BPPV: Managing Positional Vertigo
Discover causes, symptoms, and effective treatments for benign paroxysmal positional vertigo to regain balance and stability.
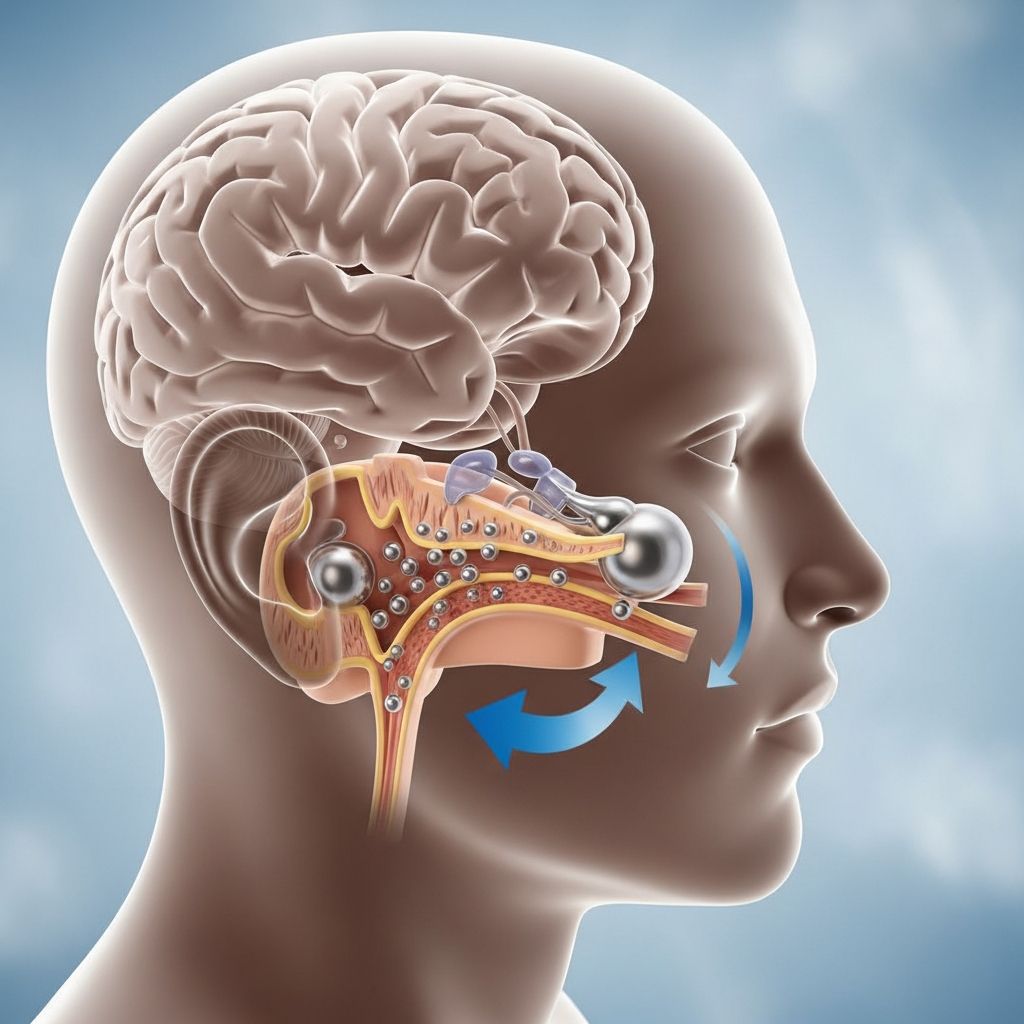
Benign paroxysmal positional vertigo (BPPV) stands as the primary culprit behind vertigo episodes in adults, particularly those over 65, manifesting as sudden, intense spinning sensations triggered by routine head movements.
Understanding the Inner Workings of BPPV
The inner ear plays a pivotal role in maintaining balance through its semicircular canals, fluid-filled structures that detect rotational movements. In BPPV, tiny calcium carbonate crystals known as otoconia dislodge from their normal position in the utricle and migrate into these canals. This displacement creates erroneous signals to the brain, simulating movement when none occurs, leading to disorienting vertigo.
Most cases involve the posterior semicircular canal, though lateral or anterior canals can be affected less frequently. These particles, or canaliths, float freely in the endolymph fluid, gravitating with head position changes and provoking symptoms.
Recognizing Key Symptoms
Sufferers experience brief vertigo attacks lasting under a minute, often accompanied by nausea, vomiting, or imbalance. Common provocations include rolling in bed, rising from a lying position, or tilting the head upward.
- Spinning sensation: The hallmark, feeling as if the room or body is whirling.
- Nausea and imbalance: Frequently co-occur, heightening fall risk.
- Nystagmus: Involuntary eye twitching during episodes, aiding diagnosis.
- Intermittent nature: Symptoms may remit for weeks or months before recurring.
Unlike persistent dizziness from other vestibular issues, BPPV episodes are strictly position-dependent and self-limiting.
