Corns And Calluses: Causes, Treatment, Prevention Guide
Comprehensive guide to understanding, preventing, and treating corns and calluses for healthier skin.
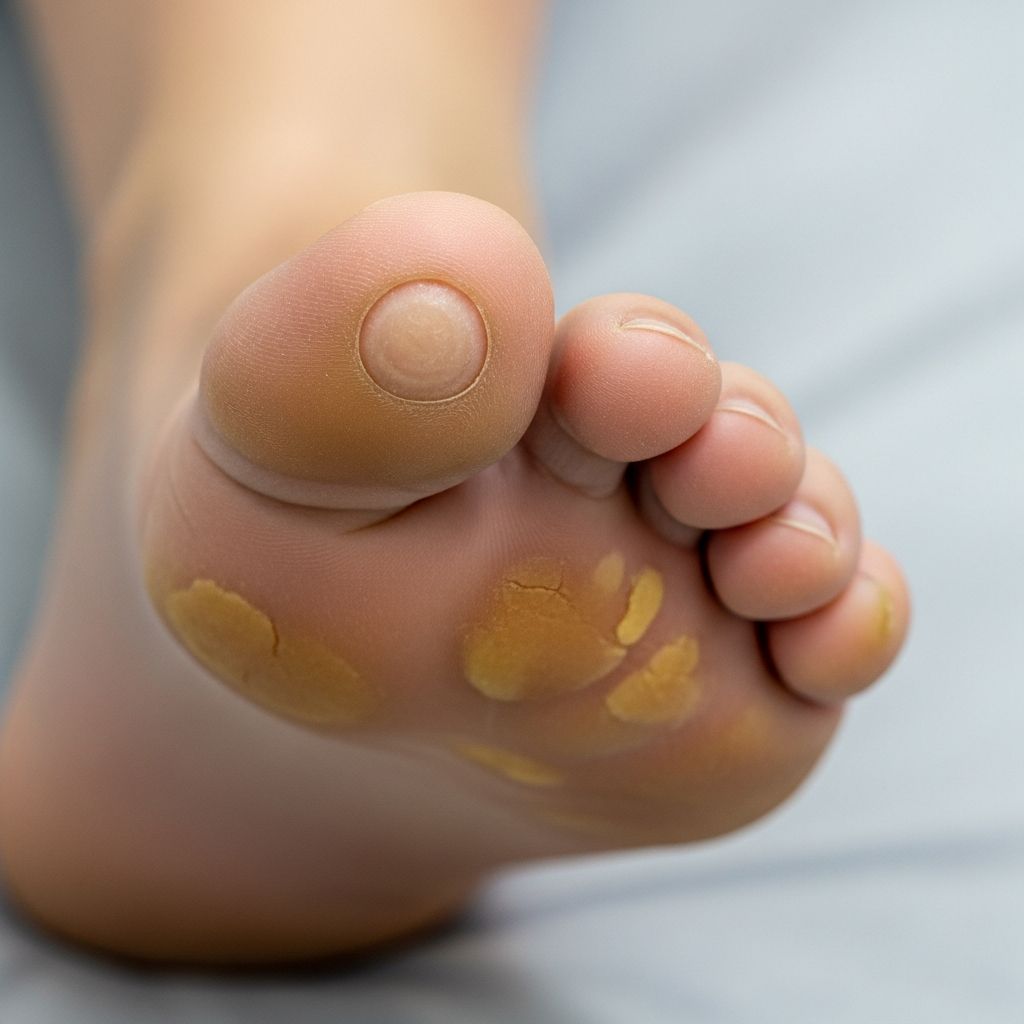
Corns and calluses (heloma, tyloma)
Corns and calluses are localised areas of thickened skin (hyperkeratosis) that develop due to repeated friction, pressure, or mechanical irritation. These protective responses of the skin often occur on the feet and hands but can appear elsewhere. Corns are typically smaller, more defined lesions with a central core, while calluses are broader and diffuse. Understanding their differences aids in effective management.
What are corns and calluses?
Corns, also known as heloma durum (hard corns) or heloma molle (soft corns), and calluses, or tyloma, form as the epidermis thickens in response to chronic stress. The skin produces excess keratin, leading to hardened plaques. Corns feature a sharp, conical core of keratin that extends into deeper dermal layers, often causing pain by pressing on nerves or bone. Calluses lack this core and are generally painless unless severe.
These conditions are common, affecting millions worldwide, particularly those in occupations involving repetitive hand or foot use, such as manual laborers or athletes. Risk increases with age due to reduced skin elasticity and slower cell turnover.
Who gets corns and calluses?
Anyone exposed to repeated friction can develop corns or calluses, but certain groups are more susceptible:
- People wearing ill-fitting shoes, especially high heels or narrow footwear.
- Individuals with foot deformities like bunions, hammertoes, or high arches.
- Athletes, runners, and those participating in sports causing repetitive impact.
- Manual workers using tools without gloves, such as gardeners or mechanics.
- Older adults, diabetics, or those with peripheral vascular disease due to poor circulation and neuropathy.
- People with abnormal gait or weight distribution issues.
Children rarely develop them unless from sports or congenital deformities. Women are more prone due to fashionable footwear choices.
What causes corns and calluses?
The primary cause is mechanical irritation from:
- Friction and pressure: Rubbing from shoes, socks, or tools.
