Cystoscopy: Purpose, Procedure, and What to Expect
Complete guide to cystoscopy: Learn about this minimally invasive bladder examination procedure.
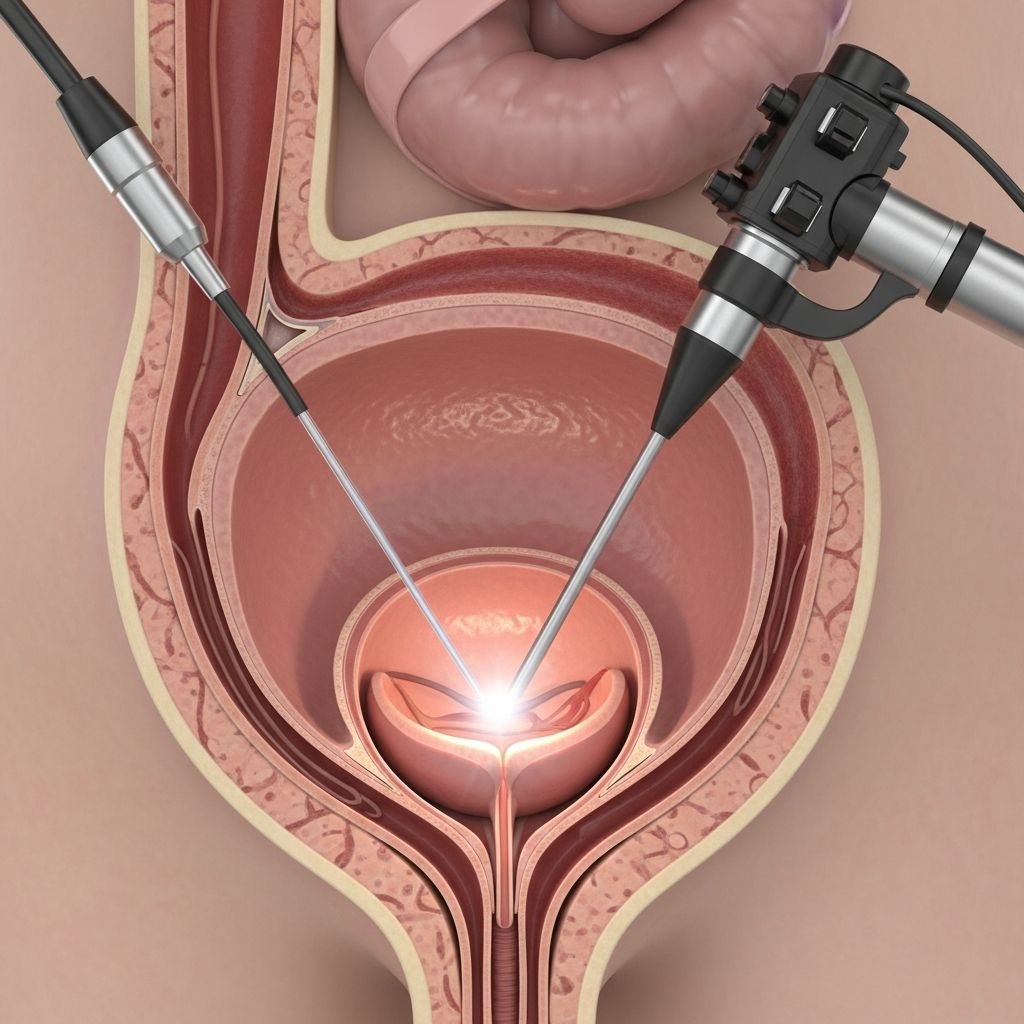
What Is a Cystoscopy?
A cystoscopy is a minimally invasive diagnostic procedure that allows your healthcare provider to examine the inside of your bladder and urethra using a specialized instrument called a cystoscope. This hollow tube, typically measuring about the diameter of a pencil, is equipped with a lens or camera that transmits real-time images to a monitor, enabling your physician to directly visualize the internal structures of your urinary tract. The procedure is commonly performed to diagnose various bladder and urethral conditions, investigate symptoms, and sometimes remove small abnormalities or collect tissue samples for laboratory analysis.
