Cholecystectomy: Gallbladder Removal Surgery Guide
Complete guide to cholecystectomy surgery: procedures, recovery, and what to expect.
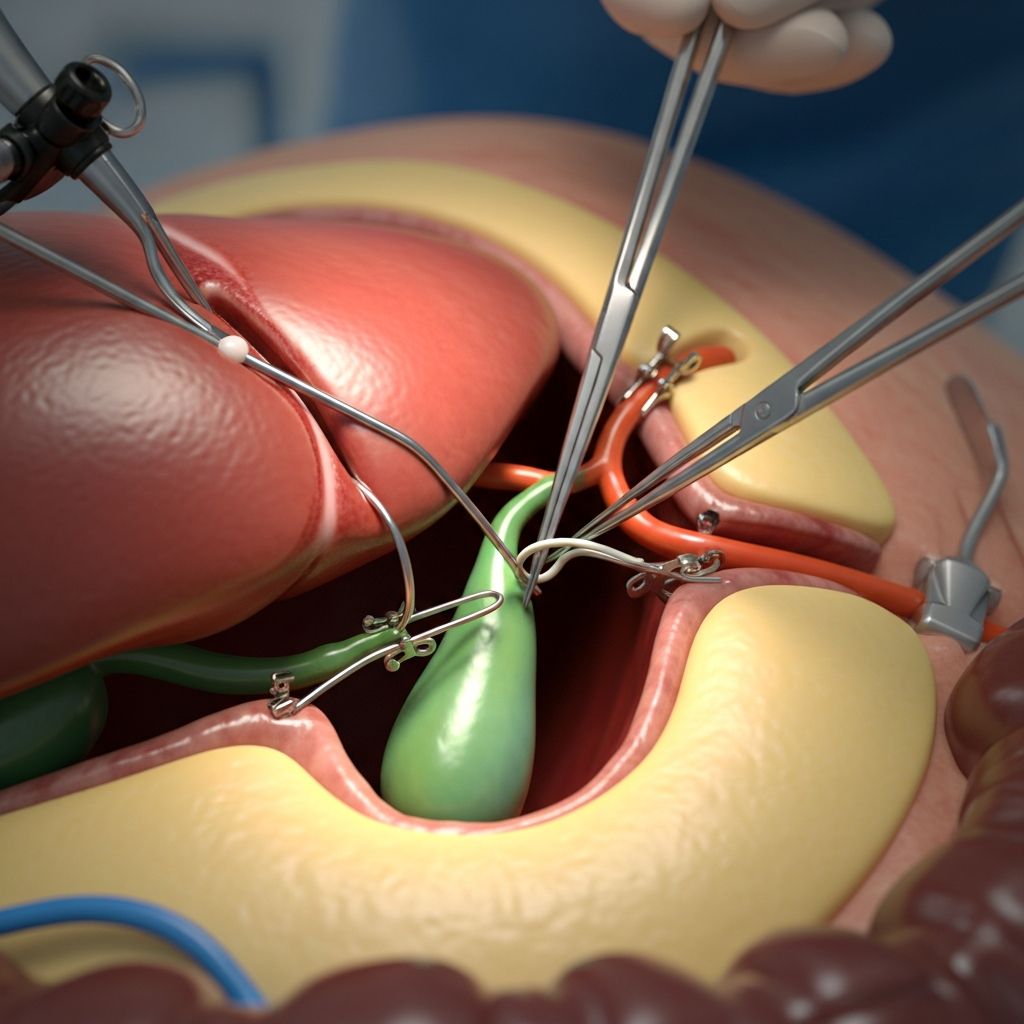
Understanding Cholecystectomy: A Complete Overview
Cholecystectomy is a surgical procedure that involves the removal of the gallbladder, a small organ located beneath the liver on the right side of the abdomen. The gallbladder stores bile, a digestive fluid produced by the liver that helps break down fats. When the gallbladder develops problems such as gallstones, inflammation, or dysfunction, a cholecystectomy may become necessary. This procedure is one of the most commonly performed surgeries in the United States, with hundreds of thousands of procedures performed annually. Modern surgical techniques have made cholecystectomy a relatively safe and routine operation with excellent outcomes for most patients.