Factors Contributing to Onset
Idiopathic BPPV lacks a clear trigger in many instances, especially with advancing age, which thins the otoconia matrix. Known precipitants include:
| Risk Factor | Description |
|---|---|
| Head trauma | Blows dislodge crystals; common after concussions. |
| Inner ear inflammation | Vestibular neuritis or labyrinthitis frees otoconia. |
| Migraines | Vascular changes may contribute. |
| Prolonged supine positioning | Post-surgery or bed rest allows particle migration. |
| Other associations | Vitamin D deficiency, osteoporosis, diabetes. |
Women face higher incidence, possibly due to hormonal influences on inner ear structures.
Diagnostic Approaches
Clinical history pinpoints positional triggers, distinguishing BPPV from central vertigo causes like strokes, which feature non-positional symptoms. The Dix-Hallpike test confirms diagnosis: the patient sits upright, then reclines with head turned 45 degrees off the exam table edge, eliciting nystagmus and vertigo if positive.
Variations like the supine roll test identify lateral canal involvement via bidirectional nystagmus. Imaging such as MRI is reserved for atypical cases to exclude tumors or strokes.
Proven Treatment Strategies
BPPV responds well to canalith repositioning maneuvers, non-invasive procedures relocating otoconia to safe zones.
Epley Maneuver
The gold standard for posterior canal BPPV involves sequential head positions guiding crystals out via gravity. Performed by clinicians or at home under guidance, success rates exceed 80% in one session.
- Sit on exam table, head turned 45 degrees toward affected side.
- Lie back rapidly with head hanging off, hold 30 seconds.
- Turn head 90 degrees opposite, hold 30 seconds.
- Roll body to opposite side, head toward floor, hold 30 seconds.
- Sit up slowly.
Post-maneuver, sleep semi-upright for 48 hours to prevent re-entry.
Other Maneuvers
- Semont Liberatory: Quicker for posterior canal, using rapid repositioning.
- Lempert Roll (BBQ): For lateral canal, sequential rolls clear horizontal canaliths.
Recurrent cases may require repeat sessions or surgical canal plugging in rare, refractory instances.
Lifestyle Adjustments and Prevention
Avoid triggers like rapid head turns during acute phases. Vestibular rehabilitation therapy strengthens compensatory mechanisms, reducing recurrence. Supplemental vitamin D addresses deficiencies linked to persistence.
Fall prevention is crucial: use assistive devices, improve home lighting, and practice balance exercises.
Potential Complications and Prognosis
Though benign, untreated BPPV elevates fall risks, especially in elderly patients, potentially causing fractures. Most resolve spontaneously within months, but maneuvers accelerate recovery and curb relapses, which affect up to 50% over five years.
Differentiate from mimicking conditions: Meniere’s involves hearing loss and longer episodes; vestibular neuritis causes constant vertigo.
Common Questions About BPPV
Can BPPV resolve without treatment?
Yes, many cases self-resolve as otoconia dissolve or resorb, though maneuvers hasten relief and prevent falls.
Is BPPV dangerous?
Rarely; it’s not life-threatening but increases imbalance-related injury risk.
How long do episodes last?
Typically 20-60 seconds per trigger, with symptom-free intervals varying widely.
Who is most at risk?
Adults over 60, women, and those with head injuries or inner ear disorders.
Can exercises cure BPPV at home?
Guided Epley or Brandt-Daroff exercises work for many, but consult a professional first to confirm diagnosis.
Brandt-Daroff Exercises for Home Management
For mild or recurrent BPPV, these habituate the system:
- Sit on bed edge.
- Lie to affected side, head tilted 45 degrees up, hold 30 seconds or until vertigo subsides.
- Sit up 30 seconds.
- Repeat to opposite side.
- Perform 5 cycles, 3x daily until symptom-free for 48 hours.
Evidence supports reduced recurrence with consistent practice.
In summary, BPPV, while disruptive, is highly manageable with targeted maneuvers and precautions, restoring normalcy for most patients swiftly.
References
- Benign paroxysmal positional vertigo (BPPV) — Better Health Channel, Victoria Government. 2023. https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/benign-paroxysmal-positional-vertigo-bppv
- Benign Paroxysmal Positional Vertigo — Merck Manuals. 2024. https://www.merckmanuals.com/home/ear-nose-and-throat-disorders/inner-ear-disorders/benign-paroxysmal-positional-vertigo
- Benign paroxysmal positional vertigo (BPPV) — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/vertigo/symptoms-causes/syc-20370055
- Benign positional vertigo — Penn Medicine. 2023. https://www.pennmedicine.org/conditions/benign-positional-vertigo
- Benign Paroxysmal Positional Vertigo (BPPV) — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/11858-benign-paroxysmal-positional-vertigo-bppv
- Benign Paroxysmal Positional Vertigo — NORD (rarediseases.org). 2023. https://rarediseases.org/rare-diseases/benign-paroxysmal-positional-vertigo/
- Benign Paroxysmal Positional Vertigo — StatPearls, NCBI Bookshelf. 2023-10-05. https://www.ncbi.nlm.nih.gov/books/NBK470308/
Read full bio of Sneha Tete