Brachial Plexus Injuries: Causes, Symptoms, and Treatment
Understanding brachial plexus injuries: comprehensive guide to causes, symptoms, diagnosis, and treatment options.
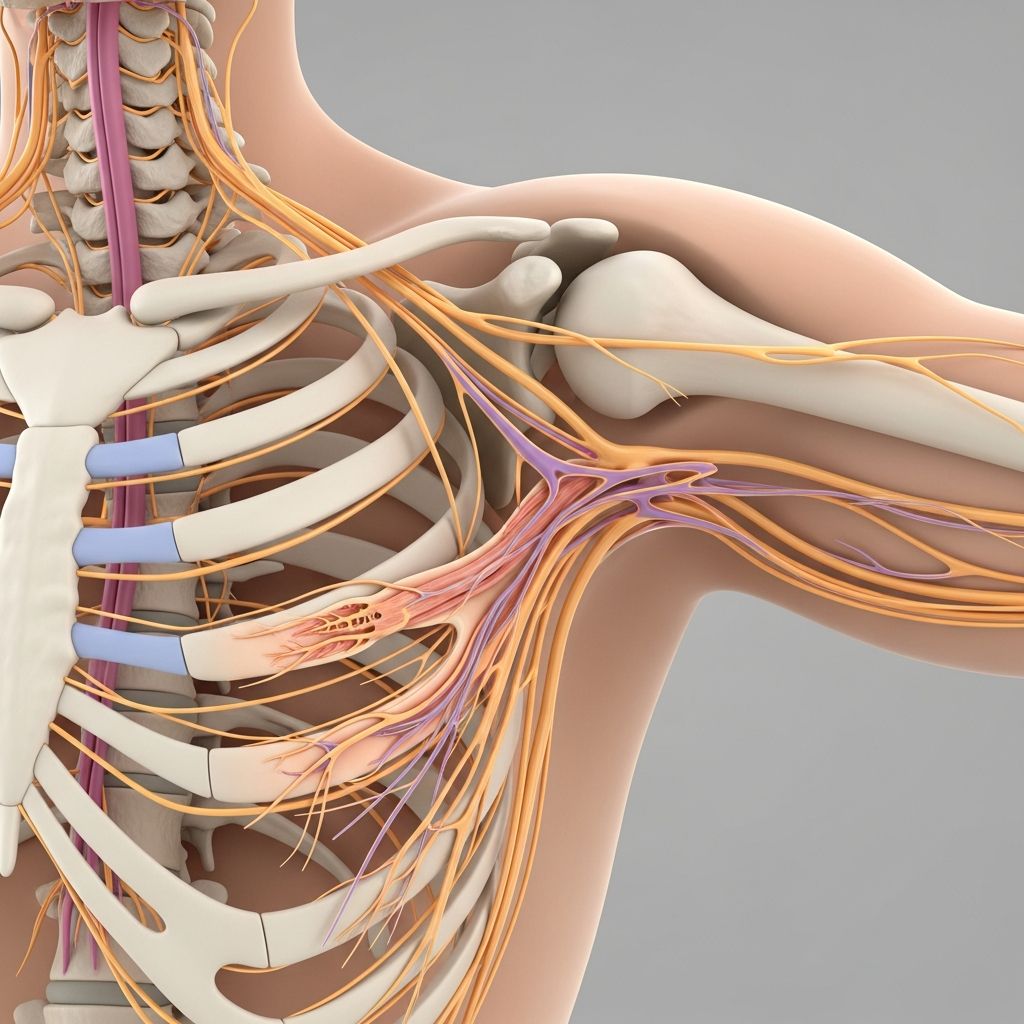
Understanding Brachial Plexus Injuries
A brachial plexus injury involves damage to the network of nerves that originates from the spinal cord in the neck and extends through the shoulder to control the arm, hand, and fingers. The brachial plexus is a complex system of nerves responsible for transmitting signals from the spine to the shoulder, arm, and hand, enabling movement and sensation. When these nerves are injured, the result can range from temporary weakness to permanent disability, depending on the severity and location of the damage.