- Footwear issues: Tight, loose, or high-heeled shoes concentrating pressure on toes or balls of feet.
- Bony prominences: Enlarged joints or malaligned toes.
- Repetitive activities: Walking, running, gripping, or weightlifting.
- Underlying conditions: Arthritis, obesity, or inherited keratoderma.
Soft corns thrive in moist interdigital spaces, while hard corns form on dry, exposed areas.
What are the clinical features of corns and callus?
Corns
- Hard corns (heloma durum): Small, well-defined, yellow-white plaques with a hard central core on toes, often the fifth toe or dorsal surfaces. Painful on pressure.
- Soft corns (heloma molle): Whitish, macerated lesions between toes (e.g., 4th/5th interspace) due to moisture; prone to infection.
- Seed corns: Tiny, clustered bumps on non-weight-bearing heel or ball of foot; usually asymptomatic.
- Fibrous corns: Tough, deeper lesions resistant to treatment.
Calluses
- Diffuse, thickened, yellowish skin without a core, often on soles, palms, or heels.
- Painless unless cracked or fissured; may cause discomfort if extensive.
- Hyperkeratotic with possible surrounding erythema.
| Feature | Corns | Calluses |
|---|---|---|
| Size/Shape | Small, focal, conical core | Large, diffuse, flat |
| Location | Toes, bony prominences | Soles, palms, heels |
| Pain | Often painful (core presses nerves) | Usually painless |
| Appearance | Hard/soft with central plug | Thickened, uniform hyperkeratosis |
Diagnosis
Diagnosis relies on clinical examination. History reveals friction sources, and inspection shows characteristic features. Paring with a scalpel differentiates: corns reveal a translucent core, calluses smooth skin, warts disrupted dermatoglyphs or black dots. Biopsy is rare but confirms in atypical cases. Differential includes plantar warts, porokeratosis, or psoriasis.
What is the treatment for a corn or callus?
Self-care and conservative measures
Address the cause first:
- Wear well-fitting shoes with adequate toe space; avoid high heels.
- Use protective padding: felt pads, moleskin, or silicone toe props.
- Soak in warm water 10-20 minutes 2-3x/week, then gently file with pumice stone or emery board. Moisturise daily with urea or emollient creams.
Topical treatments
- Keratolytics: Salicylic acid (10-40%) plasters, gels, or urea (10-40%) creams/plasters soften keratin. Apply to lesion only, protect surrounding skin with petrolatum. Use up to 3 months; avoid in diabetes/vascular disease.
- Examples: Salactol, Hydromol intensive, Eucerin urea cream.
Professional care
- Podiatrist debridement: Sharp removal of hyperkeratosis for immediate relief.
- Orthotics or custom insoles to redistribute pressure.
- Enucleation for recurrent corns.
Surgical options
For refractory cases with deformities: excision of underlying bone (e.g., arthroplasty), soft tissue correction, or bursae removal. Reserved for failures of conservative therapy.
Prevention of corns and calluses
- Select proper footwear: Wide toe box, low heels, breathable materials.
- Wear gloves for manual tasks; use protective gear in sports.
- Maintain foot hygiene: Regular moisturising, pumicing.
- Manage weight and treat deformities early.
- Custom orthotics for biomechanical issues.
Possible complications
- Infection (bacterial/fungal) in soft corns or cracks.
- Ulceration, bleeding from over-paring.
- Pain, gait changes, secondary deformities.
- In diabetics: Non-healing ulcers risking amputation.
Special circumstances
Diabetics/peripheral vascular disease patients: Avoid self-paring/salicylic acid; seek professional care promptly to prevent ulcers. Children require supervision to avoid injury.
Frequently asked questions
Q: Can I cut off a corn at home?
No. Cutting risks infection, bleeding, and scarring. Use gentle filing after soaking.
Q: Are salicylic acid products safe?
Safe for most, but avoid on legs, in diabetes, or near infected skin. Follow instructions.
Q: How long do treatments take?
Improvement in 1-4 weeks with consistent care; recurrence common if cause persists.
Q: When to see a doctor?
If painful, infected, diabetic, no improvement after 2 weeks, or recurrent.
Q: Do calluses go away on their own?
Often yes, if friction stops; otherwise, they thicken.
References
- Corns and Calluses – NHS Kernow Referral Management Service — RMS Cornwall NHS. 2023-12. https://rms.cornwall.nhs.uk/primary_care_clinical_referral_criteria/rms/primary_care_clinical_referral_criteria/dermatology/corns_and_calluses
- Corns and Calluses: Causes, Symptoms, and Home Treatments — Healthgrades. Accessed 2026. https://resources.healthgrades.com/right-care/foot-health/corns-and-calluses
- Calluses and Corns — Merck Manuals Professional Edition. Accessed 2026. https://www.merckmanuals.com/professional/dermatologic-disorders/cornification-disorders/calluses-and-corns
- Calluses and corns | Healthify — Healthify NZ. Accessed 2026. https://healthify.nz/health-a-z/c/calluses-and-corns
- Corns and Calluses (heloma, tyloma) — DermNet NZ. Accessed 2026. https://dermnetnz.org/topics/corn-callus
- Corns and Callus Podiatry Management – 2025 Guide — Algeos. 2025. https://www.algeos.com/company-news/post/algeos-product-guides/podiatry-for-corn-callus
Read full bio of Sneha Tete













