Crohn’s Disease Vs. Ulcerative Colitis: 5 Key Differences
Understand the key differences between Crohn's disease and ulcerative colitis to navigate diagnosis, treatment, and management effectively.
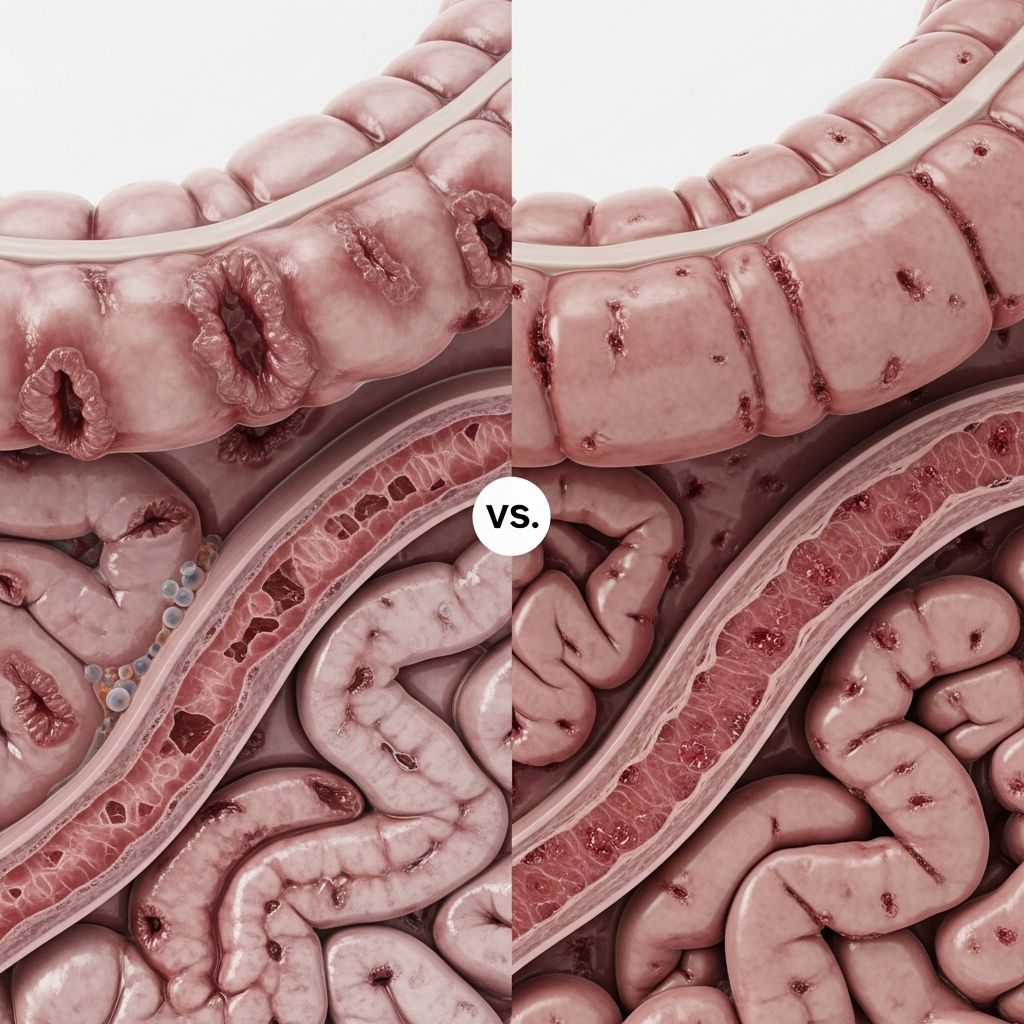
Crohn’s disease and ulcerative colitis are the two primary types of
inflammatory bowel disease (IBD)
, chronic conditions causing inflammation in the digestive tract. While they share overlapping symptoms like abdominal pain and diarrhea, key differences in location, inflammation patterns, and complications guide diagnosis and treatment.Accurate differentiation is crucial because treatments vary, and misdiagnosis can lead to suboptimal outcomes. This article breaks down their similarities, differences, symptoms, causes, diagnosis, treatments, complications, and FAQs to empower patients and caregivers.
What Are Inflammatory Bowel Diseases (IBD)?
**IBD** refers to chronic disorders involving inflammation of the gastrointestinal (GI) tract. The main forms are Crohn’s disease and ulcerative colitis. Unlike irritable bowel syndrome (IBS), which causes similar symptoms but no inflammation or tissue damage, IBD leads to ulcers, bleeding, and potential long-term complications.