These injuries can occur in individuals of all ages and can result from various traumatic events or medical conditions. Understanding the nature of brachial plexus injuries, their causes, symptoms, and available treatment options is essential for patients, caregivers, and healthcare professionals involved in managing these complex conditions.
Types of Brachial Plexus Injuries
Brachial plexus injuries are classified into several categories based on the severity and nature of the nerve damage. Each type presents different clinical presentations and requires distinct treatment approaches.
Stretch Injuries (Neuropraxia)
Stretch injuries, also known as neuropraxia, represent the mildest form of brachial plexus injury. In this type of injury, the nerves are stretched but not completely torn, resulting in damage to the protective covering of the nerves called the myelin sheath. Although nerve signals may be disrupted, these injuries often heal on their own or respond well to nonsurgical treatments such as physical therapy. Most individuals with neuropraxia experience recovery within several weeks to months without requiring surgical intervention.
Rupture Injuries
Rupture injuries occur when the nerves are forcefully stretched, causing partial or complete tearing of the nerve fibers. These injuries are more severe than simple stretches and typically require surgical repair to restore function. The extent of nerve damage in ruptures can vary significantly, with some cases involving partial tearing of individual nerve fibers and others involving complete transection of entire nerve trunks.
Avulsion Injuries
Avulsion injuries represent the most severe type of brachial plexus injury, where the nerve root is completely separated from the spinal cord. These devastating injuries often result in severe pain, permanent weakness, paralysis, and loss of sensation in the affected arm. Avulsion injuries typically require surgical intervention and present significant challenges for functional recovery.
Neuroma Formation
A brachial plexus neuroma develops when injured nerve tissue, such as from surgical trauma or laceration, forms a painful knot of scar tissue. This abnormal tissue growth can interfere with nerve function and may require surgical removal to restore proper nerve conduction.
Causes of Brachial Plexus Injuries
Brachial plexus injuries can develop through various mechanisms, with traumatic events being the most common cause in adults. The following represent the primary causes of these injuries:
Traumatic Injuries
Motor vehicle accidents, falls from significant heights, and collisions during contact sports are the leading causes of brachial plexus injuries in adults. These traumatic events can result in sudden, forceful stretching or tearing of the nerve fibers. The severity of injury depends on the force of impact, the direction of the force, and the position of the arm at the time of injury.
Birth-Related Injuries
Neonatal brachial plexus palsy (NBPP) occurs in infants and can result from compression within the uterus or trauma during difficult delivery. Certain risk factors increase the likelihood of birth-related brachial plexus injury, including large birth weight, breech presentation, and prolonged labor. Most birth-related injuries resolve spontaneously, though some cases require surgical intervention.
Inflammatory Conditions
Inflammatory responses triggered by infections, autoimmune reactions, or other medical conditions can affect the brachial plexus. Parsonage-Turner Syndrome, a rare condition characterized by inflammation of the brachial plexus, can cause severe shoulder or arm pain followed by muscle weakness and numbness without any obvious shoulder injury. This condition is sometimes misdiagnosed as cervical radiculopathy.
Symptoms and Clinical Presentation
The symptoms of brachial plexus injury vary significantly depending on the severity and location of the nerve damage. Symptoms can range from mild and transient to severe and permanent.
Common Symptoms
Patients with brachial plexus injuries may experience one or more of the following symptoms:
- Burning, stinging, or sudden severe pain in the shoulder or arm
- Weakness or numbness in the affected arm or hand
- Loss of sensation in the hand or arm
- Difficulty moving or controlling the shoulder, arm, wrist, or hand
- Paralysis of muscles in the affected limb
- Electric shock sensations (particularly in mild injuries from contact sports)
Pain Characteristics
Pain is a prominent feature of many brachial plexus injuries, particularly those involving avulsion of nerve roots from the spinal cord. This pain, called neuropathic pain, results from damage to the spinal cord and can be characterized as a debilitating, severe, crushing sensation or constant burning. Injuries occurring at or near the spinal cord level tend to produce greater pain than injuries farther from the spinal cord, and patients may experience burning numbness called paresthesia or dysesthesia. For most individuals, this severe pain diminishes within three years, though some patients experience persistent discomfort.
