Bladder and Bowel Dysfunction: Causes, Symptoms & Treatment
Comprehensive guide to understanding bladder and bowel dysfunction, its causes, symptoms, and effective treatment options.
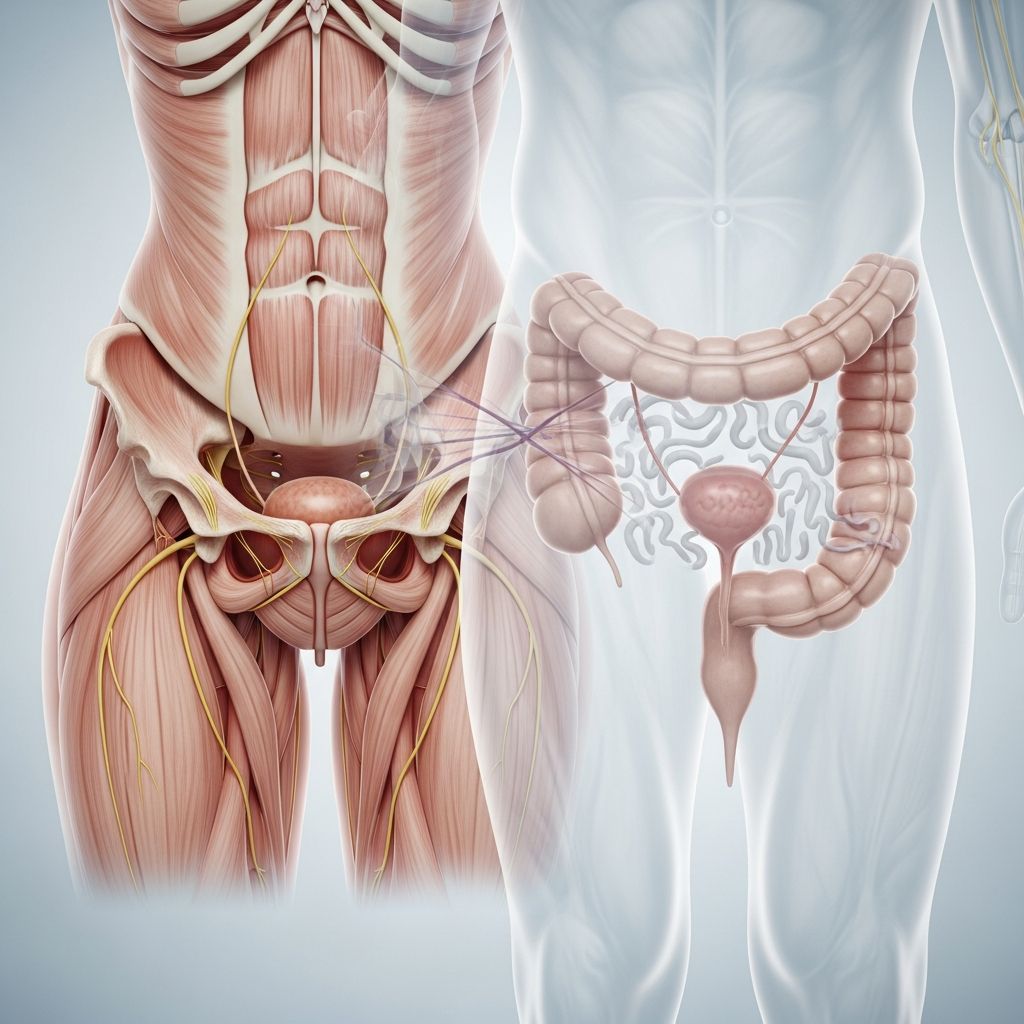
Understanding Bladder and Bowel Dysfunction
Bladder and bowel dysfunction encompasses a range of conditions that affect the normal functioning of the urinary and digestive systems. These disorders involve difficulties with storage, emptying, or control of urine or feces, significantly impacting daily life and overall well-being. Common manifestations include urinary incontinence, overactive bladder, fecal incontinence, and chronic constipation. While these conditions can be distressing and affect quality of life, various effective treatment approaches are available to help patients regain control and improve their symptoms.
