Crohn’s Disease Symptoms: 8 Common Signs To Spot
Recognize the early warning signs of Crohn's disease, from digestive distress to extraintestinal effects, for timely diagnosis and management.
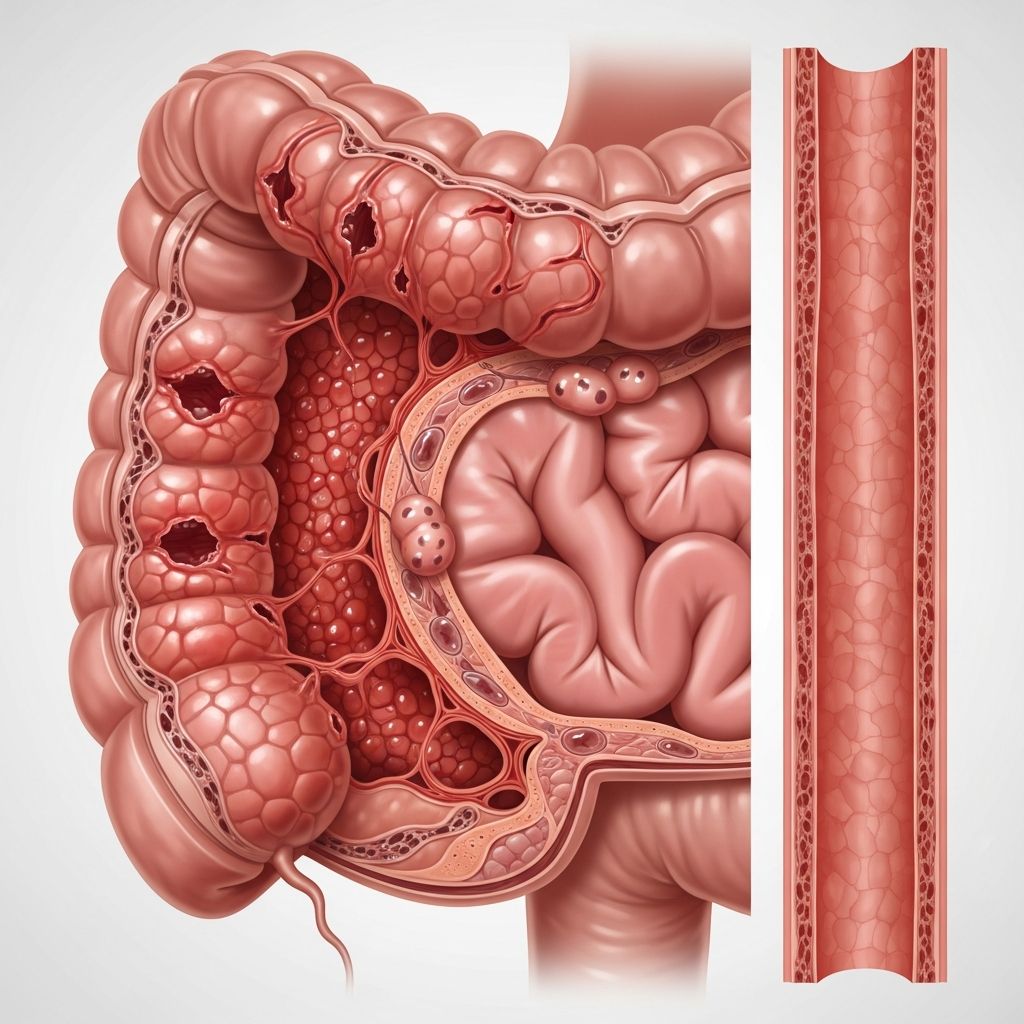
Crohn’s disease is a chronic inflammatory bowel disease (IBD) that causes inflammation in the digestive tract, leading to a range of symptoms from mild discomfort to severe complications. It can affect any part of the gastrointestinal (GI) tract, most commonly the end of the small intestine and the beginning of the large intestine, with symptoms varying based on the location and severity of inflammation.
Symptoms often develop gradually but can appear suddenly, including persistent diarrhea, abdominal pain, fatigue, and weight loss. Periods of remission without symptoms are common, but flare-ups can significantly impact quality of life. Early recognition is crucial for managing the condition and preventing complications like ulcers, fistulas, and malnutrition.
What Is Crohn’s Disease?
Crohn’s disease is a type of IBD characterized by chronic inflammation that extends through multiple layers of the bowel wall. Unlike ulcerative colitis, which is limited to the colon, Crohn’s can occur anywhere from the mouth to the anus, often in patchy segments known as “skip lesions.”
The inflammation disrupts normal digestion, leading to pain, diarrhea, and nutrient malabsorption. It affects millions worldwide, with higher prevalence in developed countries and among people of Ashkenazi Jewish descent. While the exact cause remains unknown, factors like genetics, immune system dysfunction, environmental triggers, and gut microbiome imbalances contribute to its development.
Diagnosis typically involves blood tests, stool tests, endoscopy, colonoscopy, imaging like CT or MRI scans, and sometimes biopsy to confirm inflammation patterns unique to Crohn’s. Treatment focuses on reducing inflammation with medications such as corticosteroids, immunomodulators, biologics, and lifestyle changes, though there is no cure.
Crohn’s Disease Symptoms
Symptoms of Crohn’s disease vary widely depending on the affected area of the GI tract. Common signs include:
- Diarrhea: Frequent, loose stools, often urgent and watery, due to inflammation in the intestines.
- Abdominal pain and cramping: Typically in the lower right abdomen, worsening after eating.
- Fatigue: Profound tiredness from anemia, malnutrition, or chronic inflammation.
- Fever: Low-grade during flare-ups, indicating active inflammation.