Why Cholecystectomy Is Performed
Cholecystectomy is recommended for various gallbladder-related conditions that cause pain, complications, or interfere with normal digestive function. Understanding why your doctor recommends this procedure is essential for making informed decisions about your healthcare.
Common Indications for Surgery
The most common reason for cholecystectomy is symptomatic gallstones, which develop when cholesterol or bilirubin accumulates in the gallbladder and hardens into stone-like deposits. When these gallstones obstruct the bile ducts, they can cause severe pain in the upper right abdomen or epigastric region. Additionally, acute cholecystitis, an inflammation of the gallbladder often caused by gallstone obstruction, frequently necessitates surgical removal. Chronic cholecystitis, characterized by long-term inflammation and scarring of the gallbladder wall, also commonly leads to cholecystectomy recommendations.
Other conditions requiring cholecystectomy include pancreatitis caused by gallstones, biliary dyskinesia where the gallbladder fails to function properly despite the absence of stones, and primary biliary cholangitis. In cases of gallbladder cancer, cholecystectomy may be performed along with removal of adjacent tissues to achieve complete cancer resection. Patients with sickle cell disease who experience recurrent gallstone-related problems may also benefit from this procedure.
Types of Cholecystectomy Procedures
Modern cholecystectomy can be performed using different surgical techniques, each with specific advantages and considerations. Your surgeon will recommend the most appropriate approach based on your individual circumstances, anatomy, and medical history.
Laparoscopic Cholecystectomy
Laparoscopic cholecystectomy is the preferred and most commonly performed technique for gallbladder removal. This minimally invasive procedure involves making three to four small incisions, typically five to twelve millimeters in length, in the abdomen. Through these small openings, the surgeon inserts a laparoscope—a thin tube equipped with a camera—and specialized surgical instruments. The camera projects images onto a monitor, allowing the surgeon to visualize the surgical area in detail.
During the laparoscopic procedure, the surgeon carefully identifies the critical structures, including the cystic artery and cystic duct, before removing the gallbladder. Carbon dioxide gas is used to inflate the abdomen, creating space and improving visualization. The procedure typically takes 30 to 60 minutes, depending on the complexity of the case. Laparoscopic cholecystectomy offers significant advantages over open surgery, including less postoperative pain, shorter hospital stays, faster recovery times, and smaller, less noticeable scars.
Open Cholecystectomy
Open cholecystectomy involves making a larger incision, typically four to six inches, usually below the right rib cage in a line with the right rectus muscle (subcostal incision). This traditional approach may be recommended when laparoscopic surgery is not feasible or when complications arise during a laparoscopic procedure. Conditions that might necessitate open surgery include extensive adhesions from previous abdominal surgery, severe inflammation making identification of anatomical structures difficult, or bile duct injury during laparoscopic attempts.
During open cholecystectomy, the surgeon has direct visualization of the surgical field and can more easily manage complications or unexpected findings. While this approach provides excellent visualization and control, it results in a larger scar and typically involves longer recovery periods compared to laparoscopic techniques.
The Surgical Process
Understanding what happens during your cholecystectomy can help alleviate anxiety and prepare you for the experience.
Preoperative Preparation
Before undergoing cholecystectomy, you will undergo comprehensive preoperative evaluation including laboratory tests, imaging studies, and consultation with your anesthesia provider. You will receive specific instructions regarding fasting—typically nothing to eat or drink after midnight the evening before surgery. Certain medications may need to be adjusted or held temporarily. You should arrange for someone to drive you home after the procedure, as anesthesia affects your judgment and reflexes for several hours postoperatively.
Anesthesia and Positioning
Upon arrival at the operating room, you will receive general anesthesia, which renders you unconscious and unaware during the procedure. The anesthesiologist will continuously monitor your vital signs, including heart rate, blood pressure, oxygen saturation, and carbon dioxide levels. For laparoscopic procedures, you will be positioned supine initially, then placed in reverse Trendelenburg position (head elevated) and rotated left to optimize visualization of the gallbladder.