What Are Bladder and Bowel Dysfunction?
Bladder and bowel dysfunction refers to a collection of conditions affecting the urinary and digestive systems’ ability to function normally. These conditions can involve issues with storage, emptying, or control of bodily waste. The pelvic floor muscles, which support the bladder, bowel, and reproductive organs, play a crucial role in maintaining continence and proper function. When these muscles become weakened or overactive, they can lead to various dysfunctions that interfere with daily activities and social engagement.
The bladder serves as a storage organ for urine, while the bowel manages fecal matter. Both systems rely on complex coordination between muscles, nerves, and the brain. When this coordination is disrupted, dysfunction can occur in various forms.
Common Types of Bladder and Bowel Dysfunction
Several distinct types of dysfunction can affect bladder and bowel function:
Urinary Incontinence: This condition involves involuntary leakage of urine and can occur during physical activity, while sneezing or coughing, or without warning. It affects millions of people worldwide and can significantly impact quality of life.
Overactive Bladder: Characterized by sudden, involuntary contractions of the bladder muscle, overactive bladder causes frequent and urgent urination, often accompanied by nighttime voiding episodes.
Fecal Incontinence: This involves the inability to control bowel movements, resulting in unintentional leakage of stool. It can range from occasional minor leakage to complete loss of bowel control.
Chronic Constipation: Difficulty passing stools or infrequent bowel movements can occur due to weak pelvic floor muscles, dehydration, dietary factors, or neurological issues.
Neurogenic Bladder and Bowel: Resulting from nervous system damage or disease, these conditions interrupt electrical signals between the nervous system and bladder or bowel function, affecting control and emptying.
Causes of Bladder and Bowel Dysfunction
Bladder and bowel dysfunction can develop from various causes, ranging from lifestyle factors to underlying medical conditions. Understanding these causes is essential for effective treatment planning.
Pelvic Floor Dysfunction
Weak or overactive pelvic floor muscles represent one of the most common causes of bladder and bowel dysfunction. The pelvic floor is a group of muscles that support the bladder, bowel, and reproductive organs. When these muscles become weakened due to childbirth, aging, chronic straining, or excessive exercise, they lose their ability to effectively support these organs and maintain continence.
Neurological Conditions
Conditions affecting the nervous system, such as spinal cord injuries, multiple sclerosis, Parkinson’s disease, and stroke, can disrupt the communication between the brain and the muscles controlling the bladder and bowel. This disruption prevents proper coordination of muscle contractions and relaxation.
Aging
As people age, the muscles supporting the bladder and bowel naturally weaken. Additionally, hormonal changes, particularly declining estrogen levels in women after menopause, can contribute to weakening of the urethral tissues and increased dysfunction.
Pregnancy and Childbirth
During pregnancy, hormonal changes and increased weight can weaken pelvic floor muscles. The trauma of vaginal delivery can stretch and damage these muscles further, leading to temporary or long-term incontinence.
Medical Conditions
Various health conditions contribute to bladder and bowel dysfunction, including diabetes, obesity, chronic cough, urinary tract infections, constipation, and enlarged prostate gland in men. These conditions can affect muscle function or the nervous system’s ability to control these processes.
Lifestyle Factors
Certain lifestyle habits can increase the risk of dysfunction. These include excessive caffeine or alcohol consumption, smoking, prolonged sitting or standing, chronic straining during bowel movements, and inadequate fluid intake.
Symptoms of Bladder and Bowel Dysfunction
The symptoms of bladder and bowel dysfunction vary depending on the specific condition and its severity. Recognizing these symptoms is crucial for seeking appropriate medical attention.
Bladder Dysfunction Symptoms
Individuals with bladder dysfunction may experience frequent urination, urgent need to urinate, involuntary leakage of urine during physical activity or daily activities, inability to empty the bladder completely, and nighttime incontinence. Some patients report losing bladder control entirely or experiencing constant dripping.
