Colon Polyps: Types, Symptoms, Causes & Removal
Understand colon polyps: Learn about types, symptoms, risk factors, and safe removal procedures.
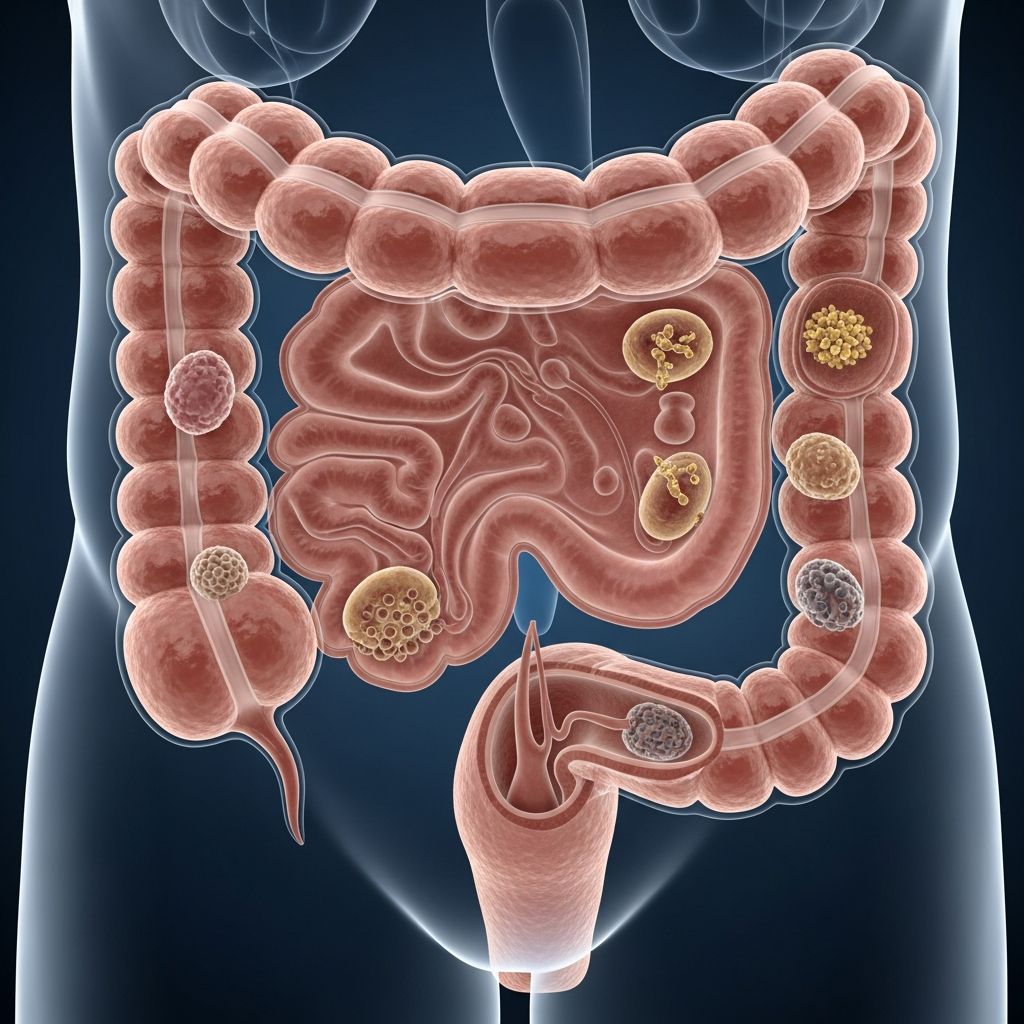
Understanding Colon Polyps
Colon polyps are growths that form on the inside lining of your colon or rectum. These small, bump-like structures are remarkably common, appearing in approximately 30% of routine colonoscopies. While most colon polyps are benign and harmless, some types can develop into colon cancer over many years if left untreated. The good news is that healthcare providers can identify and remove colon polyps during a routine colonoscopy, which significantly reduces your risk of developing colorectal cancer.
Understanding colon polyps is essential for maintaining your digestive health. Since many people with polyps experience no symptoms, regular screening becomes the most effective way to detect these growths before they become problematic. The progression from a benign polyp to cancer typically takes approximately 10 years, providing a substantial window of opportunity for early intervention and prevention.
Types of Colon Polyps
Not all colon polyps are the same. Healthcare providers classify polyps into two main categories: neoplastic and non-neoplastic. Understanding the difference between these types is crucial for determining appropriate follow-up care and cancer risk.
Neoplastic Polyps
Neoplastic polyps have the potential to become cancerous over time. This category includes adenomatous polyps, which are the most common type found during colonoscopies. These polyps originate from the glandular tissue of the colon and can progress through stages from low-grade dysplasia to high-grade dysplasia before eventually becoming cancerous. Adenomatous polyps require removal and careful monitoring through regular follow-up colonoscopies.