Cystoscopy has become a standard diagnostic tool in urology and gynecology, valued for its ability to provide direct visualization of bladder pathology without requiring invasive surgery. The procedure is typically quick, often lasting between 10 to 20 minutes, and can be performed in an outpatient setting with minimal discomfort.
Why Your Doctor May Recommend Cystoscopy
Your healthcare provider may recommend a cystoscopy for various clinical reasons. These indications include investigating symptoms related to the urinary tract, diagnosing conditions affecting the bladder and urethra, and evaluating structural abnormalities. Common reasons for ordering this procedure include:
- Chronic urinary tract infections
- Blood in the urine (hematuria)
- Bladder pain or pelvic pain
- Difficulty urinating or urinary retention
- Suspected bladder stones
- Suspected bladder cancer or other malignancies
- Urinary incontinence evaluation
- Assessment of ureteral strictures or abnormalities
- Evaluation of the bladder after trauma or injury
Types of Cystoscopes
Two main types of cystoscopes are available, each with distinct characteristics and clinical applications. The choice between them depends on the specific purpose of the examination and the procedures that may need to be performed.
Rigid Cystoscope
The rigid cystoscope is a straight, non-flexible instrument that provides excellent visualization and stability during the procedure. This type is particularly useful when your healthcare provider needs to perform therapeutic interventions or collect tissue samples. The rigid design allows for the insertion of small surgical instruments through the cystoscope to remove bladder stones, take biopsies, cauterize bleeding vessels, or remove small growths. Procedures using rigid cystoscopes are typically performed under sedation or general anesthesia due to the potential for increased discomfort.
Flexible Cystoscope
The flexible cystoscope features a bendable design that can navigate the curves of the urinary tract more easily. This type is primarily used for diagnostic purposes, allowing your doctor to visualize the bladder and urethra without performing therapeutic interventions. The flexibility of this instrument often results in less discomfort and may allow the procedure to be performed under local anesthesia with minimal sedation. Flexible cystoscopes are often preferred for diagnostic-only procedures and can be used in office-based settings.
How to Prepare for Your Cystoscopy
Proper preparation is essential for ensuring a successful cystoscopy procedure. Your healthcare provider will give you specific instructions tailored to your individual circumstances, but general preparation guidelines typically include the following:
Pre-Procedure Instructions
- Arrange transportation, as you may receive sedation or anesthesia and should not drive afterward
- Inform your healthcare provider about all medications and supplements you take, as some may need to be adjusted
- Disclose any allergies, particularly to medications or latex
- Notify your provider if you have active urinary tract infections or other acute conditions
- Follow fasting instructions if general anesthesia will be used (typically nothing to eat or drink for 6-8 hours before the procedure)
- Wear comfortable, loose-fitting clothing that is easy to remove
- Plan to have someone accompany you to drive you home after the procedure
Day of Procedure
On the day of your cystoscopy, you should empty your bladder completely before the procedure begins. You will then remove all clothing from the waist down and change into a hospital gown. Remove any jewelry or metal objects that could interfere with the procedure. Your healthcare team will review all pre-procedure paperwork and confirm that you have followed all preparation instructions.
What to Expect During the Procedure
Understanding what happens during your cystoscopy can help reduce anxiety and prepare you mentally for the experience. The procedure follows a standardized sequence of steps.
Positioning and Initial Steps
You will be asked to lie on your back on a procedure table, with your knees raised and separated. Your feet may be placed in stirrups, similar to a gynecological examination position. The exact positioning may vary slightly depending on whether a rigid or flexible cystoscope will be used. For flexible cystoscopy procedures, positioning is often more flexible and comfortable. Your vital signs, including heart rate, blood pressure, and oxygen saturation, will be continuously monitored throughout the procedure.
