Crohn’s Disease: Symptoms, Causes, Treatment
Comprehensive guide to Crohn's disease: Understand symptoms, causes, diagnosis, treatments, and living with this chronic IBD condition.
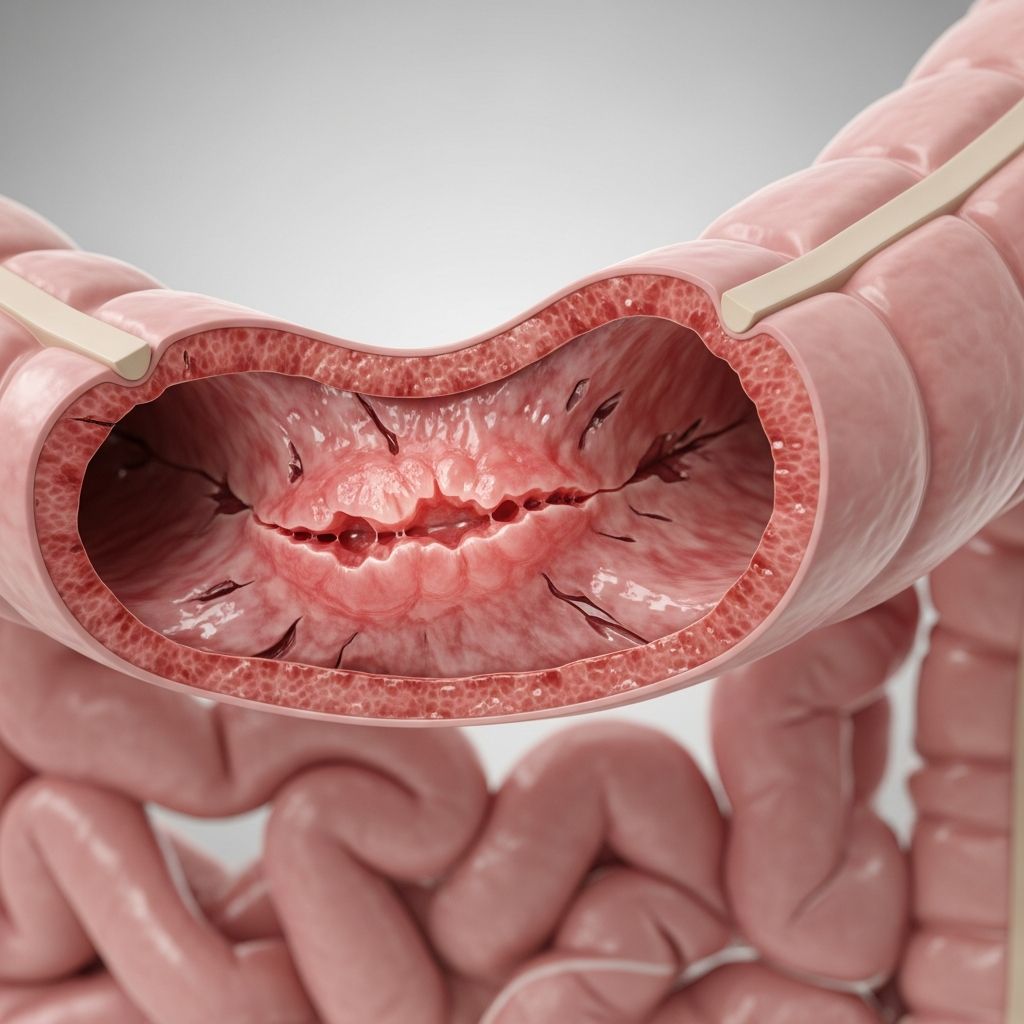
Crohn’s disease is a type of inflammatory bowel disease (IBD) that causes chronic inflammation of the digestive tract. Unlike other digestive conditions, Crohn’s can affect any part of the gastrointestinal (GI) tract, from the mouth to the anus, though it most commonly impacts the end of the small intestine (ileum) and the beginning of the large intestine (colon). This unpredictable condition leads to symptoms like abdominal pain, severe diarrhea, fatigue, weight loss, and malnutrition, significantly affecting quality of life.
Affecting over 780,000 Americans, Crohn’s disease has no cure but is manageable with medications, lifestyle changes, diet, and sometimes surgery. According to the Centers for Disease Control and Prevention (CDC), IBD cases have risen, with Crohn’s being one of two main types alongside ulcerative colitis. Understanding Crohn’s is crucial for early diagnosis and effective management.
Symptoms of Crohn’s Disease
Crohn’s symptoms vary widely in intensity and location, often flaring up and then entering remission periods. Common symptoms include:
- Abdominal pain and cramping: Typically in the lower right abdomen, worsening after eating.
- Persistent diarrhea: Can be bloody or contain pus, leading to dehydration.
- Fatigue: Due to inflammation, anemia, and nutrient malabsorption.
- Weight loss and reduced appetite: From pain, diarrhea, and poor nutrient absorption.
- Fever: During active flares.
- Mouth sores: Painful ulcers (aphthous ulcers).
Depending on the affected area, additional symptoms emerge:
Small Intestine Involvement (Ileitis)
- Pain in the middle or lower right abdomen
- Cramping after meals
- Reduced appetite and weight loss
- Diarrhea limiting nutrient absorption, especially B12 and bile salts
Colon Involvement
- Bloody diarrhea
- Anal fissures or fistulas
- Skin lesions (erythema nodosum)
- Eye inflammation (uveitis)
- Joint pain or arthritis
Rectum Involvement
- Painful bowel movements
- Constipation or feeling of incomplete emptying
- Fecal incontinence
Extra-intestinal manifestations affect about 40% of patients, including skin rashes, eye inflammation, liver issues, kidney stones, and weakened bones. Children may experience growth delays.
