Chronic Prostatitis: Symptoms, Causes & Treatment
Comprehensive guide to understanding chronic prostatitis, its symptoms, diagnosis, and effective treatment options.
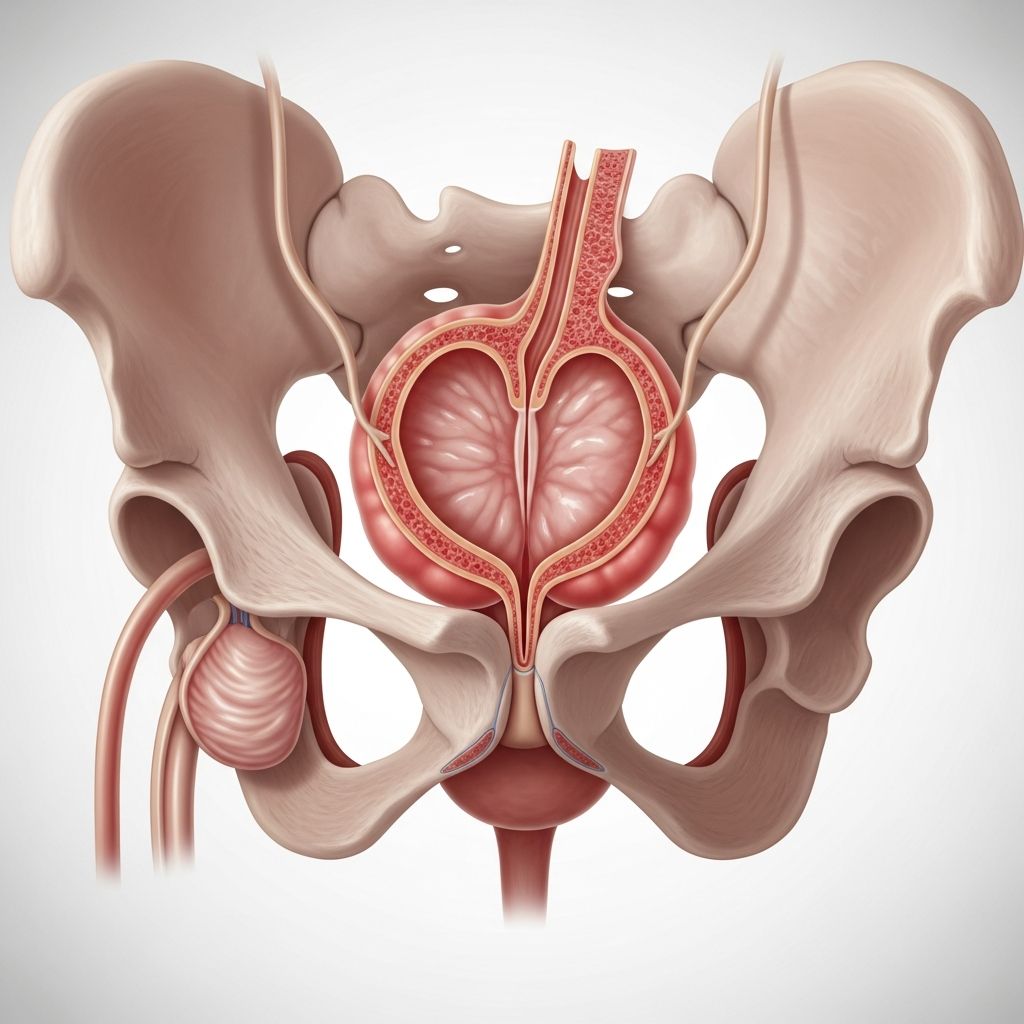
Understanding Chronic Prostatitis
Chronic prostatitis, also known as chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS), is a condition characterized by long-term inflammation and pain in the prostate gland and surrounding pelvic area. This condition affects millions of men worldwide and accounts for approximately 1.8 million doctor visits annually in the United States alone. Unlike acute prostatitis, which develops suddenly and severely, chronic prostatitis develops gradually and can persist for months or years, significantly impacting a man’s quality of life and sexual function.
Between 9% to 16% of men of all ages experience prostatitis at some point in their lives, with the notable distinction that approximately 90% of these cases cannot be attributed to an active bacterial infection. This distinguishes chronic prostatitis from other prostate conditions like benign prostatic hyperplasia (BPH) and prostate cancer, which predominantly affect older men. Understanding the nature of this condition is crucial for effective management and symptom relief.
Types of Prostatitis
Healthcare professionals recognize several distinct types of prostatitis, each with unique characteristics and treatment approaches:
Acute Bacterial Prostatitis
This is the most severe form of prostatitis, developing suddenly with intense symptoms. Men with acute bacterial prostatitis typically experience fever, chills, difficulty urinating, and acute pelvic pain. This type requires immediate medical attention and typically responds well to antibiotic treatment.