IBD affects millions worldwide, often striking teenagers and young adults, with a higher prevalence in developed countries. Both conditions result from an abnormal immune response attacking the gut lining, influenced by genetics, environment, and microbiota.
Crohn’s Disease vs. Ulcerative Colitis: Similarities
Despite differences, Crohn’s and ulcerative colitis share core traits:
- Chronic inflammation of the digestive tract, leading to flares and remissions.
- Common symptoms: abdominal cramps, persistent diarrhea, rectal bleeding, urgent bowel needs, incomplete evacuation sensation, appetite/weight loss, fatigue, and night sweats.
- Extraintestinal manifestations (EIMs): joint pain, skin rashes, eye inflammation, anemia, liver/kidney issues, and bone density loss.
- Demographics: Peak onset in teens/young adults (15-35 years); equal male/female risk; family history increases likelihood.
- No known cure; managed lifelong with medications, diet, and sometimes surgery.
These overlaps often make initial distinction challenging, mimicking infections or IBS.
The hallmark distinctions lie in affected areas, inflammation patterns, and depth:
| Aspect | Crohn’s Disease | Ulcerative Colitis |
|---|---|---|
| Location | Anywhere from mouth to anus; commonly ileum (small intestine end) and colon. | Limited to colon and rectum (large intestine). |
| Inflammation Pattern | Patchy (“skip lesions”) with healthy tissue between inflamed areas. | Continuous from rectum upward. |
| Depth of Inflammation | All bowel wall layers (transmural), causing fistulas/strictures. | Mucosa/submucosa (innermost lining) only. |
| Unique Symptoms | Mouth sores, anal fissures/ulcers, perianal disease, nutrient malabsorption (due to small bowel involvement). | Bloody diarrhea more prominent; less perianal issues. |
| Complications | Fistulas, abscesses, strictures, bowel obstruction; higher small bowel cancer risk. | Toxic megacolon, perforation; higher colon cancer risk with pancolitis. |
These differences stem from Crohn’s transmural involvement versus UC’s superficial spread.
Crohn’s Disease: Detailed Overview
Crohn’s disease is unpredictable, affecting any GI segment but most often the terminal ileum and colon (Crohn’s colitis). Inflammation penetrates deep, leading to scarring, narrowing (strictures), and abnormal connections (fistulas) between bowel loops or to skin/bladder.
Symptoms vary by location: small bowel involvement causes diarrhea/malnutrition; colonic adds bleeding/cramping. Perianal disease (fissures, abscesses) affects up to 50% of patients. Extraintestinal issues like arthritis occur in 25-40%.
Crohn’s Disease Symptoms
- Persistent diarrhea (may or may not have blood).
- Abdominal pain/cramping, often right lower quadrant.
- Fatigue, fever, weight loss.
- Mouth ulcers, anal pain/bleeding/drainage.
- Extraintestinal: joint swelling, skin lesions (erythema nodosum), eye redness.
Ulcerative Colitis: Detailed Overview
Ulcerative colitis (UC) starts in the rectum, spreading continuously proximally. Severity ranges from proctitis (rectum only) to pancolitis (entire colon). Inflammation erodes the mucosal surface, causing friable tissue, ulcers, and bleeding.
Symptoms intensify with disease extent; bloody stools are hallmark due to superficial vascular exposure. Systemic symptoms like fever/fatigue occur in severe flares.
Ulcerative Colitis Symptoms
- Bloody diarrhea with mucus/pus (key distinguisher).
- Abdominal cramping, tenesmus (urgency).
- Frequent bowel movements (10-20/day in flares).
- Fever, dehydration, tachycardia in acute cases.
- Extraintestinal: same as Crohn’s but primary sclerosing cholangitis more common.
Causes and Risk Factors
Exact causes remain unknown, but multifactorial:
- Genetics: 20-25% familial risk; over 200 IBD-associated genes (e.g., NOD2 for Crohn’s).
- Immune System: Dysregulated response attacks gut bacteria as foreign.
- Environmental: Smoking worsens Crohn’s, protects against UC; Western diet, antibiotics disrupt microbiome.
- Microbiome: Reduced diversity in IBD patients.
Both equally affect genders; Crohn’s slightly more in Ashkenazi Jews.
Diagnosis: How Do Doctors Tell Them Apart?
Diagnosis combines history, labs, imaging, and endoscopy. No single test; often trial-and-error initially (5-10% reclassified later).
- Medical History/Physical: Symptom pattern, family history, extraintestinal signs.
