Bursitis: Causes, Symptoms, and Treatment Options
Complete guide to understanding bursitis, its causes, symptoms, and effective treatment strategies.
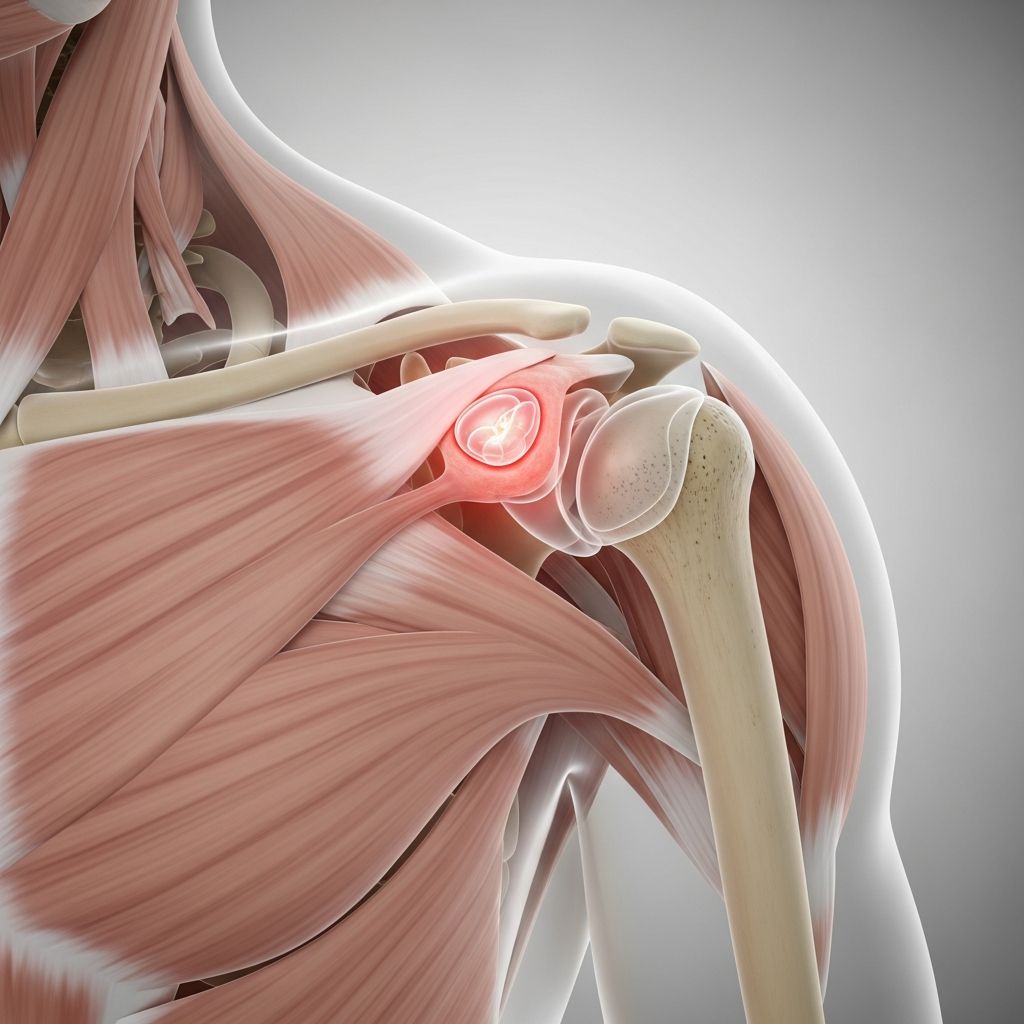
What is Bursitis?
Bursitis is a common condition characterized by inflammation of a bursa, which is a small, closed, fluid-filled sac located near joints throughout the body. These bursae serve as cushions that reduce friction between bones, tendons, ligaments, and muscles during movement. When a bursa becomes inflamed, it can cause pain, swelling, and limited mobility in the affected area. Bursitis is one of the most prevalent soft tissue pain conditions and can affect individuals of all ages, though it is particularly common in adults and athletes who engage in repetitive motions.
Understanding the Anatomy of Bursae
The human body contains approximately 150 bursae distributed throughout various joints and areas where friction is likely to occur. These fluid-filled sacs are lined with synovial membranes that produce lubricating fluid, allowing smooth movement between tissues. The largest and most commonly affected bursae include those in the shoulders, elbows, hips, and knees. Each bursa is strategically positioned to absorb shock and facilitate movement, making them essential components of joint function. When these protective structures become irritated or inflamed, they can significantly impact daily activities and quality of life.
