Cauda Equina Syndrome: Causes, Symptoms & Treatment
Learn about cauda equina syndrome: a medical emergency affecting lower back nerves requiring urgent surgical intervention.
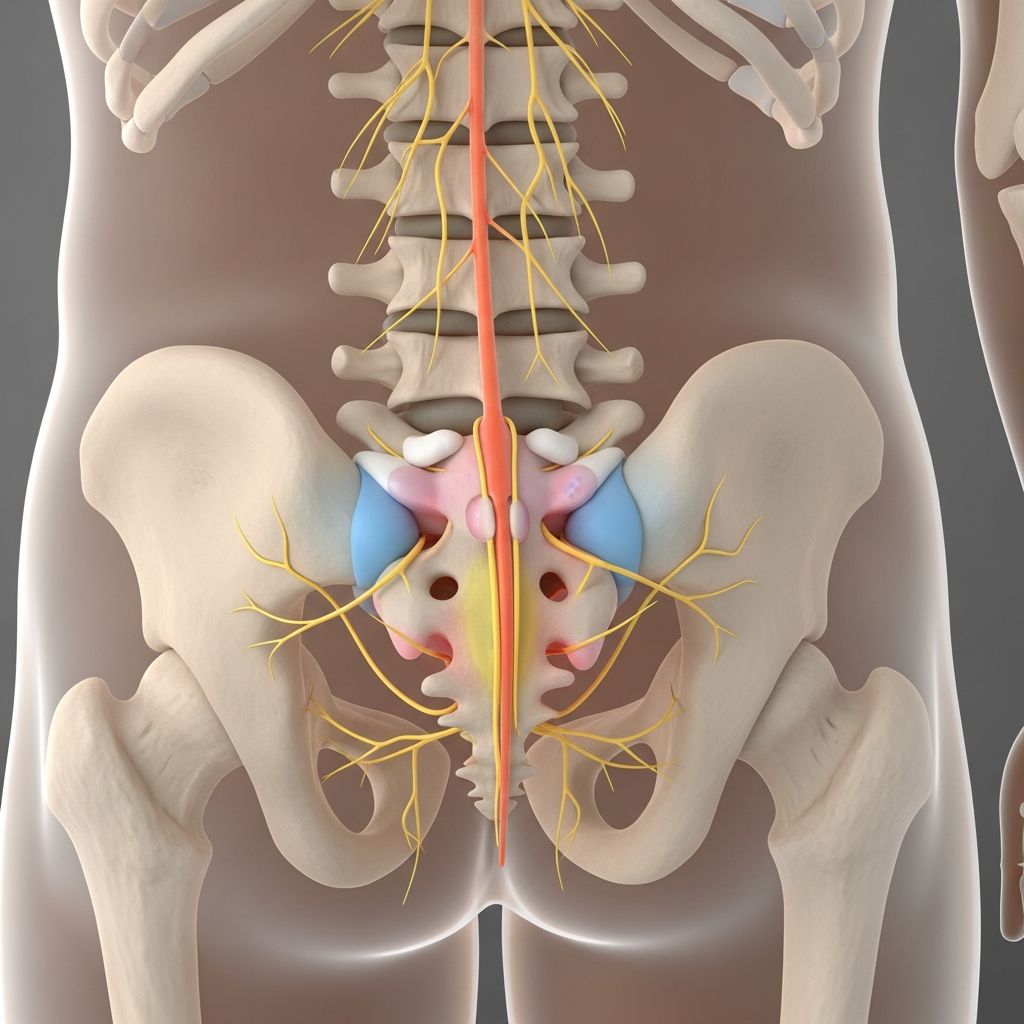
Cauda Equina Syndrome: Understanding This Spinal Emergency
Cauda equina syndrome (CES) represents a serious neurological condition that demands immediate medical attention and urgent intervention. The term “cauda equina” derives from Latin, meaning “horse’s tail,” which accurately describes the appearance of the bundle of nerves and nerve roots located at the base of the spinal cord in the lumbar region. When these vital nerve structures become compressed or severely irritated, they can no longer function properly, leading to a cascade of potentially devastating complications affecting motor function, sensation, and bodily control.
This condition is classified as a medical and surgical emergency because the window for effective treatment is extremely narrow. Research demonstrates that surgical intervention within 48 hours of symptom onset provides the most favorable outcomes and the best chance of preventing permanent neurological damage. Understanding the signs, symptoms, causes, and treatment options for cauda equina syndrome is essential for anyone experiencing lower back problems or those concerned about their spinal health.
What Is Cauda Equina Syndrome?
The cauda equina consists of a bundle of nerve roots that extend from the lumbar spine, specifically from the L1 through L5 vertebral levels. These nerves are responsible for transmitting motor and sensory signals to the legs, pelvis, and lower abdominal organs, including the bladder and bowel. When significant compression occurs in the spinal canal, these nerve roots cannot transmit signals effectively, resulting in a range of neurological symptoms and functional impairments.
