Chilblains Comprehensive Guide: Causes, Symptoms, Treatment
Understanding chilblains: symptoms, causes, diagnosis, treatment, and prevention of this cold-induced skin condition.
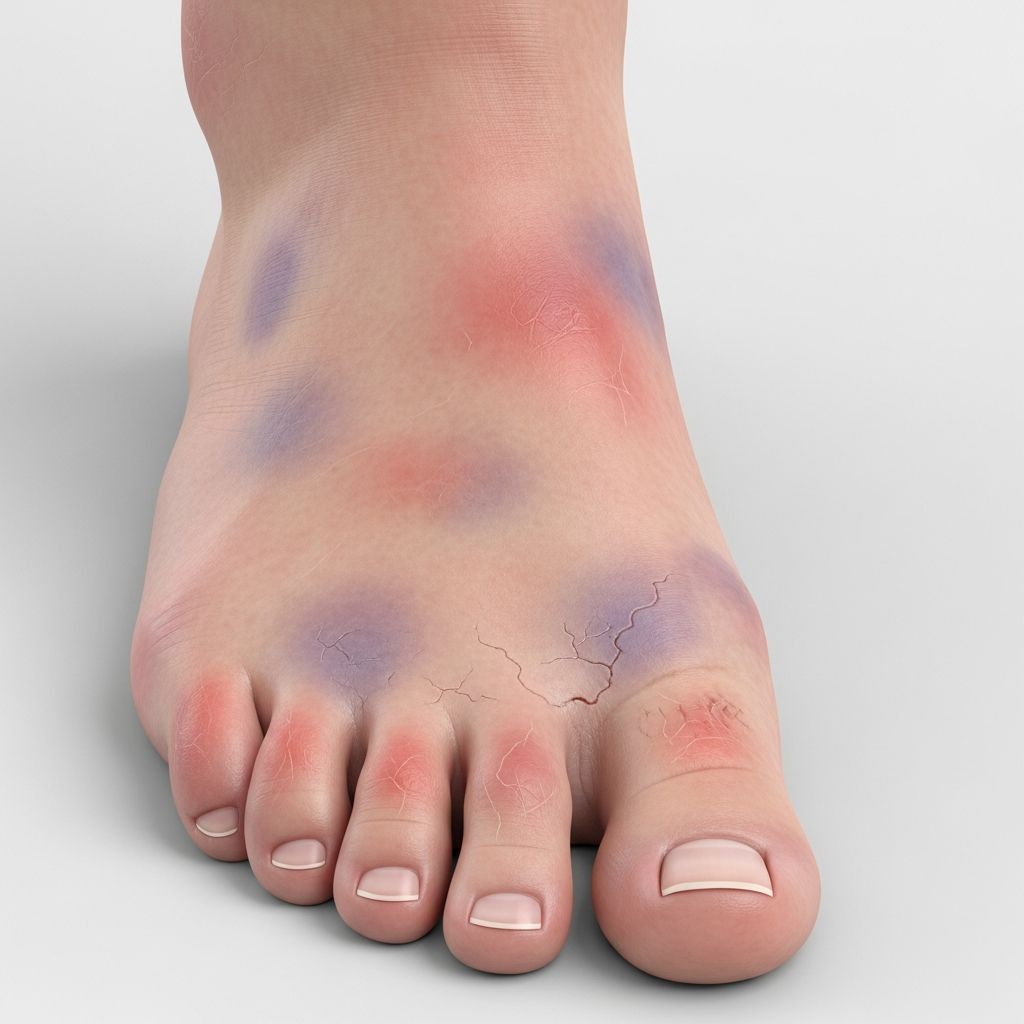
Chilblains
Chilblains, also known as pernio or perniosis, are tender and/or itchy bumps on acral sites following exposure to damp, cold, non-freezing conditions, causing a localised form of vasculitis.
Introduction
Chilblains represent a reactive inflammatory process of the skin triggered by prolonged exposure to cold, damp environments where temperatures hover above freezing. This condition manifests as localised vasculitis, primarily affecting the extremities. Unlike frostbite, which involves actual freezing, chilblains arise from non-freezing cold injury, leading to vascular instability and subsequent tissue inflammation.
The term ‘chilblains’ originates from Old English words for ‘cold’ and ‘sore,’ aptly describing the painful, sore-like eruptions that develop hours after exposure. While generally benign and self-limiting, recurrent episodes can significantly impact quality of life, particularly in susceptible individuals during winter months.
Demographics
Chilblains affect individuals of all ages, though certain groups are at higher risk. Women are more commonly affected than men, possibly due to differences in body composition and clothing choices. Children and young adults, particularly those with low body mass index (BMI), are vulnerable because of reduced subcutaneous fat insulation.
Geographically, chilblains are prevalent in temperate climates with frequent damp, cold weather, such as the United Kingdom, New Zealand, and parts of Europe. People living in warmer, drier regions rarely experience typical presentations. Babies can develop chilblains if inadequately protected from cold. Recurrent cases often follow a seasonal pattern, appearing annually in winter.
Causes
The pathogenesis of chilblains involves an abnormal vascular response to cold. Cold, damp air causes vasoconstriction of superficial blood vessels, reducing blood flow and oxygen delivery to the skin. Upon rewarming, rapid vasodilation occurs, leading to leakage of fluid into surrounding tissues, inflammation, and the characteristic lesions.