Common Types of Bursitis
Bursitis can develop in various locations throughout the body, with certain types being more prevalent than others. The most common types include:
- Shoulder bursitis: Affects the subacromial bursa, often caused by overhead activities or repetitive arm movements
- Elbow bursitis: Involves the olecranon bursa, commonly seen in athletes and individuals who lean on their elbows frequently
- Hip bursitis (Trochanteric bursitis): Affects the trochanteric bursa and is particularly common in runners and those with hip pain
- Knee bursitis (Prepatellar bursitis): Develops in the prepatellar bursa, often occurring in individuals who kneel frequently
- Achilles bursitis: Affects the bursa near the Achilles tendon, common in runners and individuals with tight calf muscles
Causes of Bursitis
Bursitis develops through various mechanisms, and understanding the underlying causes is essential for prevention and treatment. The primary causes include repetitive motion, direct trauma, and prolonged pressure on affected areas. Individuals who engage in activities requiring repetitive joint movements, such as throwing, painting, or typing, face an increased risk of developing bursitis. Direct impact or injury to the joint can cause acute inflammation of the bursa, while prolonged pressure from kneeling or leaning can trigger chronic bursitis.
Age-related changes also contribute to bursitis development. As individuals age, bursae can become less resilient and more susceptible to inflammation. Certain medical conditions, such as rheumatoid arthritis, gout, and diabetes, increase the risk of bursitis. Additionally, poor posture, muscle imbalances, and inadequate flexibility can predispose individuals to this condition. Infections can also cause septic bursitis, though this is less common than aseptic forms of the condition.
Symptoms and Diagnosis
The symptoms of bursitis vary depending on the location and severity of inflammation. Common symptoms include localized pain, swelling, redness, and warmth around the affected joint. Movement may be restricted or limited, and the discomfort can range from mild to severe. In some cases, patients experience stiffness, particularly after periods of rest or inactivity.
Diagnosis of bursitis typically begins with a thorough physical examination and medical history. Healthcare providers assess the location of pain, range of motion, and any triggering factors. Imaging studies such as ultrasound or magnetic resonance imaging (MRI) may be ordered to confirm inflammation and rule out other conditions. For suspected septic bursitis, aspiration of the bursal fluid may be performed to identify any infectious organisms and guide antibiotic treatment.
Acute, Chronic, and Infected Bursitis Presentations
Bursitis presents in three distinct clinical presentations, each requiring different management approaches. Acute bursitis typically develops suddenly following trauma or injury and is characterized by rapid onset of pain and swelling. This form often responds well to early intervention with aspiration, compression, and protective padding. Chronic nonseptic bursitis develops gradually over time, usually from repetitive activities or ongoing irritation, and generally responds to conservative therapy including physical therapy, anti-inflammatory medications, and occasional aspiration or corticosteroid injection.
Chronic infected, or septic, bursitis represents a more serious condition requiring aggressive evaluation and treatment. These inflamed bursae must be carefully assessed, as some may require aspiration and decompression with concurrent oral or intravenous antibiotics to prevent systemic infection. While incision and drainage is rarely necessary, it may be indicated for injuries that do not respond to initial conservative management.
Treatment Options
The treatment approach for bursitis depends on the type, severity, and duration of the condition. Most patients benefit significantly from conservative, noninvasive treatments. However, those who do not experience sufficient pain relief from conservative options such as physical therapy and over-the-counter medications may require additional interventions.
Conservative Treatment Approaches
Conservative management represents the first-line treatment for most bursitis cases and is often highly effective. These approaches include:
- Rest and activity modification to reduce stress on the affected bursa
- Ice application during the acute phase to reduce inflammation and swelling
- Compression using elastic bandages or wraps to minimize fluid accumulation
- Elevation of the affected limb to reduce swelling
- Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) to manage pain and inflammation
- Physical therapy and stretching exercises to improve flexibility and strengthen surrounding muscles
- Posture correction and ergonomic adjustments to prevent recurrence
Corticosteroid Injections
For patients whose symptoms persist despite conservative treatment, corticosteroid injections represent an effective intermediate option. Studies show that symptom resolution and return to activity with corticosteroid injection as the primary treatment modality ranges from 49% to 100%, particularly when combined with multimodal conservative therapy. Most patients require only a single injection, though approximately one-third may need a second administration, and some require multiple injections for sustained relief. These injections are generally well-tolerated with minimal complications, though occasional side effects such as temporary skin irritation or localized pain may occur.
Shock Wave Therapy
Low-energy shock-wave therapy (SWT) has emerged as a valuable alternative for patients who fail conventional nonoperative management. Research indicates that SWT demonstrates superior results compared to corticosteroid injection and home therapy alone, making it an attractive option for those seeking less invasive alternatives to surgery. This technology continues to evolve, with emerging research exploring innovative engineering solutions to improve treatment effectiveness and reduce patient pain duration.
