Bronchitis: Causes, Symptoms, Diagnosis & Treatment
Complete guide to understanding bronchitis: types, causes, symptoms, diagnosis, and effective treatment options.
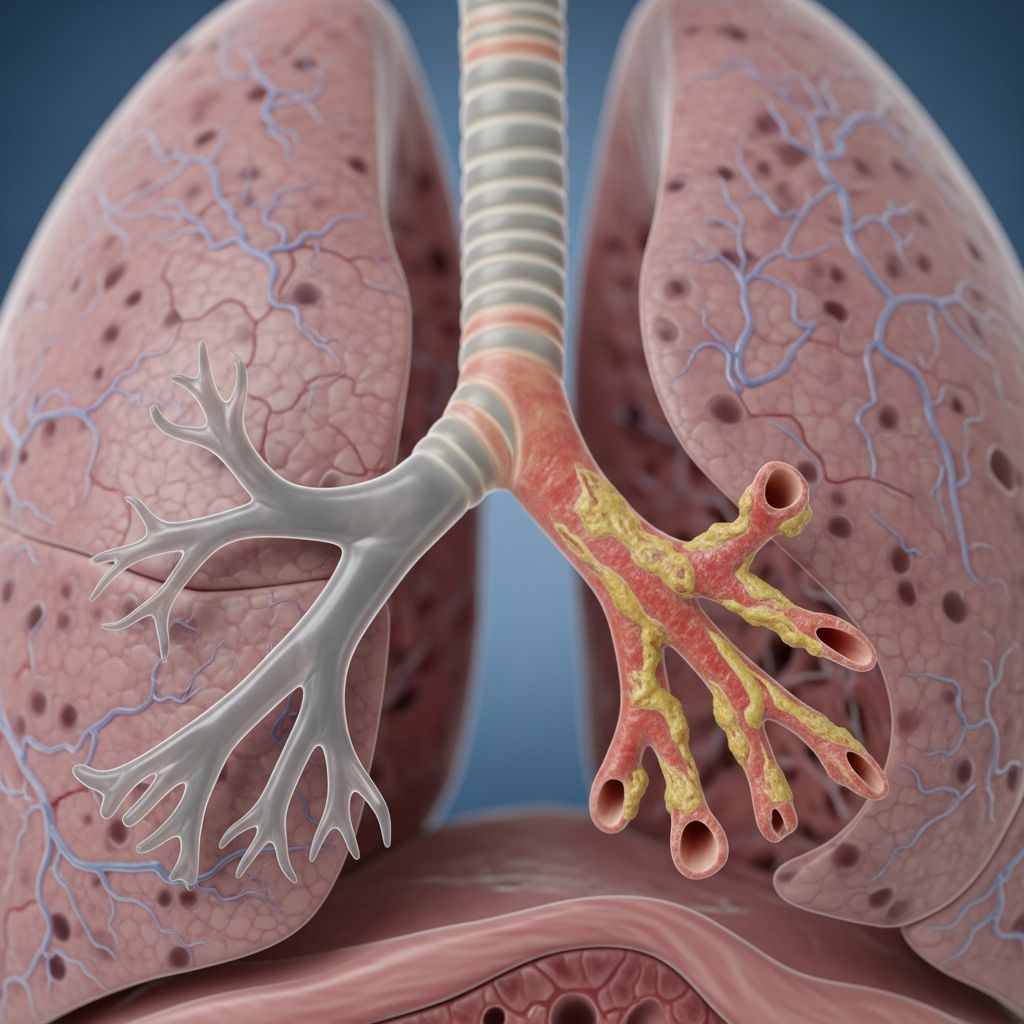
Bronchitis is a common respiratory condition that affects millions of people each year. It occurs when the bronchial tubes in your lungs become inflamed and swollen, causing persistent coughing and mucus production. Understanding this condition is essential for recognizing symptoms early and seeking appropriate treatment.
What Is Bronchitis?
Bronchitis happens when the bronchial tubes, which carry air to the lungs, become inflamed and swollen. These tubes are responsible for transporting oxygen to your lungs and removing carbon dioxide from your body. When they become irritated, your body responds by producing excess mucus and triggering a cough as it attempts to clear the airways.
The condition can range from mild to severe, and understanding which type you have is crucial for determining the appropriate treatment approach. Most cases of bronchitis are temporary and resolve within a few weeks, though some people experience longer-lasting symptoms that require ongoing management.
Types of Bronchitis
There are two primary types of bronchitis, each with distinct characteristics and treatment approaches.
Acute Bronchitis
Acute bronchitis, sometimes called a chest cold, is the more common type. This form of bronchitis typically develops following a viral infection, such as the common cold or influenza. Symptoms usually appear suddenly and last for a few weeks, though in some cases they may persist longer.
Most people with acute bronchitis don’t require specific medical treatment beyond supportive care. The condition is usually self-limiting, meaning it resolves on its own as your immune system fights off the viral infection. However, it’s important to monitor your symptoms and contact your healthcare provider if they worsen or persist beyond a few weeks.
