Boil: Causes, Symptoms, Treatment, And Prevention Guide
Comprehensive guide to boils: causes, symptoms, diagnosis, treatment, and prevention strategies for furunculosis.
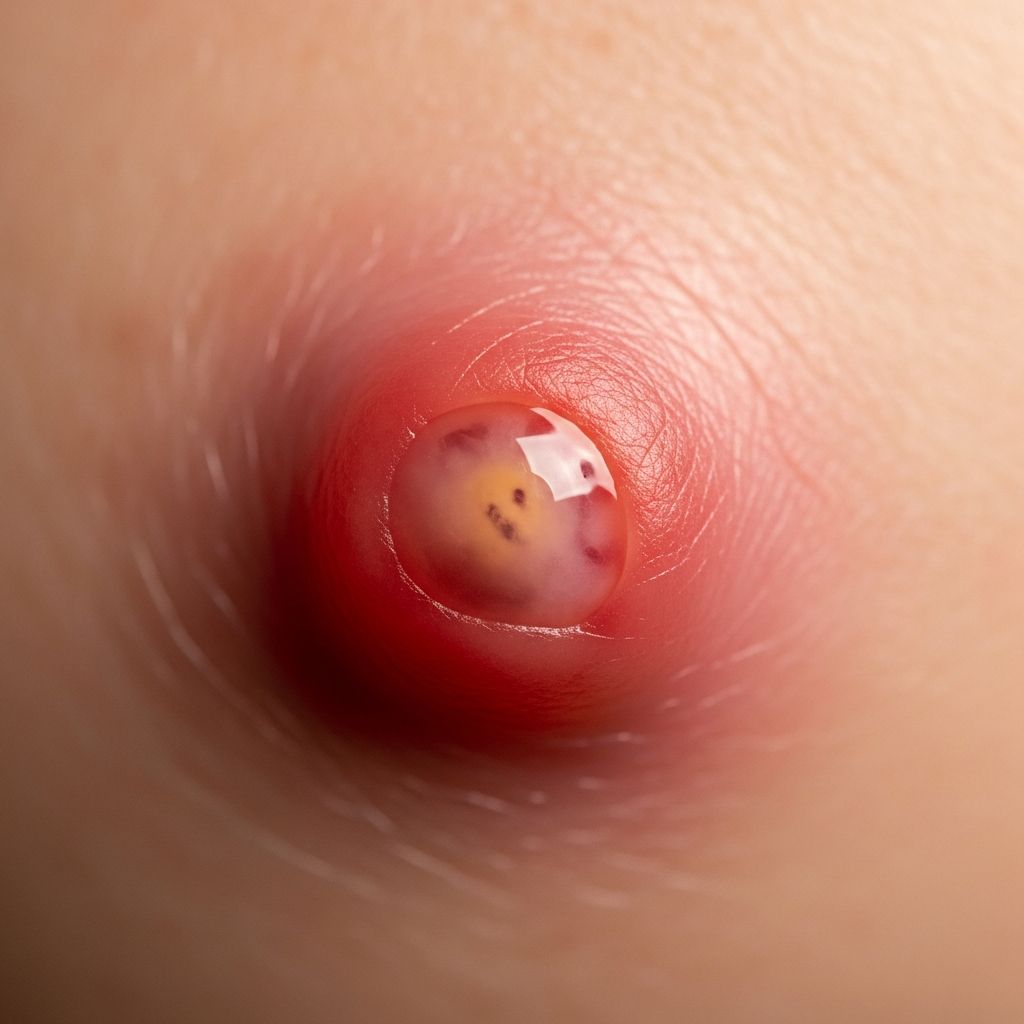
Boil
A
boil
, also known as afuruncle
, represents a deep bacterial infection centered on a hair follicle, manifesting as tender red nodules or pustules filled with pus. These common skin infections, primarily caused by *Staphylococcus aureus*, can occur singly or multiply asfurunculosis
, and require prompt recognition to prevent complications like carbuncles or systemic spread.What is a boil?
A boil (furuncle) constitutes a deep form of
bacterial folliculitis
, where infection penetrates beyond the superficial epidermis into the hair follicle and surrounding subcutaneous tissue. Unlike superficial folliculitis, which presents as itchy pustules, boils form painful, firm lumps that evolve into pus-filled abscesses.Boils typically arise from entry of bacteria through minor skin abrasions, blocked follicles, or friction sites. The most prevalent pathogen is
Staphylococcus aureus
(S. aureus), a gram-positive coccus colonizing the skin and nasal mucosa in up to 30% of healthy individuals. Less commonly, other bacteria or fungi contribute.When multiple adjacent boils coalesce, they form a
carbuncle
, a larger interconnected abscess with multiple drainage points, posing higher risks of scarring and systemic infection.Who gets boils?
Boils affect individuals across all ages, with higher incidence in adolescents, young adults, and those in communal living like athletes or military personnel due to close contact and sweating.
Key
risk factors
include:- Close skin contact (e.g., sports, households).
- Compromised skin barrier from friction, poor hygiene, or occlusion under tight clothing.
- Immunosuppression: diabetes mellitus, HIV, chemotherapy, or corticosteroid use impairs bacterial clearance.
- Obesity, which promotes skin folds and moisture retention.
- Carriage of S. aureus in the nose (anterior nares), axillae, or perineum.
Recurrent furunculosis suggests nasal colonization or underlying conditions like hyper-IgE syndrome, though most cases remain idiopathic.
What causes boils?
Boils result from bacterial invasion of the pilosebaceous unit.
Staphylococcus aureus
predominates, producing virulence factors like protein A, coagulase, and toxins that evade host immunity and form abscesses.Pathogenesis involves:
- Bacterial entry via microtrauma or follicular occlusion.
