Blepharitis: Causes, Symptoms, and Treatment Guide
Complete guide to blepharitis: Understanding inflammation, diagnosis, and effective eyelid management strategies.
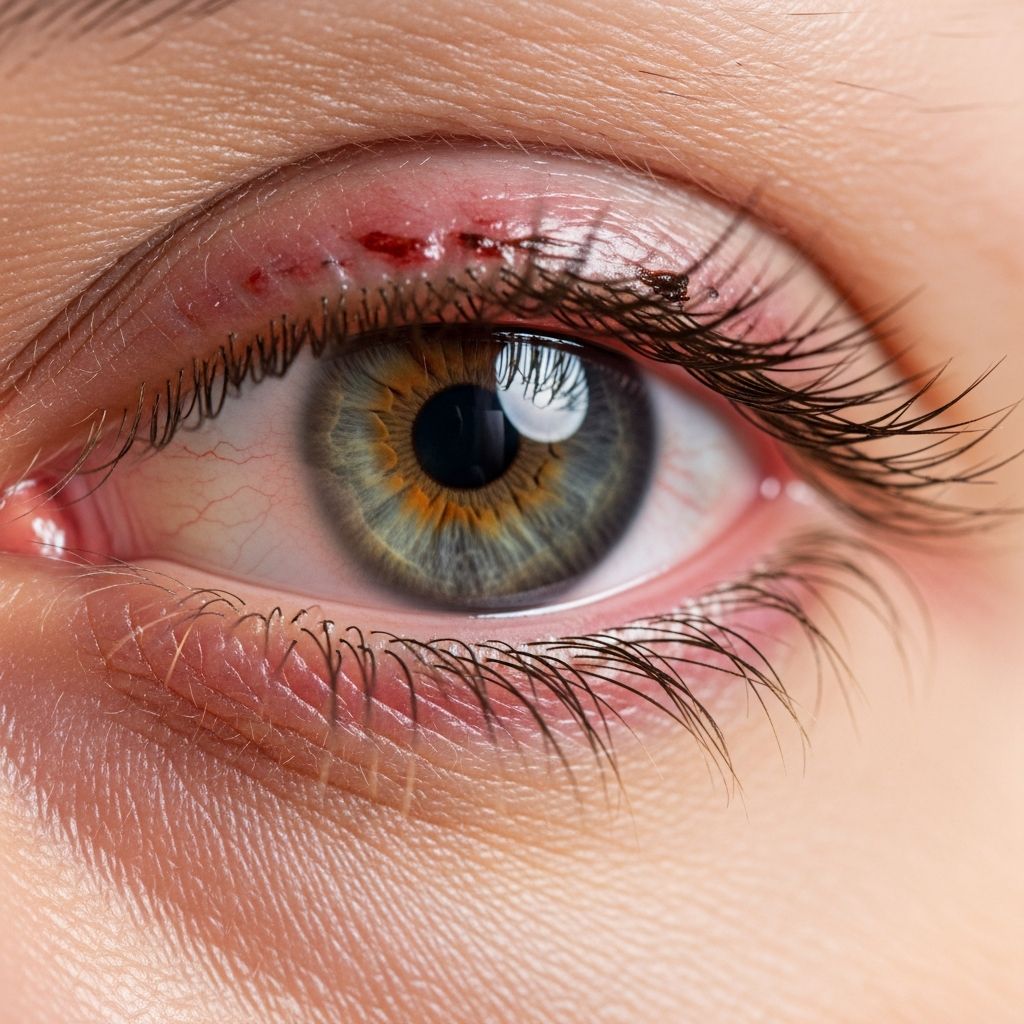
What is Blepharitis?
Blepharitis is an inflammatory condition affecting the eyelids, characterized by swelling, redness, and irritation of the eyelid margins. This chronic condition results from inflammation of the oily glands in the eyelids and is one of the most common eye conditions encountered in clinical practice. The inflammation can affect either the anterior portion of the eyelid (where eyelashes attach) or the posterior portion (involving the meibomian glands), and often both areas are affected simultaneously.
The condition typically develops when bacteria colonize the eyelid margins or when the meibomian glands become dysfunctional, leading to inadequate tear film stability. Although blepharitis is rarely a serious health threat, it is a chronic condition requiring consistent management and patient adherence to hygiene practices.
Types of Blepharitis
Blepharitis is classified into two main subtypes based on the affected eyelid structures:
- Anterior Blepharitis: Affects the anterior eyelid margin where the eyelashes are located. This type is often associated with bacterial colonization and results in crusting or characteristic “collarettes” at the base of the eyelashes.
