Understanding Bunions: Causes, Treatment, and Prevention
Complete guide to bunion management: from conservative care to surgical options and prevention strategies.
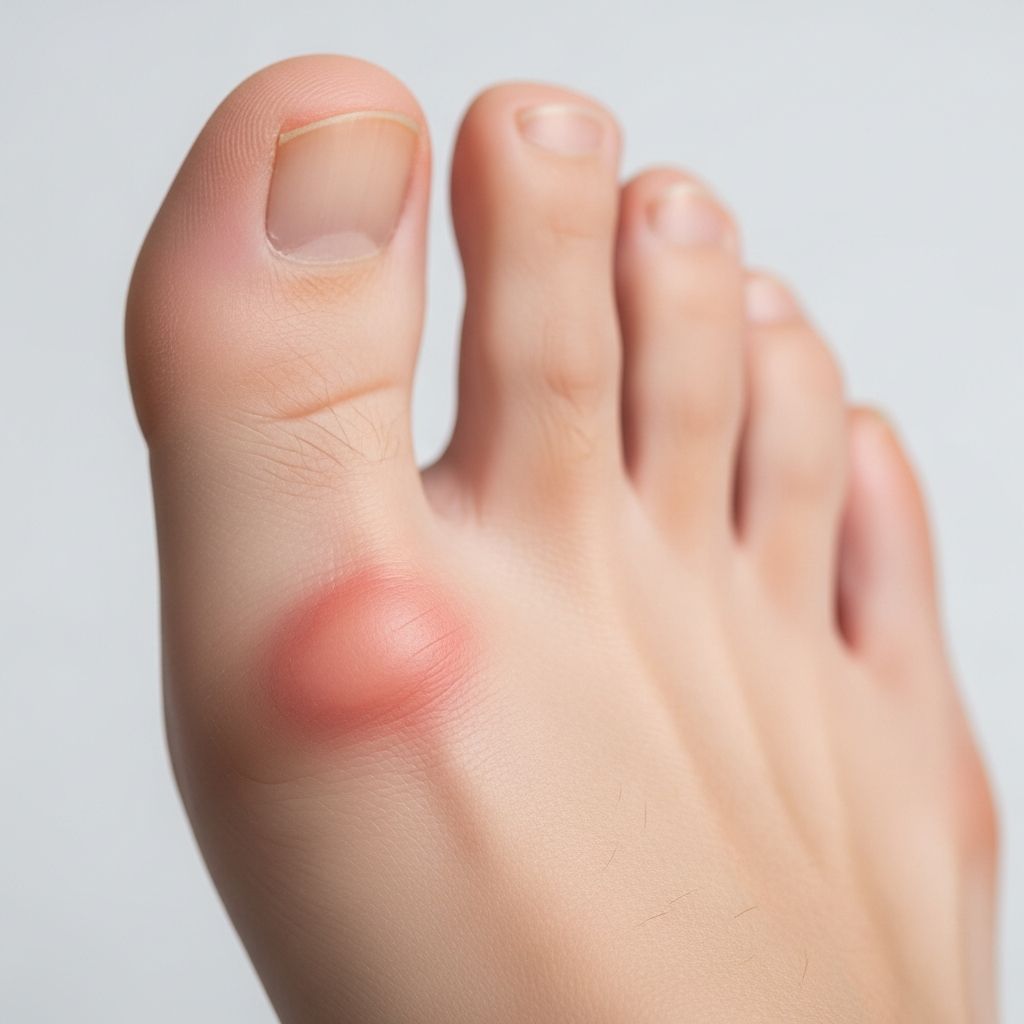
What Are Bunions?
A bunion is a bony bump that forms on the joint at the base of your big toe, a condition medically known as hallux valgus. This deformity develops when the big toe pushes inward toward the second toe, causing the joint at its base to protrude outward. The bump that forms is actually an enlargement of bone and tissue around the joint, not simply a thickened bone as many people believe. Bunions can develop on one foot or both, and while some people experience significant pain and discomfort, others may have few or no symptoms despite visible deformity.
Understanding Bunion Development
Common Causes and Risk Factors
Bunions develop due to a combination of genetic and environmental factors. If your parents or grandparents had bunions, your risk of developing them is significantly higher. Genetics play a crucial role in determining foot structure and biomechanics, making some individuals more susceptible to bunion formation than others.
Wearing tight, narrow shoes with high heels, particularly over many years, can accelerate bunion development or worsen existing deformities. While shoes don’t cause bunions in people without genetic predisposition, they can contribute to progression in those with inherited foot structure vulnerabilities. Other contributing factors include inflammatory conditions like rheumatoid arthritis, which can trigger bunion formation more rapidly than typical age-related development.