Bowel Dysfunction Symptoms
Bowel dysfunction can manifest as loss of bowel control, chronic constipation, frequent bowel movements, difficulty controlling gas, or inability to control the urge to have a bowel movement. Some individuals experience incomplete bowel emptying or unpredictable bowel movements.
Diagnosis and Assessment
Proper diagnosis of bladder and bowel dysfunction requires a comprehensive evaluation by a healthcare professional. The diagnostic process typically includes a detailed medical history, physical examination, and specialized tests.
Medical History
Healthcare providers begin by asking about the onset and progression of symptoms, factors that worsen or improve symptoms, medication use, past medical conditions, and impact on daily activities and quality of life.
Physical Examination
A physical examination may include assessment of abdominal sensation, pelvic floor strength and coordination, and evaluation of the spine and nervous system function. For neurogenic bladder or bowel, assessment of reflexes and muscle tone is particularly important.
Specialized Tests
Urinalysis screens for urinary tract infections, which commonly cause bladder symptoms. Post-void residual testing measures how much urine remains in the bladder after urination. Urodynamic studies assess bladder function and pressure. Imaging studies such as ultrasound or MRI may evaluate structural abnormalities.
Treatment Options
Effective treatment for bladder and bowel dysfunction depends on the underlying cause, severity of symptoms, and individual patient factors. Multiple treatment approaches are available, ranging from conservative measures to advanced interventions.
Pelvic Floor Physical Therapy
Physical therapy focusing on the pelvic floor muscles represents one of the most effective and widely recommended treatments. Physical therapists use neuromuscular re-education to normalize the timing and frequency of urination or bowel movements and retrain the pelvic floor muscles. Manual techniques may improve muscle tone or scar mobility. Electrical stimulation and biofeedback help patients strengthen pelvic floor muscles and improve muscle control and coordination.
Lifestyle and Dietary Modifications
Healthcare providers often recommend lifestyle changes as first-line treatment. These include scheduled bathroom breaks at regular intervals, avoiding foods and drinks that irritate the bladder (such as caffeine, alcohol, and carbonated beverages), increasing dietary fiber to improve bowel function, maintaining adequate hydration, and performing exercises to strengthen bladder and bowel muscles. Weight management through healthy diet and exercise can significantly reduce bladder pressure and improve function.
Medications
Various medications can help manage bladder and bowel dysfunction symptoms. Anticholinergic medications reduce involuntary bladder contractions and can decrease urinary frequency and urgency. Medications to treat constipation include stool softeners, fiber supplements, and osmotic laxatives. Antibiotics treat urinary tract infections that may be causing symptoms. Your healthcare provider will select medications based on your specific condition and needs.
Bladder Training
Bladder training is a nonsurgical treatment that helps retrain the bladder to hold larger amounts of urine and reduces frequency and urgency. Patients keep a bladder diary recording voiding times and amounts, gradually increasing the time between bathroom visits. This technique has proven effective for many patients with overactive bladder symptoms.
Catheterization
For patients with significant emptying dysfunction, clean intermittent catheterization (CIC) involves inserting a thin tube through the urethra into the bladder several times daily to empty the bladder completely. This prevents urinary retention and reduces infection risk. Some patients require continuous catheterization through the urethra or through an opening in the abdominal wall.
Botulinum Toxin Injections
Botulinum toxin (Botox) injected into the bladder muscle helps reduce the frequency of involuntary bladder contractions. These injections provide symptom relief that typically lasts about six months, after which repeat injections may be necessary.
Nerve Stimulation Therapies
Sacral neuromodulation (SNS) therapy and percutaneous tibial nerve stimulation (PTNS) represent advanced treatment options. These techniques involve connecting devices to nerves affecting bladder or bowel control, with the devices sending electrical impulses to modify nerve signaling and improve control. These treatments are often used when medications and lifestyle changes cannot adequately manage symptoms.
Anal Irrigation
Anal irrigation is a conservative bowel management therapy particularly useful for constipation. Fluid is inserted through a catheter with an inflatable balloon to reduce constipation and assist in effective bowel emptying and management.