True cauda equina syndrome is a relatively rare condition, but its rarity does not diminish its severity. The potential for permanent disability makes early recognition and treatment absolutely critical. Without prompt intervention, individuals may face irreversible consequences including permanent paralysis of the lower extremities, loss of bladder and bowel control, and chronic pain syndromes that significantly impact quality of life.
Causes of Cauda Equina Syndrome
Cauda equina syndrome develops through compression of the nerve roots in the lumbar spine. Multiple conditions can trigger this compression, though certain causes are more prevalent than others:
Primary Causes
Herniated Lumbar Disc: This represents the most common cause of cauda equina syndrome, accounting for approximately 45 percent of all CES cases. When the soft inner material of an intervertebral disc protrudes through the outer fibrous ring, it can compress multiple nerve roots simultaneously.
Spinal Stenosis: Progressive narrowing of the spinal canal can gradually compress nerve roots. In some cases, this process occurs rapidly enough to trigger cauda equina syndrome.
Spinal Tumors or Lesions: Cancerous or benign growths can expand within the spinal canal, compressing nerve structures.
Spinal Infections and Inflammation: Conditions such as meningitis, epidural abscess, or discitis (inflammation of the spinal discs) can cause swelling that compresses nerve roots.
Trauma or Injury: Direct injury to the lower spine from falls, accidents, or sports-related trauma can cause disc herniation or other structural damage leading to nerve compression.
Postoperative Complications: In rare cases, complications arising from previous spinal surgeries can result in cauda equina syndrome development.
Less Common Causes
Additional causes include aortic obstruction, blood clots in the vena cava, vertebral implant complications, and in rare instances, complications from chiropractic manipulation.
Risk Factors for Developing Cauda Equina Syndrome
Certain characteristics and medical conditions increase the likelihood of developing cauda equina syndrome:
Congenital spinal abnormalities: People born with structural spine anomalies face increased risk. Previous herniated lumbar discs: History of disc herniation significantly elevates risk. Prior spinal surgeries: Previous surgical interventions on the spine can predispose individuals to CES. Spinal infections: A history of spinal infections increases vulnerability. Existing spinal tumors: Patients with diagnosed tumors require careful monitoring. Trauma history: Previous traumatic injuries to the spine increase susceptibility.
Recognizing the Symptoms of Cauda Equina Syndrome
Cauda equina syndrome presents with a distinctive constellation of symptoms that require immediate medical evaluation. Recognizing these warning signs is crucial for seeking emergency care:
Primary Symptoms
Severe Lower Back Pain and Sciatica: Intense pain in the lower back and radiating pain down one or both legs is a hallmark symptom.
Bladder and Bowel Dysfunction: One of the most significant warning signs includes urinary retention (inability to empty the bladder despite it being full) or urinary incontinence (loss of bladder control). Fecal incontinence or constipation may also occur.
Saddle Anesthesia: Loss of sensation in areas that would contact a saddle, including the inner thighs, buttocks, genital region, and perineal area, represents a red flag symptom.
Bilateral Leg Weakness or Paralysis: Weakness affecting both legs or progression to paralysis indicates nerve root involvement.
Sensory Loss: Patients may experience numbness, tingling, or pins-and-needles sensations in the legs, groin, genitalia, or buttocks.
Sexual Dysfunction: Impotence or loss of sexual sensation can occur due to nerve compression.
Loss of Reflexes: Diminished or absent reflexes in the lower extremities may be detected during neurological examination.
Motor Function Loss: Difficulty walking or loss of motor control in the legs occurs as compression worsens.
When to Seek Emergency Medical Care
Cauda equina syndrome is a medical emergency requiring immediate hospitalization and urgent evaluation. Anyone experiencing the following symptoms should seek emergency medical attention immediately:
If you experience sudden onset of severe lower back pain combined with any of the following, call emergency services immediately: sudden inability to control urination or defecation, sudden weakness in both legs, saddle-area numbness or loss of sensation, or sudden difficulty walking. Time is critical—delaying treatment even by hours can mean the difference between recovery and permanent disability.
Diagnosis of Cauda Equina Syndrome
Prompt diagnosis is essential given the time-sensitive nature of this condition. Physicians typically employ multiple diagnostic approaches:
Clinical Evaluation: Detailed history and neurological examination form the foundation of diagnosis. The presence of red flag symptoms including bladder dysfunction and bilateral leg symptoms prompts immediate imaging.
Magnetic Resonance Imaging (MRI): MRI of the lumbar spine represents the gold standard imaging modality for diagnosing cauda equina syndrome. This test provides detailed visualization of nerve compression and identifies the underlying cause.
Computed Tomography (CT): In cases where MRI is contraindicated or unavailable, CT scanning can help identify structural abnormalities.
Electromyography and Nerve Conduction Studies: These tests may be performed to assess nerve function and identify the specific nerves affected.
Treatment of Cauda Equina Syndrome
The only definitively effective treatment for cauda equina syndrome is surgical decompression of the compressed nerve roots. Time-sensitive surgical intervention offers the best opportunity for functional recovery and prevention of permanent neurological damage.
Surgical Options
Lumbar Laminectomy: This is the most common surgical procedure, involving removal of part of the vertebra (the lamina) to create more space in the spinal canal and relieve pressure on the compressed nerve roots.
