Chiari Malformation: Types, Symptoms & Treatment
Understanding Chiari malformation: causes, symptoms, diagnosis, and treatment options.
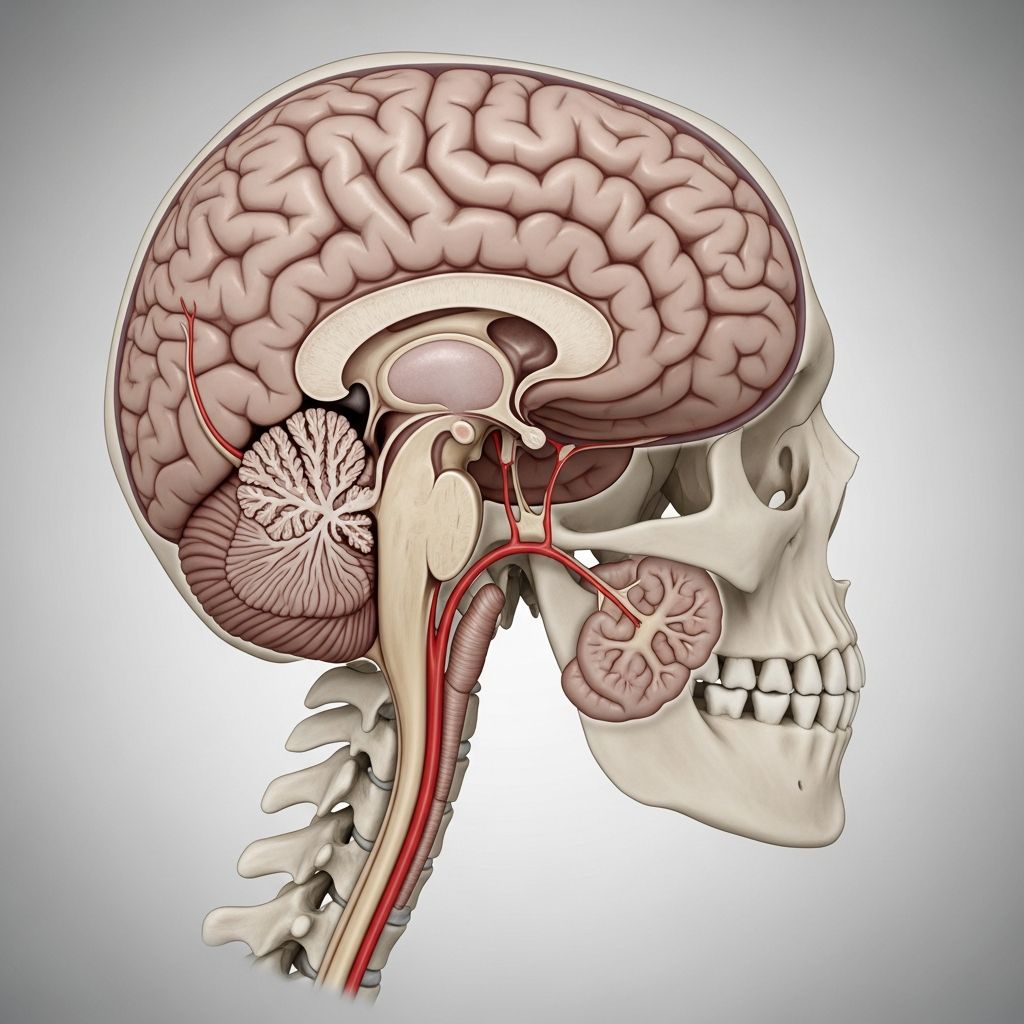
Understanding Chiari Malformation
A Chiari malformation is a structural abnormality in your skull that causes part of your brain to move into your spinal canal. This condition occurs when brain tissue from the lower back part of your skull extends into the spinal canal, specifically through an opening called the foramen magnum, where your brain and spinal cord meet. You may have mild or severe symptoms, or no symptoms at all. Some individuals experience debilitating headaches and difficulty with balance and coordination, while others discover the condition incidentally during imaging for unrelated reasons.
