Chronic Inducible Urticaria: Triggers, Diagnosis & Treatment
Comprehensive guide to managing chronic inducible urticaria with evidence-based treatment strategies.
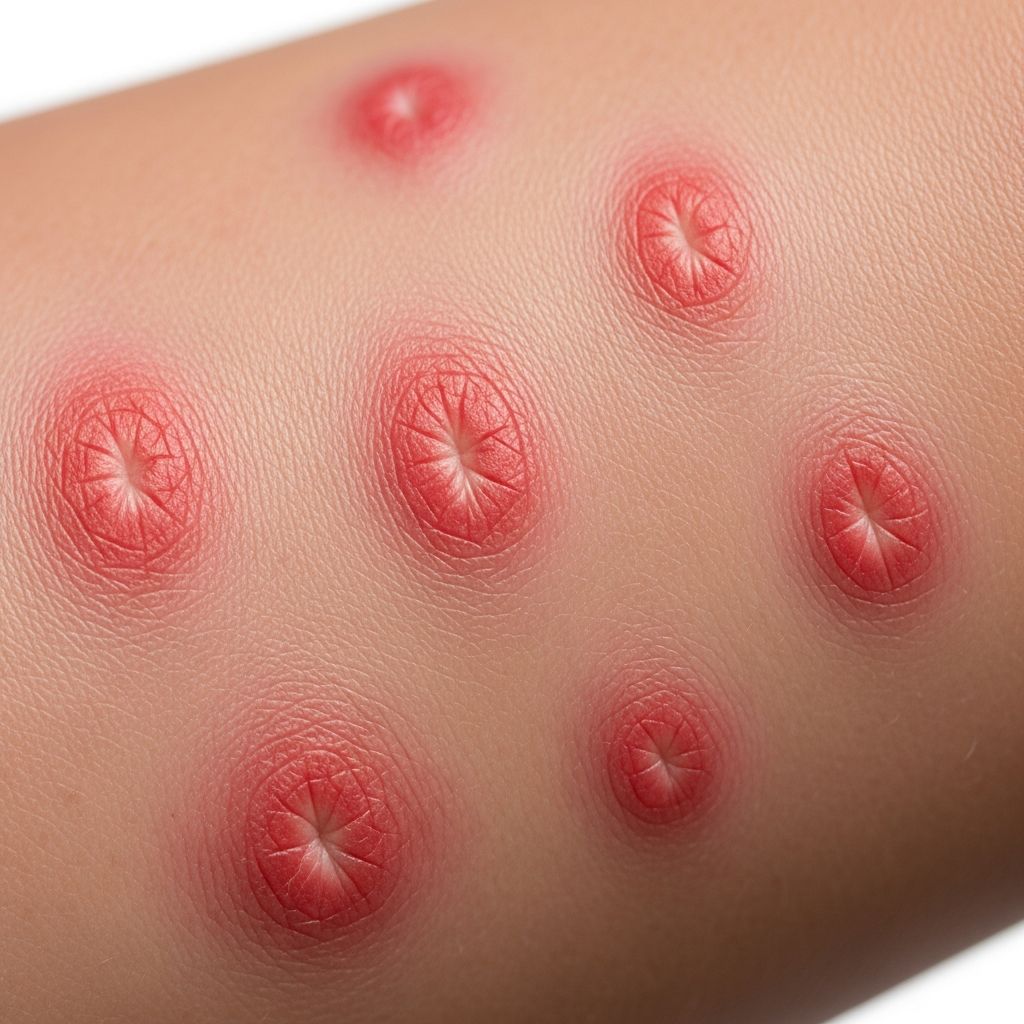
Understanding Chronic Inducible Urticaria
Chronic inducible urticaria (CIndU), also referred to as physical urticaria, is a distinct subtype of chronic urticaria characterized by recurrent itchy wheals and angioedema that persist for more than six weeks in response to specific physical stimuli or environmental triggers. Unlike chronic spontaneous urticaria (CSU), where hives appear without an identifiable cause, CIndU has a clearly defined trigger mechanism that predictably induces skin reactions. The wheals in CIndU typically have a shorter duration compared to those in CSU, and the condition often affects younger patients. Understanding the underlying mechanisms and identifying specific triggers are crucial for effective management and improving quality of life for affected individuals.