Biomechanical Factors
The way your foot functions during walking and standing significantly influences bunion development. Excessive foot pronation, flat feet, or ligament laxity can all contribute to the alignment problems that lead to bunion formation. Additionally, some neuromuscular conditions affect muscle tone and foot control, increasing the likelihood of bunion development over time.
Recognizing Symptoms and Complications
Primary Symptoms
The most obvious sign of a bunion is the visible bony bump at the base of the big toe. However, symptoms extend beyond appearance. Many people experience:
- Pain and tenderness at the bunion site, especially when pressure is applied
- Redness, swelling, and warmth around the affected joint
- Limited movement of the big toe
- Corns or calluses developing between the first and second toes
- Pain that worsens with prolonged walking or standing
- Difficulty finding comfortable shoes that fit properly
Secondary Complications
Untreated bunions can lead to complications affecting other areas of your foot. The abnormal positioning of the big toe can cause the second toe to overlap or curl, leading to hammertoe. Some individuals develop metatarsalgia, pain in the ball of the foot, because bunions alter weight distribution during walking. Over time, arthritis may develop in the affected joint due to abnormal stress and movement patterns.
Non-Surgical Treatment Approaches
Conservative Management Strategies
For many people, especially those with mild to moderate bunions, non-surgical treatments can effectively manage pain and slow progression. The goal of conservative care is to reduce pain, prevent worsening, and maintain mobility rather than eliminate the bony bump itself.
Footwear Modifications
One of the most important non-surgical interventions is wearing appropriate shoes. Choose footwear with the following characteristics:
- Wide toe boxes that don’t compress the bunion
- Soft, stretchable materials that accommodate the deformity
- Adequate arch support to improve foot biomechanics
- Low heels (preferably one inch or less)
- Cushioned soles to absorb shock during walking
- Flexibility in the forefoot area
Avoiding tight, pointed shoes with high heels is essential for preventing bunion progression and managing symptoms. Some people find that custom-made shoes or having their regular shoes professionally stretched around the bunion area provides significant relief.
Padding and Protective Devices
Bunion pads and protective cushions reduce direct pressure on the bump and surrounding tissues. These can be applied directly to the bunion or placed inside shoes to minimize friction and irritation. Gel pads specifically designed for bunion relief are available at pharmacies and medical supply stores. Additionally, moleskin applied around the bunion can protect sensitive skin from shoe friction and reduce pain when walking.
Orthotics and Shoe Inserts
Custom orthotic devices are designed to correct foot alignment and improve biomechanics. Unlike over-the-counter arch supports, custom orthotics are specifically molded to your foot’s unique contours and movement patterns. They can help reduce abnormal stress on the bunion joint by improving overall foot function. Metatarsal pads, placed in the shoe under the ball of the foot, can redistribute pressure away from the bunion joint and relieve associated pain.
Physical Therapy and Exercises
Specific exercises and stretching routines can help maintain joint mobility and strengthen supportive muscles. Physical therapists often recommend:
- Big toe flexion and extension exercises to maintain range of motion
- Foot strengthening exercises to improve muscle support
- Calf stretches to reduce tension affecting foot mechanics
- Intrinsic foot muscle strengthening
- Balance and proprioception training
Regular physical therapy may slow bunion progression and help manage pain, particularly when combined with appropriate footwear and other conservative measures.
Medication and Anti-Inflammatory Options
Over-the-counter nonsteroidal anti-inflammatory medications can help manage pain and reduce inflammation during flare-ups. Topical creams and ointments may provide temporary pain relief when applied directly to the bunion. In some cases, healthcare providers may recommend corticosteroid injections into the joint to reduce inflammation and provide pain relief, though this is typically reserved for more severe symptoms.
Ice and Heat Therapy
Applying ice packs to the bunion for 15-20 minutes several times daily can reduce acute inflammation and pain. Heat therapy may be helpful for stiffness, particularly in the morning or after periods of inactivity. Many people find alternating between ice and heat provides optimal relief, depending on whether inflammation or stiffness is the primary issue.
Surgical Treatment Considerations
When Surgery Becomes Necessary
Surgery is typically considered when conservative treatments fail to provide adequate relief, the bunion significantly interferes with daily activities, or pain persists despite proper management. Surgery may also be recommended if the bunion is rapidly progressive or causing secondary foot problems like severe hammertoe.