Non-Neoplastic Polyps
Non-neoplastic polyps, also known as hyperplastic polyps, typically have little to no cancer risk. These polyps are usually small, common, and rarely require removal unless they are particularly large or causing symptoms. Common types include inflammatory polyps, which develop in response to inflammation in the colon, and hamartomatous polyps, which are growths composed of normal tissue in abnormal locations.
Symptoms of Colon Polyps
One of the most significant challenges with colon polyps is that they often produce no symptoms. Many people with polyps are completely unaware of their presence until a healthcare provider discovers them during screening. However, some individuals may experience symptoms when polyps are large or numerous.
Potential symptoms of colon polyps include:
- Rectal bleeding or blood in the stool
- Changes in bowel habits, such as constipation or diarrhea lasting more than a week
- Abdominal discomfort or cramping
- Iron deficiency anemia, which may result from chronic bleeding
If you experience any of these symptoms, it is important to contact your healthcare provider for evaluation. However, the absence of symptoms does not mean you don’t have polyps, which is why routine screening is so critical for cancer prevention.
Risk Factors for Developing Colon Polyps
Certain factors increase your likelihood of developing colon polyps. Understanding your personal risk profile can help you make informed decisions about screening frequency and preventive measures.
Risk factors include:
- Age over 45 years old
- Family history of colon polyps or colorectal cancer
- Personal history of previous polyps
- Inflammatory bowel disease, such as Crohn’s disease or ulcerative colitis
- Sedentary lifestyle and lack of physical activity
- Unhealthy diet low in fiber and high in processed foods
- Obesity or being overweight
- Smoking and excessive alcohol consumption
- Genetic syndromes associated with polyp development
If you have multiple risk factors, your healthcare provider may recommend more frequent screening or earlier initiation of colonoscopies. As of 2021, it is recommended that all adults have their first colonoscopy at age 45. However, those with risk factors may need to begin screening earlier.
Diagnosis and Detection
The best way to find and identify colon polyps is through a colonoscopy, which is an examination that uses a lighted camera to look inside your colon. During this procedure, your healthcare provider can visualize the entire colon and identify any growths or abnormalities.
The Colonoscopy Procedure
A colonoscopy typically takes about 15 minutes to advance the scope to the end of the large intestine and another 15 minutes to withdraw it, allowing your doctor to examine your entire colon twice. If your healthcare provider finds polyps that need to be removed or treated, the procedure may take additional time.
During a colonoscopy, your healthcare provider can pass specialized tools through the scope to remove polyps or take tissue samples. These samples are sent to a laboratory for further analysis. A pathologist examines the polyp samples under a microscope to identify the type and determine whether cancer cells are present. Results typically take one to two weeks to return.
Other Imaging Tests
While other imaging tests such as CT colonography or virtual colonoscopy can identify colon polyps, colonoscopy remains the gold standard because it allows healthcare providers to both detect and remove polyps during the same procedure. This makes colonoscopy the most efficient and effective screening method.
Polyp Removal and Treatment
The standard treatment for colon polyps is removal, unless you have only non-neoplastic types that carry minimal cancer risk. Most colon polyps can be removed during a colonoscopy through a procedure called polypectomy. This is a simple, minimally invasive procedure that healthcare providers can perform through the colonoscope.
Polypectomy Procedure
During polypectomy, your healthcare provider uses specialized instruments passed through the colonoscope to remove the polyp from the colon wall. The procedure is painless for patients because the colon lining has no sensory nerves. Your provider will choose the appropriate removal technique based on the polyp’s size, location, and characteristics.
In certain cases involving larger or more complex polyps, your surgeon may need to access the polyp through your abdomen using minimally invasive surgical methods such as laparoscopy. This involves passing a scope through one small keyhole incision and operating through another. However, most polyps can be successfully removed during routine colonoscopy without the need for additional surgery.
Advanced Removal Techniques
For particularly difficult cases, healthcare providers may use specialized techniques such as endoscopic mucosal resection (EMR) or endoscopic submucosal dissection (ESD). These advanced procedures allow for the safe removal of large polyps while minimizing complications.
Impact on Colon Cancer Prevention
The importance of polyp removal cannot be overstated. Removal of precancerous polyps by colonoscopy reduces your chance of getting colon cancer by up to 70 percent. This remarkable reduction demonstrates the effectiveness of early detection and removal in preventing one of the most common cancers.
Since colon cancer develops slowly and takes approximately 10 years for a precancerous polyp to turn into a cancerous polyp, regular screening and polyp removal provide a significant opportunity for cancer prevention before symptoms ever develop.
Follow-Up Care and Screening Schedule
Your follow-up screening schedule depends on what your healthcare provider finds during your colonoscopy. The recommendations vary based on the types and numbers of polyps discovered.
