Coronary Heart Disease: Causes, Symptoms, and Treatment
Understanding coronary heart disease: symptoms, risk factors, diagnosis, and effective treatment options.
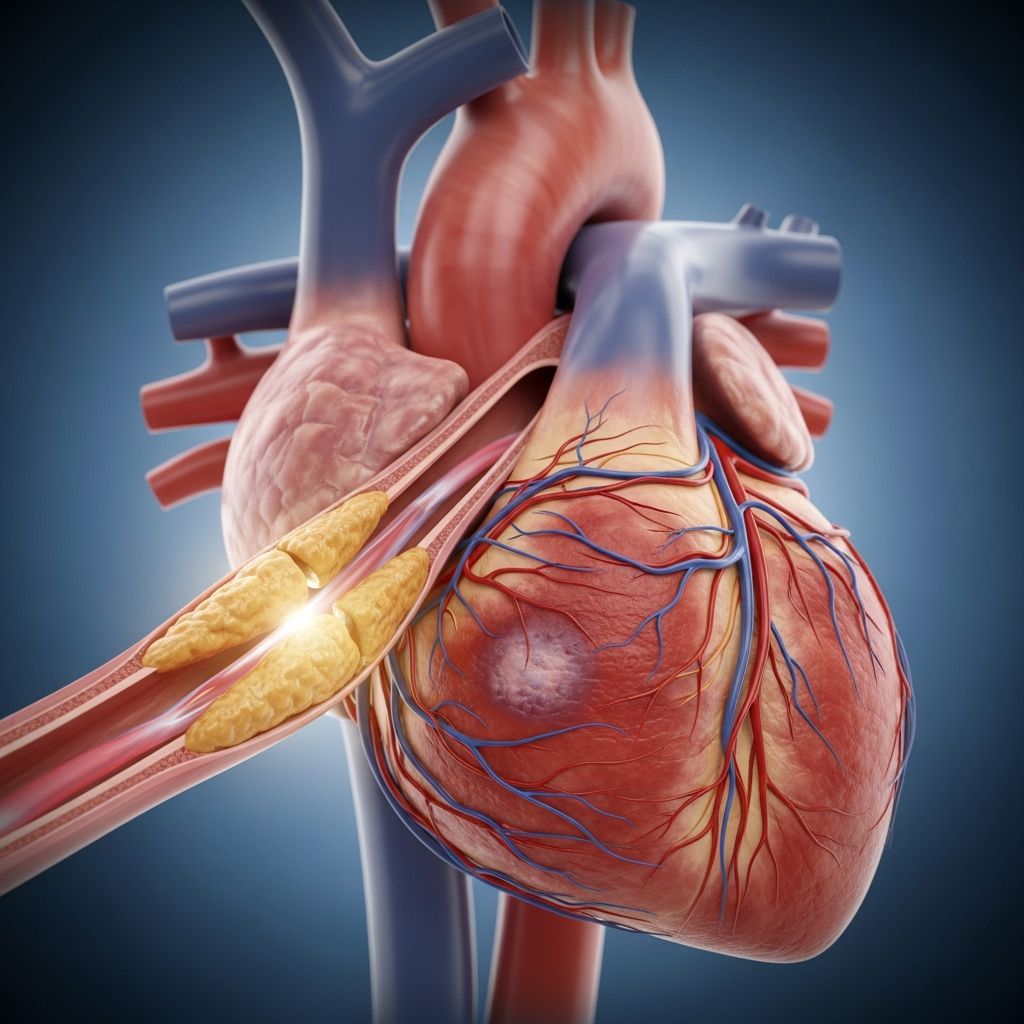
Understanding Coronary Heart Disease
Coronary heart disease (CHD), also known as coronary artery disease, stands as one of the leading causes of death in the United States. This condition develops when the coronary arteries, which supply oxygen-rich blood to the heart muscle, become narrowed or blocked due to plaque buildup. When blood flow to the heart is restricted, the heart muscle may not receive enough oxygen, leading to chest pain, shortness of breath, or a heart attack. Understanding this disease, its risk factors, and treatment options is essential for prevention and management.
What Is Coronary Heart Disease?
Coronary heart disease occurs when fatty deposits called plaque accumulate on the inner walls of the coronary arteries, a process known as atherosclerosis. Over time, this buildup narrows the arteries, reducing blood flow to the heart. The coronary arteries branch from the aorta and deliver oxygen-rich blood to the heart muscle, allowing it to pump efficiently. When these vital vessels become compromised, the heart cannot function optimally.
