Bursitis: Causes, Symptoms, and Effective Treatment
Complete guide to understanding bursitis: causes, symptoms, treatments, and prevention strategies.
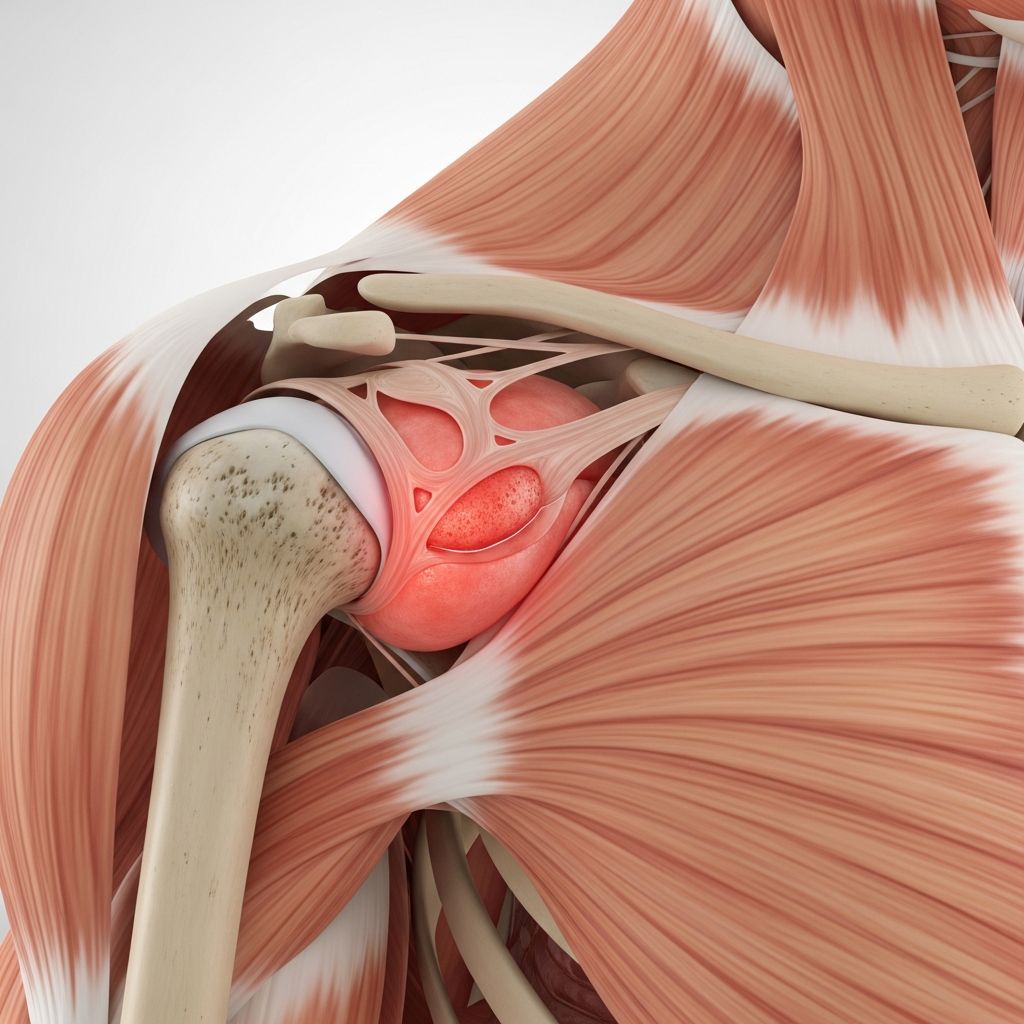
Bursitis is a painful condition that occurs when one or more of the small, fluid-filled sacs that help protect the joints become irritated or inflamed. These tiny cushions, known as bursae (the singular is bursa), are made up of a thin membrane that secretes a slick, jellylike substance. Understanding this common joint disorder is essential for proper management and recovery.
What Is a Bursa and How Does Bursitis Develop?
Bursae are fluid-filled sacs strategically located throughout the body near joints. They function as protective cushions between bones, tendons, and muscles, allowing the structures of joints—including bone, cartilage, and connective tissues—to glide over and around each other with minimal friction. When these sacs become irritated or injured, they can become inflamed, leading to the painful condition known as bursitis.
