Liver Disease: 4 Stages, Early Symptoms, And Causes
Understand liver disease symptoms, stages, and progression for early detection and management.
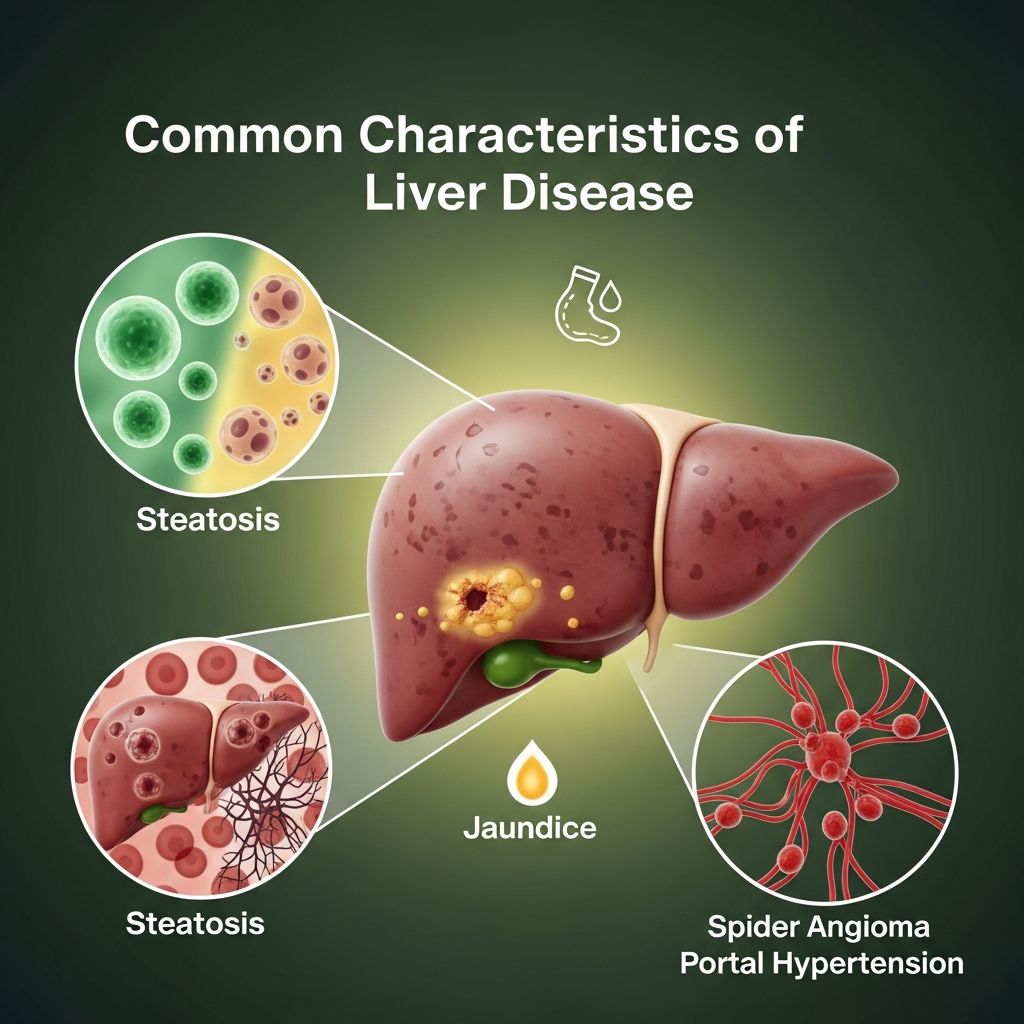
Understanding Common Characteristics of Liver Disease
Liver disease encompasses a wide range of conditions affecting the liver’s ability to function properly. The liver is one of the body’s most vital organs, responsible for filtering blood, producing bile, metabolizing nutrients, and removing toxins. When the liver becomes damaged or diseased, these critical functions are compromised, leading to various symptoms and complications. Understanding the common characteristics of liver disease is essential for early detection and effective management.
The Progression of Chronic Liver Disease
Chronic liver disease typically progresses through distinct stages, each representing increasing severity of damage and functional decline. Recognizing these stages helps healthcare providers and patients understand disease progression and determine appropriate treatment strategies.
Stage One: Hepatitis
Hepatitis refers to inflammation in the liver tissues, which represents the body’s response to injury or toxicity. This inflammation is an attempt to purge infections and initiate the healing process. Acute hepatitis, which occurs as an immediate and temporary response, often successfully resolves the issue. However, when the injury or toxicity persists, so does the inflammation. Chronic hepatitis results from ongoing damage and creates a hyperactive healing response that eventually leads to scarring of liver tissue.