- Neutrophil recruitment forming pus (neutrophils, bacteria, debris).
- Inflammation mediated by cytokines, causing erythema, heat, and pain.
Predisposing factors encompass poor hygiene, diabetes (altering skin pH and immunity), and iron deficiency. Community-associated methicillin-resistant S. aureus (CA-MRSA) emerges in outbreaks, resistant to beta-lactams.
What are the symptoms of boils?
Boils evolve over 1-2 weeks:
- Early:** Tender, erythematous papule or nodule (0.5-3 cm) centered on a hair follicle, itchy or painful.
- Peak:** Swelling, induration, central yellow-white pustule; surrounding cellulitis possible.
- Resolution:** Spontaneous rupture with purulent discharge (creamy yellow), crusting, and healing (days to weeks), often leaving a scar.
Common sites: face, neck, axillae, buttocks, thighs, groin—friction-prone, moist areas. Nasal/auricular boils risk cavernous sinus thrombosis.
**Carbuncles** cause fever, malaise, extensive cellulitis. Systemic symptoms signal deeper infection.
Clinical appearance
Boils appear as dome-shaped, tender, red-purple nodules with a central hair and punctum. Size varies from pea-like to golf ball; surface fluctuant when mature. Surrounding skin hot, edematous; lymphangitis or fever indicates severity.
Carbuncles feature multiple pustules over a broad base (3-10 cm), draining via satellite sinuses. Differentiate from cysts (fluctuant, non-inflammatory), hidradenitis suppurativa (recurrent groin nodules), or pilonidal abscess.
Diagnosis
Diagnosis relies on characteristic morphology and history; swabs unnecessary for solitary boils.
For recurrent or atypical cases:
- Culture pus/swabs (nose, skin) to identify pathogen and sensitivities.
- Swab family contacts if outbreaks occur.
- Investigate diabetes (HbA1c), HIV, IgE levels.
Imaging (ultrasound) assesses deep extension; biopsy excludes malignancy (rare).
Management
Home care
Most small boils (<5 cm, no systemic signs) resolve with supportive measures:
- Clean with antiseptic soap (chlorhexidine).
- Warm compresses (saltwater-soaked cloth, 10-20 min, 4x/day) promote drainage, relieve pain.
- Loose dressings; avoid squeezing to prevent spread.
- Analgesia (paracetamol/ibuprofen).
Do not lance prematurely; natural pointing occurs in 7-10 days.
Medical treatment
Indications: facial/large boils, carbuncles, immunosuppression, no improvement in 48h, systemic symptoms.
| Condition | Treatment |
|---|---|
| Solitary boil | Incision & drainage (I&D) under LA once fluctuant; no antibiotics unless cellulitis. |
| Cellulitis/carbuncle | Flucloxacillin 500mg QDS 7d; MRSA: clindamycin/doxycycline. |
| Recurrent | Nasal mupirocin 2% TDS 5d + chlorhexidine washes x5d; eradicate carriage. |
Surgical I&D essential for abscesses; pack cavity. Hospitalization for sepsis.
Recurrent boils (furunculosis)
Affects 20-40% with one boil; screen for carriage (65% nasal S. aureus).
- Decolonization:** Mupirocin nasal ointment + antiseptic body washes (bleach baths 1:10 dilution weekly).
- Household screening/treatment.
- Prophylactic antibiotics (doxycycline 100mg OD 3m) if frequent.
Prevention of boils
Minimize recurrence through:
- Daily showers with antibacterial soap; dry skin folds.
- Avoid sharing towels/razors; cover cuts.
- Loose clothing; manage diabetes/weight.
- Prophylactic antiseptics for carriers.
Potential complications
Most heal uneventfully, but risks include:
- Scarring, hypertrophic/keloid.
- Cellulitis, bacteremia, sepsis (rare, 0.5-3%).
- Facial: cavernous sinus thrombosis.
- Recurrence (30%).
- MRSA infection.
Seek urgent care for fever, rapid spread, facial location.
Differential diagnosis
| Condition | Key Features |
|---|---|
| Carbuncle | Multiple interconnected boils. |
| Cyst | Fluctuant, non-tender unless infected. |
| Hidradenitis suppurativa | Recurrent groin/axillae nodules/sinuses. |
| Spider bite | Necrotic center, systemic illness. |
| Squamous cell carcinoma | Non-healing, irregular. |
Frequently asked questions
Can I pop a boil myself?
No—squeezing risks bacterial dissemination, worsening infection or scarring. Use warm compresses until it drains naturally.
When should I see a doctor for a boil?
Immediately if facial, >5cm, feverish, diabetic, or no improvement in 48h.
Are boils contagious?
Indirectly via shared items or pus contact; practice hygiene.
How long do boils last?
1-2 weeks with care; longer if untreated.
Can boils be prevented in children?
Yes, via hygiene, avoiding skin trauma.
References
- Everything to Know About Boils on the Skin — Healthgrades. 2023. https://resources.healthgrades.com/right-care/skin-hair-and-nails/boil
- Boils (furunculosis) — DermNet NZ. 2016-01-28. https://dermnetnz.org/topics/boil
- Boils PIL — British Association of Dermatologists. 2025-10. https://www.skinhealthinfo.org.uk/wp-content/uploads/2018/10/Boils-PIL-Oct-2025.pdf
- Boils, Carbuncles and Furunculosis — Patient.info. 2024. https://patient.info/skin-conditions/boils-carbuncles-and-furunculosis
- Boils, carbuncles, and staphylococcal carriage — NICE CKS. 2024-05. https://cks.nice.org.uk/topics/boils-carbuncles-staphylococcal-carriage/
Read full bio of Sneha Tete