Diagnostic Evaluation
Accurate diagnosis of brachial plexus injuries involves a comprehensive clinical assessment and specialized imaging studies. Healthcare providers use various diagnostic tools to determine the type, severity, and location of nerve injury.
Clinical Examination
The initial evaluation includes a detailed history of the injury mechanism and a thorough physical examination assessing motor strength, sensory function, and reflex responses. Healthcare providers test individual muscles and nerve distributions to identify which specific nerves are affected.
Imaging Studies
Advanced imaging techniques help visualize nerve anatomy and identify areas of injury. Magnetic resonance imaging (MRI) and magnetic resonance neurography (MRN) can provide detailed images of the brachial plexus and surrounding tissues, helping clinicians identify nerve damage, scar tissue, and other abnormalities. Electromyography (EMG) and nerve conduction studies (NCS) assess the electrical activity of muscles and nerves, helping determine the extent and nature of nerve injury.
Treatment Approaches
Treatment for brachial plexus injuries depends on numerous factors, including injury severity, type, location, time since injury, and the patient’s overall health status. Treatment strategies range from conservative nonsurgical approaches to surgical interventions.
Nonsurgical Management
Many mild brachial plexus injuries heal well with nonsurgical treatment options. Conservative management typically includes a combination of the following approaches:
- Rest and activity modification to allow initial healing
- Physical therapy to restore range of motion, strength, and coordination
- Occupational therapy to restore practical skills such as dressing, eating, and cooking
- Assistive devices including braces, splints, and compression sleeves to support the affected limb
- Medications such as corticosteroids and pain management agents to control inflammation and pain during healing
- Constraint-induced movement therapy (CIMT) to encourage use of the affected limb
- Kinesiology taping and serial casting in appropriate cases
Physiotherapy and Rehabilitation
Physiotherapy forms a cornerstone of brachial plexus injury management, with treatment varying significantly according to injury type and severity. The primary goals of physiotherapy include developing strength, flexibility, stamina, and coordination; maintaining range of motion; providing functional training; controlling pain; and managing chronic swelling. Physiotherapists may employ various interventions including passive movements, exercise therapy, splinting, positioning, acupuncture, transcutaneous electrical nerve stimulation (TENS), and biofeedback. Evidence indicates that innovative physiotherapy interventions such as virtual reality simulation and electrotherapy can positively impact upper limb functionality in brachial plexus injuries.
Surgical Treatment
Healthcare providers typically recommend surgical treatment when nerves fail to heal on their own or do not recover sufficiently to restore necessary arm and hand function. Modern surgical approaches include several advanced techniques:
- Neurolysis: Surgical release of nerves from restrictive scar tissue that impedes nerve function and recovery
- Nerve repair: Direct surgical repair of nerves damaged by sharp objects or occasionally stretched nerve fibers
- Nerve grafts: Transplantation of nerves from other body regions to replace damaged nerve segments, creating a bridge for new nerve growth
- Nerve transfers: Groundbreaking microsurgical techniques that reroute healthy nerve fibers to restore function
- Microsurgery: Innovative microsurgical techniques to improve painful conditions involving the wrist, elbow, and shoulder
- Pain management surgery: Procedures to interrupt pain signals from the damaged spinal cord region for patients with severe, intractable pain
- Dorsal Root Entry Zone (DREZ) operation: A specialized procedure designed to destroy nerve signal transmission for persistent neuropathic pain
Surgical interventions are typically performed within specific timeframes, with microsurgical nerve repair often undertaken as early as three months post-injury, and primary nerve repair typically completed by approximately six months following injury.
Pain Management
Pain management is often a significant challenge in brachial plexus injury treatment. Severe pain from nerve injury can exhaust patients and hinder rehabilitation efforts, necessitating comprehensive pain management strategies.
