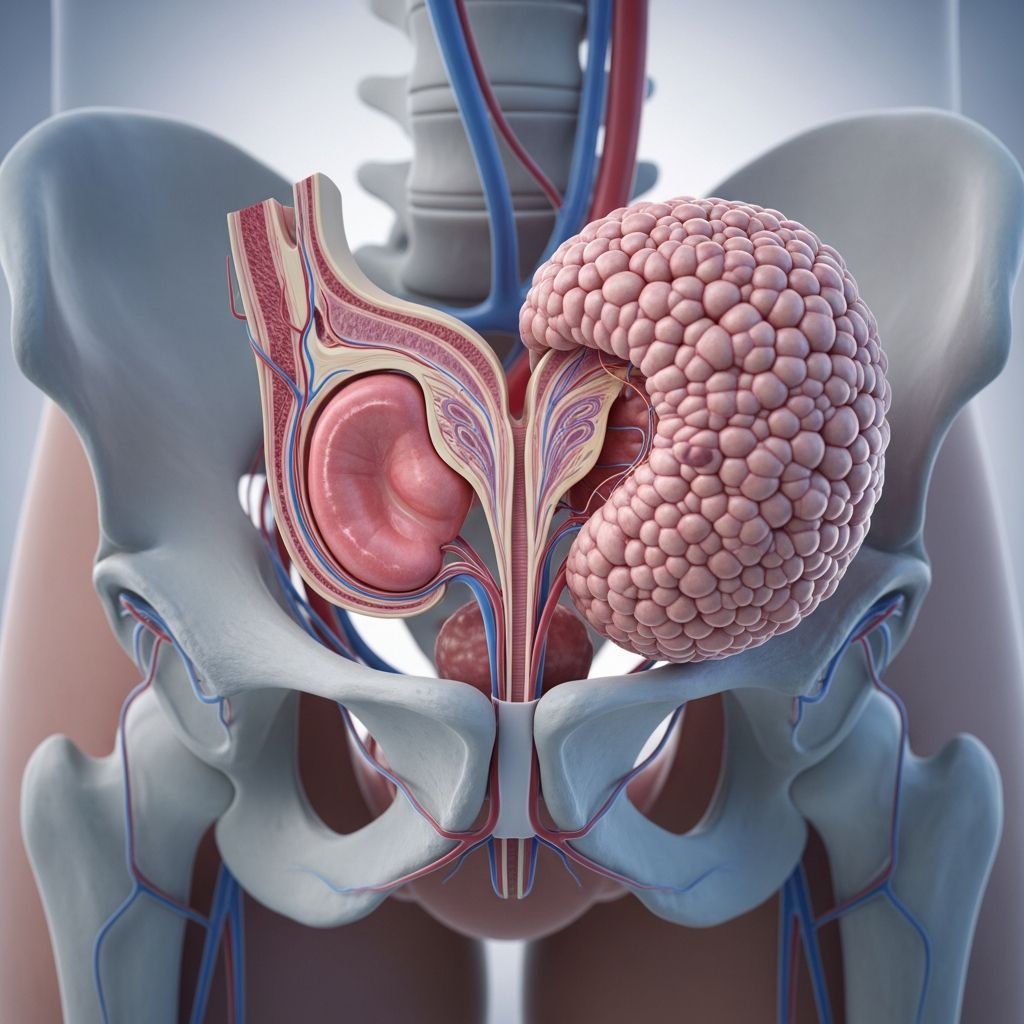
What is Benign Prostatic Hyperplasia?
Benign prostatic hyperplasia (BPH), commonly known as an enlarged prostate, is a condition in which the prostate gland grows larger over time. The prostate is a small gland located below the bladder that produces fluid for semen. As men age, the prostate naturally tends to enlarge, and this growth can compress the urethra—the tube through which urine flows from the bladder. This compression can lead to various urinary symptoms and affect quality of life. BPH is not cancer and does not increase the risk of prostate cancer, though the two conditions can coexist.
The development of BPH is characterized by stromal and epithelial cell proliferation in the prostate transition zone, which surrounds the urethra. This growth leads to urethral compression and bladder outflow obstruction, which can result in lower urinary tract symptoms, urinary retention, or infections due to incomplete bladder emptying.
Understanding the Prostate Gland
The prostate gland is a vital component of the male reproductive system. It produces seminal fluid that nourishes and transports sperm. The gland is roughly the size of a walnut in younger men but can grow significantly with age. The prostate surrounds the urethra, making it critical to urinary function. When the prostate enlarges, it can obstruct urine flow, leading to the symptoms associated with BPH.