The disease can manifest in several ways: asymptomatic coronary artery disease, where blockages exist without obvious symptoms; angina, characterized by chest pain or discomfort; or acute myocardial infarction, commonly known as a heart attack, which occurs when blood flow is severely restricted or completely blocked.
Risk Factors for Coronary Heart Disease
Multiple factors increase your likelihood of developing coronary heart disease. Understanding these risk factors allows you to take preventive measures and modify controllable aspects of your lifestyle.
Non-Modifiable Risk Factors
Certain risk factors cannot be changed but are important to understand:
- Age: Men aged 45 and older and women aged 55 and older face increased risk
- Family History: Having relatives with early coronary heart disease significantly raises your risk
- Gender: Men generally develop coronary heart disease at younger ages than women
Modifiable Risk Factors
These factors can be controlled through lifestyle changes and medical management:
- High Blood Pressure: Elevated blood pressure damages artery walls, facilitating plaque buildup
- High Cholesterol: Excess LDL cholesterol contributes directly to plaque formation
- Smoking: Tobacco use damages the arterial lining and increases clot formation risk
- Diabetes: High blood sugar levels accelerate atherosclerosis development
- Obesity: Excess weight increases strain on the heart and other risk factors
- Physical Inactivity: Regular exercise strengthens the heart and improves circulation
- Poor Diet: High-fat, high-sodium diets contribute to plaque accumulation
- Stress: Chronic stress may increase blood pressure and heart disease risk
Symptoms and Warning Signs
Recognizing symptoms of coronary heart disease is crucial for seeking timely medical attention. Symptoms vary from person to person and may differ between men and women.
Angina Symptoms
Angina, or chest pain, is the most common symptom of coronary heart disease. This discomfort typically occurs with exertion or emotional stress and may feel like:
- Pressure or squeezing in the chest
- Pain radiating to the arms, neck, jaw, or shoulder
- Shortness of breath
- Fatigue or weakness
Heart Attack Symptoms
A heart attack requires immediate emergency medical attention. Warning signs include:
- Severe chest pain or pressure
- Pain in the arms, back, neck, jaw, or stomach
- Extreme shortness of breath
- Cold sweats and nausea
- Lightheadedness or dizziness
Women may experience different symptoms, such as unusual fatigue, jaw pain, or indigestion-like discomfort. If you experience any of these symptoms, call emergency services immediately.
Diagnosis of Coronary Heart Disease
Accurate diagnosis involves several tests and evaluations to assess the extent of coronary artery blockage and heart function.
Initial Evaluation
Your healthcare provider will review your medical history, assess risk factors, and perform a physical examination, including blood pressure measurement and listening to your heart with a stethoscope.
Blood Tests
Blood work measures cholesterol levels, triglycerides, and cardiac biomarkers such as troponin, which indicate heart damage. High-sensitivity troponin tests can detect very small amounts of heart damage.
Electrocardiogram (EKG)
This test records the heart’s electrical activity and can reveal abnormalities in heart rhythm or previous heart attacks. During an EKG, electrodes placed on your skin transmit heart signals to a machine that displays your heart’s electrical patterns.
Stress Testing
Stress tests evaluate how your heart responds to increased demands. You may walk on a treadmill or receive medication that simulates exercise while your heart activity is monitored. This test helps identify blockages that cause inadequate blood flow during exertion.
Imaging Studies
Several imaging techniques provide detailed views of coronary arteries:
- Chest X-ray: Shows the size and shape of your heart and lungs
- Echocardiogram: Uses ultrasound to create moving images of your heart structure and function
- Coronary Computed Tomography Angiography (CCTA): Provides detailed images of coronary arteries using CT technology with contrast dye
- Nuclear Stress Test: Combines stress testing with radioactive tracers to visualize blood flow to the heart muscle
Cardiac Catheterization
This invasive procedure involves threading a thin tube through blood vessels to the heart. Contrast dye injected through the catheter highlights coronary arteries on X-ray images, revealing blockage locations and severity. Catheterization not only diagnoses the condition but also allows for immediate treatment if blockages are found.
Treatment Options
Treatment plans are individualized based on disease severity, symptoms, and overall health. The goal is to reduce symptoms, prevent heart attacks, and improve survival.