The condition typically results from a structural problem like a smaller-than-expected skull size. If you don’t have enough room in your skull, part of your brain, specifically your cerebellum, grows downward into the extra space available in the spinal canal. Your cerebellum is the part of your brain responsible for muscle movements, posture, balance, speech, and coordination. When this vital brain region is displaced, it can press against the base of your skull and block the flow of cerebrospinal fluid, which normally cushions your brain and spinal cord while circulating nutrients and removing waste products.
How Common Is Chiari Malformation?
Studies suggest that Chiari malformations occur in approximately 1 in every 1,000 people in the United States. However, because some people don’t have any symptoms or don’t show them until adolescence or adulthood, the condition may be significantly more common than these estimates suggest. Many individuals live their entire lives without knowing they have a Chiari malformation, discovering it only when imaging tests are ordered for completely unrelated medical concerns.
The Five Types of Chiari Malformations
Medical professionals recognize five distinct types of Chiari malformations, each with unique characteristics and clinical presentations. Understanding these types is essential for determining appropriate treatment approaches and predicting potential outcomes.
- Type 1: The most common form, characterized by cerebellar tonsils extending into the spinal canal. Type 1 is frequently discovered in adolescents and adults and may be associated with syringomyelia, a condition where fluid-filled cavities form within the spinal cord.
- Type 2: Typically present at birth and often associated with spina bifida. This type involves both cerebellar tissue and the brainstem extending into the spinal canal.
- Type 3: The rarest and most severe form, involving herniation of the cerebellum through a defect in the back of the skull. This type carries the highest risk of serious neurological complications.
- Type 4: Characterized by underdevelopment of the cerebellum without herniation into the spinal canal.
- Type 5: A recently identified category that represents variations of Chiari malformations not fitting into the previous classifications.
Causes and Development
Chiari malformations are almost always present at birth, though symptoms may not develop until later in life. This congenital condition is usually the result of a genetic change or mutation that you inherit from your biological family, or it happens randomly after conception. During fetal development, a structural growth abnormality in your brain and spinal cord creates pressure that causes your cerebellum to grow in an unexpected location.
Very rarely, a Chiari malformation can develop in someone who wasn’t born with the condition. In these cases, the skull or spinal cord might change shape due to trauma, infection, or other medical conditions that alter normal anatomy. These acquired cases represent exceptional circumstances rather than typical presentations of the condition.
Recognizing Symptoms
Symptoms of Chiari malformation vary significantly from person to person and range from no symptoms to mild to severe presentations. In some people, symptoms are present at birth. In others, symptoms appear in late childhood or adulthood. Symptoms may also get better or worse at different points in time, making long-term monitoring essential.
Common Symptoms Include:
- Headaches, particularly at the back of the head
- Neck pain and stiffness
- Loss of balance and coordination difficulties
- Numbness and tingling in the hands, arms, legs, or feet
- Weakness in the hands or legs
- Loss of temperature sensation
- Walking difficulties and gait disturbances
- Dizziness and vertigo
- Vision problems and eye movement abnormalities
- Hearing loss or ringing in the ears
The severity and specific combination of symptoms depend on the extent of cerebellar displacement and whether syringomyelia or other spinal cord complications have developed. Some patients experience progressive worsening of symptoms over time, while others remain stable for years.
Diagnosis and Imaging
MRI is the best imaging technique for visualizing and diagnosing Chiari malformations. The high-resolution images produced by MRI can clearly show the extent of cerebellar tissue extending into the spinal canal and detect any associated complications like syringomyelia. After an MRI is performed, patients are typically referred to a neurosurgeon for surgical discussion if symptoms warrant intervention.
The diagnostic process begins with a careful medical history and neurological examination. Your healthcare provider will ask about your symptoms, when they started, and how they’ve progressed over time. Physical examination may include tests of your balance, coordination, reflexes, and muscle strength. These findings, combined with imaging results, help determine the severity of your condition and guide treatment recommendations.
Treatment Options
Conservative Management
Some Chiari malformations are non-symptomatic and represent incidental findings on MRI scans performed for other reasons. For these patients, surgery is typically not offered initially. Instead, patients are observed with multiple imaging studies conducted at six-month to one-year intervals to monitor for any changes or symptom development.
For mild symptoms like headaches or neck pain, conservative treatment approaches may include pain medication to manage discomfort, physical therapy to improve strength and flexibility, and lifestyle modifications to avoid activities that trigger or worsen symptoms. Many patients find relief through these non-invasive methods and never require surgical intervention.