Surgical Interventions
When conservative treatments prove inadequate, surgical options may be considered. Bladder reconstructive surgery may resolve or improve bladder symptoms through various techniques including artificial sphincter creation, bladder bypass, increasing bladder capacity, or removing weakened sphincter sections. Bowel reconstruction surgery can address difficulties in bowel management. These procedures are performed by specialized surgeons and reserved for appropriate candidates.
When to Seek Medical Attention
Individuals should consult a healthcare provider if they experience persistent symptoms of bladder or bowel dysfunction affecting quality of life. Prompt evaluation is particularly important for new onset loss of control, recurrent urinary tract infections, inability to empty the bladder or bowel, or symptoms following injury or illness. Early intervention often leads to better outcomes and faster symptom improvement.
Living with Bladder and Bowel Dysfunction
While bladder and bowel dysfunction can be challenging, most individuals can successfully manage symptoms with appropriate treatment. Maintaining open communication with healthcare providers, consistently following treatment recommendations, and making lifestyle adjustments significantly improves outcomes. Many people experience substantial improvement in symptoms and quality of life through multimodal treatment approaches combining physical therapy, medications, behavioral modifications, and when necessary, advanced interventions.
Frequently Asked Questions
Q: Can bladder and bowel dysfunction be cured?
A: The answer depends on the underlying cause. Some causes can be resolved completely, while others require ongoing management. Many conditions improve significantly or resolve with appropriate treatment, though neurogenic bladder and bowel cannot be cured but can be effectively managed.
Q: How effective is physical therapy for bladder and bowel dysfunction?
A: Physical therapy focusing on pelvic floor muscles is highly effective for many bladder and bowel dysfunctions. Most patients experience significant improvement in function and quality of life through consistent physical therapy. The timeline for improvement varies, with some patients noticing changes within weeks while others require several months of consistent therapy.
Q: What should I avoid if I have bladder dysfunction?
A: Avoid caffeine, alcohol, carbonated beverages, and foods that irritate your bladder. Do not reduce fluid intake as this can lead to constipation and urinary tract infections. Avoid chronic straining and excessive heavy lifting that stresses the pelvic floor.
Q: How long does treatment typically take?
A: Treatment duration varies significantly depending on the condition’s cause and severity. Some patients see improvement within weeks, while others require months of consistent treatment. Your healthcare provider will monitor progress and adjust the treatment plan as needed.
Q: Are there non-invasive treatment options?
A: Yes, many non-invasive options exist including pelvic floor physical therapy, bladder training, dietary modifications, lifestyle changes, and medications. These conservative approaches successfully treat many cases of bladder and bowel dysfunction before more invasive interventions become necessary.
References
- Symptoms & Causes of Bladder Control Problems (Urinary Incontinence) — National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), U.S. Department of Health and Human Services. 2024. https://www.niddk.nih.gov/health-information/urologic-diseases/bladder-control-problems/symptoms-causes
- Neurogenic Bladder and Bowel Management — Mayo Clinic. 2024. https://www.mayoclinic.org/tests-procedures/neurogenic-bladder-bowel-management/about/pac-20394763
- Neurogenic Bladder: Causes, Symptoms & Management — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/15133-neurogenic-bladder
- Bowel and Bladder Dysfunction — ATI Physical Therapy. 2024. https://www.atipt.com/conditions/pelvic-pain/bowel-bladder-dysfunction/
- Bladder and Bowel Dysfunction (Adults) — Glencoe Regional Health. 2024. https://glencoehealth.org/our-care/service/physical-therapy/bladder-bowel-dysfunction-adults/
- Bladder and Bowel Problems — Multiple Sclerosis Association of America (MSAA). 2024. https://mymsaa.org/publications/motivator/summer-fall13/cover-story/bladder-bowel/
- Insights: Bladder and Bowel Dysfunction — Urology Care Foundation. 2022. https://www.urologyhealth.org/healthy-living/urologyhealth-extra/magazine-archives/winter-2022/insights-bladder-and-bowel-dysfunction
Read full bio of medha deb