Chronic Bacterial Prostatitis
Chronic bacterial prostatitis develops slowly and can persist for three months or longer. The symptoms are similar to acute bacterial prostatitis but less severe, and they may come and go or remain mild throughout. This condition often develops after incomplete treatment of acute bacterial prostatitis or urinary tract infections (UTIs).
Chronic Prostatitis/Chronic Pelvic Pain Syndrome
This is the most common form of prostatitis, accounting for the majority of cases. It is characterized by chronic pain in the pelvic region without evidence of bacterial infection. The symptoms are variable and complex, often requiring a multifaceted treatment approach.
Recognizing the Symptoms
The symptoms of chronic prostatitis vary significantly between individuals and can fluctuate in intensity. Recognizing these symptoms is essential for early diagnosis and treatment.
Primary Symptoms of Chronic Prostatitis/Chronic Pelvic Pain Syndrome
Men with chronic prostatitis commonly experience pain or discomfort lasting three or more months in one or more of the following areas:
- Between the scrotum and anus (perineum)
- The central lower abdomen
- The penis and scrotum
- The lower back and buttocks
- Pain during or after ejaculation
Associated Symptoms
Beyond localized pain, chronic prostatitis may present with additional symptoms that affect daily functioning and urinary health:
- Urinary urgency and frequency, particularly at night (nocturia)
- Difficulty initiating urination (hesitancy)
- Weak urine stream
- Pain or discomfort during urination
- Sexual dysfunction and reduced libido
- Psychological symptoms including anxiety and depression
The pain associated with chronic prostatitis may be continuous or intermittent, appearing suddenly or developing gradually. Some men experience localized pain in specific areas, while others have pain distributed throughout the pelvic region. This variability makes diagnosis and treatment planning particularly challenging.
Diagnostic Approaches
Accurate diagnosis of chronic prostatitis requires a comprehensive evaluation combining clinical history, physical examination, and diagnostic testing.
Medical History and Symptom Assessment
Healthcare providers begin by gathering detailed information about symptom onset, duration, severity, and any factors that worsen or improve symptoms. The National Institutes of Health (NIH) Chronic Prostatitis Symptom Index is a standardized questionnaire that helps assess symptom severity and its impact on quality of life. This tool is valuable for establishing baseline symptoms and measuring treatment effectiveness over time.
Physical Examination
During a physical examination, a healthcare provider typically:
- Examines the body for discharge from the urethra
- Checks for enlarged or tender lymph nodes in the groin
- Assesses for swelling or tenderness in the scrotum
- Performs a digital rectal examination to evaluate the prostate gland
Diagnostic Testing
Laboratory tests may include urinalysis and urine culture to identify bacterial infections. Some specialists may order imaging studies such as ultrasound or MRI to evaluate prostate structure and rule out other conditions. However, diagnosis is often clinical, based on symptom presentation and physical findings, particularly when bacterial infection has been excluded.
Treatment Options and Management Strategies
Treatment for chronic prostatitis is individualized, as no single approach works for every patient. A comprehensive treatment plan typically combines medical therapy with lifestyle modifications and behavioral strategies.
Pharmacological Treatments
Several medication classes have shown effectiveness in managing chronic prostatitis symptoms:
Antibiotics: Although most cases of chronic prostatitis are non-bacterial, urologists may prescribe antibiotics initially to rule out bacterial infection. If bacterial infection is confirmed, prolonged antibiotic therapy may be necessary, potentially lasting up to six months at lower doses to prevent recurrent infection.
Alpha-Blockers: These medications relax bladder muscles near the prostate, reducing urinary symptoms and improving urine flow. Alpha-blockers can significantly decrease painful urination and urinary urgency.
Muscle Relaxants: Medications such as cyclobenzaprine (Amrix, Flexeril) and clonazepam (Klonopin) help reduce pelvic floor muscle tension and associated pain.
Neuromodulators: Drugs including amitriptyline, nortriptyline (Aventyl, Pamelor), and pregabalin (Lyrica) can effectively reduce chronic pain by modulating nerve signals.
Complementary Agents: Chondroitin sulfate and other compounds show promise in reducing inflammation and symptoms associated with chronic prostatitis.
Non-Pharmacological Interventions
Evidence-based non-drug therapies play an important role in chronic prostatitis management:
Physical Therapy and Pelvic Floor Rehabilitation: Specialized physical therapy targeting pelvic floor muscles can significantly reduce pain and improve function. Techniques include myofascial release, stretching, and strengthening exercises to normalize muscle tension.
Relaxation Techniques: Biofeedback and progressive relaxation exercises help reduce muscle tension and stress-related symptom exacerbation.
Phytotherapy: Plant-based extracts including quercetin, bee pollen, and saw palmetto have demonstrated efficacy in some studies for reducing symptoms of chronic prostatitis.
Acupuncture: This traditional therapy may provide pain relief and symptom improvement for some patients.
Behavioral and Lifestyle Modifications
Lifestyle changes significantly impact symptom severity and treatment success:
Sexual Activity Moderation: Maintaining regular but moderate ejaculation frequency is beneficial. While prolonged abstinence can increase pelvic congestion and worsen symptoms, excessive ejaculation (more than seven times per month) may exacerbate pain through pelvic floor muscle spasm. Finding a balanced approach helps maintain sexual health while managing symptoms.