- Posterior Blepharitis: Involves dysfunction of the meibomian glands located in the deeper portion of the eyelid. This type is characterized by meibomian gland dysfunction (MGD) and eyelid telangiectasia (small dilated blood vessels).
Most patients experience a combination of both anterior and posterior blepharitis, though one type may predominate. Accurately identifying the primary type is essential for developing targeted treatment strategies.
Causes and Risk Factors
While the exact etiology of blepharitis remains incompletely understood, multiple factors contribute to its development. The primary mechanisms involve bacterial colonization and inflammatory processes affecting the eyelid structures.
Primary Contributing Factors
- Bacterial Colonization: Bacteria, particularly Staphylococcus species, colonize the eyelid margins and meibomian glands, triggering inflammatory responses.
- Meibomian Gland Dysfunction: Obstruction or dysfunction of these oil-secreting glands compromises the lipid layer of the tear film, leading to instability and evaporative dry eye.
- Seborrheic Dermatitis: Individuals with dandruff or scalp dermatitis have increased susceptibility to blepharitis due to similar inflammatory processes affecting the eyelid skin.
- Ocular Rosacea: This vascular condition frequently coexists with blepharitis and shares similar inflammatory mechanisms.
- Allergic Responses: Some cases of blepharitis are triggered by allergic reactions affecting the eyelid tissues.
- Demodex Mites: Excessive proliferation of eyelash follicle mites can contribute to inflammation and symptoms.
Signs and Symptoms
Blepharitis presents with a variety of symptoms that often worsen throughout the day and may intensify upon waking.
Common Symptoms
- Chronic redness and swelling of the eyelid margins
- Burning sensation and ocular discomfort
- Itching and irritation of the eyelids
- Foreign body sensation in the eyes
- Crusting or sticky residue on eyelashes, particularly upon waking
- Thick scales or flaking at the eyelid edges
- Blurred or hazy vision, especially when tear film is compromised
- Watery or frothy tears
- Light sensitivity (photophobia)
- Frequent blinking and tearing
- Possible loss of eyelashes in severe cases
Symptoms often worsen during nighttime hours due to tear film stagnation and accumulation of inflammatory mediators during prolonged eyelid closure. Morning symptoms are typically most severe, with gradual improvement throughout the day.
Diagnosis
Accurate diagnosis of blepharitis requires a comprehensive clinical assessment combining patient history, physical examination, and diagnostic testing.
Diagnostic Approaches
Clinical Examination: Healthcare providers begin with a careful examination of the eyelids and eyes. The patient is instructed to blink fully and then maintain open eyes for 10 seconds while tear film integrity is assessed under cobalt blue light.
Slit-Lamp Biomicroscopy: This primary diagnostic method allows detailed visualization of the tear film, meibomian glands, and eyelid margins. The examination helps distinguish anterior blepharitis features (crusting and collarettes at the lash base) from other conditions affecting the eyelid skin.
Tear Break-Up Time (TBUT): A measurement of less than 10 seconds is typically considered abnormal and indicates tear film instability.
Laboratory Testing: When bacterial infection is suspected, an eyelid swab may be obtained to culture microorganisms and guide antibiotic selection. Microscopic examination of eyelashes can reveal excess Demodex mites.
Additional Considerations: If symptoms persist despite appropriate treatment in one eye, additional testing may be warranted to exclude eyelid skin cancer or systemic immune disorders.
Differential Diagnosis
Several conditions present with symptoms overlapping blepharitis, making differential diagnosis important for appropriate treatment.
- Ocular Rosacea: Shares meibomian gland dysfunction and eyelid telangiectasia features, making differentiation challenging.
- Seborrheic Dermatitis: Presents with oily scales on the eyelid that must be distinguished from bacterial crusting in anterior blepharitis.
- Contact Dermatitis: Allergic reactions to eye makeup or contact solutions can mimic blepharitis symptoms.
- Eyelid Skin Cancer: Persistent unilateral symptoms warrant investigation to exclude malignancy.
Treatment Options
Blepharitis management focuses on symptom relief and preventing exacerbations through a combination of hygiene practices and medications. Treatment should be individualized based on disease severity, subtype, and underlying contributing factors.
Self-Care Measures
Eyelid Hygiene: Daily eyelid cleansing forms the foundation of blepharitis management. This includes gentle cleaning of the eyelid margins to remove crusts and bacterial biofilms.
Warm Compresses: Applying warm compresses for 5-10 minutes helps soften eyelid crusts, improve meibomian gland secretion, and relieve discomfort. This should be performed daily, preferably in the morning.
Artificial Tears: Lubricating eye drops help manage dry eye symptoms associated with tear film instability.