Anesthesia and Numbing
Depending on the type of procedure being performed and your healthcare provider’s preferences, you may receive local, regional, or general anesthesia. Local anesthesia typically involves applying a numbing jelly (lidocaine) directly to your urethra, which helps prevent discomfort as the cystoscope is inserted. If sedation is used, you will receive intravenous medication that makes you feel relaxed and drowsy while remaining aware of your surroundings. General anesthesia puts you completely to sleep for the duration of the procedure. Your anesthesia provider will explain your options and help determine which approach is best for your situation.
Cystoscope Insertion and Examination
After the numbing medication takes effect, your healthcare provider will gently insert the cystoscope through your urethra and advance it into your bladder. The cystoscope is typically the smallest size possible that will allow adequate visualization. The lens on the end of the cystoscope magnifies the internal structures, making them appear larger and easier to examine. Your provider will carefully inspect the entire lining of your urethra and bladder, looking for any abnormalities such as inflammation, bleeding, polyps, tumors, stones, or structural abnormalities.
Bladder Filling
To allow for complete visualization of the bladder wall, your provider may fill your bladder with sterile saline solution or sterile water through the cystoscope. As your bladder fills, you may experience the sensation of needing to urinate, which is completely normal. This distension allows your provider to examine the entire bladder surface and identify any areas of concern that might not be visible in an empty bladder.
Tissue Sampling or Treatment
If your provider identifies an area of concern, such as an abnormal-looking tissue or a suspected polyp, they may take a small tissue sample (biopsy) using instruments passed through the cystoscope. This tissue sample is sent to the laboratory for microscopic examination to determine if cancer or other abnormal conditions are present. Additionally, if bladder stones are present, your provider may remove them during the procedure using specialized instruments.
Procedure Completion
Once the examination is complete and any necessary interventions have been performed, your provider will carefully remove the cystoscope from your urethra. Your bladder will drain of any remaining fluid, and you will be moved to a recovery area where you can begin to wake up if sedation was used.
Risks and Complications
While cystoscopy is generally a safe procedure with a low complication rate, as with any medical intervention, certain risks exist. These complications are typically minor and self-limited. Understanding these potential risks allows you to recognize warning signs and seek appropriate care if needed.
- Urinary tract infection: Bacterial infection can occur after cystoscopy, which is why prophylactic antibiotics are sometimes prescribed
- Burning with urination: Temporary discomfort and burning sensation during urination is common and usually resolves within 24-48 hours
- Urinary frequency: Increased urge to urinate frequently after the procedure, typically temporary
- Hematuria: Mild blood in the urine is common and usually clears within 24 hours
- Urethral perforation: Rare perforation of the urethra or bladder wall
- Bladder perforation: Uncommon but potentially serious complication requiring hospitalization
- Sepsis: Rare but serious systemic infection
- Allergic reaction: Uncommon reaction to anesthetic agents
Recovery and Post-Procedure Care
Recovery from cystoscopy is typically quick, with most patients able to resume normal activities within a day or two. However, following proper post-procedure care guidelines is important to minimize discomfort and reduce the risk of infection.
Immediate Recovery
After the procedure, you will be moved to a recovery area where you will remain under observation until the effects of any sedation or anesthesia wear off. Your vital signs will continue to be monitored. Nurses will provide you with an information sheet outlining home-care instructions. If you received general anesthesia, you may feel drowsy for several hours, and you should not drive or operate machinery for at least 24 hours after the procedure.
