Bronchoscopy: Purpose, Procedure, Risks & Results
Complete guide to bronchoscopy: Learn about this minimally invasive lung examination procedure and what to expect.
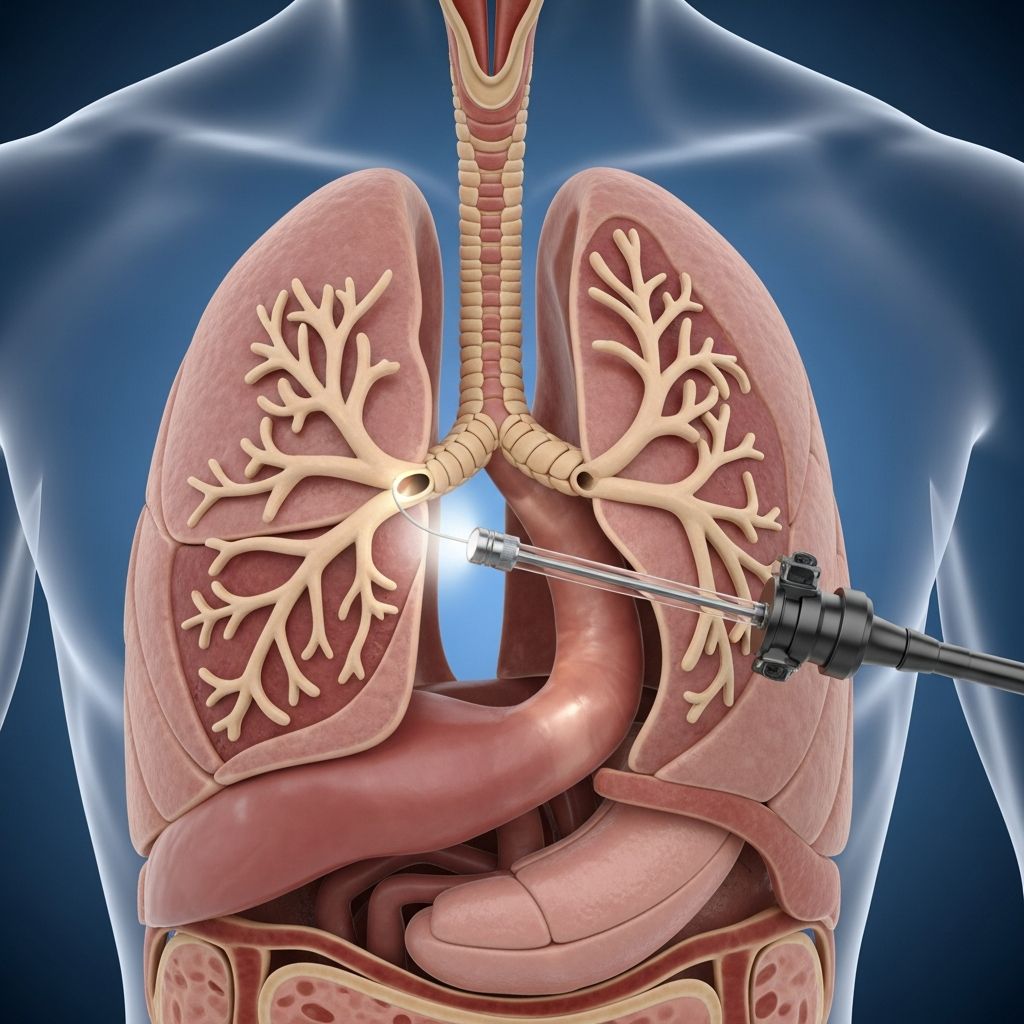
What Is Bronchoscopy?
A bronchoscopy is a minimally invasive procedure that allows your healthcare provider to look inside your airways and lungs with a specialized instrument called a bronchoscope. This thin, flexible tube contains a small camera and light source that transmits images to a television monitor, enabling your physician to examine the structures within your respiratory system in detail. The procedure involves little risk and is generally not painful, making it a preferred diagnostic and therapeutic tool in modern pulmonary medicine.
