DCIS Breast Cancer Stage 0: Essential Facts To Know
Understand DCIS, the earliest form of breast cancer: symptoms, diagnosis, treatments, and why it's often called stage 0 breast cancer.
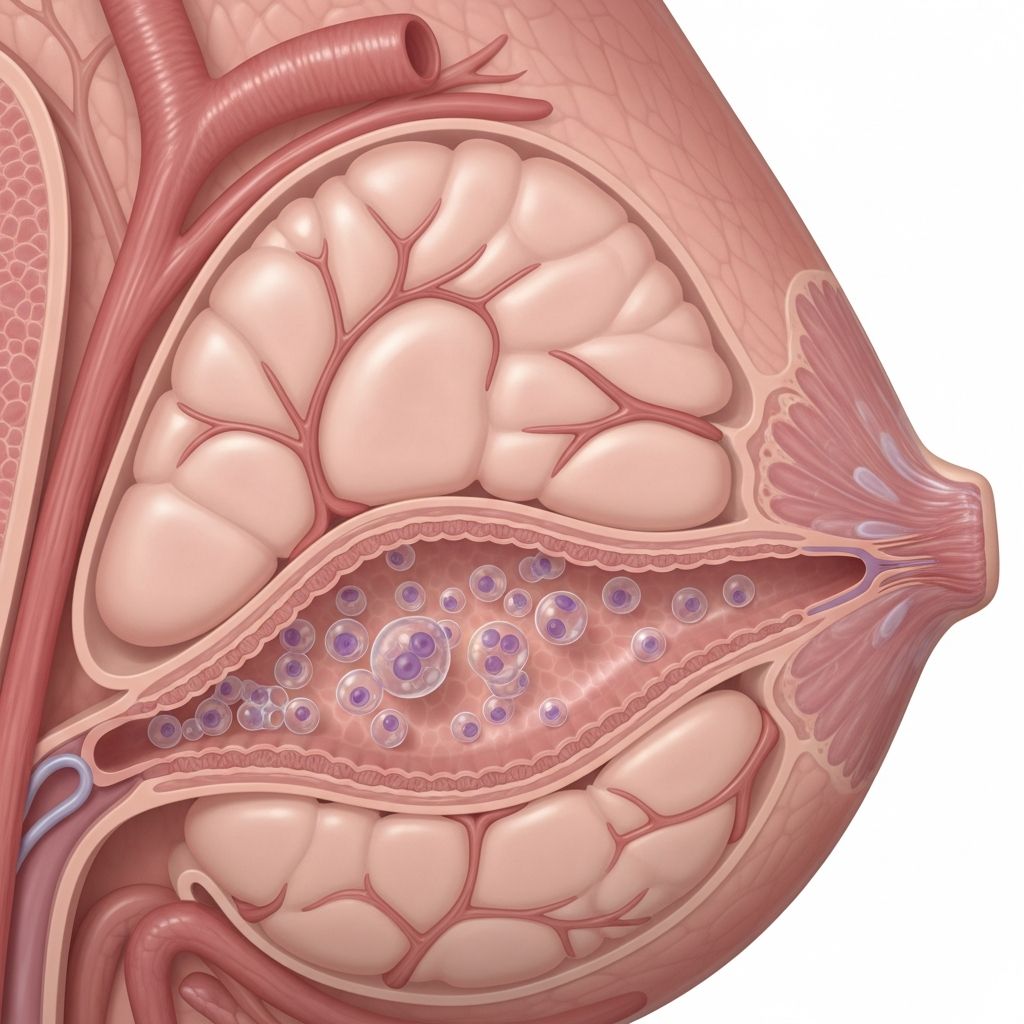
DCIS Breast Cancer: Stage 0 Explained
Ductal carcinoma in situ (DCIS) represents the earliest detectable form of breast cancer, confined to the milk ducts without invading surrounding tissue. Often termed
stage 0 breast cancer
, DCIS has a near-perfect prognosis with 98% 10-year survival, yet treatment remains standard to prevent potential progression to invasive cancer.What Is DCIS?
**Ductal carcinoma in situ (DCIS)** is a non-invasive breast condition where abnormal cells multiply within the lining of the breast’s milk ducts but do not break through to invade nearby tissue. This containment classifies it as ‘in situ,’ meaning ‘in place,’ distinguishing it from invasive breast cancers that spread beyond the ducts.
DCIS accounts for 20-25% of breast cancer diagnoses detected through screening programs. While the cells are cancerous, DCIS is not immediately life-threatening. However, if untreated, 20-50% of cases may progress to invasive breast cancer over time, though predicting which ones remains challenging.
Key characteristics include:
- Localized to ducts: No spread to lobules, fat, or lymph nodes.
- Molecular subtypes: Similar to invasive cancers but triple-negative and basal-like subtypes are rare in DCIS.
- Detection: Often asymptomatic, found via mammograms as microcalcifications.
Symptoms of DCIS
DCIS is typically
asymptomatic
, discovered incidentally during routine screening mammography. When symptoms occur, they mimic other breast conditions:- A new lump or thickening in the breast or underarm.
- Changes in breast size, shape, or skin texture (e.g., dimpling, redness).
- Nipple discharge, often bloody or clear.
