Bronchiectasis: Causes, Symptoms, Treatment & Prevention
Understanding bronchiectasis: Learn about causes, symptoms, diagnosis, and effective treatment options.
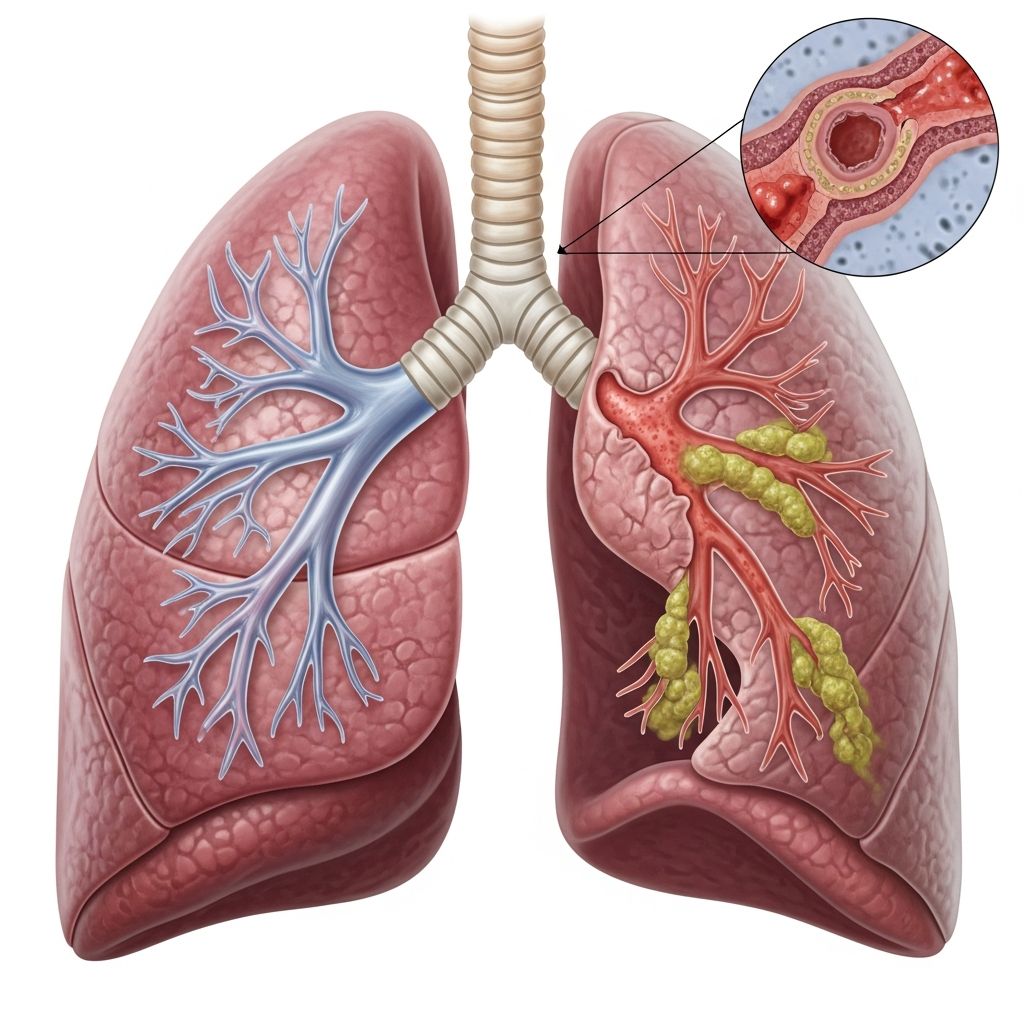
Understanding Bronchiectasis: A Comprehensive Guide
Bronchiectasis is a chronic lung condition characterized by permanent widening and damage to the airways (bronchi) that carry air into and out of your lungs. This progressive condition develops when the walls of your airways become damaged and thickened due to inflammation and repeated infections. The damage is permanent and cannot be fully reversed, but with proper management and treatment, most people with bronchiectasis can maintain a good quality of life and experience similar life expectancy to those without the condition.
