Dermatoscopic-Histologic Correlation in Skin Lesion Diagnosis
Understanding the relationship between dermoscopic patterns and histological findings in pigmented skin lesions.
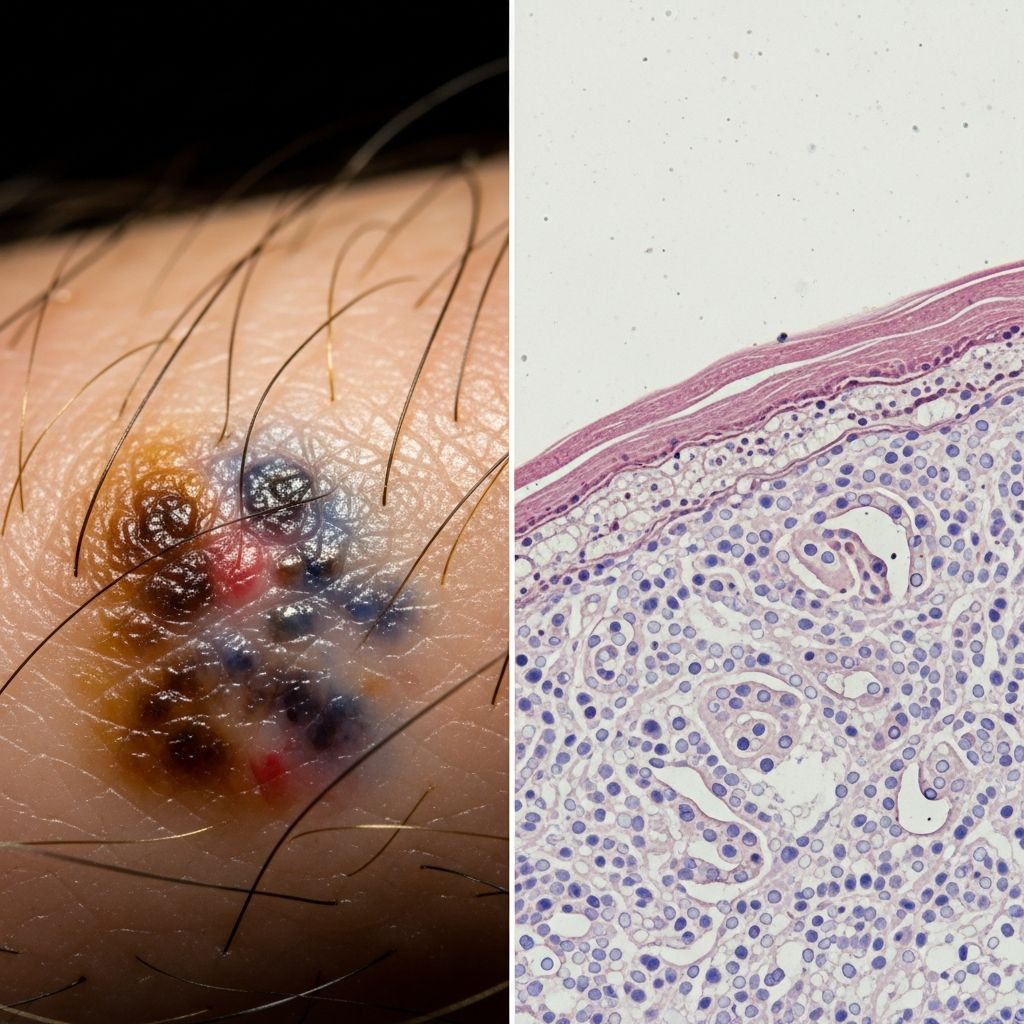
The examination of skin lesions requires a comprehensive understanding of how clinical observations correlate with underlying tissue pathology. Dermatoscopic-histologic correlation represents the fundamental bridge between in vivo dermoscopic examination and histopathological diagnosis, particularly for pigmented lesions. There is a close correlation between the patterns and features observed dermatoscopically and the histological features of biopsied or excised skin lesions, enabling clinicians to predict histopathological findings based on dermoscopic examination.