After Benign Polyps
If your colonoscopy doesn’t find any neoplastic polyps, you may not need another colonoscopy for 10 years. If benign, non-neoplastic polyps are found, your doctor might recommend continuing your usual recommended screening schedule. However, if a large number of benign polyps were discovered, your doctor may recommend more frequent colonoscopies.
After Precancerous Polyps
If you have neoplastic polyps removed, your provider will recommend you return for follow-up colonoscopy within one, three, five, or seven years, depending on your personal risk factors. If precancerous polyps are found, your doctor may recommend a repeat colonoscopy within 1 to 3 years, and sometimes repeating the procedure within 6 months may be recommended. This allows your healthcare provider to check the area where each polyp was removed and look for other polyps or problems.
Preparing for Your Colonoscopy
Proper preparation is essential for a successful colonoscopy. Your healthcare provider will give you specific instructions, which typically include dietary restrictions and bowel cleansing procedures in the days before your appointment. You’ll need to clear your colon completely so your doctor can see the lining clearly and identify any polyps. Your provider will also discuss any medications you’re taking, as some may need to be adjusted before the procedure. You should arrange for someone to drive you home, as you’ll receive sedation during the procedure.
What to Expect After Polyp Removal
After your colonoscopy and any polyp removal, you may experience mild cramping or bloating as gas used to inflate your colon is expelled. Most patients recover quickly and can return to normal activities the next day. Your healthcare provider will discuss your results and any recommendations for follow-up care before you leave. Even if your polyp is benign, your provider will want to test you again from time to time to see if more polyps appear, as they often do.
Lifestyle Modifications to Reduce Polyp Risk
While screening and removal are the most effective ways to prevent colorectal cancer, adopting healthy lifestyle habits may help reduce your risk of developing polyps in the first place. These include maintaining a diet rich in fiber from fruits, vegetables, and whole grains; exercising regularly; maintaining a healthy weight; limiting red and processed meat consumption; avoiding tobacco and limiting alcohol; and managing stress effectively. These modifications support overall colon health and may reduce polyp formation.
Frequently Asked Questions
Q: How common are colon polyps?
A: Colon polyps are quite common, appearing in approximately 30% of routine colonoscopies. Although most are benign, standard procedure involves removing them when detected.
Q: Can I feel a polyp?
A: Most people cannot feel colon polyps. Many individuals with polyps experience no symptoms at all, which is why regular screening is so important.
Q: Is polyp removal painful?
A: No, polyp removal is a painless procedure because the colon lining contains no sensory nerves. Patients receive sedation during the colonoscopy for comfort.
Q: How long does a colonoscopy take?
A: A typical colonoscopy takes about 30 minutes total—approximately 15 minutes to reach the end of the colon and 15 minutes to withdraw. If polyps need removal, additional time may be required.
Q: What should I do if polyps are found?
A: Follow your healthcare provider’s recommendations regarding removal and follow-up screening. Most polyps can be removed during the same colonoscopy procedure.
Q: Can all polyps become cancer?
A: Not all polyps become cancer. Neoplastic polyps have the potential to become cancerous over time if not removed, while non-neoplastic polyps typically have little to no cancer risk.
Q: At what age should I start getting colonoscopies?
A: As of 2021, it is recommended that all adults have their first colonoscopy at age 45. Those with risk factors may need to begin screening earlier and more frequently.
References
- Colonoscopy: Prep & Procedure Details — Cleveland Clinic. Accessed December 2025. https://my.clevelandclinic.org/health/diagnostics/4949-colonoscopy
- What You Can Do to Catch Colon Cancer Early with Dr. James Church — Cleveland Clinic Podcasts. Accessed December 2025. https://my.clevelandclinic.org/podcasts/butts-and-guts/what-you-can-do-to-catch-colon-cancer-early
- Polypectomy: Definition, Preparation, Procedure & Recovery — Cleveland Clinic. Accessed December 2025. https://my.clevelandclinic.org/health/treatments/23479-polypectomy
- Colon Polyps: Symptoms, Causes, Types & Removal — Cleveland Clinic. Accessed December 2025. https://my.clevelandclinic.org/health/diseases/15370-colon-polyps
- Colon Cancer: Symptoms, Causes & Treatment — Cleveland Clinic. Accessed December 2025. https://my.clevelandclinic.org/health/diseases/14501-colorectal-colon-cancer
- What to Know If Polyps Were Found During Your Colonoscopy — American Cancer Society. Accessed December 2025. https://www.cancer.org/cancer/latest-news/what-to-know-if-polyps-were-found-during-your-colonoscopy.html
- Colonoscopy Procedure and Preparation — Cleveland Clinic. Accessed December 2025. https://pages.clevelandclinic.org/colonoscopy-index-3.html
Read full bio of Sneha Tete