In healthy lungs, the bronchi are flexible tubes with muscular walls that help move air efficiently. In bronchiectasis, these airways lose their structural integrity, becoming dilated and weakened. This damage prevents the walls from functioning properly to move mucus out of the lungs, leading to mucus accumulation and increased infection risk. Additionally, the cilia—tiny hair-like structures that normally help propel mucus upward—are destroyed in affected airways, further compromising the lung’s natural cleaning mechanisms.
What Causes Bronchiectasis?
Bronchiectasis can develop from various underlying conditions and causes. Understanding the root cause is essential for effective management and treatment planning. While approximately one-third of bronchiectasis cases have an identifiable cause, many cases remain idiopathic.
Common causes of bronchiectasis include:
– Cystic Fibrosis (CF)—a genetic disorder causing persistent lung infections and reduced breathing ability- Cystic Fibrosis (non-CF)—bronchiectasis occurring independently of cystic fibrosis- Primary ciliary dyskinesia—a genetic condition affecting ciliary function- Allergic bronchopulmonary aspergillosis—an allergic reaction to fungal infection- Alpha-1 antitrypsin deficiency—a genetic deficiency increasing lung disease risk- Asthma—chronic airway inflammation- Crohn’s disease—inflammatory bowel condition with pulmonary manifestations- Chronic aspiration or inhalation injury—from stomach contents or environmental irritants- Chronic Obstructive Pulmonary Disease (COPD)—progressive airway obstruction- Immune system deficits—immunodeficiency disorders- Nontuberculous mycobacteria (NTM) infections—opportunistic bacterial infections- Rheumatoid arthritis—autoimmune condition affecting lung tissue- Sjögren’s syndrome—autoimmune disorder affecting airways- Tracheobronchomegaly—abnormal enlargement of large airways- Ulcerative colitis—inflammatory bowel disease- Yellow nail syndrome—rare condition affecting nail and lung function
Recognizing the Symptoms
The symptoms of bronchiectasis can vary in severity and may develop gradually. Recognizing these symptoms early is crucial for timely diagnosis and treatment.
Primary symptoms include:
– Persistent coughing that produces large amounts of mucus (sputum)- Coughing up blood-tinged mucus, known as hemoptysis- Chest pain or tightness, particularly when breathing- Wheezing or whistling sounds during breathing- Clubbing of fingers and toes—thickening and widening of nail beds- Progressive weight loss- Shortness of breath, especially during physical activity
Acute exacerbations often include:
– Increased fatigue and general malaise- Fever and chills- Significantly increased shortness of breath- Night sweats- Increased mucus production- Worsening cough
These exacerbations represent periods when symptoms temporarily worsen and may indicate a respiratory tract infection or other complication requiring medical attention.
Types of Bronchiectasis
Healthcare providers classify bronchiectasis based on the appearance of airway damage and its distribution pattern. This classification helps determine severity and guides treatment decisions.
Based on appearance, bronchiectasis is categorized as:
– Cylindrical bronchiectasis—The most common and least severe form, where airways appear uniformly dilated- Varicose bronchiectasis—A moderate form where airways show irregular, beaded appearance- Cystic bronchiectasis—The most severe form, characterized by severely dilated airways forming cyst-like pouches- Traction bronchiectasis—Occurs when lung scarring pulls airways out of their normal shape
Based on distribution:
– Focal bronchiectasis—Damage limited to one specific area of the lungs- Diffuse bronchiectasis—Damage affecting multiple areas throughout both lungs
Cylindrical bronchiectasis, being the most common presentation, often has a better prognosis than cystic forms. However, even mild bronchiectasis requires proper management to prevent progression.
Diagnosis of Bronchiectasis
Accurate diagnosis is essential for developing an appropriate treatment plan. Healthcare providers use multiple diagnostic approaches to confirm bronchiectasis and identify underlying causes.
