COPD: Symptoms, Causes, Diagnosis, And Treatment Guide
Understand chronic obstructive pulmonary disease: symptoms, causes, stages, treatments, and prevention strategies for better lung health.
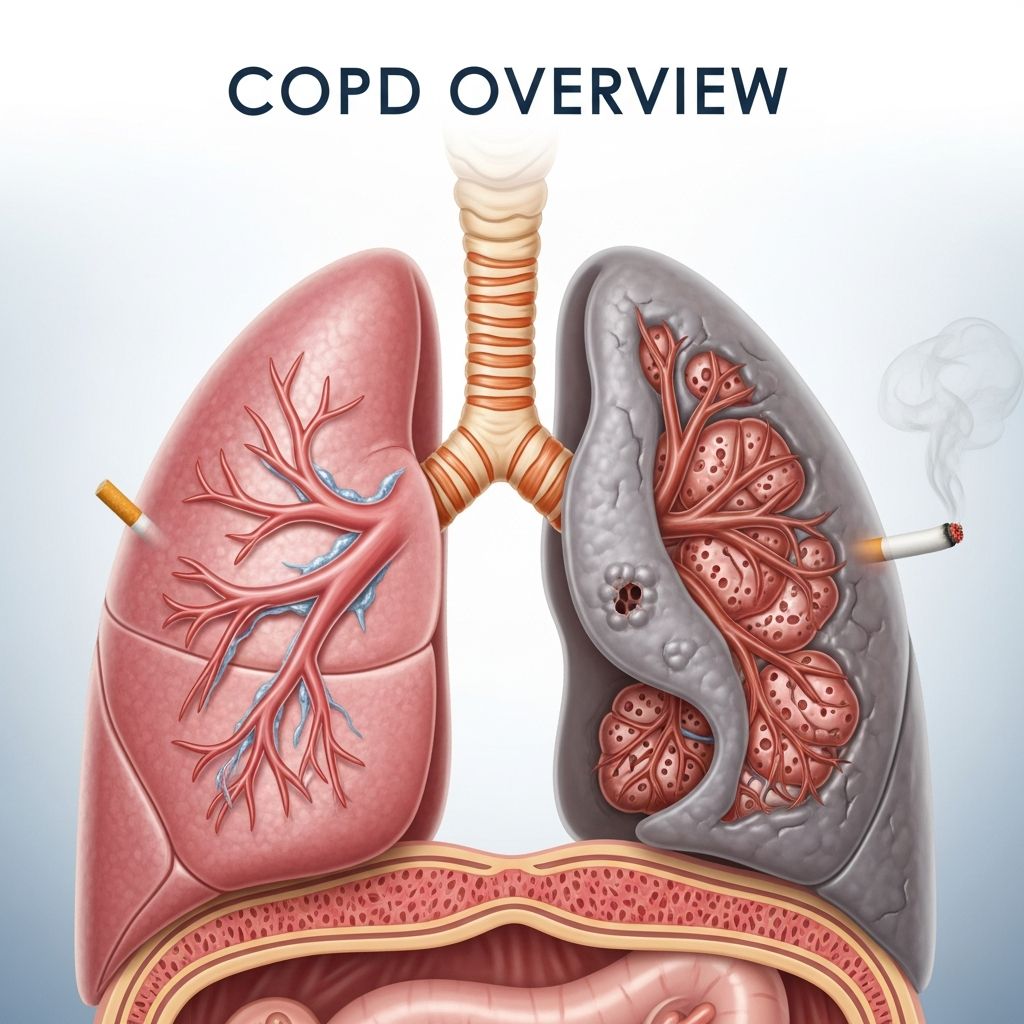
Chronic obstructive pulmonary disease (COPD) is a progressive lung condition characterized by persistent airflow limitation, primarily caused by smoking and exposure to harmful particles or gases. It encompasses chronic bronchitis and emphysema, leading to breathing difficulties that worsen over time.
What Is COPD?
COPD refers to a group of lung diseases that obstruct airflow and cause breathing problems, including emphysema (damage to air sacs) and chronic bronchitis (inflammation of bronchial tubes with excess mucus production). The Global Initiative for Chronic Obstructive Lung Disease (GOLD) defines it as a disease state with airflow limitation that is not fully reversible, usually progressive, and associated with an abnormal inflammatory response in the lungs to noxious particles or gases. Unlike asthma, which features reversible airflow obstruction and airway hyperresponsiveness, COPD’s limitations are poorly reversible.
Key features include loss of lung elasticity, inflamed and narrowed airways, damaged alveoli (air sacs), and thick mucus buildup, making breathing increasingly difficult. COPD develops gradually, often over decades, and affects millions worldwide as a leading cause of morbidity and mortality.
COPD Symptoms
Symptoms of COPD typically emerge in mid-life and worsen progressively, including:
- Shortness of breath, especially during physical activity
- Chronic cough, often with phlegm (clear, white, yellow, or green mucus)
- Wheezing or whistling sounds when breathing
- Chest tightness
- Fatigue and lack of energy
- Frequent respiratory infections
- Unintended weight loss and muscle weakness in advanced stages
Early stages may be asymptomatic, with symptoms appearing when forced expiratory volume in 1 second (FEV1) drops to about 50% of predicted normal. As COPD advances, daily activities become challenging due to breathlessness. Exacerbations—sudden worsenings—can cause increased dyspnea, cough, and sputum, lasting days to weeks.
COPD Causes and Risk Factors
The primary cause of COPD is long-term exposure to irritants that damage lungs and airways. Key risk factors include:
- Smoking: The leading cause, responsible for 85-90% of cases; tobacco smoke inflames airways and destroys lung tissue.