The Operative Technique
In laparoscopic cholecystectomy, after establishing pneumoperitoneum with carbon dioxide insufflation, the surgeon places trocars (small tubes) through which instruments are inserted. The first step involves careful inspection of the abdomen to identify any adhesions, anatomy variations, or additional pathology. The surgeon then identifies Calot’s triangle, the anatomical area bounded by the common bile duct, hepatic artery, and the cystic artery, which must be cleared of all tissue.
The surgeon carefully dissects tissue around the cystic artery, which is identified, isolated, and divided using electrocautery, clips, or sutures. Next, the cystic duct is identified and carefully cleared of periductal tissue. If there is any question about the anatomy or a ductal stone is present, an intraoperative cholangiogram may be obtained. The cystic duct is then divided, and the gallbladder is carefully removed from the liver bed using electrocautery or other hemostatic techniques. Before completing the procedure, the surgeon inspects the liver bed for bleeding or bile leaks, irrigates the area, and ensures hemostasis.
Recovery and Hospital Stay
The length of your hospital stay and recovery timeline depend on the type of procedure performed and your individual health status.
Immediate Postoperative Period
Following laparoscopic cholecystectomy, most patients recover in the post-anesthesia care unit for one to two hours before discharge home the same day. Some patients, particularly those with complex cases or significant comorbidities, may require overnight hospitalization. You will experience grogginess from anesthesia and should not drive or make important decisions for at least 24 hours.
You may notice mild abdominal distension and discomfort from the carbon dioxide gas used during the procedure; this typically resolves within a few days. Some patients experience shoulder pain, referred from the diaphragm irritation by the insufflation gas, which also resolves spontaneously. Pain is typically mild and managed with over-the-counter or prescription pain medication.
Wound Care at Home
Your surgical incisions will be covered with sterile dressings that should be removed after 24 to 48 hours. Underneath the adhesive bandage, you may find small strips of tape called Steri-strips, which should remain in place for approximately two weeks to provide additional support and protection to the incision. These strips will fall off naturally and do not need to be replaced. Keep the incisions clean and dry; you may shower after the bandages are removed, but avoid baths and submersion until the incisions are fully healed.
Some redness, mild swelling, or bruising around the incision is normal. However, contact your surgeon if you notice active bleeding, increasing redness, pus, opening of the incision, or signs of infection such as fever.
Activity and Lifestyle After Surgery
Most patients who undergo laparoscopic cholecystectomy can resume light activities within one to two weeks and return to normal activities within three to four weeks. However, you should avoid strenuous exercise, heavy lifting (more than ten pounds), and demanding physical labor for at least four to six weeks to allow proper wound healing and prevent complications.
Driving should be avoided until you have stopped taking narcotic pain medications, typically one to two weeks postoperatively. You may resume driving when you feel comfortable and have adequate control for emergency maneuvers. Return to work depends on your job type; desk work can usually resume within one to two weeks, while physically demanding jobs may require four to six weeks recovery.
Potential Complications
While cholecystectomy is generally safe, like all surgical procedures, it carries potential risks that you should understand before surgery.
Intraoperative Complications
The most significant intraoperative risk is unintended bile duct injury, which occurs in approximately 0.3 to 0.5 percent of laparoscopic cholecystectomies. This complication may require immediate or delayed repair and can potentially result in long-term morbidity if not recognized and managed appropriately. Other intraoperative risks include bleeding requiring transfusion, bowel or vascular injury, and conversion to open surgery, which occurs in two to fifteen percent of laparoscopic cases depending on patient factors and surgeon experience.
Postoperative Complications
Early postoperative complications include infection, bleeding, bile leak from the cystic duct stump or liver bed, and retained stones. Bile leaks may cause peritonitis or form a bile collection requiring drainage. Retained stones in the common bile duct can cause pancreatitis or jaundice and may require postoperative endoscopic retrograde cholangiopancreatography (ERCP) for removal.