Symptoms of Benign Prostatic Hyperplasia
BPH symptoms vary widely among men and may develop gradually over time. Some men experience significant symptoms, while others with larger prostates may have minimal discomfort. Common symptoms include:
- Frequent urination, particularly during the day
- Urgency to urinate, sometimes accompanied by difficulty delaying urination
- Weak or interrupted urine stream
- Difficulty starting urination
- Nocturia (excessive urination at night)
- Feeling of incomplete bladder emptying
- Post-void dribbling (leaking after urination)
Less common but more serious symptoms include urinary tract infections, inability to urinate, and blood in the urine. The symptoms of BPH tend to slowly worsen over time, though in some cases they may remain stable or even improve. Importantly, the size of the prostate does not always correlate with symptom severity—some men with modestly enlarged prostates experience severe symptoms, while others with significantly enlarged glands may have minimal problems.
Causes and Risk Factors
The exact cause of BPH remains not completely understood, but age and hormones play significant roles. Key risk factors include:
- Age: BPH primarily affects older men, becoming increasingly common after age 50
- Family History: Men with a family history of BPH are at higher risk
- Hormonal Changes: The male hormone testosterone and its conversion to dihydrotestosterone (DHT) appear to stimulate prostate growth
- Medical Conditions: Certain health conditions may increase risk
- Lifestyle Factors: Obesity and lack of physical activity may contribute to BPH development
Diagnosis of BPH
Your doctor will diagnose an enlarged prostate after a detailed examination to rule out other possible causes of lower urinary tract symptoms. The diagnostic process typically includes:
Medical History and Symptom Assessment: Your healthcare provider will ask about your symptoms, how often they occur, and how much they affect your daily life. The International Prostate Symptom Score (IPSS) or American Urological Association (AUA) symptom score helps quantify symptom severity.
Physical Examination: A digital rectal examination (DRE) allows your doctor to feel the prostate and assess its size and consistency.
Urinalysis: A urine test can detect signs of infection or other abnormalities.
Prostate-Specific Antigen (PSA) Test: A blood test measuring PSA levels may be performed, though elevated PSA can result from BPH, infection, or prostate cancer.
Uroflow Study: This test measures the force and amount of urine flow.
Post-Void Residual (PVR) Measurement: Ultrasound or catheterization determines how much urine remains in the bladder after urination.
Potential Complications
While BPH itself is not life-threatening, untreated or poorly managed disease can lead to complications:
- Urinary Tract Infections: Incomplete bladder emptying increases infection risk
- Urinary Retention: Inability to urinate can require catheterization
- Bladder Stones: These form from concentrated urine in the bladder
- Bladder Damage: A chronically overfull bladder can stretch and weaken, reducing its ability to contract and empty completely
- Kidney Damage: Severe, prolonged obstruction may affect kidney function
Treatment Options for BPH
Treatment approaches range from watchful waiting to medications and surgical interventions. The choice depends on symptom severity, prostate size, other health conditions, and patient preference.
Watchful Waiting
For mild symptoms that don’t significantly impact quality of life, watchful waiting may be appropriate. Regular monitoring through follow-up exams ensures symptoms aren’t worsening.
Medical Therapy
Alpha-Blockers: These medications relax smooth muscle in the bladder neck and prostate, making urination easier. Common alpha-blockers include alfuzosin (Uroxatral), doxazosin (Cardura), tamsulosin (Flomax), silodosin (Rapaflo), and terazosin. They often work quickly, particularly in men with smaller prostates. Side effects may include dizziness and retrograde ejaculation (semen flowing backward into the bladder rather than out through the penis).
5-Alpha Reductase Inhibitors: These medications shrink the prostate by blocking hormone changes that cause growth. Examples include finasteride (Proscar) and dutasteride (Avodart). They can take up to six months to achieve maximum effectiveness and may cause sexual side effects, including erectile dysfunction and decreased libido. These medications also decrease prostate-specific antigen (PSA) values, potentially delaying prostate cancer diagnosis.
Phosphodiesterase-5 Inhibitors: Medications like tadalafil (Cialis) can improve lower urinary tract symptoms and erectile dysfunction.
Combination Therapy: Combining alpha-blockers with 5-alpha reductase inhibitors is more effective than either medication alone for certain patients, though combination therapy increases the risk of adverse effects.
Surgical and Minimally Invasive Procedures
Transurethral Resection of the Prostate (TURP): TURP is the gold standard surgical treatment for average-sized prostates (30 mL to 80 mL) with symptoms uncontrolled by medication. An instrument called a resectoscope is inserted through the urethra, and excess prostate tissue is removed using an electric loop. TURP is highly effective but carries risks including bleeding, infection, urinary incontinence, and sexual dysfunction.