Topical Medications
Antibiotic Eye Drops: Prescribed when bacterial infection is suspected or confirmed, antibiotic drops such as polymyxin B with trimethoprim (Polytrim) or fluoroquinolones provide direct antimicrobial action.
Antibiotic Ointments: Preparations containing erythromycin, bacitracin, or combination products like Polysporin provide sustained eyelid margin contact.
Anti-Inflammatory Medications: Steroid eyedrops or ointments effectively reduce inflammation in patients who do not respond to other therapies. Short courses of corticosteroids may be used for acute exacerbations.
Cyclosporine: This immunosuppressive medication (Restasis, Cequa) reduces inflammation and may be particularly useful when blepharitis is triggered by allergic responses.
Systemic Medications
Oral Antibiotics: When topical antibiotics prove insufficient, systemic antibiotics such as doxycycline or azithromycin are prescribed. These medications penetrate eyelid tissues effectively and provide sustained therapeutic levels.
Treatment of Underlying Conditions: Managing concurrent conditions such as rosacea, seborrheic dermatitis, or dandruff often improves blepharitis symptoms. Dermatological or systemic treatments targeting the primary condition may be necessary.
Management Strategy Table
| Severity Level | Primary Interventions | Medications | Duration |
|---|---|---|---|
| Mild | Daily eyelid hygiene, warm compresses, artificial tears | None typically required | Ongoing daily |
| Moderate | Enhanced hygiene, warm compresses | Topical antibiotics or anti-inflammatory drops | 2-4 weeks |
| Severe | Intensive hygiene protocol | Topical + oral antibiotics, steroids, cyclosporine | 4-12 weeks or longer |
Prognosis and Long-Term Management
While blepharitis is a chronic condition without definitive cure, the prognosis is generally favorable. Most patients respond well to appropriate treatment, though the condition is characterized by periods of exacerbation and remission.
Long-term success depends critically on patient adherence to daily hygiene practices and maintenance medications. Even with successful initial treatment, blepharitis typically requires ongoing attention to prevent recurrence and manage symptoms. Regular follow-up with eye care professionals helps monitor disease progression and adjust treatment plans as needed.
When to Seek Professional Help
- Symptoms persist despite home care measures for more than 2 weeks
- Severe pain, vision loss, or photophobia develops
- Unilateral symptoms suggestive of other conditions
- Signs of eyelash loss or eyelid scarring
- Suspected bacterial infection requiring culture
- Inadequate response to initial treatment
Frequently Asked Questions
Q: Is blepharitis contagious?
A: While blepharitis itself is not contagious, bacterial infections causing it could potentially spread through direct contact. Maintaining good eyelid hygiene and avoiding sharing eye care items reduces transmission risk.
Q: Can blepharitis cause permanent vision loss?
A: Uncomplicated blepharitis rarely causes permanent vision loss. However, chronic tear film instability may lead to refractive changes or hazy vision that typically improves with treatment.
Q: How long does blepharitis treatment take to work?
A: Improvement typically occurs within 1-2 weeks of consistent treatment, though complete resolution of symptoms may require 4-6 weeks or longer depending on severity and adherence.
Q: Can blepharitis be prevented?
A: While complete prevention is not always possible, maintaining excellent eyelid hygiene, avoiding eye irritants, managing underlying conditions like rosacea, and not sharing eye makeup reduce risk and severity.
Q: What is the difference between anterior and posterior blepharitis?
A: Anterior blepharitis affects the eyelash area and involves bacterial colonization, while posterior blepharitis involves meibomian gland dysfunction. Most patients have both types coexisting.
Q: Are there any natural remedies for blepharitis?
A: Warm compresses, proper eyelid hygiene, and gentle massage of the eyelid margins are evidence-based self-care approaches. However, medical supervision is recommended for optimal outcomes.
References
- Blepharitis — StatPearls, National Center for Biotechnology Information (NCBI). 2024. https://www.ncbi.nlm.nih.gov/books/NBK459305/
- Are There Treatments Available for Blepharitis? — Sierra Nevada Eye Center. 2024. https://www.nveyedoc.com/uncategorized/are-there-treatments-available-for-blepharitis/
- Blepharitis — Diagnosis & Treatment — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/blepharitis/diagnosis-treatment/drc-20370148
- Blepharitis (Eyelid Inflammation): Causes & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/10032-blepharitis
- Blepharitis — Healthdirect Australia. 2024. https://www.healthdirect.gov.au/blepharitis
- Blepharitis — Children’s Hospital of Philadelphia. 2024. https://www.chop.edu/conditions-diseases/blepharitis
- Blepharitis — Boston Children’s Hospital. 2024. https://www.childrenshospital.org/conditions-treatments/blepharitis
Read full bio of medha deb