Diagnostic procedures and tests include:
– High-resolution computed tomography (HRCT) of the chest—The gold standard imaging test that clearly shows airway dilation and structural damage- Chest X-ray—May show characteristic findings, though less sensitive than HRCT- Pulmonary function tests (spirometry)—Measures how well your lungs function- Sputum cultures—Identifies infectious organisms present in mucus samples- Genetic testing—For cystic fibrosis and ciliary dyskinesia- Immunological testing—Evaluates immune system function- Bronchoscopy—Direct visualization of airways when diagnosis is unclear- Allergy testing—To identify potential allergic triggers
During the diagnostic process, your healthcare provider will perform a comprehensive physical examination and review your medical history. They may order additional tests to rule out other conditions that present similarly.
Treatment Strategies for Bronchiectasis
While bronchiectasis cannot be completely cured, effective treatment focuses on managing symptoms, clearing airways of mucus, treating infections, and slowing disease progression. A comprehensive approach combining multiple strategies typically yields the best results.
Treatment approaches include:
Airway Clearance Techniques
Clearing mucus from airways is the cornerstone of bronchiectasis management. Various techniques and devices help thin and mobilize secretions for easier expulsion.
– Chest physiotherapy and percussion techniques- Controlled coughing methods- Positive expiratory pressure (PEP) devices- Oscillating positive expiratory pressure devices- High-frequency chest wall oscillation vests- Medications that thin mucus, such as mucolytics- Nebulized medications to help loosen secretions
Infection Management
Treating and preventing respiratory infections is critical, as infections accelerate lung damage in bronchiectasis.
– Inhaled antibiotics targeting common pathogens like Pseudomonas aeruginosa- Oral or intravenous antibiotics during acute infections- Specialized laboratory testing to identify difficult-to-detect organisms- Prophylactic antibiotics in some cases- Regular monitoring for nontuberculous mycobacteria (NTM) infections
Anti-inflammatory Therapy
Daily anti-inflammatory medications help reduce airway inflammation and stabilize lung function.
– Inhaled corticosteroids- Systemic corticosteroids during acute flares- Other anti-inflammatory agents as prescribed
Additional Therapeutic Options
– Bronchodilators to improve airflow- Mucosal hydration strategies- Vaccination against respiratory infections- Pulmonary rehabilitation programs- Oxygen therapy when needed
Managing Your Condition
Living with bronchiectasis requires active participation in your care and daily management routines. Consistent adherence to treatment recommendations significantly impacts disease progression and quality of life.
Daily management strategies include:
– Performing prescribed airway clearance techniques regularly- Taking medications exactly as prescribed- Staying hydrated to help thin mucus- Avoiding environmental irritants and pollutants- Maintaining physical activity within tolerance- Receiving recommended vaccinations- Attending regular healthcare appointments- Monitoring for signs of infection or exacerbation- Maintaining good nutrition- Managing stress
Potential Complications
While most people with bronchiectasis manage their condition successfully, severe cases can lead to serious complications. Understanding these risks emphasizes the importance of proper treatment adherence.
Possible complications include:
– Recurrent pneumonia- Respiratory failure requiring hospitalization- Massive hemoptysis (coughing up large amounts of blood)- Cor pulmonale (heart disease from lung disease)- Respiratory acidosis
Severe bronchiectasis can significantly impact quality of life and may require more intensive interventions. In rare cases where damage is limited to a small lung area and standard treatments fail, surgical removal of the affected portion may be considered.
Long-Term Outlook and Prognosis
Your prognosis depends on several factors, including disease severity, how well you respond to treatment, presence of other health conditions, smoking history, and baseline lung function. With proper treatment, most people with bronchiectasis can expect longevity comparable to the general population.
However, certain factors can negatively impact life expectancy. A significant smoking history and reduced baseline lung function may lower long-term outlook. The degree to which you adhere to treatment recommendations and manage exacerbations also influences outcomes.