Types and Triggers of Chronic Inducible Urticaria
CIndU encompasses multiple distinct subtypes, each with unique triggers and pathophysiological mechanisms. Comprehensive knowledge of these different forms is essential for accurate diagnosis and targeted treatment approaches.
Cold Urticaria
Cold urticaria occurs upon exposure to cold air, cold water, or cold objects. This subtype can trigger immediate hive outbreaks and potentially severe allergic responses, including anaphylaxis in severe cases. Cold urticaria affects patients differently depending on the intensity and duration of cold exposure, and the severity can vary from localized wheals to generalized reactions.
Cholinergic Urticaria
Cholinergic urticaria manifests as heat-induced hives that emerge following exercise, hot showers, emotional stress, or increased body temperature. The exact pathophysiology involves multiple factors including histamine release, acetylcholine involvement, sweat allergy, serum factors, and anhidrosis. It is clinically important to differentiate exercise-induced anaphylaxis from cholinergic urticaria, as provocation testing can help distinguish between these conditions. The disease typically begins during puberty with higher prevalence in females.
Dermatographic Urticaria (Symptomatic Dermographism)
Dermatographic urticaria is characterized by the development of visible raised marks, wheals, and erythema that appear following light scratching, stroking, or rubbing of the skin. This condition results in characteristic linear lesions that follow the pattern of mechanical trauma applied to the skin.
Delayed Pressure Urticaria
This subtype develops hours after sustained pressure is applied to the skin, such as from tight clothing, backpacks, belts, or other mechanical pressure sources. Lesions typically appear six to eight hours after pressure exposure and can persist for extended periods.
Aquagenic Urticaria
Water serves as the primary triggering factor in aquagenic urticaria, with lesions developing within twenty to thirty minutes of contact with water of any temperature or form, including sweat and tears. The disease predominantly starts during puberty with greater female predominance. Lesions characteristically disappear within thirty to sixty minutes of cessation of water contact. The condition is mediated by histamine release triggered by water exposure to the skin.
Solar Urticaria
Solar urticaria develops in response to ultraviolet and visible light exposure, with triggering factors including radiation spectrum from ultraviolet B to visible light within the 300 to 500 nanometer wavelength range. The disease typically begins during puberty with increased female prevalence.
Contact Urticaria
Contact urticaria can be either immunogenic (allergic type I IgE-mediated hypersensitivity) or non-immunogenic. The immunogenic type develops after previous sensitization to specific allergens. Common triggering agents include latex, plant-derived proteins, animal products, enzymes, and drugs or cosmetics. Lesions can progress from localized reactions to generalized urticaria with systemic symptoms and potential anaphylactic shock, a progression termed contact urticaria syndrome.
Clinical Presentation and Diagnosis
The clinical presentation of CIndU varies depending on the subtype and trigger involved. However, all forms share the characteristic feature of recurrent wheals and potentially angioedema appearing in response to identified physical stimuli. The shorter duration of wheals in CIndU compared to CSU serves as a diagnostic clue, along with the younger age of affected patients and the predictable relationship between trigger exposure and symptom onset.