The Importance of Dermatoscopic-Histologic Correlation
Understanding the relationship between dermoscopic and histopathological findings is essential for both clinicians and pathologists. The two diagnostic modalities provide complementary information when used together in the diagnosis of pigmented skin lesions. Dermoscopy utilizes an immersion technique with optical magnification to visualize structures not visible to the naked eye, while histopathology reveals the microscopic architecture and cellular composition of tissue. When these approaches are integrated, diagnostic accuracy improves significantly.
With experience, clinicians can predict the histopathological features that will be observed based on dermoscopic examination alone. This predictive capability enhances diagnostic confidence and helps guide clinical management decisions. The correlation is particularly robust in melanocytic lesions, where specific dermoscopic patterns consistently correspond to identifiable histological features.
Pattern Analysis and Color Assessment
Dermatoscopic assessment of pigmented lesions using pattern analysis involves careful evaluation of color and pattern, combined with identification of diagnostic clues. Each component of this assessment correlates directly with histopathological findings.
Color Correlation with Pigment Depth
The colors observed dermatoscopically correlate with the nature of the pigment and, in the case of melanin, the depth at which the pigment is located histopathologically. Different colors indicate different locations within the skin:
- Black color typically represents superficial epidermal melanin
- Brown color indicates pigment in the basal epidermis or superficial dermis
- Gray color corresponds to melanin in the papillary dermis
- Blue color represents deeper dermal melanin or melanophages
- White color may indicate dermal fibrosis or epidermal remodeling
Reticular and Branched Line Patterns
Two fundamental dermoscopic patterns observed in pigmented lesions are reticular and branched lines. Reticular lines are straight and intersect at regular intervals at right angles, creating a network appearance. Branched lines are also straight but intersect at irregular intervals and not at right angles.
These dermoscopic patterns correlate with specific histological features. They are observed in lesions showing basal epidermal hyperpigmentation and/or proliferation of pigmented melanocytes that preferentially involve the epidermal rete ridges while preserving the epidermal architecture. The less-pigmented “holes” of the network correspond to the tips of the dermal papillae and the overlying suprapapillary plates of the epidermis. A wide diameter of dermal papillae corresponds dermoscopically to wider network “holes,” whereas narrow dermal papillae result in a denser appearance of the grid pattern.
Structureless Patterns and Their Histologic Correlates
The combination of structureless and reticular patterns may result from marked pigmentation of lesional cells that obscures the pattern of lines, or from loss of the epidermal rete in part of the lesion. These patterns have distinct histopathological origins:
- Heavy melanin pigmentation can obscure underlying architectural patterns, appearing as structureless zones
- Epidermal remodeling in melanoma can eliminate the normal rete ridge pattern
- Past regression of melanocytic proliferations may result in rete loss
- Underlying expansile dermal lesions can disrupt normal epidermal architecture
The color of the structureless zone provides additional diagnostic information. It may be white if due to dermal fibrosis, skin-colored if associated with epidermal remodeling and proliferation of non-pigmented melanocytes, or black, brown, gray, or blue if due to heavy melanin pigmentation at varying depths.
Dots and Their Histopathological Significance
Dots observed during dermoscopic examination represent distinct histopathological entities based on their color and appearance:
| Dot Color | Histopathological Correlate | Clinical Significance |
|---|---|---|
| Black Dots | Pagetoid pigmented melanocytes or free pigment within the stratum corneum | Superficial melanin or atypical distribution |
| Brown Dots | Small nests of melanocytes in basal epidermis, focal pigmented keratinocytic proliferation, or superficial dermal haemosiderin deposition | Benign or reactive changes |
| Gray Dots | Melanin pigment within the papillary dermis, either free, in small nests of melanocytes, or in melanophages | Dermal involvement of melanocytic lesion |
| Blue Dots | Deeper dermal melanin | Significant dermal pigmentation |
Pseudopods and Melanocytic Proliferation
Pseudopods—finger-like projections at the periphery of lesions—have important histological correlates. The distribution pattern of pseudopods provides diagnostic clues:
- Regularly distributed circumferential pseudopods suggest a pigmented spindle cell (Reed) naevus, with histologic correlation showing large nests of pigmented melanocytes at the lesion periphery
- Segmental pseudopods create asymmetry and represent a clue to melanoma, similarly correlating with large nests of pigmented melanocytes at the peripheral margins
Nail Matrix Melanoma and Longitudinal Melanonychia
Examination of the pigmented stripe in nail lesions can reveal hallmark clues of pigmented nail-matrix melanoma. Key dermoscopic features include longitudinal melanonychia with lines that are parallel and chaotic, or lines parallel with varying width, interval, and color. These patterns reflect disruption of the normal nail matrix by atypical melanocytes.