Discectomy: When a herniated disc causes compression, this procedure removes the herniated disc material pressing on the nerves.
Sequestrectomy: This procedure involves removal of damaged or necrotic tissue that affects nerve function.
Timing of Surgical Intervention
Research overwhelmingly demonstrates that surgery performed within 48 hours of symptom onset produces significantly better outcomes. Patients treated within this critical window show improved recovery of sensory and motor function, as well as superior outcomes regarding bladder and bowel control. However, even patients who undergo surgery beyond the 48-hour window may experience meaningful improvement.
Adjunctive Treatments
Corticosteroids: High-dose corticosteroids may be prescribed to reduce inflammation and swelling around the spinal cord and nerve roots.
Antibiotics: When infection causes cauda equina syndrome, appropriate antibiotic therapy is essential.
Radiation or Chemotherapy: If a tumor is responsible for nerve compression, these treatments may be indicated following surgical decompression.
Post-Surgical Pain Management
Following surgery, patients may require various pain management strategies including neuropathic pain medications such as antidepressants and anti-seizure medications, topical treatments like capsaicin cream or lidocaine patches, and in some cases, opioid analgesics for severe pain.
Bladder and Bowel Management
Medications to manage bladder and bowel dysfunction may include hyoscyamine (Levsin), oxybutynin (Ditropan), and tolterodine (Detrol). In some cases, catheterization or other interventions may be necessary.
Complications and Long-Term Outcomes
Despite prompt treatment, cauda equina syndrome can result in significant long-term complications:
Permanent Lower Body Weakness or Paralysis: Even with surgical intervention, some patients experience persistent weakness or paralysis in the legs.
Chronic Pain Syndromes: Neurogenic pain can develop and persist long-term, sometimes becoming “centralized” and radiating to other body areas. This pain often worsens at night and can become severe and unrelenting.
Permanent Bladder and Bowel Dysfunction: Loss of control over urination and defecation may persist despite treatment.
Sexual Dysfunction: Erectile dysfunction and loss of sexual sensation commonly persist following cauda equina syndrome.
However, with early surgical intervention, many patients continue to experience gradual functional improvement for years following treatment. Recovery is not always complete, but earlier treatment offers the best opportunity for optimal outcomes.
Frequently Asked Questions
Q: Is cauda equina syndrome always a surgical emergency?
A: True cauda equina syndrome with specific red flag symptoms (particularly bilateral leg symptoms and bowel/bladder dysfunction) is indeed a surgical emergency. These patients require urgent evaluation and surgery ideally within 48 hours of symptom onset.
Q: Can cauda equina syndrome be treated with conservative management?
A: No. Surgical decompression is the only effective treatment for cauda equina syndrome. Delayed or conservative treatment risks permanent neurological damage including paralysis and loss of bladder/bowel control.
Q: What percentage of patients fully recover from cauda equina syndrome?
A: Recovery varies based on the severity of compression, duration of symptoms, and timing of surgical intervention. While early surgery offers the best outcomes, some patients experience permanent deficits even with treatment.
Q: How long does recovery take after cauda equina syndrome surgery?
A: Recovery varies significantly among individuals. Some patients may continue experiencing gradual improvement in bladder and bowel function for years following surgery. Motor and sensory function recovery occurs over months following surgical decompression.
Q: What should I do if I suspect cauda equina syndrome?
A: Seek emergency medical attention immediately. Do not delay evaluation if you experience sudden severe back pain combined with bilateral leg symptoms, saddle anesthesia, or bowel/bladder dysfunction. Call emergency services or go to the nearest emergency department.
References
- Cauda Equina Syndrome: Causes, Symptoms, and Treatments — University of Pittsburgh Medical Center (UPMC). 2024. https://www.upmc.com/services/spine/conditions/cauda-equina-syndrome
- Cauda Equina Syndrome Diagnosis & Treatment — Columbia University Neurosurgery. 2024. https://www.neurosurgery.columbia.edu/patient-care/conditions/cauda-equina-syndrome
- Cauda Equina Syndrome: Symptoms, Treatment, Surgery, and More — WebMD Medical Reference. 2024. https://www.webmd.com/back-pain/cauda-equina-syndrome-overview
- Cauda Equina Syndrome — American Association of Neurological Surgeons (AANS). 2024. https://www.aans.org/patients/conditions-treatments/cauda-equina-syndrome/
- Cauda Equina Syndrome Information — Cedars-Sinai Health Library. 2024. https://www.cedars-sinai.org/health-library/diseases-and-conditions/c/cauda-equina-syndrome.html
- Cauda Equina Syndrome: Symptoms, Causes & Treatment — Riverside Online. 2024. https://www.riversideonline.com/en/medical-services/neurological-and-spine-institute/spine/conditions/cauda-equina-syndrome
- Cauda Equina Syndrome: An Overview and Treatment Guide — Orthopaedic Surgery Information (OrthoInfo, AAOS). 2024. https://orthoinfo.aaos.org/en/diseases–conditions/cauda-equina-syndrome/
Read full bio of Sneha Tete











