Carotid Endarterectomy: Procedure, Benefits & Recovery
Learn about carotid endarterectomy surgery, its benefits, risks, and recovery process for stroke prevention.
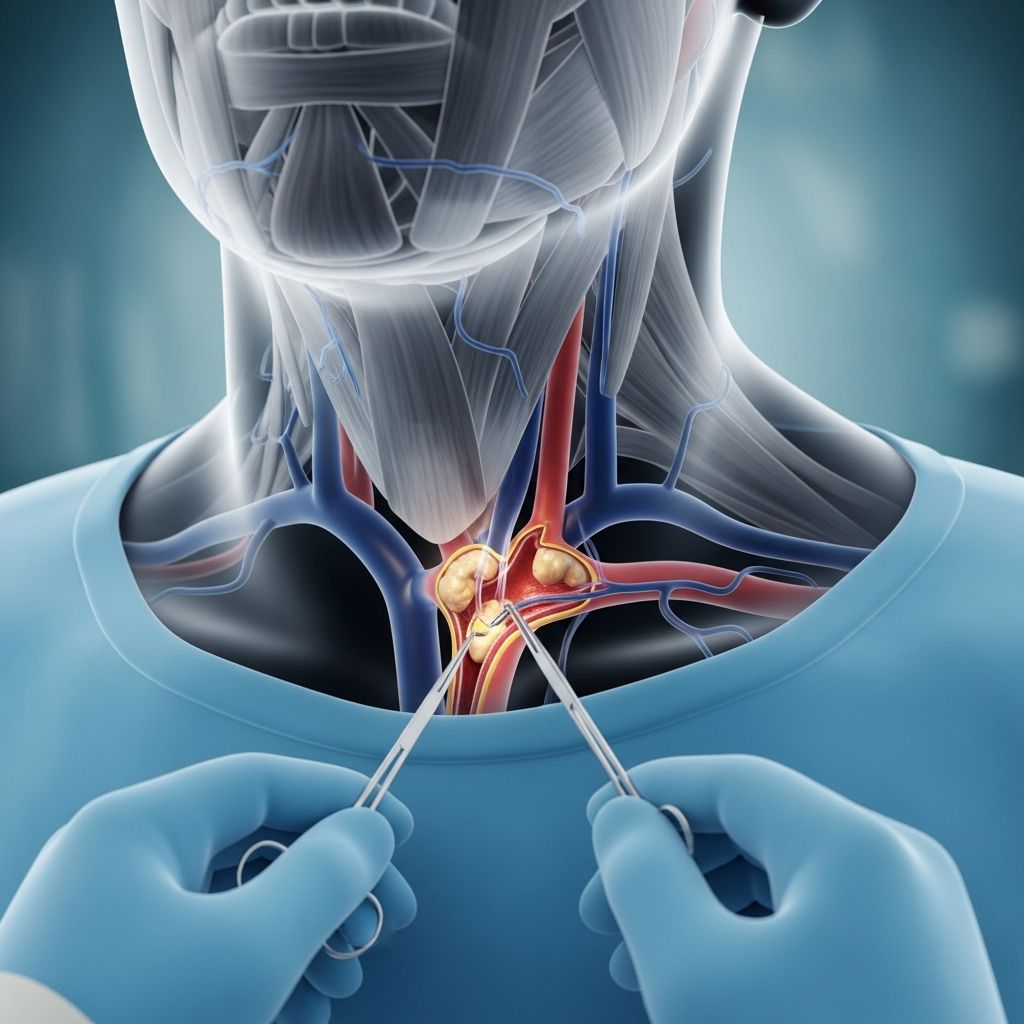
Carotid Endarterectomy: Understanding the Procedure
Carotid endarterectomy is a surgical procedure designed to remove fatty plaque buildup from the carotid arteries, the major blood vessels on either side of the neck that supply oxygen-rich blood to the brain. When plaque accumulates in these arteries—a condition known as atherosclerosis or carotid artery disease—it can significantly narrow the vessel and restrict blood flow to the brain. This narrowing, called stenosis, substantially increases your risk of stroke and transient ischemic attack (TIA), also known as a mini-stroke. By removing this plaque buildup, carotid endarterectomy improves blood flow and reduces the likelihood of experiencing a stroke or other cerebrovascular complications.
Why Carotid Endarterectomy Is Performed
Your healthcare provider may recommend carotid endarterectomy if you have significant narrowing in one or both of your carotid arteries. The decision to proceed with surgery considers several important factors beyond just the degree of blockage. These factors include whether you have experienced stroke symptoms, the severity of your condition, your overall health status, and your ability to tolerate surgery.
The primary goal of this procedure is to prevent stroke in patients with known carotid artery disease. Research has demonstrated that removing plaque from narrowed carotid arteries can substantially reduce stroke risk, particularly in patients who have already experienced symptoms such as transient ischemic attack or minor stroke.