Home Care Instructions
- Increase fluid intake: Drink plenty of water and other fluids to help flush your urinary system and reduce infection risk
- Pain management: Over-the-counter pain relievers such as ibuprofen or acetaminophen can help manage mild discomfort
- Antibiotic therapy: Take any prescribed antibiotics exactly as directed to prevent bladder infection
- Rest: Avoid strenuous activities and heavy lifting for several days after the procedure
- Limited sexual activity: Avoid sexual intercourse for at least 1-2 weeks after the procedure
- Normal diet: You can resume your normal diet immediately after the procedure
- Avoid irritants: Limit caffeine and alcohol, which can irritate the bladder
Expected Symptoms After Cystoscopy
Mild side effects are common after cystoscopy and typically resolve within a few days. You may experience burning or discomfort with urination, increased urinary frequency, mild blood-tinged urine, and mild pelvic discomfort. These symptoms usually subside within 24-48 hours as your urethra heals. However, you should contact your healthcare provider if you experience severe pain, fever, chills, inability to urinate, persistent heavy bleeding in your urine, or signs of infection such as warmth or redness at the procedure site.
When to Contact Your Healthcare Provider
While most cystoscopy procedures are uncomplicated, certain symptoms warrant immediate medical attention. You should contact your healthcare provider or seek emergency care if you experience:
- Severe pain that is not relieved by over-the-counter pain medication
- Fever above 101°F (38.3°C) or chills
- Inability to urinate 8 hours after the procedure
- Heavy bleeding in your urine that persists beyond a few hours
- Signs of infection such as increased warmth, redness, or drainage from the urethra
- Severe lower abdominal pain or bloating
- Nausea or vomiting that does not improve
Frequently Asked Questions
Q: How long does a cystoscopy procedure take?
A: A typical cystoscopy procedure takes approximately 10 to 20 minutes, depending on the complexity of the examination and whether any therapeutic interventions are performed during the procedure.
Q: Will I experience pain during a cystoscopy?
A: Most patients experience minimal discomfort during cystoscopy because the urethra is numbed with local anesthetic before the procedure. Some patients report a sensation of pressure or mild discomfort, particularly when the bladder is being filled, but severe pain should not occur. If you do experience significant pain, inform your healthcare provider immediately.
Q: Can I drive home after my cystoscopy?
A: If you received only local anesthesia, you may be able to drive home. However, if you received sedation or general anesthesia, you will not be able to drive for at least 24 hours after the procedure and must arrange for someone else to drive you home.
Q: What should I expect after the procedure?
A: Mild burning with urination, increased urinary frequency, and mild blood-tinged urine are common after cystoscopy and typically resolve within 24-48 hours. You can resume most normal activities the next day, but should avoid strenuous exercise and heavy lifting for several days.
Q: Is cystoscopy safe?
A: Yes, cystoscopy is a safe procedure with a low complication rate. Serious complications are rare, and most patients experience only minor, temporary side effects that resolve without intervention.
Q: What is the difference between rigid and flexible cystoscopes?
A: Rigid cystoscopes are straight and allow for therapeutic interventions such as biopsy or stone removal. Flexible cystoscopes are bendable and are primarily used for diagnostic purposes. Flexible cystoscopy is often more comfortable and may be performed in an office setting.
Q: How soon will I get my results?
A: Your healthcare provider may discuss preliminary findings immediately after the procedure. However, if tissue samples were taken, laboratory analysis typically takes 3-7 business days, and your provider will contact you with detailed results.
References
- Cystoscopy or Bladder Scope Test — WebMD. 2024. https://www.webmd.com/prostate-cancer/cystoscopy
- About Your Cystoscopy — Cleveland Clinic Florida. https://my.clevelandclinic.org/health/diagnostics/16553-cystoscopy
- Cystoscopy for Kidney Transplant Recipients — Cleveland Clinic Abu Dhabi. 2024. https://www.clevelandclinicabudhabi.ae/en/health-hub/health-resource/treatments-and-procedures/cystoscopy-for-kidney-transplant-recipients
- Cystoscopy — Mayo Clinic. 2024. https://www.mayoclinic.org/tests-procedures/cystoscopy/about/pac-20393694
- Cystoscopy in Cleveland, Ohio — Cleveland Urology. https://clevelandurology.net/services/cystoscopy/
Read full bio of medha deb