The inflammation causes characteristic symptoms including pain, swelling, tenderness, and redness in the affected area. In cases where bursitis is caused by bacterial infection, a fever may also develop.
Common Locations and Types of Bursitis
Bursitis can develop in various locations throughout the body, though certain sites are more commonly affected than others. The most frequent locations include:
- Shoulder bursitis – One of the most common forms, often resulting from repetitive overhead movements
- Elbow bursitis – Frequently associated with activities like tennis (tennis elbow)
- Hip bursitis – Often involves the iliopsoas bursa near the groin or trochanteric bursitis at the outer hip
- Knee bursitis – Common in people who kneel frequently (clergyman’s knee)
- Heel bursitis – Associated with Achilles tendon strain
Bursitis can be classified into two main categories based on cause: septic (infectious) bursitis and aseptic (nonseptic) bursitis. Septic bursitis occurs when bacteria directly invade the bursa, usually through punctured skin, and requires urgent treatment. Aseptic bursitis typically results from repeated minor trauma or strain injury.
Causes of Bursitis
Bursitis develops through various mechanisms, with overuse being the primary culprit. The most common causes include:
- Repetitive motion – Repeated movements or pressure on joints increase bursitis risk significantly
- Overuse injuries – Excessive use of a joint without adequate rest
- Physical trauma – Direct impact or injury to the joint area
- Changes in activity level – Sudden increases in exercise intensity, such as training for a marathon
- Bacterial infection – Introduction of bacteria through wounds in surrounding skin
- Underlying health conditions – Gout, rheumatoid arthritis, and scleroderma increase bursitis risk
- Being overweight – Excess weight increases stress on joints
Middle-aged men are particularly affected by bursitis, likely because they more commonly have jobs associated with greater bursitis risk.
Recognizing the Symptoms of Bursitis
Bursitis presents with characteristic symptoms that vary depending on severity and location. Key symptoms include:
- Pain that increases with movement or pressure on the affected area
- Tenderness, even without movement
- Swelling and inflammation
- Loss of movement or limited mobility
- Reddening of the skin over the affected joint
In cases of septic (infectious) bursitis, additional symptoms develop:
- Fever and chills
- Skin discoloration in the affected area
- The affected area feeling hot to the touch
When to Seek Medical Attention
While many people successfully treat bursitis at home, certain symptoms warrant professional medical evaluation:
- Joint pain that prevents all movement
- Pain lasting longer than 2 weeks
- Sharp, shooting pains
- Excessive swelling, bruising, or skin discoloration
- Fever or signs of infection
If rest and anti-inflammatory measures don’t help after a reasonable period, it’s important to consult with a healthcare provider.
Diagnosis of Bursitis
Doctors typically diagnose bursitis through physical examination and imaging studies. If a bacterial infection is suspected, the healthcare provider may perform a bursal fluid analysis by drawing a small fluid sample from the affected area and sending it to a laboratory for testing to identify bacteria and crystal deposits. This diagnostic approach ensures appropriate treatment selection, particularly when infection may be present.
Treatment Options for Bursitis
Treatment focuses on taking steps to ease inflammation and restore function. The approach varies depending on severity and underlying causes.
Conservative Home Treatment
For most cases of bursitis, conservative measures prove highly effective:
- Rest – Taking a break from the activity that caused bursitis is crucial for recovery
- Ice application – Cold packs help reduce swelling and pain
- Over-the-counter pain relievers – NSAIDs such as ibuprofen, naproxen, and aspirin reduce swelling and manage pain effectively
- Supportive devices – Wearing a brace or splint supports the joint and helps reduce inflammation
- Gentle physical therapy – A gentle stretching program, along with easy strengthening exercises, aids recovery
- Home exercises – Exercises designed to build strength and maintain joint mobility as pain subsides
The positive news is that bursitis often resolves over the course of a few weeks with proper rest and anti-inflammatory care.
Medical Treatments
When conservative treatment proves insufficient, healthcare providers may recommend:
Corticosteroid Injections
Cortisone injections offer quick relief from pain and inflammation when pain persists despite rest and anti-inflammatories. The doctor may inject steroids into the affected area to relieve symptoms by blocking a chemical in the body called prostaglandin, which causes inflammation. However, doctors prescribe steroids with care, as these drugs may raise blood pressure and increase infection risk with prolonged use.