The bronchoscope is typically passed through either your nose or mouth, past the vocal cords, and into your windpipe to visualize the large and small airways of your lungs. Beyond simple visualization, healthcare providers can use bronchoscopy to collect tissue samples, washings, or perform various therapeutic interventions when needed.
Purpose of Bronchoscopy
Bronchoscopy serves both diagnostic and therapeutic purposes in pulmonary care. Healthcare providers use this procedure to investigate and treat various conditions affecting the airways and lungs.
Diagnostic Uses
Bronchoscopy helps diagnose numerous lung and airway disorders by allowing direct visualization and tissue sampling. Healthcare providers may recommend bronchoscopy to:
– Investigate persistent cough lasting more than three weeks- Evaluate abnormal chest imaging findings- Diagnose infections, including suspected tuberculosis or fungal infections- Detect benign tumors, polyps, and other airway lesions- Assess lung cancer and obtain tissue samples for biopsy- Evaluate cases of hemoptysis (coughing up blood)- Investigate chronic obstructive pulmonary disease (COPD)- Diagnose interstitial lung disease- Assess suspected foreign body aspiration
Therapeutic Uses
Beyond diagnosis, bronchoscopy offers therapeutic interventions for airway and lung conditions:
– Removal of foreign bodies from airways- Clearing excessive mucus or secretions- Placement of airway stents for narrowed passages- Laser therapy for obstructing tumors- Thermal ablation procedures- Argon plasma coagulation for bleeding control- Treatment of severe asthma through bronchial thermoplasty- Placement of endobronchial valves for air leak management
How Bronchoscopy Is Performed
Preparation Before the Procedure
Proper preparation is essential for a successful bronchoscopy. Your healthcare team will provide specific instructions tailored to your situation. Generally, you should plan to:
– Refrain from eating or drinking for a specified period before the procedure, typically six to eight hours- Arrange transportation home, as you won’t be able to drive after sedation- Wear comfortable, loose-fitting clothing- Remove any dentures, hearing aids, or contact lenses- Inform your healthcare provider of all medications, especially blood thinners- Discuss any allergies or medical conditions
Anesthesia Options
Bronchoscopy can be performed under different levels of sedation based on the procedure type and patient factors. Options include:
– Topical anesthesia with mild sedation for simple diagnostic procedures- Moderate conscious sedation for standard bronchoscopies- General anesthesia with a supraglottic airway for advanced procedures- General anesthesia with an endotracheal tube for complex interventions- General anesthesia with rigid bronchoscopy for specialized therapeutic procedures
The Procedure Steps
Once anesthesia is administered and you’re comfortable, your healthcare provider will begin the examination. Your throat will be numbed to reduce the gag reflex, and the bronchoscope will be carefully passed through your mouth or nose into your windpipe. The provider then performs a complete inspection of all airways, examining the branching pattern and structures within your lungs.
If specific areas require closer evaluation, the provider may perform bronchoalveolar lavage, in which the bronchoscope is wedged at the opening of an airway leading to the area of interest. Sterile saline is then instilled and aspirated to collect cells and fluid for laboratory analysis. Additional diagnostic techniques may include biopsy sample collection, brush biopsies, or washings depending on clinical findings and the suspected diagnosis.
For advanced diagnostic procedures such as endobronchial ultrasound (EBUS), the bronchoscope is equipped with ultrasound capabilities. The ultrasound function allows detection and avoidance of mediastinal blood vessels, with lymph nodes typically biopsied if they measure greater than 0.5 millimeters. Samples are often evaluated immediately through rapid on-site pathology evaluation, allowing verification of adequate samples and preliminary diagnosis during the same procedure.
Advanced Bronchoscopy Techniques
Electromagnetic Navigation Bronchoscopy (ENB)
Electromagnetic navigation bronchoscopy represents a significant advancement in reaching peripheral lung lesions that are difficult to access with standard techniques. This technology uses electromagnetic fields to guide the bronchoscope to specific target areas within the lungs, improving diagnostic accuracy for suspicious nodules and lesions.