It is essential that nail matrix biopsy be performed competently to obtain adequate tissue for histological diagnosis. The “pop the bonnet” technique is preferred over the fenestration technique, as it allows direct visualization of the entire matrix including dermoscopy of both nail bed and nail plate, facilitating accurate histopathological assessment.
Atypical Pigment Network
The atypical pigment network represents one of the most important dermoscopic findings for identifying potentially malignant lesions. The irregular lines of an atypical network correspond histopathologically to variation in the width, length, and spacing of rete ridges. This variation results from the size, spacing, and tendency to confluence of melanocytic nests. Rete ridges that are elongated and widened by larger junctional nests of melanocytes appear as darker and wider lines on dermoscopy.
The atypical network is frequently observed in melanoma and dysplastic nevi. The irregular appearance reflects the disorganized growth pattern of melanocytes that characterizes these lesions. This finding serves as an important warning sign for potential malignancy and typically warrants histopathological evaluation through biopsy.
Homogenous Blue Pattern and Deep Dermal Pigmentation
The homogenous blue pattern, characterized by the presence of blue color with the absence of other dermoscopic structures throughout the entire lesion, correlates histologically with densely pigmented melanocytes or melanophages in the dermis. This pattern indicates significant dermal involvement with melanin or melanin-containing cells.
The differential diagnosis of homogenous blue pattern is broad and includes blue nevi, combined nevi, areas of extensive regression, pigmented nodular melanoma, primary or metastatic melanoma, basal cell carcinoma, and radiation tattoos. Histopathological examination is often necessary to distinguish among these entities, particularly when homogenous blue pattern is present without other distinguishing features.
Negative Network and Melanoma Detection
The negative network—an absence of pigmentation in a networked pattern—is a highly specific dermoscopic finding for melanoma, with specificity approaching 95%. Histopathologically, the negative network corresponds to thin elongated rete ridges accompanied by large melanocytic nests within a widened papillary dermis, or to bridging of rete ridges. This architectural disorganization is characteristic of melanoma growth and reflects the aggressive behavior of malignant melanocytes.
Granularity and Superficial Dermal Melanin
Granularity observed during dermoscopic examination correlates histologically with melanin in the superficial dermis. This melanin may appear as fine melanin particles in melanophages or as extracellular “dust-like” particles. The distribution and extent of granularity provide important diagnostic information:
- In benign nevi, granularity typically encompasses less than 10% of the lesion’s surface area
- In melanoma, granularity often encompasses more than 50% of the lesion’s surface area
- The extent of granularity correlates with the degree of superficial dermal involvement
Non-Pigmented Lesions and Vascular Patterns
When pigment is not present in a skin lesion, other dermatoscopic features must be utilized for diagnosis. Key features used in non-pigmented lesions include the presence or absence of non-traumatic ulceration, the recently described “white clues,” and vascular patterns.
The pattern of blood vessels can provide diagnostic clues for both pigmented and non-pigmented lesions and is a key component in the assessment of non-pigmented lesions by dermoscopy. However, there is relatively poor correlation between dermatoscopic vascular patterns and the histology of particular lesions. This is of little clinical importance for non-pigmented lesions, as such lesions are obviously visible following staining of tissue sections for histology, precluding the need to assess secondary vascular features for histological prediction.
Pigmented Basal Cell Carcinoma
Pigmented basal cell carcinoma (BCC) presents unique dermoscopic-histologic correlation challenges. While dermoscopy has great value in the diagnosis of pigmented BCC, the precise histopathological correlates of dermoscopic features have not been fully established until recent investigations. Research correlating dermatoscopic features of pigmented BCC with their histopathological counterparts has provided clear histopathological definitions of specific dermoscopic features, enhancing diagnostic accuracy for this clinical variant.