How the Procedure Works
Carotid endarterectomy is performed by a vascular surgeon in a hospital setting under either local anesthesia with sedation or general anesthesia. The surgical technique has evolved since carotid artery reconstructions began in the early 1950s, and modern procedures are highly refined and effective.
Traditional Surgical Technique
During the traditional carotid endarterectomy approach, your surgeon follows these key steps:
- Makes an incision along the front or side of your neck, typically 2 to 3 inches long
- Carefully dissects through the skin, fat, and muscle layers to expose the carotid artery
- Places clamps above and below the plaque to temporarily stop blood flow through the artery
- Inserts a small flexible bypass tube called a shunt to divert blood flow around the surgical site, ensuring your brain continues to receive adequate blood supply during the procedure
- Opens the carotid artery along its length to fully visualize the plaque deposits
- Carefully removes the plaque from the inner lining of the artery
- Uses ultrasound Doppler or angiography to confirm adequate blood flow has been restored
- Closes the artery with stitches or reinforces it with a patch made from vein tissue or synthetic material to prevent future narrowing
- Removes the shunt and releases the clamps
- Closes the incision with stitches
Eversion Technique
An alternative surgical approach called eversion carotid endarterectomy offers some distinct advantages. In this technique, the surgeon completely transects or cuts the internal carotid artery at its origin where it branches from the common carotid artery. The vessel is then turned inside out circumferentially around the plaque, and the plaque is carefully divided and removed. The artery is then reattached in an end-to-end fashion.
The eversion method offers several benefits compared to the traditional approach. It eliminates the need for a patch closure, typically requires shorter carotid clamping time, and results in a shorter overall operative time. These advantages may translate to reduced surgical stress and potentially faster recovery for some patients.
Benefits of Carotid Endarterectomy
The primary benefit of carotid endarterectomy is significant stroke risk reduction. For patients with symptomatic carotid artery disease—meaning they have already experienced symptoms like TIA or minor stroke—this procedure can reduce the risk of future stroke by approximately 50% or more over two years.
Additional benefits include:
- Improved cerebral blood flow, which may enhance brain function and cognitive performance
- Prevention of embolic events, where plaque fragments break off and travel to the brain
- Restoration of more normal blood circulation patterns
- Potential improvement in symptoms if you have experienced transient ischemic attacks
- Durable, long-term results that can provide stroke protection for many years
Risks and Complications
Like all surgical procedures, carotid endarterectomy carries some risks, though serious complications are relatively uncommon when performed by experienced surgeons. Understanding these potential risks helps you make an informed decision about your treatment:
- Stroke: In rare cases, plaque may break free during surgery or blood clots may form, potentially causing a stroke during or after the procedure
- Transient ischemic attack (TIA): Temporary neurological symptoms may occur if small emboli reach the brain
- Nerve injury: Surgical manipulation may temporarily or permanently damage nerves controlling facial muscles, tongue, or shoulder movement
- Bleeding or hematoma: Accumulation of blood under the surgical site may require drainage
- Infection: Although uncommon, surgical site infections can occur
- Blood pressure changes: Temporary fluctuations in blood pressure may occur after surgery
- Myocardial infarction: Heart attack risk exists, particularly in patients with significant cardiac disease
- Restenosis: The artery may narrow again over time, though this is relatively uncommon
Your surgeon will discuss your individual risk factors and how they apply to your specific situation. Most patients tolerate the procedure well, and in studies of even elderly patients over 80 years old, the majority were alive five years after the procedure.
Who Is a Good Candidate
Ideal candidates for carotid endarterectomy typically have:
- Significant narrowing (typically 70% or greater) of a carotid artery
- Symptoms related to their carotid disease, such as TIA or minor stroke
- Good overall health and ability to tolerate surgery
- No major contraindications to surgery
- Reasonable life expectancy to benefit from stroke prevention
Your healthcare team will conduct a thorough evaluation including imaging studies, blood work, and cardiac assessment to determine whether you are an appropriate candidate.
Alternative Treatments
While carotid endarterectomy is considered the standard treatment for carotid stenosis, alternative approaches may be appropriate for certain patients:
Carotid Angioplasty
In carotid angioplasty, a surgeon inserts a long, hollow tube called a catheter through an artery, typically in the groin, and guides it to the narrowed carotid artery. A filter is placed to catch any debris that might break loose during the procedure. A tiny balloon at the catheter tip is then inflated to open the narrowed area. This minimally invasive procedure may be appropriate for selected patients.
Carotid Stenting
Carotid stenting is another minimally invasive alternative that uses a catheter to place a small wire mesh coil, called a stent, into the narrowed vessel to keep it open. This approach may be recommended for patients at high risk for traditional surgery or those with repeat narrowing after previous endarterectomy. The catheter is removed after stent placement, and a filter that caught any debris is also removed.
What to Expect Before Surgery
Before your carotid endarterectomy, you will undergo several pre-operative tests and evaluations to ensure you are ready for surgery. These may include blood work, an electrocardiogram to assess heart function, and imaging studies such as ultrasound, CT, or MRI to confirm the extent of your carotid artery narrowing. Your surgeon will review your medications and may ask you to stop taking certain medications before surgery, particularly blood thinners.
