Deep Vein Thrombosis: Causes, Symptoms, and Treatment
Complete guide to understanding DVT: symptoms, risk factors, diagnosis, and effective treatment options.
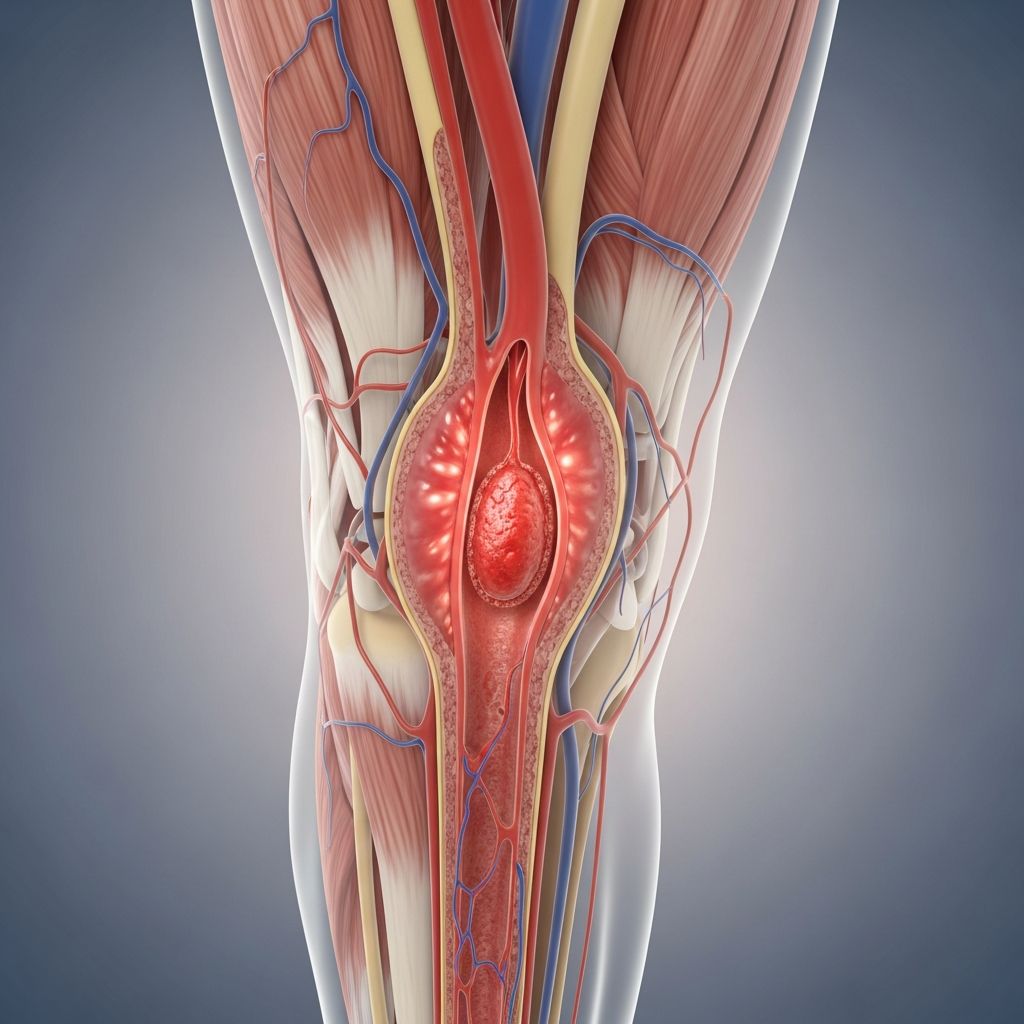
What Is Deep Vein Thrombosis?
Deep vein thrombosis (DVT) is a serious medical condition in which a blood clot forms in a deep vein, usually in the legs or arms. The condition occurs when blood flow slows or becomes damaged, allowing platelets and fibrin to accumulate and form a clot within the vessel. DVT is a common condition that requires prompt diagnosis and treatment to prevent life-threatening complications such as pulmonary embolism, where the clot breaks free and travels to the lungs.
The deep veins are the large blood vessels that run through the center of your limbs, beneath the muscles. When a clot develops in these veins, it can block blood flow and cause significant discomfort. Some people experience mild symptoms or may not notice any signs at all, which makes awareness of risk factors and regular health monitoring essential.