- Inversion or retraction of the nipple.
These signs warrant immediate medical evaluation, though palpable lumps are rare in pure DCIS and may indicate mixed invasive components.
Causes and Risk Factors
The exact causes of DCIS are not fully understood but involve genetic mutations in duct-lining cells, triggered by:
- Age: Most common in women over 50.
- Family history: BRCA1/BRCA2 mutations increase risk.
- Hormonal factors: Early menstruation, late menopause, hormone replacement therapy (HRT), or no pregnancies.
- Lifestyle: Obesity, alcohol use, physical inactivity.
Autopsy studies reveal 1-14% prevalence of undetected DCIS in women, suggesting many cases never progress. High-grade DCIS shows a slight progression tendency, but grade alone is unreliable.
Diagnosis of DCIS
Diagnosis begins with
mammography
, where DCIS appears as clusters of microcalcifications. Additional steps include:- Diagnostic mammogram and ultrasound: To assess extent.
- Biopsy: Core needle or stereotactic biopsy confirms DCIS grade (low, intermediate, high) and markers like estrogen receptor (ER), progesterone receptor (PR), HER2.
- MRI: For multifocal or high-risk cases to map extent.
Pathology reports detail nuclear grade, necrosis, architectural pattern (solid, cribriform, etc.), aiding treatment planning. Grading inconsistencies highlight the need for biomarkers.
DCIS Treatment Options
Treatment aims to excise DCIS and reduce recurrence risk, with 98% 10-year survival regardless of some approaches. Options depend on size, grade, extent, and patient factors.
Surgery
Breast-conserving surgery (BCS/lumpectomy): Removes DCIS and a margin of healthy tissue. Ideal for small, localized lesions. Recurrence risk: 7.2% without radiation, 4.1% with.
Mastectomy: Removes entire breast for widespread/multifocal DCIS or genetic risks. Recurrence: <1%. No further therapy often needed.
Radiation Therapy
Post-BCS, radiation halves local recurrence risk across all subgroups (age, grade, presentation). Typically 5-6 weeks of external beam radiation; partial breast irradiation for low-risk cases.
Hormone (Endocrine) Therapy
For ER-positive DCIS (common), tamoxifen or aromatase inhibitors (5 years) reduce recurrence by 30-50%, especially contralateral breast risk.
| Treatment | Indications | Recurrence Risk Reduction | Side Effects |
|---|---|---|---|
| Lumpectomy + Radiation | Localized DCIS | 50% vs. surgery alone | Fatigue, skin changes |
| Mastectomy | Multifocal/extensive | <1% | Loss of breast, reconstruction options |
| + Hormone Therapy | ER+ | 30-50% | Hot flashes, bone density loss |
Is DCIS Cancer? To Treat or Not?
DCIS is ‘pre-invasive cancer’ due to malignant duct cells, but indolent behavior questions aggressive treatment. 50-80% never invade; overtreatment concerns rise as mortality hasn’t dropped with increased detection.
Low-risk DCIS may match survival without surgery per SEER data. Dilemma: Benefits (recurrence prevention) vs. costs (physical/emotional toll). Active surveillance trials test monitoring low-risk cases.
Prognosis and Follow-Up
**Prognosis is excellent**: 98% 10-year survival; normal life expectancy. Post-treatment monitoring: Mammograms every 6-12 months for 5 years, then annually. Self-exams monthly.
Recurrence risks: Ipsilateral in situ (14%), invasive (5-10%). Contralateral breast cancer risk elevated.
Ongoing Research and Future Directions
BCRF and others investigate:
- Biomarkers for progression risk (low vs. high).
- Trials: Surveillance vs. treatment for low-risk DCIS.
- Immune landscape: Duct-lining cells blocking immune surveillance.
- Lesion age to predict aggressiveness.
- HER2: More common in DCIS (34%) vs. invasive (13%), potential recurrence marker.
Goals: Personalize care, avoid overtreatment, understand origins.
Frequently Asked Questions (FAQs)
What is the survival rate for DCIS?
98% at 10 years, nearly 100% with treatment.
Can DCIS spread?
No, pure DCIS does not metastasize; risk is local invasion if untreated.
Is radiation always needed after lumpectomy?
Not for all; low-risk may omit, but standard reduces recurrence 50%.
How often does DCIS become invasive?
20-50%; unpredictable currently.
Can DCIS be cured?
Yes, treatment cures nearly all cases.
References
- Ductal Carcinoma In Situ (DCIS) — Breast Cancer Research Foundation. 2023. https://www.bcrf.org/about-breast-cancer/dcis-ductal-carcinoma-in-situ/
- Ductal carcinoma in situ: to treat or not to treat, that is the question — PMC/NCBI (Peer-reviewed). 2019-08-15. https://pmc.ncbi.nlm.nih.gov/articles/PMC6697179/
- Your Breast Pathology Report: Ductal Carcinoma In Situ (DCIS) — American Cancer Society. 2024. https://www.cancer.org/cancer/diagnosis-staging/tests/biopsy-and-cytology-tests/understanding-your-pathology-report/breast-pathology/ductal-carcinoma-in-situ.html
Read full bio of medha deb