You will receive detailed instructions about fasting before surgery, typically requiring you to avoid food and drink for several hours before your procedure. Plan to have someone available to drive you home from the hospital, as you will not be able to drive immediately after surgery.
What to Expect During Surgery
On the day of your procedure, you will arrive at the hospital and undergo final pre-operative preparations. An intravenous line will be placed, and you will be taken to the operating room. If you are receiving general anesthesia, you will be put into a sleep-like state. If local anesthesia is used, you will be awake but the surgical site will be numbed.
Your surgeon will make an incision along your neck and carefully expose the carotid artery. After taking measures to protect your brain from inadequate blood flow, your surgeon will open the artery and remove the plaque. The artery will be repaired with stitches or a patch, and your incision will be closed. The entire procedure typically takes one to two hours.
Recovery and Aftercare
Most patients are able to return home the day after their carotid endarterectomy procedure, making this a relatively quick recovery compared to many surgical procedures. However, complete healing takes several weeks.
Hospital Stay
You will spend at least one night in the hospital for monitoring. Nurses will check your vital signs regularly and monitor for any complications. You may experience some mild pain or discomfort at the surgical site, which can be managed with prescribed pain medications.
Activity Restrictions
During the first week after surgery, you should avoid strenuous activity, heavy lifting, and vigorous exercise. Gradually resume normal activities as tolerated, typically over two to four weeks. Your surgeon will provide specific guidance based on your individual situation.
Wound Care
Keep your surgical incision clean and dry. You may shower once the incision has healed sufficiently, typically after a few days. Avoid submerging the incision in water until it is completely healed. Watch for signs of infection such as increasing redness, swelling, warmth, drainage, or fever, and report these to your surgeon immediately.
Medication Management
Continue taking all prescribed medications as directed. Your surgeon may prescribe aspirin or other antiplatelet medications to prevent blood clots and reduce the risk of restenosis. Blood pressure and cholesterol medications are typically continued or prescribed if not already being taken.
Follow-up Care
You will have follow-up appointments with your surgeon at intervals after your procedure to monitor your recovery and ensure adequate healing. Your surgeon may order imaging studies such as ultrasound to confirm that your carotid artery remains adequately open and free from new plaque buildup.
Long-Term Outcomes
Carotid endarterectomy provides durable, long-term stroke risk reduction for most patients. Studies demonstrate that the benefits of the procedure persist for many years. Maintaining a healthy lifestyle, including regular exercise, a heart-healthy diet, smoking cessation if applicable, and control of blood pressure and cholesterol levels, will help optimize your long-term outcomes.
Frequently Asked Questions
Q: How long does the carotid endarterectomy procedure take?
A: The procedure typically takes one to two hours, depending on the complexity of your case and which surgical technique is used.
Q: Can carotid endarterectomy be performed on both sides of the neck?
A: While bilateral procedures are possible, surgeons typically perform one side at a time, allowing adequate recovery time between procedures if both sides require treatment.
Q: What is the success rate of carotid endarterectomy?
A: Success rates are high when performed by experienced surgeons, with most patients experiencing significant stroke risk reduction. Serious complications occur in less than 2-3% of cases at high-volume centers.
Q: Will my carotid artery narrow again after surgery?
A: Restenosis, or re-narrowing of the artery, occurs in a small percentage of patients but is relatively uncommon when the procedure is performed correctly and you maintain healthy lifestyle habits.
Q: Can I return to normal activities after recovery?
A: Yes, most patients return to their normal activities within a few weeks after surgery. Your surgeon will provide specific recommendations based on your individual circumstances.
Q: Is carotid endarterectomy covered by insurance?
A: Most insurance plans cover carotid endarterectomy when it is medically necessary. Contact your insurance provider to understand your specific coverage.
Q: What happens if I don’t have carotid endarterectomy?
A: Without treatment, patients with significant carotid narrowing remain at increased risk for stroke. Your doctor will discuss your individual risk factors and recommend appropriate management strategies.
References
- Carotid Endarterectomy — National Center for Biotechnology Information (NCBI), National Library of Medicine. 2025. https://www.ncbi.nlm.nih.gov/books/NBK470582/
- Carotid Endarterectomy — Mayo Clinic. 2024. https://www.mayoclinic.org/tests-procedures/carotid-endarterectomy/about/pac-20393379
- Carotid Endarterectomy: Surgery & Recovery — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/treatments/16849-carotid-endarterectomy
- Carotid Endarterectomy Overview — Brigham and Women’s Hospital. 2024. https://www.brighamandwomens.org/neurosurgery/cerebrovascular/carotid-endarterectomy
- Carotid Endarterectomy — Kaiser Permanente Health Encyclopedia. 2024. https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.carotid-endarterectomy.hw224563
Read full bio of Sneha Tete