Crohn’s Disease vs. Ulcerative Colitis
Both are IBDs but differ significantly:
| Aspect | Crohn’s Disease | Ulcerative Colitis |
|---|---|---|
| Affected Area | Any GI tract part; patchy, skip lesions | Colon and rectum only; continuous |
| Depth | Full thickness (transmural) | Mucosa and submucosa |
| Complications | Fistulas, strictures, abscesses | Toxic megacolon, perforation |
| Small Bowel Cancer Risk | Higher | Lower (colon-focused) |
Causes of Crohn’s Disease
The exact cause remains unknown, but it’s believed to result from an abnormal immune response where the body attacks its own GI tract. Key factors include:
- Genetics: Over 200 genes linked; 10-20% have family history. Higher risk if a close relative has IBD.
- Immune System: Triggers like infections lead to chronic inflammation.
- Environmental Factors: Smoking (doubles risk, triples surgery need), Western diets high in fats/sugars, urban living.
- Microbiome Imbalance: Dysbiosis contributes to inflammation.
- Childhood Factors: Breastfeeding and hygiene hypothesis suggest protection.
Risk Factors for Crohn’s Disease
- Age: Most diagnosed 15-35; possible second peak 50-70.
- Ethnicity: Higher in White people of Ashkenazi Jewish descent; rising in Black populations.
- Family History: Increases risk 10-fold.
- Smoking: Worst modifiable factor.
- NSAIDs: May trigger flares.
- Geography: Northern climates higher risk.
Diagnosis of Crohn’s Disease
Diagnosis combines history, exams, blood/stool tests, imaging, and endoscopy. No single test confirms it.
- Medical History & Exam: Symptoms, family history, abdominal tenderness.
- Blood Tests: Anemia, inflammation markers (CRP, ESR), antibodies (ASCA).
- Stool Tests: Calprotectin, lactoferrin for inflammation; rule out infections.
- Endoscopic Procedures: Colonoscopy with biopsy (gold standard), upper endoscopy, capsule endoscopy, balloon-assisted enteroscopy.
- Imaging: CT/MR enterography, small bowel follow-through, endoscopic ultrasound, MRI for fistulas.
Treatment for Crohn’s Disease
Treatment aims for remission using medications, nutrition, and surgery. Tailored to disease location and severity.
Anti-Inflammatory Drugs
- Corticosteroids (prednisone, budesonide) for flares.
- Oral 5-ASAs (less effective).
Immune Suppressants
- Azathioprine, methotrexate, JAK inhibitors (tofacitinib).
Biologics
- Anti-TNF (infliximab, adalimumab), ustekinumab, vedolizumab, risankizumab.
Antibiotics
Metronidazole, ciprofloxacin for abscesses/fistulas.
Surgery
70% need surgery; not curative. Includes strictureplasty, resection, colectomy.
Nutritional Support
Enteral/parenteral nutrition for malnutrition.
Crohn’s Disease Diet and Nutrition
No specific diet cures Crohn’s, but modifications help:
- Avoid triggers (dairy, high-fiber during flares).
- Low-residue, Mediterranean, SCD, low-FODMAP diets.
- Supplements: calcium, D, iron, B12, multivitamins.
- Hydration vital; limit caffeine/alcohol.
Complications of Crohn’s Disease
- Bowel Obstruction: Scarring causes blockages.
- Fistulas: 33-50% develop abnormal connections.
- Abscesses: Pus pockets.
- Anal Issues: Fissures, fistulas, hemorrhoids.
- Malnutrition: Weight loss, deficiencies.
- Colon Cancer: 2% risk after 10 years.
- Osteoporosis: From steroids/malabsorption.
Living With Crohn’s Disease
Manage with medication adherence, trigger avoidance, stress reduction (yoga, meditation), support groups (Crohn’s & Colitis Foundation), mental health care. Track symptoms with apps/journals.
Frequently Asked Questions (FAQs)
Is Crohn’s disease fatal?
Not typically, but complications like colorectal cancer or infections can be serious. Proper management improves outcomes.
Is Crohn’s disease an autoimmune disease?
Yes, it involves immune system dysfunction attacking the GI tract.
What triggers a Crohn’s flare-up?
Smoking, NSAIDs, infections, stress, certain foods.
Can you live a normal life with Crohn’s disease?
Yes, many do with treatment, though flares may occur.
Does Crohn’s disease cause weight gain or loss?
Usually loss during flares; gain possible on steroids.
Can Crohn’s disease be sexually transmitted?
No.
Does Crohn’s disease get worse with age?
Not necessarily; some improve post-surgery.
References
- What is IBD? — Centers for Disease Control and Prevention. 2024-05-21. https://www.cdc.gov/ibd/what-is-IBD.htm
- Crohn’s Disease — National Institute of Diabetes and Digestive and Kidney Diseases. 2023-01-27. https://www.niddk.nih.gov/health-information/digestive-diseases/crohns-disease
- Crohn’s disease — Mayo Clinic. 2024-07-08. https://www.mayoclinic.org/diseases-conditions/crohns-disease/symptoms-causes/syc-20353304
- Crohn’s Disease: What It Is, Symptoms, Causes & Treatment — Cleveland Clinic. 2024-02-08. https://my.clevelandclinic.org/health/diseases/9357-crohns-disease
- Epidemiology of inflammatory bowel disease — National Center for Biotechnology Information. 2022. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9090751/
- AGA Clinical Practice Guidelines on the Medical Management of Moderate to Severe Luminal and Perianal Fistulizing Crohn’s Disease — American Gastroenterological Association. 2021-06-01. https://doi.org/10.1053/j.gastro.2021.04.063
Read full bio of medha deb