Surgical Treatment
Patients experiencing severe symptoms are generally appropriate candidates for surgical decompression. These patients typically benefit significantly from surgery, with symptoms improving substantially post-operatively. At specialized centers like Cleveland Clinic Florida, minimally invasive surgical approaches are used to treat Chiari malformation through very small incisions.
Surgical procedures may include bony decompression, where bone at the base of the skull is carefully removed to create more space for the cerebellum. In some cases, surgeons also open the dura, the membrane envelope surrounding the brain, to provide additional relief. These minimally invasive techniques result in faster recovery times and generally acceptable outcomes for patients.
The specific surgical approach depends on the type and severity of the malformation, whether syringomyelia is present, and individual patient factors. Your neurosurgeon will discuss the procedure details, expected outcomes, and potential risks before surgery.
Recovery and Long-Term Outlook
The timeline for recovery depends on the treatment chosen. Patients taking pain medication or participating in therapy for mild symptoms may find relief soon after beginning treatment. Those undergoing surgery typically require several weeks to months before fully healing. Many patients notice their symptoms go away or reduce significantly after surgery, though complete resolution is not guaranteed.
Your long-term outlook varies depending on the severity and type of Chiari malformation. If you don’t have symptoms or you have mild symptoms after a Chiari malformation diagnosis, you’ll likely have a normal life expectancy. However, severe symptoms and certain types of Chiari malformation can be fatal, which is why professional medical guidance is crucial.
It’s important to work closely with your healthcare provider and care team, who can monitor your symptoms and determine the right treatment plan for you. Repeat surgeries might be necessary as you age, particularly if symptoms recur or new complications develop.
Important Considerations
Although there isn’t a cure for a Chiari malformation, treatment like surgery can help manage your symptoms to help you feel better and prevent life-threatening complications. Every surgery comes with possible risks. Surgery around your brain and skull is high risk due to the location of the incision and procedure being near your brain.
Your healthcare provider will discuss the side effects of treatment before you begin so you can make an informed decision about your health. There’s no known way to prevent a Chiari malformation, as it’s primarily a congenital condition determined by genetics and fetal development.
Frequently Asked Questions
Q: Can Chiari malformation be cured?
A: There is no cure for Chiari malformation, but treatment including surgery can effectively manage symptoms and prevent serious complications. Many patients experience significant symptom improvement with appropriate intervention.
Q: Is Chiari malformation life-threatening?
A: Chiari malformation can be very serious in some cases, but not all. Most cases are manageable with appropriate treatment. However, severe symptoms and certain types can be fatal, which is why professional medical evaluation is essential.
Q: When should someone have surgery for Chiari malformation?
A: Surgery is typically recommended for patients with severe, progressive symptoms that significantly impact daily activities. Patients with mild or no symptoms may be monitored without surgery, while those with severe symptoms generally benefit greatly from surgical decompression.
Q: How is Chiari malformation diagnosed?
A: MRI imaging is the gold standard for diagnosing Chiari malformation. High-resolution MRI scans can clearly show cerebellar tissue extending into the spinal canal and detect associated complications.
Q: Can symptoms develop later in life if I was born with the condition?
A: Yes, many people with Chiari malformation are born with the condition but don’t experience symptoms until late childhood, adolescence, or adulthood. Symptoms may also fluctuate over time, getting better or worse at different points.
Q: What is syringomyelia and how does it relate to Chiari malformation?
A: Syringomyelia is a condition where fluid-filled cavities form within the spinal cord. It often accompanies Chiari malformation, particularly Type 1, and can contribute to additional neurological symptoms.
Q: Is Chiari malformation hereditary?
A: Chiari malformation is usually the result of a genetic mutation inherited from biological family members, though it can also occur randomly after conception. If you have Chiari malformation, genetic counseling may be beneficial for family members.
References
- Chiari Malformation: What It Is, Symptoms, Types & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/6008-chiari-malformation
- What Is a Chiari Malformation? — Cleveland Clinic. August 5, 2025. https://www.youtube.com/watch?v=z2sdBmovCow
- Neuro-ophthalmology of Type 1 Chiari Malformation — PubMed/National Center for Biotechnology Information. https://pubmed.ncbi.nlm.nih.gov/26843890/
Read full bio of medha deb