Symptoms of Deep Vein Thrombosis
DVT symptoms vary depending on the location and size of the clot. Many people experience recognizable warning signs, while others may have no symptoms until the condition becomes serious.
Common symptoms of DVT include:
- Leg pain or tenderness in the affected area
- Swelling in the leg, ankle, or foot (edema)
- Red or darker-colored skin over the affected vein
- Skin that feels warm to the touch
- Prominent superficial veins visible under the skin
- Discoloration or cyanosis (bluish tint) of the skin
It is important to note that some people may not experience any symptoms initially. However, if a blood clot dislodges and travels to the lungs, it can cause a pulmonary embolism (PE), a medical emergency. Symptoms of PE include chest pain, shortness of breath, cough with blood, lightheadedness, and fainting. If you experience any of these symptoms, seek emergency medical care immediately.
Risk Factors for Developing DVT
Understanding your risk factors is crucial for prevention and early detection. Several conditions and lifestyle factors increase the likelihood of developing blood clots.
Common risk factors include:
- Prolonged immobility, such as bed rest, long flights, or extended sitting
- Recent surgery or fractures, particularly of the hips, pelvis, or legs
- Family history of blood clots or inherited clotting disorders
- Obesity or being overweight
- Use of oral contraceptives or hormone replacement therapy
- Cancer and certain cancer treatments
- Heart failure
- Smoking, which affects blood flow and clotting
- Pregnancy or childbirth within the past six months
- Long-term indwelling catheters (tubes placed in blood vessels)
- Polycythemia vera, a condition causing excess blood cell production
Slow blood flow in damaged deep veins, particularly after injury, surgery, or hospital stays, is a primary cause of DVT formation. Inflammation in blood vessels and prolonged inactivity contribute to clot development. Understanding these risk factors helps individuals take preventive measures and recognize when medical attention is necessary.
How Is DVT Diagnosed?
Accurate diagnosis is essential for initiating appropriate treatment. Your healthcare provider will conduct a comprehensive evaluation including physical examination and medical history review, followed by specialized testing.
Diagnostic methods include:
- Physical examination to assess swelling, pain, and skin changes
- Duplex ultrasound, the most common imaging test to visualize blood clots
- CT or MRI scanning for detailed imaging in complex cases
- Blood tests to measure clotting factors and identify clotting disorders
- Antithrombin III level testing to determine if you have adequate antithrombin, which prevents excess clotting
- Genetic testing to identify mutations that increase clotting risk, such as the prothrombin G20210A mutation or Factor V Leiden mutation
- Assessment of lupus-related problems, including antiphospholipid antibodies or lupus anticoagulant
- Measurement of protein C and protein S levels, which help regulate clotting
Early diagnosis prevents complications and allows your healthcare team to develop an appropriate treatment plan tailored to your specific condition and medical history.
Treatment Options for DVT
The primary goal of DVT treatment is to prevent the clot from growing larger, stop it from breaking loose and traveling to the lungs, and reduce the risk of developing additional blood clots. Treatment typically involves a combination of medications and supportive measures.
Anticoagulant Medications (Blood Thinners)
Anticoagulants are the cornerstone of DVT treatment. These medications work by preventing clots from growing and inhibiting the formation of new clots. Most people take blood-thinning medication for at least three months after a DVT diagnosis.
Types of blood-thinning medications include:
- Heparin: Often administered as an initial injection while awaiting ultrasound confirmation
- Warfarin: An oral anticoagulant requiring regular monitoring through blood tests
- Rivaroxaban: A direct oral anticoagulant offering convenient dosing
- Other direct oral anticoagulants: Including dabigatran and edoxaban, though some may increase gastrointestinal bleeding risk
- Apixaban: Preferred for patients with specific digestive concerns
Your healthcare provider will select the most appropriate blood-thinning medication based on your medical history, current medications, and individual circumstances. Regular blood tests are essential to monitor the effectiveness and safety of these medications.
Compression Therapy
Compression stockings or wraps help reduce swelling and pain by improving blood circulation in affected limbs. These specialized garments apply graduated pressure, highest at the ankle and decreasing toward the knee, promoting blood flow back to the heart.
Leg Elevation and Movement
Elevating your affected leg above heart level at various times throughout the day reduces swelling and improves circulation. Gentle movement and exercise, as approved by your healthcare provider, also help prevent additional clots and maintain overall circulation.
Invasive and Surgical Interventions
In certain cases, particularly with large or threatening clots, more aggressive treatments may be necessary.