Endobronchial Ultrasound (EBUS)
EBUS has revolutionized the diagnosis and staging of lung cancer by replacing traditional mediastinoscopy procedures. During EBUS-guided transbronchial needle aspiration (EBUS-TBNA), the ultrasound probe on the bronchoscope allows visualization of lymph nodes and other structures, with Doppler capabilities enabling detection and avoidance of major blood vessels. The procedure is generally performed under general anesthesia with sedation, often with muscle relaxation to minimize coughing and patient movement that could complicate biopsy accuracy.
Robotic-Assisted Bronchoscopy
The FDA approval of robot-assisted bronchoscopy (RAB) has transformed clinicians’ ability to obtain biopsies of hard-to-reach peripheral lung nodules. This technology enhances precision and diagnostic yield, particularly for suspicious lesions in the lung periphery that might otherwise require more invasive procedures.
Narrow-Band Imaging Bronchoscopy (NBI)
Narrow-band imaging uses specialized light wavelengths to enhance visualization of mucosal abnormalities and vascular patterns within the airways, improving detection of early cancerous changes and other pathological conditions.
Risks and Complications
While bronchoscopy is generally considered a safe procedure with minimal risk, complications can occasionally occur. Understanding potential risks helps you make informed decisions about your care.
Common Side Effects
– Sore throat lasting one to two days- Hoarseness of voice- Mild cough- Temporary difficulty swallowing- Temporary nausea
Rare but Serious Complications
Serious complications are uncommon but may include:
– Bronchospasm (airway constriction)- Hemoptysis (bleeding from airways)- Pneumothorax (collapsed lung)- Respiratory depression- Infection- Aspiration- Cardiac arrhythmias- Airway perforation (very rare)
Your healthcare provider will take precautions to minimize these risks, including proper patient selection, careful technique, appropriate anesthesia management, and continuous monitoring throughout the procedure. Preoperative testing may include cardiac risk assessment, glucose control evaluation for diabetic patients, coagulation studies in those with impaired hemostasis, and hemoglobin evaluation in anemic patients.
After Your Bronchoscopy
Recovery Timeline
Most patients recover quickly from bronchoscopy. You’ll be monitored in a recovery area until the sedation wears off completely. Vital signs and oxygen saturation will be checked regularly. Most people are discharged home the same day after EBUS procedures, though specific discharge timing depends on the type of procedure performed and your individual recovery.
Post-Procedure Care
Following your bronchoscopy, observe these guidelines:
– Rest for the remainder of the day- Avoid eating or drinking until the numbing sensation in your throat wears off (typically one to two hours)- Avoid strenuous activity for 24 hours- Do not operate a vehicle or machinery for 24 hours after receiving sedation- Take throat lozenges if desired for comfort- Use over-the-counter pain relievers if you experience throat discomfort- Stay hydrated with plenty of fluids- Contact your healthcare provider if you experience persistent symptoms
Results and Follow-Up
Bronchoscopy results depend on what was found during the procedure and what samples were collected. Your healthcare provider will discuss initial findings with you, though final pathology results from tissue biopsies may take several days to several weeks.
What Results Mean
Negative results indicate that no obvious abnormalities were detected during the visual examination, and tissue samples showed no signs of infection, malignancy, or other pathology. However, negative results don’t completely rule out disease, particularly if symptoms persist.
Positive results indicate that abnormalities were identified, which may include infections, tumors, inflammatory conditions, or other pathology. Your healthcare provider will explain findings in detail and recommend appropriate follow-up treatment or additional testing based on results.
Follow-Up Care
Depending on your results, follow-up may include repeat bronchoscopy, additional imaging studies, specialist consultations, or initiation of specific treatments. Your healthcare provider will create a personalized follow-up plan based on your diagnosis and clinical situation.