In most cases, bronchiectasis should not prevent you from living a full, active life. Working closely with your healthcare provider to address bothersome symptoms and manage exacerbations can greatly improve your quality of life. Sometimes small modifications to your treatment plan or lifestyle can produce significant improvements.
Prevention Strategies
While you cannot prevent bronchiectasis if you have a genetic predisposition or underlying condition, certain measures may help slow progression and reduce exacerbations:
– Avoiding respiratory irritants and pollution- Not smoking and avoiding secondhand smoke- Preventing respiratory infections through vaccination- Practicing good hand hygiene- Seeking prompt treatment for respiratory infections- Avoiding aspiration of stomach contents- Managing underlying conditions effectively- Following your prescribed treatment regimen consistently
Frequently Asked Questions About Bronchiectasis
Q: Is bronchiectasis curable?
A: No, bronchiectasis cannot be fully cured because the damage to airways is permanent. However, treatment focuses on managing symptoms, preventing progression, and maintaining quality of life. With appropriate care, most people with bronchiectasis can live normal lifespans.
Q: How is bronchiectasis diagnosed?
A: Bronchiectasis is primarily diagnosed through high-resolution CT scans of the chest, which clearly show airway dilation and damage. Your doctor will also perform pulmonary function tests, sputum cultures, and may order genetic or immunological testing based on clinical suspicion.
Q: What is the most important part of bronchiectasis treatment?
A: Airway clearance is considered the cornerstone of therapy. Regularly clearing mucus from airways helps prevent infections and slows disease progression. This involves using special techniques and devices prescribed by your healthcare team.
Q: Can bronchiectasis be prevented?
A: You cannot prevent bronchiectasis if you have underlying genetic or medical conditions causing it. However, you can slow progression by avoiding respiratory irritants, preventing infections through vaccinations, managing underlying conditions, and following your treatment plan consistently.
Q: How often should I see my doctor with bronchiectasis?
A: Regular monitoring is essential. Most patients require periodic follow-up appointments to assess disease progression, adjust medications, and screen for complications. Your doctor will recommend an appropriate schedule based on your individual condition severity.
Q: What lifestyle changes help manage bronchiectasis?
A: Important lifestyle modifications include performing daily airway clearance techniques, staying hydrated, avoiding smoking and environmental pollutants, maintaining physical activity within your tolerance, getting recommended vaccinations, and managing stress levels effectively.
Q: Can exercise help with bronchiectasis?
A: Yes, physical activity and pulmonary rehabilitation programs can benefit bronchiectasis patients. Exercise helps improve lung function, clearance of secretions, and overall cardiovascular health. Always consult your healthcare provider before starting new exercise programs.
Q: What should I do during a bronchiectasis exacerbation?
A: During exacerbations, increase your airway clearance frequency, monitor symptoms closely, and contact your healthcare provider promptly. You may need antibiotics or other medications. Seek emergency care if experiencing severe shortness of breath or coughing up blood.
References
- Bronchiectasis: Causes, Symptoms, Treatment & Prevention — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/21144-bronchiectasis
- Bronchiectasis – Overview and Department Information — Cleveland Clinic. 2024. https://my.clevelandclinic.org/departments/respiratory/depts/bronchiectasis
- Bronchiectasis — American Lung Association. 2024. https://www.lung.org/lung-health-diseases/lung-disease-lookup/bronchiectasis
- Etiology and Clinical Characteristics of Non-Cystic Fibrosis Bronchiectasis — National Institutes of Health. 2023. https://pmc.ncbi.nlm.nih.gov/articles/PMC10334600/
- Bronchiectasis and Nontuberculous Mycobacteria (NTM) Center — Cleveland Clinic Florida. 2024. https://my.clevelandclinic.org/florida/departments/respiratory/depts/bronchiectasis-nontuberculous-mycobacteria-center
- Bronchiectasis Program — Cleveland Clinic Abu Dhabi. 2024. https://www.clevelandclinicabudhabi.ae/en/institutes-and-specialties/integrated-hospital-care/bronchiectasis
Read full bio of medha deb