Late complications include adhesions, chronic pain, and postcholecystectomy syndrome—a condition characterized by persistent abdominal pain or digestive symptoms after surgery. Some patients experience postcholecystectomy diarrhea, thought to result from increased bile flow into the colon.
Postcholecystectomy Syndrome and Long-Term Outcomes
Postcholecystectomy syndrome refers to persistent or recurrent abdominal pain, bloating, and digestive dysfunction occurring after cholecystectomy. This syndrome develops in five to fifteen percent of patients and may result from retained bile duct stones, bile reflux gastritis, altered intestinal motility, or functional bowel disorder unrelated to the gallbladder. Most patients reporting postcholecystectomy symptoms had underlying functional disorders that persisted despite gallbladder removal.
Long-term satisfaction rates following cholecystectomy are excellent, with seventy-five to ninety percent of patients reporting complete symptom relief and high satisfaction with the procedure. Most patients tolerate a normal diet without restrictions after complete healing.
Diet After Cholecystectomy
Immediately after surgery, you will consume clear liquids until your bowel function returns. You can then gradually advance to a regular diet. Unlike before surgery, there are typically no dietary restrictions after cholecystectomy, though some patients find it helpful to avoid very fatty or greasy foods initially while adjusting to the changes in bile delivery to the intestines. Most patients can resume their normal diet within two to three weeks postoperatively without complications.
Special Considerations
Acute vs. Elective Cholecystectomy
Acute cholecystectomy performed during an acute illness with active inflammation carries higher operative risk than elective surgery on a stable patient. However, current evidence supports early laparoscopic cholecystectomy even in acute settings, as it reduces the risk of recurrent biliary complications and is cost-effective compared to delayed surgery.
Cholecystectomy for Gallbladder Cancer
When cholecystectomy is performed for gallbladder cancer, the surgeon typically removes the gallbladder along with a portion of the adjacent liver and regional lymph nodes to ensure complete tumor resection. Advanced tumors may require more extensive resection, including bile duct resection or pancreaticoduodenectomy (Whipple procedure) for distal bile duct cancers.
Frequently Asked Questions
Q: Can the gallbladder grow back after removal?
A: No, the gallbladder is a fully removed organ and cannot regenerate or grow back. Once removed, it is permanently gone.
Q: How long does laparoscopic cholecystectomy take?
A: Most laparoscopic cholecystectomies take 30 to 60 minutes, though complex cases may require longer operative time.
Q: When can I return to work after cholecystectomy?
A: Light desk work can usually resume within one to two weeks, while physically demanding work may require four to six weeks recovery.
Q: Are there alternatives to surgery for gallstones?
A: For symptomatic gallstones causing significant problems, cholecystectomy is the definitive treatment. Medications to dissolve stones are rarely used today due to limited effectiveness and high recurrence rates.
Q: What is the success rate for laparoscopic cholecystectomy?
A: Laparoscopic cholecystectomy has a success rate exceeding ninety percent, with most patients experiencing complete symptom relief and satisfaction with the procedure.
References
- Laparoscopic Cholecystectomy: Safety and Efficacy in General Surgery — Johns Hopkins University Research. 2024. https://pure.johnshopkins.edu/en/publications/laparoscopic-cholecystectomy-10
- Treatment Guidelines for Gallbladder and Bile Duct Cancer — Johns Hopkins Pathology Department. 2024. https://pathology.jhu.edu/gbbd/treatment
- Cholecystitis Management and Early Cholecystectomy — Johns Hopkins ABX Guide. 2024. https://www.hopkinsguides.com/hopkins/view/Johns_Hopkins_ABX_Guide/540122/all/Cholecystitis
- Hopkins General Surgery Review Manual — Johns Hopkins Medical Education. 2019. https://peterattiamd.com/wp-content/uploads/2019/09/Hopkins-General-Surgery-Review-Manual.pdf
- Postoperative Care Instructions for Gallbladder Removal Surgery — Johns Hopkins All Children’s Hospital. 2024. https://www.youtube.com/watch?v=Ef-YM9CKLjA
Read full bio of medha deb