Lifestyle Modifications
Lifestyle changes form the foundation of coronary heart disease management:
- Diet: Adopt a heart-healthy diet rich in fruits, vegetables, whole grains, and lean proteins while limiting saturated fats and sodium
- Exercise: Engage in at least 150 minutes of moderate-intensity aerobic activity weekly, as approved by your healthcare provider
- Smoking Cessation: Quitting smoking dramatically improves outcomes and reduces future cardiac events
- Weight Management: Achieving a healthy weight reduces strain on your heart
- Stress Reduction: Practice relaxation techniques such as meditation or yoga
- Alcohol Moderation: Limit alcohol consumption to recommended amounts
Medications
Several medications help manage coronary heart disease and reduce complications:
- Statins: Lower cholesterol levels and stabilize plaque
- Beta-blockers: Reduce heart rate and blood pressure, decreasing heart workload
- ACE Inhibitors: Lower blood pressure and reduce strain on the heart
- Antiplatelet Agents: Aspirin and other agents prevent blood clots
- Nitrates: Dilate blood vessels to improve blood flow and reduce chest pain
- Calcium Channel Blockers: Relax blood vessels and improve blood flow
Revascularization Procedures
When medications prove insufficient, invasive procedures restore blood flow to the heart muscle.
Percutaneous Coronary Intervention (PCI)
During PCI, a catheter with a balloon at its tip is guided to the blockage site. The balloon is inflated to compress plaque against the artery wall, widening the vessel. Most procedures include stent placement—a small metal mesh tube that keeps the artery open and prevents re-narrowing.
Coronary Artery Bypass Grafting (CABG)
This surgical procedure creates new pathways for blood to reach the heart by grafting healthy blood vessels around blocked coronary arteries. Surgeons typically use saphenous veins from the leg or internal mammary arteries from the chest. CABG is often recommended for patients with multiple blockages, severely narrowed left main coronary artery, or those unsuitable for PCI.
Prognosis and Complications
The outlook for coronary heart disease depends on disease severity, treatment timing, and how well you manage risk factors. Early diagnosis and aggressive treatment of risk factors significantly improve prognosis. However, coronary heart disease can lead to serious complications including heart attack, heart failure, arrhythmias, and sudden cardiac death if left untreated.
Prevention Strategies
Prevention is always preferable to treatment. Implementing preventive measures reduces your risk of developing coronary heart disease or experiencing recurrent events.
- Maintain healthy blood pressure below 120/80 mmHg
- Keep total cholesterol below 200 mg/dL and LDL cholesterol below 100 mg/dL
- Avoid tobacco products in all forms
- Maintain a healthy body weight with BMI between 18.5 and 24.9
- Exercise regularly and maintain an active lifestyle
- Follow a Mediterranean or DASH diet
- Manage diabetes effectively if you have this condition
- Control stress through healthy coping mechanisms
- Limit alcohol consumption
- Get adequate sleep, aiming for 7-9 hours nightly
Frequently Asked Questions
Q: Can coronary heart disease be reversed?
A: While advanced atherosclerotic plaques cannot be completely reversed, aggressive lifestyle changes and medications can slow disease progression and stabilize existing plaques, reducing heart attack risk significantly.
Q: How often should I be screened for coronary heart disease?
A: Screening frequency depends on age, risk factors, and family history. Men over 45 and women over 55 should discuss screening with their healthcare provider, particularly if they have multiple risk factors.
Q: What is the difference between angina and a heart attack?
A: Angina involves temporary chest discomfort when blood flow is restricted but not completely blocked. A heart attack occurs when blood flow is severely restricted or completely blocked, causing permanent heart muscle damage.
Q: Is coronary heart disease preventable?
A: While you cannot modify some risk factors like age and family history, controlling modifiable risk factors through lifestyle changes and medical management can significantly reduce your coronary heart disease risk.
Q: Can I exercise if I have coronary heart disease?
A: Yes, regular exercise is beneficial for coronary heart disease patients. However, exercise programs should be tailored to your condition and approved by your cardiologist. Cardiac rehabilitation programs provide supervised exercise and education.
References
- Cardiovascular Disease Screening and Management — Johns Hopkins Diabetes Guide, The Johns Hopkins University. 2016. https://www.hopkinsguides.com/hopkins/view/Johns_Hopkins_Diabetes_Guide/547024/all/Cardiovascular_Disease_Screening_and_Management
- Coronary Heart Disease: Definition and Classification — American Heart Association. 2024. https://www.heart.org/
- Prevention and Risk Factor Modification — National Institutes of Health, National Heart, Lung, and Blood Institute. 2024. https://www.nhlbi.nih.gov/
Read full bio of Sneha Tete











