Cervical Spondylosis: What It Is, Symptoms & Treatment
Complete guide to cervical spondylosis: causes, symptoms, diagnosis, and effective treatment options.
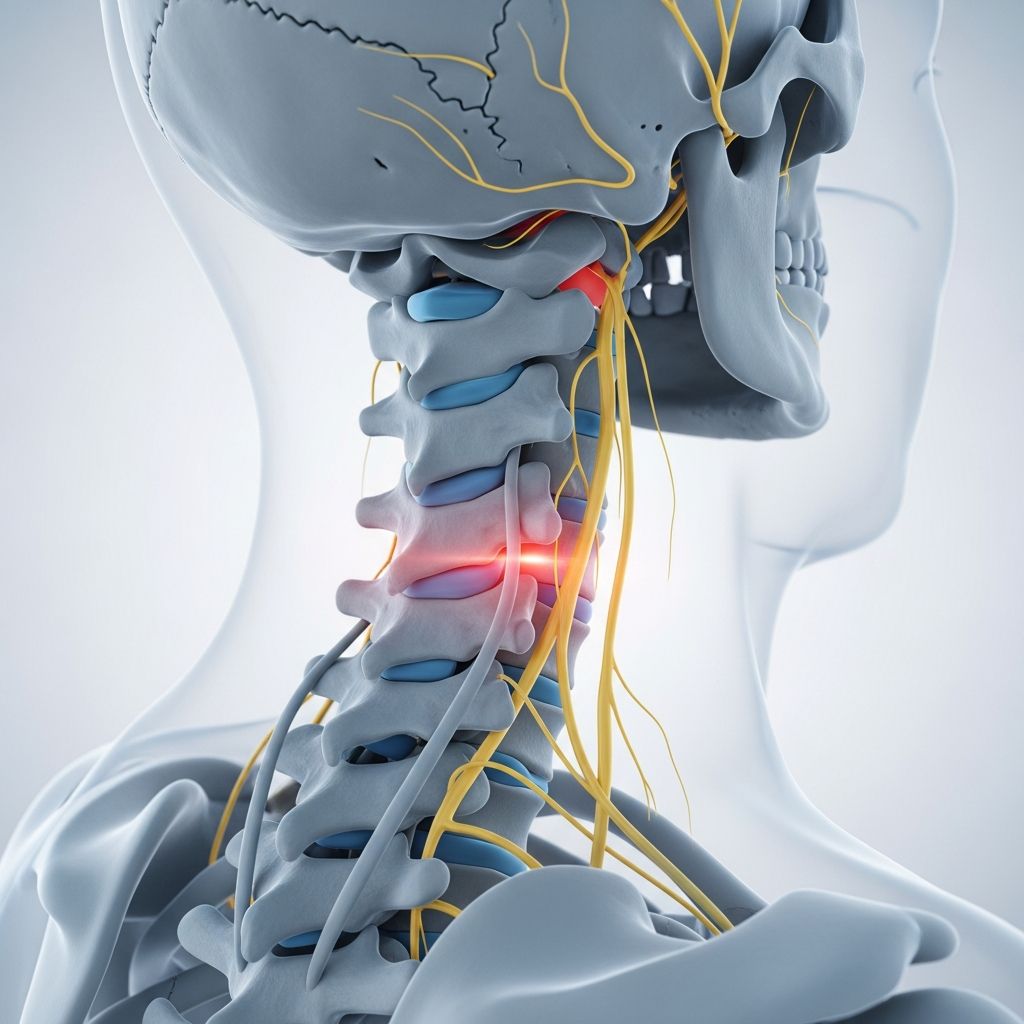
Cervical spondylosis is a general term for wear and tear that affects your cervical spine. Cervical refers to the seven stacked bones, or vertebrae, in your neck. This progressive degenerative condition encompasses a wide range of age-related changes that affect all the components of the cervical spine, including the discs, joints, and ligaments.
As you age, the discs and joints in your cervical spine can break down over time. This natural wear and tear process may develop into cervical spondylosis, which is one of the most common conditions affecting the spine. While it can cause significant discomfort and limitations, many treatment options are available to help manage symptoms and improve quality of life.