- Blood/Stool Tests: Anemia, inflammation markers (CRP, ESR), calprotectin/fecal lactoferrin (distinguishes IBD from IBS).
- Endoscopy: Colonoscopy with biopsies shows continuous vs. patchy inflammation, depth.
- Imaging: CT/MRI enterography for small bowel; ultrasound for complications.
- Capsule Endoscopy: For suspected small bowel Crohn’s.
Definitive: Visual/histological patterns (e.g., granulomas in Crohn’s).
Treatment Options
Tailored to location/severity; goals: induce remission, prevent flares/complications.
Medications (Step-Up Approach)
- Mild: 5-ASAs (mesalamine) more effective in UC.
- Moderate-Severe: Corticosteroids (budesonide for ileal Crohn’s), immunomodulators (azathioprine), biologics (anti-TNF: infliximab; anti-integrins: vedolizumab).
- UC-Specific: Janus kinase inhibitors (tofacitinib).
Surgery
- Crohn’s: Resection of diseased segments (recurs in 50% at anastomosis).
- UC: Curative total proctocolectomy with ileal pouch-anal anastomosis (IPAA); 30% pouchitis risk.
Lifestyle/Diet
- Anti-inflammatory diet (Mediterranean); avoid triggers.
- Smoking cessation critical for Crohn’s.
- Probiotics, nutritional therapy (exclusive enteral nutrition in pediatric Crohn’s).
Multidisciplinary care: gastroenterologists, surgeons, dietitians.
Complications and Long-Term Risks
| Complication | Crohn’s Disease | Ulcerative Colitis |
|---|---|---|
| Strictures/Obstruction | Common (50% lifetime) | Rare |
| Fistulas/Abscesses | 30-50% | Rare |
| Colorectal Cancer | Lower risk | High with pancolitis (>8-10 years) |
| Toxic Megacolon | Rare | Acute emergency (5% severe UC) |
Regular surveillance colonoscopies advised.
Living with IBD: Prognosis and Management
With modern biologics, 50-70% achieve remission; surgery rates declining. Quality of life improves with adherence. Mental health support vital (anxiety/depression common). Track flares via apps; join support groups like Crohn’s & Colitis Foundation.
Frequently Asked Questions (FAQs)
Can you have both Crohn’s disease and ulcerative colitis?
No, they are mutually exclusive diagnoses. However, Crohn’s colitis mimics UC, and re-diagnosis occurs in 5-10%.
Which is worse: Crohn’s or ulcerative colitis?
Neither is inherently “worse”; Crohn’s has more complications outside colon, UC offers surgical cure but cancer risk.
Do Crohn’s and UC cause colon cancer?
Yes, both increase risk (UC higher); annual screening after 8-10 years.
Is IBD the same as IBS?
No, IBS lacks inflammation/damage; normal tests vs. IBD’s visible changes.
Can diet cure IBD?
No, but specific diets (e.g., low-FODMAP, SCD) manage symptoms.
References
- The Difference Between Ulcerative Colitis and Crohn’s Disease — ACE Clinic. Accessed 2026. https://aceclinic.org/the-difference-between-ulcerative-colitis-and-crohns-disease/
- Crohn’s Disease vs. Ulcerative Colitis — Temple Health. Accessed 2026. https://www.templehealth.org/services/conditions/crohns-disease-versus-ulcerative-colitis
- Ulcerative Colitis vs Crohn’s Disease — UCLA Health. Accessed 2026. https://www.uclahealth.org/medical-services/gastro/ibd/patient-resources/ulcerative-colitis-vs-crohns-disease
- Early signs of Crohn’s & Ulcerative Colitis — Crohn’s & Colitis Foundation. Accessed 2026. https://www.crohnscolitisfoundation.org/blog/ulcerative-colitis-vs-crohns-disease-what-are-the-early-signs-and-how-are-they-diagnosed
- Crohn’s Disease vs. Ulcerative Colitis: Key Differences — Newtown GI. Accessed 2026. https://www.newtowngi.com/blog/crohn-s-disease-vs-ulcerative-colitis-key-differences
- Crohn’s and Ulcerative Colitis: What’s Different — Dartmouth Health (YouTube). 2025-08-27. https://www.youtube.com/watch?v=e7sipfdmOXU
- Ulcerative colitis vs. Crohn’s disease — Mayo Clinic. Accessed 2026. https://www.mayoclinic.org/diseases-conditions/inflammatory-bowel-disease/in-depth/ulcerative-colitis-vs-crohns-disease/art-20590269
Read full bio of Sneha Tete