Surgical Approaches
Several surgical techniques are available, and your orthopedic surgeon will recommend the most appropriate based on the severity of your bunion and individual foot characteristics. Common approaches include:
- Minimally invasive procedures that use small incisions and specialized instruments
- Traditional open surgery involving larger incisions for more complex corrections
- Arthroscopic procedures allowing visualization and treatment through small portals
- Joint-preserving surgeries that correct alignment without fusion
- Fusion procedures for severe or arthritic joints
Recovery and Outcomes
Recovery time varies depending on the surgical technique used. Minimally invasive procedures typically involve faster recovery, often allowing weight-bearing within days. Traditional surgery may require several weeks of protected weight-bearing and gradual return to normal activities. Complete healing and final results typically take several months. Most patients experience significant pain reduction and improved function following successful bunion surgery, though some residual swelling may persist for a year or longer.
Prevention and Long-Term Management
Preventive Strategies
While you cannot prevent bunions if genetics predispose you to them, you can take steps to delay onset or slow progression:
- Wear properly fitting shoes with adequate toe box space
- Avoid high heels and tight shoes whenever possible
- Maintain a healthy weight to reduce foot stress
- Stay physically active with low-impact exercises
- Perform regular foot stretches and strengthening exercises
- Address other foot problems promptly to prevent compensation patterns
Ongoing Foot Care
Regular monitoring of your bunion helps catch progression early. Keep your toenails trimmed straight across and avoid cutting into the corners. Moisturize your feet daily and check for signs of skin breakdown or infection, particularly between toes where corns or calluses may develop. Seeing a podiatrist or orthopedic surgeon periodically can help ensure your treatment plan remains appropriate for your condition.
Lifestyle Modifications and Self-Care
Daily Comfort Measures
Simple changes in your daily routine can significantly impact bunion-related pain. Elevating your feet while resting reduces swelling and discomfort. Taking breaks during prolonged standing or walking allows inflammatory responses to settle. Alternating shoes throughout the day prevents continuous pressure on the same area. Many people find that wearing sandals or open-toed shoes at home provides relief by eliminating shoe pressure entirely.
Activity Management
While you don’t need to avoid activity, modifying how you exercise can help manage symptoms. Low-impact activities like swimming, cycling, and elliptical training are generally more comfortable than running or high-impact sports. Properly fitting athletic shoes with good arch support are essential for anyone with bunions who exercises regularly. Gradually building intensity and duration helps prevent acute flare-ups that can set back progress.
Frequently Asked Questions
Q: Can bunions go away on their own?
A: No, bunions do not resolve spontaneously. However, with appropriate conservative treatment, many people manage symptoms effectively without surgery. The bony bump will not disappear without surgical intervention, but pain and progression can often be controlled through proper footwear, padding, orthotics, and other non-surgical methods.
Q: Are bunions hereditary?
A: Yes, genetics play a significant role in bunion development. If family members have bunions, your risk is considerably higher. However, having the genetic predisposition doesn’t guarantee you’ll develop bunions—environmental factors like footwear choices also influence whether and when they develop.
Q: Does surgery always solve bunion problems?
A: Surgery successfully reduces pain and improves function in most cases, but recurrence can occur in some people, particularly if underlying biomechanical issues aren’t addressed. Following post-operative care instructions and wearing appropriate shoes helps maximize long-term surgical success.
Q: Can children have bunions?
A: While bunions are more common in adults, children can develop them, especially if there’s a family history. Early intervention with appropriate footwear and conservative measures may help slow progression in younger individuals.
Q: How long does it take to recover from bunion surgery?
A: Recovery varies depending on the surgical technique. Minimally invasive procedures may allow weight-bearing within days, while traditional surgery requires several weeks of protected activity. Complete healing typically takes several months, with final results becoming apparent after six to twelve months.
Q: Are there exercises I can do to prevent bunions?
A: While exercises cannot prevent bunions in genetically predisposed individuals, strengthening and stretching exercises for the foot and lower leg can improve biomechanics and potentially slow progression. Regular foot care and appropriate footwear remain the most important preventive measures.
References
- Bunions (Hallux Valgus) — American Academy of Orthopaedic Surgeons (AAOS). 2024. https://orthoinfo.aaos.org/en/diseases–conditions/bunions-hallux-valgus/
- Foot and Ankle Health — American Podiatric Medical Association (APMA). 2024. https://www.apma.org/
- Conservative and Surgical Treatment of Hallux Valgus: A Systematic Review — Journal of Foot and Ankle Research, 2023. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10208289/
- Bunion Management: Conservative and Operative Approaches — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/bunions/diagnosis-treatment/drc-20350522
- Non-Surgical Treatment for Bunions and Bunionettes — News Medical Life Sciences. 2023. https://www.news-medical.net/health/Non-Surgical-Treatment-for-Bunions-and-Bunionettes.aspx
- Biomechanics of the Foot and Ankle: Normal and Pathological Function — University of Delaware Biomechanics Laboratory, Department of Health Sciences. 2022. https://www.udel.edu/
Read full bio of Sneha Tete