Antibiotics
If a fluid test confirms a bacterial infection, doctors prescribe antibiotics to eliminate the infection. They generally recommend oral antibiotics, though more severe cases may require intravenous administration. Antibiotics are particularly important for septic bursitis cases and are often sufficient to resolve the condition.
Surgical Intervention
In rare instances, surgery becomes necessary. If bursitis doesn’t improve or recurs despite treatment, the affected bursa is usually surgically removed. Additionally, in cases where bursitis is caused by bacterial infection, surgery may be more urgently recommended to drain the affected bursa. Surgery is also considered when the inflammation becomes chronic and other treatments have failed.
Recovery Timeline and Prognosis
The recovery timeline for bursitis varies based on treatment adherence and underlying conditions. If the area is properly rested, inflammation usually resolves within 2 to 3 weeks. However, some factors may extend recovery or increase the likelihood of chronicity:
- Continued activity that caused the initial injury
- Chronic diseases such as diabetes and rheumatoid arthritis
- Underlying health problems that cannot be cured
- Inadequate initial diagnosis and treatment
Your condition will likely improve with appropriate treatment, though bursitis can become chronic in some cases.
Prevention Strategies
Preventing bursitis is more effective than treating it. People can help prevent bursitis through several practical strategies:
- Protect vulnerable joints – Use proper padding and protective equipment during activities prone to joint stress
- Take breaks during repetitive tasks – Regularly pause to rest joints during activities involving repetitive movements
- Maintain a moderate weight – Excess weight increases stress on joints, particularly in the lower body
- Avoid repetitive movements – When possible, modify activities or techniques to reduce joint strain
- Practice proper posture and body mechanics – Using correct technique during work and exercise reduces injury risk
- Warm up and stretch properly – Adequate warm-up and stretching improve joint flexibility and resilience
- Gradually increase activity levels – Avoid sudden increases in exercise intensity or duration
Frequently Asked Questions
Q: How long does bursitis typically last?
A: Most cases of bursitis resolve within 2 to 3 weeks with proper rest and anti-inflammatory treatment. However, chronic cases may persist longer, especially if the underlying cause isn’t addressed or if the person continues the activity that caused it.
Q: Can bursitis be prevented?
A: Yes, bursitis can often be prevented by protecting vulnerable joints, taking breaks during repetitive tasks, maintaining a moderate weight, and using proper technique during activities that stress joints.
Q: Is bursitis ever serious?
A: Most cases of bursitis are not serious and respond well to conservative treatment. However, septic (infectious) bursitis requires prompt medical attention and antibiotics. Any case with fever, severe swelling, or pain preventing movement should be evaluated by a healthcare provider.
Q: Can I exercise with bursitis?
A: During acute bursitis, rest is essential. As pain subsides, gentle exercises and physical therapy help maintain joint mobility and build strength. Your healthcare provider can recommend appropriate exercises for your specific situation.
Q: What’s the difference between bursitis and tendinitis?
A: Bursitis involves inflammation of the bursa (fluid-filled sac), while tendinitis involves inflammation of the tendon itself. Both cause joint pain but may require different treatment approaches.
Q: Are there natural remedies for bursitis?
A: While conventional treatments like NSAIDs and rest are most effective, some people find relief through ice therapy, elevation, and gentle stretching. However, persistent bursitis requires professional medical evaluation and treatment.
References
- Bursitis pain comes from inflammation of bursae — UCLA Health. Accessed January 2026. https://www.uclahealth.org/news/article/bursitis-pain-comes-inflammation-bursae
- Overview: Bursitis — NCBI Bookshelf, InformedHealth.org. Accessed January 2026. https://www.ncbi.nlm.nih.gov/books/NBK525773/
- Bursitis: symptoms and treatment — Healthdirect. Accessed January 2026. https://www.healthdirect.gov.au/bursitis
- Bursitis: Types, treatment, and symptoms — Medical News Today. Accessed January 2026. https://www.medicalnewstoday.com/articles/152120
- Bursitis — MedlinePlus Medical Encyclopedia, U.S. National Library of Medicine. Accessed January 2026. https://medlineplus.gov/ency/article/000419.htm
- Bursitis: Symptoms, Types, Treatment & More — Healthline. Accessed January 2026. https://www.healthline.com/health/bursitis
Read full bio of medha deb