Understanding the Cervical Spine
Your cervical spine consists of seven vertebrae stacked on top of each other, forming the structural support of your neck. Between each vertebra are intervertebral discs that act as shock absorbers and allow for flexibility and movement. The cervical spine also contains facet joints that enable rotation and bending of the neck. Nerves and blood vessels pass through this region to supply the upper body, shoulders, and arms.
The cervical spine is particularly vulnerable to degenerative changes because it bears the weight of your head and undergoes constant movement throughout daily activities. Over time, factors such as age, repetitive stress, poor posture, and previous injuries can contribute to the development of cervical spondylosis.
Causes and Risk Factors
Cervical spondylosis develops primarily due to age-related wear and tear. The most common risk factors include:
– Age: The condition becomes increasingly common after age 50- Repetitive neck strain from work or activities- Poor posture, particularly from prolonged computer use- Previous neck injuries or trauma- Smoking, which may accelerate disc degeneration- Genetic predisposition to spine conditions- Sports and physical activities involving repeated neck movement- Osteoarthritis affecting the cervical spine
The degenerative process typically begins with the intervertebral discs losing water content and becoming less flexible. This can lead to disc bulging or herniation. Simultaneously, bone spurs, or osteophytes, may develop on the vertebrae as the body attempts to stabilize the degenerating segments. These changes can narrow the spinal canal and compress nerve roots, leading to symptoms.
Symptoms of Cervical Spondylosis
The symptoms of cervical spondylosis vary widely depending on the severity of the condition and which structures are affected. Some individuals experience no symptoms, while others may have significant pain and functional limitations. Common symptoms include:
– Neck stiffness and reduced range of motion- Neck pain that may be chronic or intermittent- Headaches, particularly at the base of the skull- Shoulder and upper back pain- Radiating pain, tingling, or numbness into the arms and hands- Muscle weakness in the shoulders, arms, or hands- Loss of balance or coordination- Difficulty with fine motor tasks such as writing or buttoning clothes- Pain that worsens with certain activities or positions
In more severe cases, cervical spondylosis can progress to cervical radiculopathy (nerve root compression) or cervical myelopathy (spinal cord compression), which may cause more pronounced neurological symptoms. Cervical spondylotic myelopathy is the most common cause of spinal cord impairment in adults over age 55.
Diagnosis of Cervical Spondylosis
Physical Examination
Your healthcare provider will begin the diagnostic process with a comprehensive physical examination. This includes assessing your posture, looking for bumps or knots in your neck, and evaluating the general structure and alignment of your cervical spine. The provider will also perform several functional tests to determine the extent of your condition.
During the physical exam, your doctor will typically:
– Test your reflexes to check for nerve involvement- Assess muscle strength and look for weakness or atrophy- Evaluate sensory function in your arms and hands- Test your neck’s range of motion in all directions- Observe your gait and walking pattern- Perform special tests to check for nerve compression or spinal cord involvement
Imaging and Diagnostic Tests
If cervical spondylosis is suspected based on your symptoms and physical examination, your provider will order imaging tests to visualize your spine and confirm the diagnosis. These tests may include:
– X-rays: Basic imaging that shows bone structure and degenerative changes such as bone spurs and disc narrowing- Magnetic Resonance Imaging (MRI): Provides detailed images of the soft tissues, discs, nerves, and spinal cord to assess for compression or myelopathy- Computed Tomography (CT) Scan: Offers detailed cross-sectional images of the cervical spine, particularly useful for evaluating bone structure- Nerve Function Tests: Electromyography (EMG) and nerve conduction studies to assess nerve damage or dysfunction- Myelography: Imaging test where contrast dye is injected to highlight the spinal cord and nerves
These diagnostic tools help your healthcare provider determine the severity of your condition, identify which structures are affected, and rule out other conditions that may cause similar symptoms.