Stress Management: Chronic stress exposure increases the likelihood and severity of pelvic pain through muscle guarding and tension. Effective stress reduction techniques include deep breathing exercises, meditation, yoga, and physical activity. Taking warm baths can help de-stress while relaxing pelvic floor muscles.
Dietary Considerations: Increasing liquid intake and avoiding bladder irritants such as caffeine, alcohol, spicy foods, and acidic beverages can reduce urinary symptoms and pelvic discomfort.
Clothing Choices: Wearing loose, comfortable clothing rather than tight underwear or constrictive pants reduces pressure on the pelvic area and may alleviate symptoms.
Physical Activity: Aerobic exercise and regular physical activity have been found beneficial for managing chronic pain and pelvic pain associated with prostatitis. A sedentary lifestyle may worsen symptoms, while moderate regular exercise promotes healing and symptom relief.
Psychological Support
For men whose symptoms are significantly affected by psychological stress, appropriate psychiatric treatment and stress reduction strategies may reduce symptom recurrence and improve overall quality of life.
Treatment Efficacy Monitoring
Healthcare providers use standardized assessment tools to measure treatment effectiveness. The NIH Chronic Prostatitis Symptom Index questionnaire is administered at multiple timepoints—before treatment, during therapy, and after completion—to objectively assess symptom severity changes and quality of life improvements. This systematic approach helps clinicians adjust treatment strategies based on individual response.
When Surgery May Be Necessary
While surgery is not typically the first-line treatment for chronic prostatitis, it may be considered in specific circumstances. Men experiencing urinary retention caused by chronic bacterial prostatitis may benefit from surgical removal of scar tissue in the urethra, which often improves urine flow and reduces retention symptoms.
Finding the Right Treatment Plan
Because chronic prostatitis presents with diverse symptoms and varies significantly between individuals, treatment must be personalized. Working closely with a urologist experienced in managing chronic prostatitis is essential. Your healthcare team can:
- Accurately diagnose the specific type of prostatitis
- Rule out other urological conditions
- Develop a comprehensive treatment plan combining appropriate medications and therapies
- Monitor treatment effectiveness and adjust strategies as needed
- Provide education about lifestyle modifications and symptom management
It is important to discuss all treatments, including complementary and alternative medical practices and dietary supplements, with your healthcare provider to ensure coordinated and safe care.
Frequently Asked Questions
Q: What is the difference between acute and chronic prostatitis?
A: Acute prostatitis develops suddenly with severe symptoms and typically responds well to antibiotics. Chronic prostatitis develops gradually, lasts three months or longer, and often does not involve bacterial infection, requiring different treatment approaches.
Q: Can chronic prostatitis be cured?
A: While complete cure varies by individual, chronic prostatitis symptoms can be significantly managed through appropriate treatment combinations of medications, physical therapy, and lifestyle modifications. Many men experience substantial symptom improvement with proper management.
Q: Is chronic prostatitis contagious?
A: Most cases of chronic prostatitis are non-bacterial and therefore not contagious. Bacterial prostatitis cases are not typically transmitted between individuals through sexual contact.
Q: How long does chronic prostatitis treatment take?
A: Treatment duration varies significantly depending on the underlying cause and individual response. Some men experience improvement within weeks, while others require months of consistent treatment. Chronic bacterial prostatitis may require antibiotics for up to six months.
Q: Can lifestyle changes alone manage chronic prostatitis?
A: While lifestyle modifications are important components of treatment, most men benefit from a combination of medical therapy, physical rehabilitation, and behavioral changes for optimal symptom management.
Q: How does stress affect chronic prostatitis symptoms?
A: Chronic stress increases muscle tension in the pelvic floor and is directly connected to increased pelvic pain severity. Stress reduction through meditation, exercise, and relaxation techniques can help alleviate symptoms.
References
- Inflammation of the Prostate — National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), National Institutes of Health. 2024. https://www.niddk.nih.gov/health-information/urologic-diseases/prostate-problems/prostatitis-inflammation-prostate
- A Guide To Managing Prostatitis-Related Pelvic Pain — Fusion Wellness Physical Therapy. 2024. https://fusionwellnesspt.com/blog/evidence-based-recommendations-for-managing-prostatitis-related-pain-healthy-sex-and-lifestyle-habits
- Collins MM, Meigs JB, Barry MJ, et al. — Journal of Urology. 2002. Prevalence and correlates of prostatitis in the health professionals follow-up study cohort.
- Gallo L. — Journal of Prostate Cancer and Prostatic Disease. 2014. Evidence-based recommendations for managing prostatitis related pain in men.
- Pierce AN, Christianson JC. — Neuroscience & Biobehavioral Reviews. 2015. Stress and chronic pain: new insights and therapeutic approaches. 49:136-146.
Read full bio of Sneha Tete