- Blood in stool: Bright red or dark, tarry stools from ulcers or fissures.
- Mouth sores: Painful aphthous ulcers on the lips, gums, or inside the cheeks.
- Reduced appetite and weight loss: From pain, malabsorption, or nausea.
- Pain or drainage near the anus: From fistulas or abscesses.
These symptoms can range from mild to severe and may come and go. In children, growth delays and delayed puberty are additional concerns.
Where Crohn’s Disease Occurs
Crohn’s can affect any GI segment:
- Ileum (end of small intestine): Most common site, causing diarrhea, cramping, and weight loss.
- Colon (large intestine): Leads to bloody diarrhea and urgency.
- Multiple areas: Widespread inflammation increases complication risks.
- Mouth or upper GI: Rare, but can cause sores or swallowing issues.
The pattern—continuous or patchy—helps differentiate it from other IBDs.
Symptoms Outside the Intestines
Crohn’s disease often manifests beyond the gut, affecting up to 40% of patients with extraintestinal symptoms:
- Joints: Arthritis in knees, ankles, or spine, mirroring intestinal flares.
- Eyes: Uveitis, episcleritis causing redness, pain, and vision changes.
- Skin: Erythema nodosum (painful red nodules) or pyoderma gangrenosum (ulcerating sores).
- Liver and bile ducts: Primary sclerosing cholangitis, leading to jaundice.
- Kidney stones: From oxalate malabsorption or dehydration.
- Anemia: Iron or B12 deficiency from bleeding or poor absorption.
These symptoms can precede GI issues, complicating diagnosis.
When to See a Doctor
Consult a healthcare provider if you experience persistent symptoms such as:
- Abdominal pain or cramping.
- Diarrhea lasting over two weeks.
- Unexplained weight loss.
- Blood in stool.
- Fever with GI symptoms.
- Nausea or vomiting preventing eating.
Prompt evaluation prevents complications like bowel obstruction. Family history of IBD warrants screening.
Crohn’s Disease Complications
Untreated Crohn’s leads to serious issues:
- Bowel obstruction: Scarring narrows the intestine, causing bloating and vomiting.
- Ulcers: Deep sores in the GI tract, mouth, or anus.
- Fistulas: Abnormal tunnels between organs or skin, often infected.
- Fissures: Tears in anal lining causing pain and bleeding.
- Anal abscesses: Pus collections requiring drainage.
- Malnutrition: Nutrient deficiencies from malabsorption.
| Complication | Description | Risk Factors |
|---|---|---|
| Bowel Obstruction | Narrowing from scar tissue | Repeated flares |
| Fistulas | Abnormal connections | Deep inflammation |
| Malnutrition | Vitamin/mineral deficits | Diarrhea, resection |
| Colon Cancer | Increased risk in colon | Long-standing disease |
Long-term risks include blood clots and colorectal cancer.
Crohn’s Disease Causes and Risk Factors
The precise cause is unknown, but involves:
- Immune system: Abnormal response attacks healthy tissue.
- Genetics: Family history increases risk 10-fold.
- Environment: Smoking doubles risk; NSAIDs worsen symptoms.
- Microbiome: Bacterial imbalances trigger inflammation.
Risk factors include age (teens-30s), family history, smoking, and Caucasian ethnicity.
How Crohn’s Disease Is Diagnosed
Diagnosis uses:
- Medical history and exam.
- Blood/stool tests: For inflammation (CRP, calprotectin), infection, anemia.
- Endoscopy/colonoscopy: Visualizes inflammation, biopsies.
- Imaging: CT, MRI, ultrasound for strictures/fistulas.
- Capsule endoscopy: For small bowel.
Differential diagnosis rules out infections, IBS, celiac.
Crohn’s Disease Treatment
Treatment aims for remission:
- Medications: Aminosalicylates, steroids, biologics (anti-TNF like infliximab).
- Surgery: For strictures, fistulas (resection, stricturoplasty).
- Lifestyle: Diet (low-residue during flares), quit smoking, stress management.
- Nutrition: Supplements for deficiencies.
Personalized plans improve outcomes.
Living With Crohn’s Disease
Manage with education, support groups, mental health care. Track flares via apps, adhere to meds, maintain bone health with calcium/vitamin D. Pregnancy is possible with planning.
Frequently Asked Questions
Can Crohn’s disease be cured?
No, but treatments achieve long-term remission.
Does stress cause Crohn’s flares?
Stress may trigger flares but doesn’t cause the disease.
Is Crohn’s disease hereditary?
Genetic risk exists, but environment plays a role.
Can diet cure Crohn’s?
Diet helps manage symptoms but not cure.
What foods trigger Crohn’s?
Common triggers: dairy, fiber, spicy foods—individualized.
References
- Crohn’s Disease – Symptoms and Causes — Mayo Clinic. 2023-10-28. https://www.mayoclinic.org/diseases-conditions/crohns-disease/symptoms-causes/syc-20353304
- Crohn’s Disease — National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). 2023-03-07. https://www.niddk.nih.gov/health-information/digestive-diseases/crohns-disease
- Crohn’s Disease — Centers for Disease Control and Prevention (CDC). 2024-01-15. https://www.cdc.gov/ibd/what-is-ibd/crohns-disease.htm
- Clinical Manifestations and Diagnosis of Crohn Disease in Adults — UpToDate (Wolters Kluwer). 2025-11-20. https://www.uptodate.com/contents/clinical-manifestations-and-diagnosis-of-crohn-disease-in-adults
- Crohn’s Disease: Symptoms, Causes & Treatment — Cleveland Clinic. 2024-05-12. https://my.clevelandclinic.org/health/diseases/9357-crohns-disease
Read full bio of medha deb