Laser Therapy: High-energy lasers destroy or remove overgrown prostate tissue. Laser procedures have lower risks of side effects than traditional TURP. Options include:
- Photoselective Vaporization of the Prostate (PVP): Ablates prostate tissue blocking urine flow
- Holmium Laser Ablation: Another ablative approach that may cause irritating post-operative symptoms
- Holmium Laser Enucleation of the Prostate (HoLEP): Removes tissue completely, preventing regrowth and allowing tissue analysis for cancer
Transurethral Microwave Thermotherapy (TUMT): A special catheter is placed through the urethra into the prostate area. Microwave energy destroys the inner prostate tissue, shrinking the gland and easing urine flow. Results may be gradual, and the procedure is typically reserved for small prostates.
Water Vapor Thermal Therapy (WVTT): A device placed in the urethra converts water into steam that wears away excess prostate tissue. WVTT is less likely to cause sexual side effects compared to many traditional surgical treatments.
Prostate Lift: Special tags compress the sides of the prostate to improve urine flow. This approach is suitable when the prostate’s middle section doesn’t obstruct urine flow and is less likely to cause sexual dysfunction.
Robotic Waterjet Treatment: Imaging and robotic tools guide a device into the urethra that releases powerful water jets to remove excess tissue, easing symptoms.
Prostate Artery Embolization (PAE): This minimally invasive procedure blocks blood supply to chosen areas of the prostate, causing it to shrink. Evidence suggests both short-term and long-term benefits, including improved urinary symptoms for certain BPH patients.
Possible Side Effects of Treatment
Different treatments carry varying risks. Common side effects across procedures include:
- Retrograde ejaculation
- Urinary incontinence (leaking urine)
- Urinary tract infections
- Bleeding
- Erectile dysfunction
When Surgery May Not Be Appropriate
Surgery or other procedures may not be suitable if you have:
- An untreated urinary tract infection
- Urethral stricture disease
- A history of prostate radiation therapy or urinary tract surgery
- A neurological disorder, such as Parkinson’s disease or multiple sclerosis
Frequently Asked Questions
Q: Is BPH the same as prostate cancer?
A: No. Benign prostatic hyperplasia is not cancer and does not increase your cancer risk, though both conditions can occur simultaneously. Regular screening is still important for prostate cancer detection.
Q: At what age does BPH typically develop?
A: BPH primarily affects men over 50, becoming increasingly common with advancing age. However, some younger men may experience symptoms.
Q: Can BPH symptoms improve without treatment?
A: Yes. In some men, BPH symptoms remain stable or even improve over time without treatment. Your healthcare provider can help determine if watchful waiting is appropriate for your situation.
Q: How long does it take for medications to work?
A: Alpha-blockers typically work quickly, often within days to weeks. 5-alpha reductase inhibitors can take up to six months to achieve maximum effectiveness.
Q: What are the sexual side effects of BPH treatment?
A: Depending on the treatment chosen, sexual side effects may include erectile dysfunction, decreased libido, and retrograde ejaculation (where semen enters the bladder rather than exiting through the urethra). Discuss these risks with your doctor before treatment.
Q: Will my symptoms return after surgery?
A: While most surgical procedures provide long-lasting relief, symptoms can recur in some cases. TURP has the highest success rate, though some procedures may need repetition.
Living with BPH
Managing BPH involves working closely with your healthcare provider to choose the most appropriate treatment based on your symptoms, prostate size, other health conditions, and personal preferences. Regular follow-up appointments help monitor your condition and adjust treatment as needed. Lifestyle modifications, such as limiting fluid intake before bedtime, reducing caffeine and alcohol consumption, and practicing pelvic floor exercises, can help manage symptoms. Always discuss any new or worsening symptoms with your doctor promptly.
References
- Benign Prostatic Hyperplasia (BPH) — Diagnosis and Treatment — Mayo Clinic. 2023-06-15. https://www.mayoclinic.org/diseases-conditions/benign-prostatic-hyperplasia/diagnosis-treatment/drc-20370093
- Benign Prostatic Hyperplasia — StatPearls, National Center for Biotechnology Information (NCBI). 2024. https://www.ncbi.nlm.nih.gov/books/NBK558920/
- Benign Prostatic Hyperplasia: Rapid Evidence Review — American Academy of Family Physicians (AAFP). 2023-06-00. https://www.aafp.org/pubs/afp/issues/2023/0600/benign-prostatic-hyperplasia.html
- Benign Prostatic Hyperplasia (BPH) — Symptoms and Causes — Mayo Clinic. 2023-06-15. https://www.mayoclinic.org/diseases-conditions/benign-prostatic-hyperplasia/symptoms-causes/syc-20370087
- Enlarged Prostate or Benign Prostatic Hyperplasia (BPH) — Society of Interventional Radiology (SIR). https://www.sirweb.org/for-patients/conditions-and-treatments/enlarged-prostate/
Read full bio of medha deb