Diagnostic Procedures
Diagnosis of specific CIndU subtypes relies on clinical history combined with appropriate provocation testing:
- Cold urticaria: Ice cube test applied to the skin for diagnostic confirmation
- Cholinergic urticaria: Exercise challenge testing or controlled heating to reproduce symptoms
- Dermatographic urticaria: Light stroking or scratching of the skin to elicit wheals
- Delayed pressure urticaria: Application of controlled pressure to skin sites for several hours
- Aquagenic urticaria: Controlled water immersion testing at varying temperatures
- Solar urticaria: Phototesting using different light sources (UVA, UVB, and visible light) delivered from light sources positioned ten to fifteen centimeters from the back, with assessment performed every ten minutes for one hour
- Contact urticaria: Controlled exposure to suspected allergens followed by observation for reactions
These diagnostic procedures help confirm the diagnosis and identify specific triggers, enabling patients to develop effective avoidance strategies.
Management and Treatment Approach
The management of CIndU is based on a two-pronged approach: minimizing exposure to identified triggers and utilizing pharmacological treatments to achieve symptom control when trigger avoidance is not feasible.
Trigger Avoidance
Patient education regarding trigger identification and avoidance represents a fundamental component of CIndU management. It is often difficult for patients to completely avoid the physical stimuli that provoke wealing, as the threshold for triggers is frequently low. However, minimizing exposure to triggers as much as possible remains an important management principle. Special considerations include:
- Cold urticaria patients should avoid cold exposure and dress appropriately in warm clothing
- Cholinergic urticaria patients should implement temperature control measures and avoid excessive heat exposure
- Solar urticaria patients should avoid direct sun exposure and wear protective clothing, hats, and sunglasses, along with sunscreens containing high protection index (SPF 50+)
- Aquagenic urticaria patients should minimize water contact duration and avoid unnecessary water exposure
- Dermatographic urticaria patients should minimize skin friction and avoid tight clothing
- Delayed pressure urticaria patients should avoid sustained pressure application and wear loose-fitting clothing
Tolerance Induction
In select cases, inducing tolerance through controlled daily exposure to triggers can be useful, particularly in cold urticaria, cholinergic urticaria, and solar urticaria. However, tolerance induction requires consistent daily exposure to maintain effectiveness, with tolerance lasting only several days after exposure cessation. This approach necessitates careful medical supervision and patient education.
Pharmacological Treatment
First-line therapy: Second-generation H1-antihistamines represent the first-line pharmacological treatment for CIndU. These medications are preferred over first-generation antihistamines due to reduced sedation and improved tolerability. There is no significant difference in the recommended treatment approach between CIndU and CSU regarding antihistamine therapy. Intermittent or continuous treatment with H1-antihistamines is supported by clinical trial data for histamine-mediated forms of CIndU.
Dose escalation: For patients not responding to standard antihistamine doses, dose escalation up to four-fold the standard dose may be attempted, as approximately half of CIndU patients do not respond to second-generation H1-antihistamines at standard doses.
Timed dosing: A key difference between CSU and CIndU treatment involves the potential for as-needed dosing in patients with predictable triggers. Patients may take an H1-antihistamine approximately two hours before anticipated trigger exposure if they can reliably predict when exposure will occur.
Second-line therapy: Omalizumab, a monoclonal antibody with high affinity for free immunoglobulin E (IgE), serves as an effective second-line treatment for antihistamine-refractory cases. The standard dosing regimen involves subcutaneous injection of 300 mg every four weeks. Approximately 65% of patients not responding to antihistamines demonstrate positive responses to omalizumab. However, omalizumab is currently used off-label for CIndU due to the absence of well-designed clinical trials specifically assessing its efficacy in various CIndU subtypes and lack of regulatory approvals for these specific indications.
Immunomodulatory treatments: Immunomodulatory treatments such as dapsone may provide value in particular clinical situations, notably in cold urticaria. However, evidence supporting these alternative treatments remains limited.
Additional Considerations
Patients should avoid medications and substances that may worsen urticaria symptoms, including aspirin, non-steroidal anti-inflammatory drugs (NSAIDs), and alcohol. Tight clothing should also be avoided as it can exacerbate symptoms. Short courses of systemic corticosteroids may provide relief during acute flares; however, topical corticosteroids have no established role in CIndU management.