Micropunch Technique for Direct Correlation
A micropunch technique has been developed that allows for the first time a direct correlation between dermoscopic and histopathologic findings with visual control. This technique involves performing a small punch biopsy precisely at the dermoscopically examined site, allowing pathologists to identify the exact location and tissue depth of structures observed dermatoscopically. This advancement has significantly improved the understanding of dermoscopic-histologic correlation and has validated many previously suspected correlations.
Actinic Keratosis: An Exception to Strong Correlation
It is important to note that not all skin lesions demonstrate strong dermoscopic-histologic correlation. The correlation between histological and dermoscopic features of actinic keratosis is relatively poor, with limited predictive value of dermoscopic findings for histopathological appearance in this lesion type. This emphasizes the importance of understanding which lesion types demonstrate reliable correlation and which do not.
Clinical Application and Diagnostic Enhancement
Understanding dermoscopic-histologic correlation enhances clinical practice in several ways. It improves diagnostic accuracy, increases confidence in clinical management decisions, and facilitates communication between clinicians and pathologists. Dermatoscopy improves the accuracy of clinical diagnosis, particularly for identifying atypical melanocytic nevi and distinguishing them from benign lesions.
The integration of dermoscopic and histopathological information allows for more precise diagnosis and better prediction of lesion behavior. This is particularly important in melanoma detection and in the identification of dysplastic nevi that may carry increased melanoma risk.
Frequently Asked Questions
Q: How does dermoscopy help predict histopathological findings?
A: Dermoscopy visualizes the microscopic architecture and pigment distribution in skin lesions. Specific dermoscopic patterns correlate with identifiable histopathological features. For example, reticular patterns correlate with hyperpigmentation of basal epidermis and rete ridge involvement, while blue color indicates deeper dermal melanin. With experience, clinicians can predict histological findings based on these correlations.
Q: What does an atypical pigment network indicate histologically?
A: An atypical pigment network corresponds histologically to irregular variation in rete ridge width, length, and spacing caused by variation in the size and spacing of melanocytic nests. This finding is often seen in melanoma and dysplastic nevi and warrants biopsy evaluation.
Q: Why is nail matrix biopsy technique important for dermoscopic-histologic correlation?
A: Proper nail matrix biopsy technique ensures adequate tissue collection for accurate histopathological diagnosis. The “pop the bonnet” technique allows direct visualization of the entire nail matrix including both nail bed and plate, enabling precise correlation with dermoscopic findings of longitudinal melanonychia.
Q: Which skin lesions have poor dermoscopic-histologic correlation?
A: Actinic keratosis demonstrates relatively poor correlation between dermoscopic and histopathological features. In contrast, pigmented melanocytic lesions generally show strong and reliable correlation between the two modalities.
Q: How does the extent of granularity help distinguish benign nevi from melanoma?
A: Granularity correlates with melanin in the superficial dermis within melanophages. In benign nevi, granularity typically involves less than 10% of the lesion’s surface, while in melanoma it often encompasses more than 50% of the surface area, reflecting greater dermal involvement.
References
- Dermatoscopic-histologic correlation — DermNet NZ. 2024. https://dermnetnz.org/cme/dermoscopy-course/dermatoscopic-histologic-correlation
- Histopathologic Correlation in Dermoscopy: A Micropunch Technique — JAMA Dermatology. https://jamanetwork.com/journals/jamadermatology/fullarticle/479224
- Histopathological correlation (full text) — Dermoscopedia. https://dermoscopedia.org/Histopathoilogical_correlation_(full_text)
- Correlation between the dermatoscopic and histopathological features of pigmented BCC — PubMed NCBI. https://pubmed.ncbi.nlm.nih.gov/20337825/
- Correlation Between Clinical, Dermatoscopic, and Histopathologic findings of melanocytic nevi — Actas Dermosifiliográficas. http://www.actasdermo.org/en-correlation-between-clinical-dermatoscopic-histopathologic-articulo-S1578219008702713
Read full bio of medha deb