Treatment Options for Cervical Spondylosis
The best treatment approach is one that helps ease your symptoms and improves your functional ability. Treatment strategies depend on the severity of your condition and your response to initial interventions. In the absence of significant neurological involvement, healthcare providers typically start with conservative, noninvasive treatments before considering more invasive options.
Conservative Treatment Approaches
Conservative treatment is the first-line approach for most patients with cervical spondylosis. A structured, progressive physical therapy program lasting four to six weeks forms the primary foundation of conservative management.
Physical Therapy
Physical therapy is one of the most effective nonsurgical treatments for cervical spondylosis. A skilled physical therapist will design a personalized program that includes:
– Stretching exercises targeting the neck, shoulders, and upper back muscles- Strengthening exercises to improve cervical and thoracic muscle stability- Postural correction and ergonomic training- Cervical spine mobilization techniques- Proprioception and balance training- Gradual progression from pain management to functional restoration
Early stages of physical therapy focus on pain management, reduction of inflammation, and gradual reintroduction of mobility exercises. As you progress, your therapist will transition to strengthening and proprioception exercises targeting cervical and thoracic musculature. Physical therapy helps build muscle strength and endurance, which reduces stress on the degenerative spinal structures and improves overall neck stability.
Neck Traction
Cervical traction uses weights and specialized equipment to increase the space between the cervical joints and reduce pressure on the cervical discs and nerve roots. This can provide significant relief for radicular symptoms and is often incorporated into a comprehensive physical therapy program.
Medications
Your healthcare provider may recommend various medications to manage pain and inflammation:
– Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen- Acetaminophen for pain relief- Muscle relaxants to reduce muscle spasms- Corticosteroids for more significant inflammation- Nerve pain medications for radicular symptoms
Lifestyle Modifications
Simple changes in your daily activities can significantly reduce symptoms:
– Maintain proper posture when sitting, standing, and working- Take regular breaks from computer work- Use ergonomic furniture and accessories- Apply ice or heat therapy as appropriate- Sleep with proper neck support- Avoid activities that aggravate your symptoms- Manage stress through relaxation techniques
Interventional Treatments
If conservative management is insufficient after several weeks of treatment, your provider may recommend more invasive interventional treatments to provide pain relief and reduce inflammation.
Cervical Epidural Steroid Injection
Cervical epidural steroid injections deliver anti-inflammatory medication directly into the epidural space surrounding the spinal cord and nerve roots. A 2019 systematic review found that nearly half of patients with cervical radicular pain experienced over 50% pain reduction after cervical transforaminal epidural steroid injections at 1-3 months follow-up. These injections can provide temporary or long-term relief and may be repeated if necessary.
Facet Joint and Medial Branch Injections
These injections target the small joints on the sides of the vertebrae (facet joints) or the nerves that supply them. They can help determine if facet joint pain is a significant component of your symptoms and provide therapeutic relief.
Radiofrequency Ablation
This procedure uses heat generated by radiofrequency energy to damage the nerves responsible for transmitting pain signals from the facet joints. This can provide longer-lasting pain relief than injections alone.
Surgical Treatment
If your condition is complicated by cervical myelopathy, cervical radiculopathy with significant neurological deficits, or if conservative and interventional treatments have not provided adequate relief, your provider may recommend surgery. Several surgical options are available.
Anterior Disc Replacement with Fusion
This procedure involves removing the damaged intervertebral disc from the front of the neck and replacing it with either a fusion (solid bone graft) or an artificial disc replacement. This approach is typically used for one- or two-level disease and relieves pressure on nerve roots while maintaining or restoring spinal alignment.
Laminectomy and Fusion
In this procedure, the lamina (back portion of the vertebra) is removed to decompress the spinal cord and nerves. A fusion is then performed to stabilize the spine using bone graft and hardware. This is a posterior approach that effectively relieves pressure from the back of the spinal canal.
Laminoplasty
Laminoplasty is an alternative posterior procedure that involves creating a hinge on one side of the lamina while opening the spinal canal on the other side. Unlike fusion procedures, laminoplasty preserves some neck motion, though it may be limited. This technique is particularly useful for patients with multilevel myelopathy.