Advanced treatment options include:
- Thrombectomy: A minimally invasive procedure where surgeons use small tools to remove large blood clots from veins
- Thrombolytic therapy: Administration of clot-busting medications through catheters to dissolve clots
- Stent placement: Insertion of tiny metal tubes (stents) into veins, particularly in the legs or pelvis, to keep vessels open and maintain blood flow
- Vena cava filter placement: Insertion of a filter in the body’s largest vein to capture blood clots and prevent them from traveling to the lungs. Retrievable filters can be removed once the contraindication to anticoagulation resolves
These procedures are typically reserved for cases where anticoagulation alone is insufficient or contraindicated due to bleeding risk.
Special Considerations
DVT During Pregnancy
Pregnant individuals with DVT require special management. Treatment consists of blood-thinning injections throughout pregnancy and continuing until six weeks after delivery. This approach protects both mother and developing baby while preventing serious complications.
Catheter-Associated Thrombosis
For patients with clots developing around indwelling catheters, treatment typically involves catheter removal or anticoagulation while the catheter remains in place.
Complications of Deep Vein Thrombosis
Without prompt treatment, DVT can lead to serious complications. Understanding these risks emphasizes the importance of seeking immediate medical attention.
Potential complications include:
- Pulmonary embolism (PE): The most dangerous complication, occurring when a clot travels to the lungs
- Postphlebitic syndrome: Long-term damage to veins from the blood clot, reducing blood flow and causing chronic leg pain, swelling, skin discoloration, and sores
- Bleeding complications: Blood thinners increase bleeding risk; excessive bleeding requires immediate emergency care
- Recurrent DVT: Additional blood clots may develop despite treatment
Managing Treatment Side Effects
While blood-thinning medications are essential for DVT treatment, they can cause side effects requiring monitoring. Important considerations include:
- Regular blood tests to monitor medication effectiveness and safety
- Reporting unusual bruising or heavy periods to your healthcare provider
- Seeking emergency care for signs of excessive bleeding, including bright red blood in vomit or stool
- Informing all healthcare providers about anticoagulation therapy before any procedures
- Using caution during activities that may cause injury or bleeding
Frequently Asked Questions
Q: How long does DVT treatment typically last?
A: Most people take blood-thinning medications for at least three months following a DVT diagnosis. However, treatment duration depends on whether the DVT was provoked (caused by surgery or immobility) or unprovoked (without an obvious trigger). Your healthcare provider will determine the appropriate duration based on your specific circumstances.
Q: Can DVT be prevented?
A: Yes, several prevention strategies can reduce DVT risk, including maintaining regular movement during travel, avoiding prolonged immobility, maintaining healthy weight, quitting smoking, and using compression stockings when recommended. Individuals with high risk may benefit from preventive anticoagulation before surgery.
Q: Is DVT life-threatening?
A: DVT itself is serious and requires treatment, but the greatest danger occurs if the clot dislodges and travels to the lungs, causing pulmonary embolism, which can be fatal. Prompt diagnosis and treatment significantly reduce this risk.
Q: Can I exercise with DVT?
A: Gentle movement and approved exercise help prevent additional clots and maintain circulation. However, consult your healthcare provider about appropriate activities, as high-impact exercise may be restricted during initial treatment.
Q: What should I do if I suspect DVT?
A: Seek medical attention immediately or visit the emergency room if you experience symptoms such as leg swelling, pain, redness, or warmth. Do not wait to see if symptoms resolve; prompt evaluation is essential.
References
- Deep Vein Thrombosis (DVT) – Symptoms and Causes — Penn Medicine. 2025. https://www.pennmedicine.org/conditions/deep-vein-thrombosis
- Deep vein thrombosis (DVT) – Symptoms & causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/deep-vein-thrombosis/symptoms-causes/syc-20352557
- Deep Vein Thrombosis (DVT): Symptoms & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/16911-deep-vein-thrombosis-dvt
- DVT (deep vein thrombosis) — National Health Service (NHS). 2024. https://www.nhs.uk/conditions/deep-vein-thrombosis-dvt/
- Deep Venous Thrombosis — StatPearls, National Center for Biotechnology Information (NCBI). 2024. https://www.ncbi.nlm.nih.gov/books/NBK507708/
- Deep vein thrombosis (DVT) – Diagnosis & treatment — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/deep-vein-thrombosis/diagnosis-treatment/drc-20352563
Read full bio of medha deb