Chronic Bronchitis
Chronic bronchitis is a more serious condition that represents a form of chronic obstructive pulmonary disease (COPD). Unlike acute bronchitis, chronic bronchitis is defined by symptoms lasting at least three months out of the year, recurring for at least two consecutive years. This condition causes ongoing inflammation and irritation of the bronchial tube lining, with frequent mucus production that characterizes the persistent cough.
Chronic bronchitis never fully goes away and may worsen over time, though it can be managed effectively with proper treatment. The condition significantly impacts quality of life and requires ongoing medical supervision and symptom management strategies.
Causes of Bronchitis
Different factors cause acute and chronic bronchitis, and understanding these triggers is important for prevention and management.
Causes of Acute Bronchitis
Acute bronchitis is usually caused by a viral infection. The most common culprits include:
– Common cold viruses- Influenza (flu)- COVID-19- Respiratory syncytial virus (RSV)- Parainfluenza virus
In rare cases, bacterial infections can cause acute bronchitis, though viral infections are responsible for the vast majority of cases. Your immune system responds to these infections by inflaming the bronchial tubes, triggering the characteristic cough and mucus production.
Causes of Chronic Bronchitis
Chronic bronchitis is almost always caused by smoking and exposure to lung irritants. The primary causes include:
– Cigarette smoking (the leading cause)- Environmental pollutants and air quality issues- Occupational exposures to harmful substances- Underlying lung conditions like asthma- Genetic predisposition in some cases
Unlike acute bronchitis, chronic bronchitis develops gradually over time as repeated exposure to irritants damages lung tissue and causes persistent inflammation. The longer someone smokes or is exposed to harmful substances, the greater the risk of developing this serious condition.
Symptoms of Bronchitis
While the primary symptom of bronchitis is a persistent cough, several other signs may accompany this condition.
Common Symptoms
The main symptom of bronchitis is a nagging cough that produces mucus. Additional symptoms may include:
– Mucus or sputum production (clear, white, yellowish, or greenish)- Fatigue and weakness- Shortness of breath or difficulty breathing- Wheezing or whistling sounds when breathing- Chest discomfort or mild chest pain- Slight fever or chills- Sore throat
In acute bronchitis, these symptoms typically develop after an upper respiratory infection and gradually improve over time. In chronic bronchitis, these symptoms persist or frequently recur, significantly impacting daily activities and quality of life.
When to See a Doctor
You should contact your healthcare provider if you experience:
– A persistent cough lasting more than three weeks- Cough accompanied by a foul-tasting fluid in your mouth- Fever above 100.4°F- Wheezing or shortness of breath- Symptoms that worsen despite home treatment- Blood in your sputum- If you’re 75 or older with an ongoing cough- If you have a lung condition like COPD and experience a flare-up
Additionally, if you develop symptoms suggesting pneumonia, such as high fever or severe shortness of breath, seek immediate medical attention.
Diagnosis of Bronchitis
Your healthcare provider can diagnose bronchitis based on your health history and symptoms through a clinical diagnosis. There aren’t any specific tests that definitively diagnose bronchitis, but your doctor will use various methods to confirm the diagnosis and rule out other conditions.
Diagnostic Methods
During your examination, your healthcare provider will:
– Listen to your lungs with a stethoscope for signs of congestion- Check that you’re breathing well- Review your medical history and symptom timeline- Perform a physical examination
Possible Tests
While not always necessary, your doctor may order the following tests:
– Chest X-ray to check for pneumonia or other illnesses causing your cough- Blood tests to identify signs of infection or measure oxygen and carbon dioxide levels in your blood- Mucus samples to rule out bacterial diseases like whooping cough (pertussis)- Nasal swabs if your doctor suspects influenza, COVID-19, or whooping cough- Pulmonary function tests to assess how well your lungs are working- C-reactive protein tests to detect inflammation
If you frequently develop bronchitis, your healthcare provider may investigate whether you have chronic bronchitis caused by an underlying condition requiring specialized treatment.
Treatment Options
Treatment approaches differ significantly between acute and chronic bronchitis, tailored to each condition’s specific characteristics.
Acute Bronchitis Treatment
Most people with acute bronchitis don’t need specific medical treatment beyond supportive care. The condition typically resolves on its own in a few weeks as your immune system clears the viral infection. Treatment focuses on managing symptoms and supporting your body’s natural healing process:
– Rest: Allow your body adequate time to recover- Hydration: Drink plenty of fluids to help loosen mucus- Humidification: Use a humidifier or breathe steam to ease congestion- Over-the-counter medications: Pain relievers and cough suppressants for symptom relief- Honey: Can help soothe throat irritation and reduce cough
Antibiotics are not typically prescribed for acute bronchitis unless a bacterial infection is confirmed, as they’re ineffective against viral infections and unnecessary in most cases.