Advanced Bronchoscopy Services Available
Specialized bronchoscopy programs offer comprehensive diagnostic and therapeutic services. Cleveland Clinic and similar advanced centers provide procedures including argon plasma coagulation for tumor ablation, balloon dilation for airway narrowing, brachytherapy for tumor destruction, bronchial thermoplasty for severe asthma, broncholith removal, chest tube placement, endobronchial valve insertion, foreign body removal, stent placement and removal, and various laser and thermal ablation modalities.
Frequently Asked Questions
Q: Is bronchoscopy painful?
A: No, bronchoscopy is not painful. Your throat will be numbed with topical anesthesia, and you’ll receive sedation to keep you comfortable throughout the procedure. You may feel pressure or mild discomfort but should not experience pain.
Q: How long does a bronchoscopy take?
A: A typical diagnostic bronchoscopy takes 15 to 45 minutes, depending on the procedure type and findings. Therapeutic procedures may take longer. Time in recovery typically adds another hour to your total visit duration.
Q: Can I go home the same day?
A: Yes, most patients go home the same day. However, you’ll need someone to drive you home since you cannot operate a vehicle within 24 hours of receiving sedation.
Q: What should I avoid after bronchoscopy?
A: Avoid eating or drinking until the numbing sensation wears off, strenuous activity for 24 hours, and operating vehicles or machinery while sedated. Rest is recommended for the remainder of the procedure day.
Q: When will I receive my results?
A: Visual findings are typically discussed immediately after the procedure. Pathology results from tissue samples may take several days to weeks, depending on the complexity of testing required.
Q: Are there alternatives to bronchoscopy?
A: Depending on your condition, alternatives may include CT imaging, chest X-rays, or other diagnostic tests. However, bronchoscopy offers unique advantages, including direct visualization and tissue sampling capabilities that other tests cannot provide.
Q: Can I take my regular medications before bronchoscopy?
A: This depends on your specific medications. Inform your healthcare provider of all medications you take, particularly blood thinners. Some medications may need to be adjusted or held before the procedure.
Conclusion
Bronchoscopy remains one of the most valuable tools in pulmonary medicine, offering both diagnostic and therapeutic capabilities with minimal risk. Whether evaluating persistent respiratory symptoms, investigating abnormal imaging findings, or treating airway obstructions, this procedure provides essential information and intervention options. Understanding the procedure, its purposes, and what to expect helps patients approach bronchoscopy with confidence, knowing they’re receiving advanced, evidence-based diagnostic and therapeutic care from qualified healthcare professionals.
References
- Anesthetic considerations for bronchoscopic procedures: a narrative review — PubMed Central, National Institutes of Health. 2019. https://pmc.ncbi.nlm.nih.gov/articles/PMC6688002/
- Bronchoscopy Services — Cleveland Clinic Department of Respiratory. 2025. https://my.clevelandclinic.org/departments/respiratory/depts/bronchoscopy
- Navigational bronchoscopy: A guide through history, current use and future directions — Journal of Thoracic Disease, AME Medical Journal. 2021. https://jtd.amegroups.org/article/view/39529/html
- Novel bronchoscopy platforms for biopsy of peripheral pulmonary lesions — ConsultQD, Cleveland Clinic. 2024. https://consultqd.clevelandclinic.org/novel-bronchoscopy-platforms-for-biopsy-of-peripheral-pulmonary-lesions
- Robotic-assisted bronchoscopy reshapes early lung cancer management — ConsultQD, Cleveland Clinic. 2024. https://consultqd.clevelandclinic.org/precision-and-progress-robotic-assisted-bronchoscopy-reshapes-early-lung-cancer-management
- Bronchoscopy and interventional bronchoscopy program — Cleveland Clinic Abu Dhabi. 2024. https://www.clevelandclinicabudhabi.ae/en/institutes-and-specialties/integrated-hospital-care/bronchoscopy-and-interventional-bronchoscopy-program
Read full bio of Sneha Tete