Stage Two: Fibrosis
Fibrosis develops as a gradual stiffening of the liver caused by accumulating thin bands of scar tissue. This scarring reduces blood flow through the liver, limiting its access to oxygen and nutrients, which gradually diminishes the organ’s vitality. Importantly, some degree of fibrosis is reversible. Liver cells possess the remarkable ability to regenerate, and scarring can diminish if damage slows sufficiently to allow recovery.
Stage Three: Cirrhosis
Cirrhosis represents severe, permanent scarring of the liver tissue. At this stage, fibrosis is no longer reversible, as the liver no longer has sufficient healthy cells to regenerate its tissues. However, progression can still be slowed or halted. Cirrhosis begins to affect liver function, but the body attempts to compensate for these losses, which may mean initial symptoms are not immediately apparent.
Stage Four: Liver Failure
Liver failure occurs when the liver can no longer function adequately for the body’s needs, also called decompensated cirrhosis. At this point, the body cannot compensate for functional losses. As liver functions deteriorate, systemic effects become noticeable throughout the body. Chronic liver failure is a gradual process that ultimately proves fatal without a liver transplant.
Early Symptoms of Liver Disease
Chronic liver disease often produces no symptoms during early stages, though it may sometimes begin with acute hepatitis. For instance, a viral hepatitis infection may present with acute symptoms initially. If the immune system fails to eliminate the infection, it progresses to a chronic phase. Early symptoms of liver disease tend to be vague and nonspecific:
- Abdominal pain or discomfort
- Loss of appetite
- Fatigue or lack of energy
- Diarrhea
- General malaise or feeling unwell
Many individuals experience these symptoms without recognizing them as potential liver problems, attributing them instead to other causes.
Advanced Symptoms and Signs
As liver function declines in later stages of disease, more specific and pronounced symptoms emerge. One of the first effects of declining liver function is impaired bile flow in the biliary tract. The liver no longer produces or delivers bile effectively to the small intestine, and bile instead leaks into the bloodstream.
Jaundice and Related Signs
Jaundice represents one of the hallmark signs of advanced liver disease. The skin and whites of the eyes take on a yellow appearance due to excessive bilirubin accumulation. Normally, the liver clears bilirubin efficiently, but a damaged liver cannot keep pace with accumulation. Associated with jaundice, patients often experience persistent itching, which may occur without any visible skin rash and can significantly impact sleep quality and daily activities.
Changes in Bowel and Urine Appearance
The liver produces bile salts responsible for the brown color of healthy stool. When the liver fails to produce bile normally or when bile flow is blocked, stool becomes pale, resembling the color of clay. Additionally, excess bilirubin can cause unusually dark urine, often occurring alongside jaundice.
Fluid Accumulation in the Body
As liver disease advances, it affects blood flow, hormones, and nutritional status. Liver scarring can block blood flow and raise pressure in surrounding blood vessels, causing fluid to seep out and accumulate in the abdomen—a condition called ascites. This may result in mild swelling or significant abdominal enlargement with the belly button protruding outward. In some cases, fluid also accumulates in the legs and ankles. Infected ascites requires antibiotic treatment, and excessive fluid may require drainage through a tube.
Skin and Nail Changes
Advanced liver disease produces distinctive skin manifestations. Spider angiomas appear as red marks resembling spider webs, typically developing on the cheeks, nose, and neck areas. These vascular lesions are strong indicators of liver problems. Patients may also develop palmar erythema, characterized by blotchy red palms, which represents another symptom of advanced liver disease.
Neurological and Systemic Effects
As liver disease progresses, toxin buildup in the body and bloodstream affects multiple organ systems. Lingering fatigue is common among liver disease patients, potentially resulting from the accumulation of toxins that the liver cannot effectively clear. This toxin buildup also impairs brain function, potentially causing confusion, difficulty concentrating, memory problems, or other cognitive changes.
Gastrointestinal Symptoms
Nausea and vomiting are common gastrointestinal manifestations of liver disease. Raised toxin levels worsen these symptoms as disease progresses. In advanced liver failure, patients may experience blood in their vomit or stool, indicating serious complications.
Bleeding and Clotting Disorders
Advanced liver disease increases bleeding tendency, with patients developing bruises more easily. Cuts and nosebleeds may not stop as expected. Paradoxically, while advanced liver disease patients are prone to bleeding, they also face increased risk of blood clots.
Gender-Specific Considerations
While liver disease affects individuals of all genders, certain symptoms may present differently or with varying prominence between men and women. Women may experience specific hormonal-related symptoms, while men may present with different manifestations. Healthcare providers should consider these gender-specific variations when evaluating patients for liver disease.