Pharmacological Approaches
Initial pain management typically involves nonsteroidal anti-inflammatory drugs (NSAIDs) and opioid medications during early stages of injury. However, neuropathic pain resulting from nerve damage requires different pharmacological approaches. Anti-epileptic drugs such as gabapentin and carbamazepine, along with antidepressants like amitriptyline, are commonly used for chronic neuropathic pain management, though less than one-third of patients report significant pain relief with these medications alone.
Multimodal Pain Management
Physiotherapy offers additional pain relief strategies including TENS, biofeedback, acupuncture, and pain neuroscience education. For persistent pain unresponsive to medical management, healthcare providers may recommend surgical interventions such as the DREZ operation or other procedures designed to interrupt pain signal transmission from the damaged spinal cord.
Potential Complications and Long-Term Outcomes
Recovery from brachial plexus injury depends on numerous factors, including patient age, injury type, severity, and location. Even with surgical treatment, some individuals experience long-term complications including stiff joints, persistent numbness, muscle atrophy, and permanent disability.
Common Complications
- Stiff joints: Paralysis or prolonged immobility can lead to joint stiffness and contractures
- Persistent pain: Neuropathic pain may become chronic and last indefinitely
- Loss of sensation: Numbness increases risk of unintentional burns or injuries
- Muscle atrophy: Slow nerve regeneration combined with prolonged disuse causes muscle breakdown
- Permanent disability: Severe injuries may result in lasting weakness or paralysis despite treatment
Frequently Asked Questions
Q: Can brachial plexus injuries heal without surgery?
A: Yes, many mild brachial plexus injuries can heal without surgery over several weeks to months with appropriate physical therapy, rest, and activity modification. However, more severe injuries often require surgical intervention.
Q: How long does recovery from brachial plexus injury typically take?
A: Recovery time varies significantly depending on injury severity. Mild injuries may heal within weeks to months, while severe injuries may require years of rehabilitation and some individuals may have permanent effects.
Q: What is neuropathic pain and why is it associated with brachial plexus injuries?
A: Neuropathic pain results from damage to nerve fibers and can manifest as burning, crushing sensations or electric shock feelings. It’s particularly common in avulsion injuries and can be difficult to treat with standard pain medications.
Q: What role does physical therapy play in brachial plexus injury recovery?
A: Physical therapy is essential for maintaining range of motion, developing strength and coordination, managing pain, and restoring functional abilities. It forms a cornerstone of both nonsurgical treatment and post-surgical rehabilitation.
Q: Are there different treatment approaches for birth-related brachial plexus injuries?
A: Yes, birth-related injuries often have better prognosis with most resolving spontaneously. Treatment typically begins with physical and occupational therapy, with surgery considered if adequate recovery doesn’t occur within certain timeframes.
References
- Brachial Plexus Injury — Physiopedia. 2024. https://www.physio-pedia.com/Brachial_Plexus_Injury
- Brachial Plexus Injury – Symptoms and Causes — Penn Medicine, University of Pennsylvania. 2024. https://www.pennmedicine.org/conditions/brachial-plexus-injury
- Brachial Plexus Injury | Condition — UT Southwestern Medical Center. 2024. https://utswmed.org/conditions-treatments/brachial-plexus-injury/
- Brachial Plexus Injury: What It Is, Symptoms, Treatment & Types — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/22822-brachial-plexus-injury
- Brachial Plexus Injury – Symptoms and Causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/brachial-plexus-injury/symptoms-causes/syc-20350235
- Brachial Plexus Injuries — American Academy of Orthopaedic Surgeons (AAOS). 2024. https://orthoinfo.aaos.org/en/diseases–conditions/brachial-plexus-injuries/
- Brachial Plexus Injury – Diagnosis and Treatment — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/brachial-plexus-injury/diagnosis-treatment/drc-20350241
Read full bio of medha deb