Surgical Interventions
Surgical treatment becomes necessary for refractory cases that do not respond to conservative and minimally invasive approaches. Multiple surgical options have been documented, including bursectomy, longitudinal release of the iliotibial band, proximal or distal Z-plasty, osteotomy, and repair of gluteus medius tears. Surgical techniques have demonstrated superior outcomes compared to corticosteroid therapy and physical therapy according to various clinical outcome measures. For elbow and knee bursitis specifically, surgical excision of the bursa is recommended only for recalcitrant cases that fail conservative management.
Treatment Efficacy and Comparison
Research systematically evaluating treatment efficacy reveals important insights for clinical decision-making. According to validated outcome measures, treatment efficacy is ranked in ascending order: home therapy only, multimodal conservative therapy including injection, injection alone, bursectomy alone, low-energy shock-wave therapy, longitudinal iliotibial band release, proximal Z-plasty, and distal Z-plasty. This evidence-based hierarchy helps healthcare providers and patients make informed decisions about which interventions are most likely to provide relief.
Managing Refractory Bursitis
When bursitis becomes refractory to standard treatments, more aggressive approaches are warranted. Recurrence of symptoms is common, and patients may undergo multiple courses of nonoperative treatment, experiencing only temporary and incomplete pain relief. For these challenging cases, surgical options provide more durable relief. The least invasive surgical approach is endoscopic bursectomy, while more invasive options include open osteotomy. The choice of surgical technique depends on the specific location, underlying pathology, and patient factors.
Prevention Strategies
Preventing bursitis is more effective than treating it. Key prevention strategies include maintaining proper posture and ergonomic positioning during daily activities and work. Regular stretching and flexibility exercises help maintain joint mobility and reduce stress on bursae. Strengthening exercises targeting muscles around affected joints provide additional support and stability. Gradually increasing activity levels rather than sudden changes helps prevent overuse injuries. Wearing appropriate protective equipment during sports and activities, taking frequent breaks during repetitive tasks, and maintaining a healthy weight all contribute to bursitis prevention.
When to Seek Medical Attention
While many cases of bursitis resolve with home care, certain symptoms warrant professional medical evaluation. Severe pain that significantly limits function, swelling accompanied by redness and warmth suggesting infection, or symptoms persisting beyond two weeks despite conservative treatment should prompt a healthcare provider visit. Additionally, if you have concerns about underlying conditions such as arthritis or if you experience recurrent bursitis episodes, professional assessment is recommended.
Frequently Asked Questions
Q: How long does bursitis typically last?
A: Most cases of bursitis resolve within weeks to months with appropriate conservative treatment. However, some individuals experience recurrent symptoms or persistent inflammation requiring more aggressive intervention.
Q: Can bursitis cause permanent damage?
A: While bursitis is typically not permanently damaging, chronic or untreated cases may lead to complications such as reduced joint function or chronic pain. Prompt treatment generally prevents long-term complications.
Q: Is bursitis related to arthritis?
A: While bursitis and arthritis are distinct conditions affecting different joint structures, individuals with arthritis have an increased risk of developing bursitis due to underlying joint inflammation.
Q: Can I exercise with bursitis?
A: Gentle movement and appropriate physical therapy exercises can be beneficial, but high-impact activities causing pain should be avoided. Consult your healthcare provider or physical therapist for appropriate exercise recommendations.
Q: What is the difference between bursitis and tendinitis?
A: Bursitis involves inflammation of a bursa (fluid-filled sac), while tendinitis involves inflammation of a tendon (tissue connecting muscle to bone). These conditions can coexist but require similar conservative treatment approaches.
Q: Are there any complications from corticosteroid injections?
A: Corticosteroid injections are generally safe with minimal complications. Rare side effects may include temporary increased pain, skin irritation, or infection at the injection site.
References
- Evaluation of current bursitis treatments and directions for future treatment technology — Johns Hopkins University, Department of Biomedical Engineering. 2024. https://www.bme.jhu.edu/hello-world/evaluation-of-current-bursitis-treatments-and-directions-for-future-treatment-technology/
- Efficacy of Treatment of Trochanteric Bursitis: A Systematic Review — Clinical Journal of Sport Medicine, National Center for Biotechnology Information. 2011. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3689218/
- Olecranon and Prepatellar Bursitis: Treating Acute, Chronic, and Infected Presentations — The Physician and Sportsmedicine, Johns Hopkins University. 2000. https://pure.johnshopkins.edu/en/publications/olecranon-and-prepatellar-bursitis-treating-acute-chronic-and-inf-4/
- Johns Hopkins Arthritis Center: Bursitis and Tendinitis — Johns Hopkins Medicine. 2024. https://www.hopkinsarthritis.org/ask-the-expert-topic/bursitis-and-tendinitis/
Read full bio of Sneha Tete