- Air pollution: Indoor (e.g., biomass fuel) and outdoor pollution narrow airways and promote mucus production.
- Occupational exposure: Dust, chemicals, and fumes in workplaces like mining or manufacturing.
- Genetics: Alpha-1 antitrypsin deficiency, a rare genetic disorder causing early-onset COPD.
- Early life events: Low birth weight, prematurity, childhood respiratory infections, or asthma impairing lung growth.
- Secondhand smoke: Increases risk in non-smokers.
Not all smokers develop COPD; genetic susceptibility and cumulative exposure determine risk.
COPD Diagnosis
Diagnosis begins with suspecting COPD in patients with typical symptoms like chronic cough and dyspnea. Confirmation requires spirometry—a breathing test measuring FEV1 and forced vital capacity (FVC). A post-bronchodilator FEV1/FVC ratio <0.70 indicates airflow limitation consistent with COPD.
Additional tests may include:
- Chest X-ray or CT scan to assess lung damage and rule out other conditions
- Arterial blood gas analysis for oxygen and carbon dioxide levels
- Alpha-1 antitrypsin deficiency screening in early-onset or non-smoker cases
- 6-minute walk test for exercise capacity
In low-resource settings, spirometry may be unavailable, leading to underdiagnosis. Early detection is crucial to slow progression.
COPD Stages
COPD severity is classified using the GOLD system, combining spirometry (FEV1 percentage predicted) with symptom burden and exacerbation history:
| Stage | FEV1 % Predicted | Description |
|---|---|---|
| GOLD 1 (Mild) | ≥80% | Few symptoms; often undiagnosed |
| GOLD 2 (Moderate) | 50-79% | Shortness of breath with activity |
| GOLD 3 (Severe) | 30-49% | Severe breathlessness; frequent exacerbations |
| GOLD 4 (Very Severe) | <30% | Life-threatening; respiratory failure possible |
Staging guides treatment; stages aren’t solely tied to symptoms.
COPD Treatment
There is no cure for COPD, but treatments relieve symptoms, prevent exacerbations, and improve quality of life:
- Bronchodilators: Inhaled short- and long-acting medications (e.g., albuterol, tiotropium) relax airway muscles.
- Inhaled corticosteroids: For frequent exacerbators, reduce inflammation.
- Combination inhalers: Bronchodilator + steroid for better control.
- Oxygen therapy: For low blood oxygen levels, extends survival.
- Pulmonary rehabilitation: Exercise, education, and nutrition programs enhance endurance.
- Surgery: Lung volume reduction or transplant in select severe cases.
- Vaccinations: Flu, pneumococcal, and COVID-19 to prevent infections.
Treatment is personalized based on stage, symptoms, and exacerbations.
COPD Exacerbations
Exacerbations are acute symptom worsenings beyond daily variation, often triggered by infections (bacterial/viral), pollution, or unknown causes. Symptoms include intensified dyspnea, cough, and sputum changes; severe cases lead to respiratory failure. Management involves:
- Increased bronchodilators and oral corticosteroids
- Antibiotics if infection suspected
- Hospitalization for oxygen or ventilation if needed
Frequent exacerbations accelerate decline; early intervention is key.
COPD Complications
COPD raises risks for:
- Respiratory infections (pneumonia, flu)
- Heart disease and heart failure
- Lung cancer
- Muscle wasting, osteoporosis, and depression
- Respiratory failure in end-stage disease.
Systemic effects like weight loss and frailty compound issues.
COPD Prevention and Management
Prevention focuses on avoiding risks:
- Quit smoking and avoid secondhand smoke
- Reduce pollutant exposure
- Get vaccinated and practice infection prevention (hand hygiene, masks)
- Maintain healthy weight and exercise.
Self-management tips:
- Follow medication schedules
- Use energy-conserving techniques
- Join support groups
- Monitor symptoms and seek early care for exacerbations.
Lifestyle changes can significantly slow progression.
Frequently Asked Questions (FAQs)
What is the difference between COPD and asthma?
COPD features irreversible airflow limitation from lung damage, while asthma involves reversible obstruction and airway hyperreactivity.
Is COPD curable?
No, but symptoms can be managed effectively with medications, rehabilitation, and lifestyle changes to improve quality of life.
How can I prevent COPD exacerbations?
Avoid triggers like infections and pollution, adhere to medications, get vaccinated, and follow your action plan.
Can you live a long life with COPD?
Yes, with proper management; progression varies, and many live years without severe symptoms.
Who is at risk for COPD?
Primarily smokers, those exposed to pollutants, with occupational dust/chemical exposure, or genetic factors like alpha-1 deficiency.
References
- Chronic Obstructive Pulmonary Disease: An Overview — National Center for Biotechnology Information (PMC). 2014-08-15. https://pmc.ncbi.nlm.nih.gov/articles/PMC4106574/
- Chronic Obstructive Pulmonary Disease (COPD) — Cleveland Clinic. 2023-11-20. https://my.clevelandclinic.org/health/diseases/8709-chronic-obstructive-pulmonary-disease-copd
- Chronic obstructive pulmonary disease (COPD) — World Health Organization. 2023-05-10. https://www.who.int/news-room/fact-sheets/detail/chronic-obstructive-pulmonary-disease-(copd)
- COPD – Symptoms and causes — Mayo Clinic. 2023-07-02. https://www.mayoclinic.org/diseases-conditions/copd/symptoms-causes/syc-20353679
Read full bio of medha deb