End-Stage Liver Disease Complications
End-stage liver disease refers to decompensated cirrhosis and liver failure, when the liver has lost its regenerative capacity and is in decline. The most significant complications include portal hypertension and primary liver cancer, which are leading causes of hospitalization and death in cirrhosis and liver failure patients.
Portal Hypertension
Portal hypertension develops when liver scarring compresses the portal vein running through the organ. Elevated blood pressure in this vessel causes the body to divert blood flow to other connected veins, which become enlarged and stretched thin. These varices can leak, rupture, and bleed, potentially causing sudden, severe, and life-threatening internal bleeding.
Hepatocellular Carcinoma
While not all chronic liver disease patients develop primary liver cancer, most individuals with liver cancer have underlying chronic liver disease. The repeated cycle of inflammation, repair, and scarring alters liver cells in ways that increase cancer risk. Healthcare providers believe that chronic hepatitis viruses may particularly interfere with liver cell DNA, further increasing carcinoma development.
Causes and Risk Factors
Over 100 types of liver disease exist, falling into several categories based on etiology. Common causes include viral infections, alcohol consumption, fatty liver disease, autoimmune conditions, genetic disorders, and medication-induced injury. Certain factors increase liver disease susceptibility, including excessive alcohol consumption, obesity, viral hepatitis infection, family history of liver disease, and certain medical conditions like diabetes.
Diagnostic Approaches
Healthcare providers employ multiple methods to diagnose liver disease. Initial assessment includes physical examination to identify visible signs, followed by questions about symptoms, diet, lifestyle, and medical history. Laboratory tests measure liver enzymes, bilirubin levels, and other markers of liver function. Imaging scans, including ultrasound, CT scans, or MRI, visualize liver structure and detect abnormalities. In some cases, liver biopsy provides definitive diagnosis by examining tissue samples under microscopy.
Understanding Disease Transmission and Prevalence
Certain liver diseases, particularly those caused by hepatitis viruses, require understanding of transmission routes. Hepatitis C represents a significant public health concern, with over 3 million people infected in the United States, though more than half remain undiagnosed. Hepatitis C transmits through contact with infected blood, and many individuals remain unaware of their infection status. Notably, most individuals living with hepatitis C do not experience obvious symptoms, making screening crucial for identification.
Why Early Recognition Matters
Understanding common liver disease characteristics is critical because early detection enables intervention before irreversible damage occurs. Many individuals can have liver disease without feeling ill, as symptoms often develop only after significant damage has occurred. Early recognition allows for lifestyle modifications, medical treatment, and management strategies that can halt disease progression or allow the liver to heal. Once damage becomes extensive, restoration options become limited, making early identification and intervention paramount.
Frequently Asked Questions
Q: Can liver disease be reversed?
A: Some stages of liver disease can be reversed or halted. Early-stage fibrosis may be reversible if the underlying cause is eliminated and the liver receives adequate support to recover. However, once cirrhosis develops, scarring becomes permanent, though disease progression can often be slowed or stopped with appropriate treatment and lifestyle changes.
Q: What are the most common causes of liver disease?
A: Common causes include chronic viral hepatitis infections, excessive alcohol consumption, nonalcoholic fatty liver disease, autoimmune hepatitis, genetic conditions, and medication-induced liver injury. The specific cause varies by population and geography.
Q: How is liver disease diagnosed?
A: Diagnosis typically involves physical examination, medical history assessment, blood tests measuring liver enzymes and function markers, and imaging studies like ultrasound or CT scans. In some cases, liver biopsy provides definitive diagnosis by examining tissue samples.
Q: Can people have liver disease without symptoms?
A: Yes, many individuals have liver disease without experiencing symptoms, especially in early stages. This is why screening and regular check-ups are important for those at risk, particularly those with hepatitis virus infections or other risk factors.
Q: What lifestyle changes help manage liver disease?
A: Eliminating alcohol consumption, maintaining healthy weight, eating a balanced diet, managing blood sugar levels, and avoiding hepatotoxic substances are crucial. Regular medical follow-up and adherence to prescribed treatments are also essential for optimal outcomes.
References
- Liver Disease: Signs & Symptoms, Causes, Stages, Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/17179-liver-disease
- Slideshow: Symptoms of Liver Problems — WebMD. 2024. https://www.webmd.com/fatty-liver-disease/ss/slideshow-symptoms-liver-problems
- Hepatitis C: Overview and Public Health Impact — Johns Hopkins Medicine Viral Hepatitis Center. 2018. https://www.hopkinsmedicine.org/health/conditions-and-diseases/viral-hepatitis
- Liver Pathology and Clinical Assessment — Johns Hopkins University School of Medicine. 2024. https://pathology.jhu.edu/gi-liver/for-patients
Read full bio of Sneha Tete