Primary (idiopathic) chilblains occur without underlying disease, while secondary forms are associated with systemic conditions. Risk factors include:
- Low BMI or thin body habitus, reducing natural insulation.
- Poor circulation from smoking, tight clothing, or sedentary lifestyle.
- Connective tissue diseases like lupus erythematosus (chilblain lupus).
- Family history suggesting genetic predisposition.
Exposure to chronic cold on exposed areas, such as fingers, toes, or thighs in equestrian activities (‘equestrian panniculitis’), exacerbates risk.
Clinical features
Chilblains typically develop 12-24 hours after cold exposure and persist for 1-3 weeks. They present as:
- Erythematous (red) or dusky purple papules, nodules, or plaques on acral sites (fingers, toes, ears, nose, heels).
- Itching, burning, or tenderness, worsening upon rewarming.
- Swelling, shiny skin, or blistering in severe cases.
- Less common sites: cheeks, shins, thighs, hips, or buttocks.
On darker skin, lesions may appear less red and more hyperpigmented. Dermoscopy shows non-specific vascular patterns, but nailfold capillaroscopy may reveal abnormalities in connective tissue disease cases.
Complications
Most chilblains resolve without sequelae, but complications include:
- Blistering, ulceration, or secondary bacterial infection leading to scarring.
- Chronic recurrent pernio, potentially unmasking underlying connective tissue disease like lupus.
- Pain and swelling interfering with daily activities.
Severe or persistent cases warrant investigation for secondary causes.
Diagnosis
Diagnosis is primarily clinical, supported by the Mayo Clinic criteria:
| Major Criterion (Required) | Minor Criteria (≥1 required) |
|---|---|
| Localised redness and swelling of acral sites lasting ≥24 hours | Winter prominence |
| Response to vasodilators (e.g., nifedipine) | |
| Biopsy showing perivascular lymphocytic infiltrate |
Investigations for secondary chilblains may include blood tests (ANA, RF), skin biopsy revealing superficial/deep lymphocytic vasculitis, eccrine gland involvement, and subepidermal oedema. Differential diagnoses encompass frostbite, erythromelalgia, acrocyanosis, and chilblain lupus erythematosus (CHLE), distinguished by biopsy and serology.
Differential diagnoses
- Chilblain lupus erythematosus: Persistent lesions, positive ANA, genetic mutations; biopsy shows interface dermatitis.
- Frostbite: History of freezing temperatures, tissue necrosis.
- Acrocyanosis: Persistent bluish discoloration without inflammation.
- Raynaud phenomenon: Episodic pallor, cyanosis, rubor triphasic pattern.
- Cellulitis: Fever, rapid spread, bacterial cause.
Treatment
Chilblains often resolve spontaneously in 1-3 weeks with supportive care:
- Self-care: Gradual rewarming (alternate warm/cold water soaks), emollients, avoid scratching. NSAIDs (ibuprofen) for pain/swelling.
- Topical: Corticosteroids (e.g., betamethasone valerate) for inflammation; nitroglycerin for vasodilation.
- Systemic: Calcium channel blockers like nifedipine (oral) to prevent vasoconstriction; pentoxifylline improves circulation. Prescribed for severe/recurrent cases.
Prevention is paramount: Wear warm, layered, waterproof clothing; avoid sudden temperature changes; maintain good circulation.
Outcome
Acute chilblains resolve in 7-21 days with warmth. Chronic/recurrent forms may persist seasonally, requiring prophylactic nifedipine. Early intervention prevents complications; consult a dermatologist for non-resolving lesions.
Frequently Asked Questions
What causes chilblains?
Chilblains result from vasoconstriction in cold, damp conditions followed by rapid rewarming, causing vessel leakage and inflammation.
How long do chilblains last?
Typically 1-3 weeks, resolving with warmth; recurrent annually in winter.
Are chilblains contagious?
No, they are inflammatory reactions, not infectious.
What is the best cream for chilblains?
Corticosteroid creams (e.g., triamcinolone 0.1%) reduce itching and swelling; prescribed by a doctor.
Can chilblains lead to other diseases?
Recurrent cases may indicate connective tissue disease like lupus.
References
- Chilblains: Causes, Symptoms, Diagnosis, Treatment, and Prevention — WebMD. 2023. https://www.webmd.com/skin-problems-and-treatments/chilblains-causes-symptoms-diagnosis-treatment-and-prevention
- Chilblains (Pernio): What Is It, Symptoms, Causes & Treatment — Cleveland Clinic. 2023-10-10. https://my.clevelandclinic.org/health/diseases/21817-chilblains-pernio
- Chilblains: Causes, Symptoms and Treatment — Patient.info. 2023. https://patient.info/foot-care/chilblains
- Chilblain lupus erythematosus — DermNet NZ. 2023. https://dermnetnz.org/topics/chilblain-lupus-erythematosus
- Chilblains (Pernio): Symptoms and Management — DermNet NZ. 2023. https://dermnetnz.org/topics/chilblains
- Pernio — StatPearls, NCBI Bookshelf. 2023-08-08. https://www.ncbi.nlm.nih.gov/books/NBK549842/
Read full bio of Sneha Tete