Surgical intervention is typically recommended when patients fall within moderate to severe ranges on outcome measures like the modified JOA score, particularly when coupled with disease progression or symptom deterioration. Advanced image guidance technology helps surgeons perform these procedures more safely and precisely.
What to Expect from Treatment
Conservative treatments rarely cause side effects and are the safest initial approach. Most patients respond well to physical therapy, medications, and lifestyle modifications. Response to treatment typically becomes apparent within 4-6 weeks.
More invasive treatments such as steroid injections, radiofrequency ablation, and spinal surgery do carry potential side effects and complications that your healthcare provider will discuss with you before proceeding. The benefits of these interventions often outweigh the risks for patients with significant pain or neurological symptoms.
Prevention and Long-Term Management
While you cannot completely prevent age-related cervical degeneration, you can take steps to slow its progression and minimize symptoms:
– Maintain excellent posture throughout daily activities- Strengthen your neck and upper back muscles regularly- Stretch regularly to maintain flexibility- Use proper ergonomics at work and home- Take regular breaks from repetitive activities- Manage stress effectively- Avoid smoking, which accelerates disc degeneration- Maintain a healthy weight to reduce stress on your spine- Practice neck-friendly sleeping positions
Frequently Asked Questions (FAQs)
Q: Is cervical spondylosis the same as arthritis?
A: Cervical spondylosis is a form of osteoarthritis affecting the cervical spine. It involves degenerative changes to the discs and joints of the neck, so while they are related, cervical spondylosis is a specific type of arthritis affecting the neck region.
Q: Can cervical spondylosis be cured?
A: Cervical spondylosis cannot be completely cured because it represents age-related wear and tear of the spine. However, symptoms can be effectively managed through conservative treatment, interventional procedures, or surgery. The condition can be stabilized and further degeneration may be slowed through appropriate management.
Q: How long does physical therapy take to work?
A: Most patients notice improvement within 4-6 weeks of consistent physical therapy. However, the timeline varies based on severity, individual factors, and adherence to the prescribed program. Continued long-term exercise is often beneficial for preventing symptom recurrence.
Q: Is cervical spondylosis progressive?
A: Cervical spondylosis is a progressive degenerative condition. However, the rate of progression varies significantly among individuals. Appropriate management, physical therapy, and lifestyle modifications can help slow progression and prevent complications.
Q: When should I consider surgery for cervical spondylosis?
A: Surgery is typically considered when conservative and interventional treatments have not provided adequate relief, or when you develop significant neurological symptoms such as spinal cord compression (myelopathy) with progressive weakness or loss of coordination.
Q: Can I work with cervical spondylosis?
A: Many people with cervical spondylosis continue working successfully by making ergonomic adjustments, taking regular breaks, maintaining proper posture, and performing prescribed exercises. Your healthcare provider can help determine appropriate work modifications based on your condition.
References
- Cervical Spondylosis Management and Treatment — Physio-pedia. 2024. https://www.physio-pedia.com/Cervical_Spondylosis
- Cervical Spondylosis: What It Is, Symptoms & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/17685-cervical-spondylosis
- Surgical Treatment of Cervical Spondylotic Myelopathy — Cleveland Clinic. 2024. https://consultqd.clevelandclinic.org/surgical-treatment-landscape-for-cervical-spondylotic-myelopathy-podcast
- Cervical Spondylosis: Causes, Symptoms, Home Remedies, and More — Healthline. 2024. https://www.healthline.com/health/cervical-spondylosis
- Cervical Spondylotic Myelopathy: Evolution of Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/podcasts/neuro-pathways/cervical-spondylotic-myelopathy-evolution-of-treatment
- Cervical Spondylotic Myelopathy — Cleveland Clinic Journal of Medicine, Vol. 70, No. 10. 2003. https://www.ccjm.org/content/ccjom/70/10/899.full.pdf
- Cervical Spine (Neck): What It Is, Anatomy & Disorders — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/articles/22278-cervical-spine
Read full bio of Sneha Tete