Chronic Bronchitis Treatment
Chronic bronchitis treatment focuses on managing symptoms and slowing disease progression. Depending on severity, treatment may include:
– Medications such as antibiotics (for bacterial infections), anti-inflammatories, and bronchodilators to open airways- Mucus-clearing devices to help cough up fluid more easily- Oxygen therapy to improve breathing- Pulmonary rehabilitation programs featuring exercise regimens- Mucolytics (inhaled or oral medications) to loosen mucus- Flu and pneumonia vaccinations to prevent complications
Your healthcare provider will develop a personalized treatment plan based on your specific condition’s severity and your individual needs.
Prevention Strategies
Reducing your risk of bronchitis involves several preventive measures:
– Quit smoking if you currently smoke- Avoid secondhand smoke exposure- Limit exposure to air pollutants and environmental irritants- Practice good hygiene: wash hands frequently and avoid touching your face- Get vaccinated: annual flu shot and pneumonia vaccine as recommended- Maintain good nutrition and adequate sleep- Manage underlying conditions like asthma effectively- Use protective equipment in occupational settings with potential irritant exposure
Complications and When to Seek Emergency Care
While bronchitis usually doesn’t cause serious complications, it’s important to recognize warning signs. Bronchitis can lead to pneumonia in rare cases, though this is uncommon. Seek emergency medical attention if you experience:
– Severe shortness of breath- Chest pain- High fever (above 103°F)- Confusion or altered mental status- Blue lips or fingernails- Coughing up blood
People with COPD or other underlying lung conditions are at higher risk of complications and should maintain close contact with their healthcare provider.
Living with Bronchitis
For those with acute bronchitis, recovery typically occurs within a few weeks with appropriate self-care. However, for chronic bronchitis, ongoing management is necessary.
Understanding your treatment plan and medications is crucial. Ask your healthcare provider to explain how to take prescribed medications and use any medical devices like inhalers or supplemental oxygen. Regular follow-up appointments help monitor your condition’s progression and adjust treatment as needed.
Remember that while chronic bronchitis cannot be cured, symptoms can improve significantly with proper treatment. Your healthcare provider can help manage symptoms, slow disease progression, and reduce flare-ups, ultimately improving your quality of life.
Frequently Asked Questions
Q: Can acute bronchitis turn into chronic bronchitis?
A: Acute bronchitis itself doesn’t turn into chronic bronchitis. However, if you experience repeated episodes of acute bronchitis, this may indicate an underlying condition requiring evaluation. Chronic bronchitis is a long-term condition caused by ongoing irritation, usually from smoking or environmental exposure, whereas acute bronchitis is a temporary viral infection.
Q: Is bronchitis contagious?
A: Acute bronchitis caused by viral infections is contagious, and you can spread the underlying virus to others. However, chronic bronchitis itself is not contagious. People with chronic bronchitis are more susceptible to catching contagious illnesses like colds and flu, which may worsen their symptoms.
Q: How long does acute bronchitis typically last?
A: Acute bronchitis usually lasts a few days to a few weeks. In some cases, the cough may persist for four weeks or longer, even after other symptoms resolve. If symptoms last more than three weeks, contact your healthcare provider.
Q: Can bronchitis lead to pneumonia?
A: While bronchitis can lead to pneumonia, this is rare. Most people recover from bronchitis without developing pneumonia. However, certain risk factors increase this possibility, including advanced age, weakened immune system, or underlying lung conditions.
Q: What’s the difference between bronchitis and pneumonia?
A: Both are respiratory infections, but they affect different parts of your lungs. Bronchitis affects the bronchial tubes that carry air to your lungs, while pneumonia affects the air sacs (alveoli) where oxygen exchange occurs. Pneumonia is generally more serious and requires specific antibiotic treatment.
Q: Should I take antibiotics for bronchitis?
A: Most cases of acute bronchitis are caused by viruses, so antibiotics are ineffective and unnecessary. Your doctor may prescribe antibiotics only if a bacterial infection is confirmed. For chronic bronchitis, antibiotics may be used during flare-ups if bacterial infection is present.
References
- Bronchitis: Causes, Symptoms, Diagnosis & Treatment — Cleveland Clinic. 2022-09-08. https://my.clevelandclinic.org/health/diseases/3993-bronchitis
- Chronic Bronchitis: Causes, Symptoms, Diagnosis & Treatment — Cleveland Clinic. 2023-01-24. https://my.clevelandclinic.org/health/diseases/24645-chronic-bronchitis
- Bronchitis (Acute and Chronic): Symptoms, Causes & Treatment — WebMD. https://www.webmd.com/lung/understanding-bronchitis-basics
- Acute bronchitis – Symptoms, diagnosis and treatment — BMJ Best Practice. https://bestpractice.bmj.com/topics/en-us/135
- Bronchitis vs. Pneumonia: How To Tell the Difference — Cleveland Clinic Health. https://health.clevelandclinic.org/bronchitis-vs-pneumonia
Read full bio of medha deb