Prognosis and Long-term Outcomes
CIndU may resolve with appropriate symptom management and consistent avoidance of physical stimuli that trigger reactions. However, in many patients, the threshold for relevant physical triggers remains low, making total symptom avoidance nearly impossible. Achieving complete disease remission requires sustained adherence to treatment protocols and trigger avoidance strategies. Treatment should be continued as required until the urticaria completely clears.
Special Populations and Considerations
International treatment guidelines exist for chronic urticaria management; however, these guidelines should be applied with particular caution in specific populations including children and pregnant or lactating women. Certain medications contraindicated during pregnancy should be avoided in these patient populations, necessitating individualized treatment approaches and consultation with obstetric and dermatologic specialists.
Frequently Asked Questions
Q: What is the difference between chronic inducible urticaria and chronic spontaneous urticaria?
A: The primary difference is that CIndU has identifiable physical triggers that reliably provoke hives, while CSU occurs without an obvious trigger. Additionally, CIndU wheals are typically shorter-lasting than CSU wheals, and CIndU often affects younger patients.
Q: Can chronic inducible urticaria be cured?
A: CIndU may resolve with appropriate treatment and trigger avoidance; however, many patients experience persistent symptoms due to low thresholds for triggering stimuli. Long-term management with antihistamines and trigger avoidance strategies is often necessary.
Q: Is complete avoidance of triggers possible?
A: Complete avoidance is often difficult because many patients have low thresholds for their specific triggers. The goal is to minimize exposure as much as possible while using pharmacological treatment to manage symptoms when exposure occurs.
Q: What should I do if antihistamines don’t work?
A: If standard-dose antihistamines prove ineffective, your healthcare provider may increase the dose up to four-fold. If dose escalation fails, omalizumab or other immunomodulatory treatments may be considered as second-line options.
Q: How long does tolerance induction last?
A: Tolerance induction typically lasts only several days after exposure cessation. Consistent daily exposure to the trigger is required to maintain the tolerance effect.
Q: Are there any medications I should avoid with CIndU?
A: Yes, patients should avoid aspirin, non-steroidal anti-inflammatory drugs (NSAIDs), and alcohol, as these may worsen urticaria symptoms. Tight clothing should also be avoided.
Conclusion
Chronic inducible urticaria represents a distinct subtype of chronic urticaria with identifiable physical triggers and characteristic clinical features. Successful management requires a comprehensive approach combining trigger identification and avoidance with evidence-based pharmacological therapy. Second-generation H1-antihistamines serve as the foundation of treatment, with dose escalation and advanced biologic therapies available for refractory cases. Patient education and individualized treatment planning are essential for optimizing outcomes and improving quality of life in affected individuals.
References
- Chronic inducible urticaria — DermNet NZ. 2024. https://dermnetnz.org/topics/chronic-inducible-urticaria
- Chronic inducible urticaria: Clinical presentation, diagnosis, and management — Skin Allergy Journal. 2024. https://skinallergyjournal.com/chronic-inducible-urticaria-clinical-presentation-diagnosis-and-management/
- Chronic Urticaria: Causes, Symptoms, Diagnosis, & Treatment — Allergy & Asthma Network. 2024. https://allergyasthmanetwork.org/chronic-urticaria/cu-causes-symptoms-diagnosis-treatment/
- Chronic Urticaria — StatPearls, NCBI Bookshelf. 2024. https://www.ncbi.nlm.nih.gov/books/NBK555910/
- Hives (Urticaria) & Angioedema Symptoms, Diagnosis & Treatment — American Academy of Allergy, Asthma & Immunology. 2024. https://www.aaaai.org/tools-for-the-public/conditions-library/allergies/hives-(urticaria)-and-angioedema-overview
- Chronic hives – Symptoms and causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/chronic-hives/symptoms-causes/syc-20352719
Read full bio of medha deb












