Diabetic Foot Ulcer: Complete Prevention And Treatment Guide
Comprehensive guide on causes, symptoms, diagnosis, management, and prevention of diabetic foot ulcers to avoid complications like amputation.
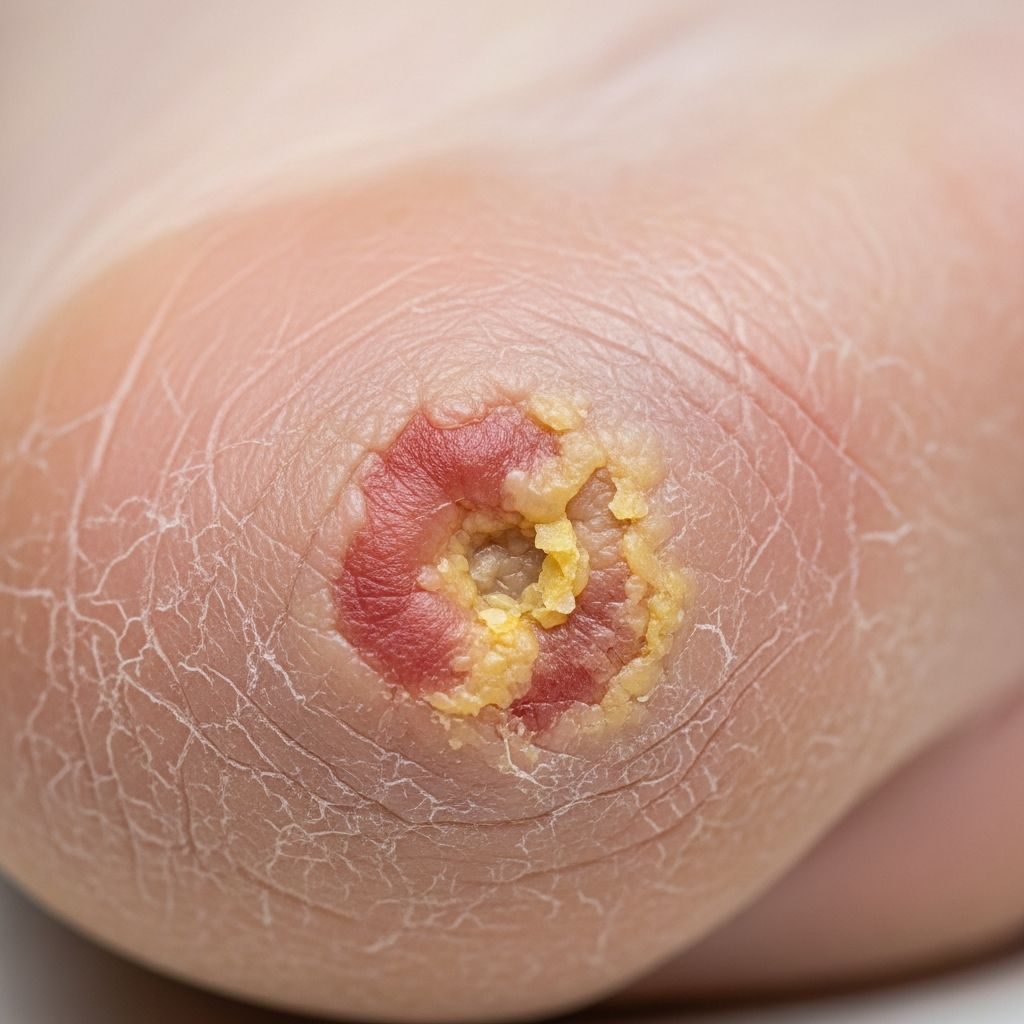
Diabetic foot ulcers are open sores or wounds that develop on the feet of individuals with diabetes, primarily due to peripheral neuropathy, poor circulation, and repetitive trauma. These ulcers affect approximately 15% of diabetic patients and represent a leading cause of non-traumatic lower extremity amputations[10]. Effective management requires multidisciplinary care focusing on glycemic control, wound debridement, infection control, and pressure offloading.
What is a diabetic foot ulcer?
A diabetic foot ulcer (DFU) is a breakdown in the skin of the foot in a person with diabetes, often starting as a small cut or blister that fails to heal due to underlying complications like nerve damage and vascular insufficiency. These ulcers commonly occur on the plantar surface (bottom) of the foot, particularly over pressure points such as the metatarsal heads or heels. Unlike typical wounds, DFUs progress slowly because diabetes impairs the body’s natural healing processes, including reduced blood flow, diminished sensation, and weakened immune response. If untreated, they can lead to deep infections, osteomyelitis (bone infection), gangrene, and ultimately amputation. Early recognition and intervention are critical, as healing can take weeks to months, and recurrence rates exceed 40% within a year.
Who gets diabetic foot ulcers?
Diabetic foot ulcers primarily affect individuals with long-standing diabetes, particularly those with poor glycemic control. Key risk factors include:
- Duration of diabetes: Patients with diabetes for over 10 years are at highest risk due to cumulative nerve and vascular damage.
- Peripheral neuropathy: Present in up to 50% of diabetics, it causes loss of protective sensation, allowing unnoticed injuries to develop into ulcers.
- Peripheral artery disease (PAD): Reduces blood flow to the feet, impairing healing; affects 20-50% of DFU patients.
- Foot deformities: Such as claw toes, hammertoes, or high arches from motor neuropathy, leading to abnormal pressure distribution.
- Trauma or repetitive pressure: Ill-fitting shoes, calluses, or minor injuries exacerbate risk.
- Other factors: Smoking, obesity, alcohol use, edema, and uncontrolled hyperglycemia increase susceptibility by promoting inflammation and poor circulation.
Globally, DFUs lead to over 1 million amputations annually, with higher incidence in males and those over 60 years old.
What causes diabetic foot ulcers?
DFUs result from a multifactorial interplay of neuropathy, ischemia, biomechanical abnormalities, and trauma. Neuropathy is the primary driver: sensory loss prevents pain detection, motor changes cause deformities, and autonomic dysfunction leads to dry, fissured skin. Ischemic ulcers stem from PAD, where arterial plaque narrows vessels, starving tissues of oxygen and nutrients. Repetitive microtrauma from high plantar pressures over bony prominences, combined with callus formation, erodes the skin. Hyperglycemia further delays healing via chronic inflammation, impaired angiogenesis, and matrix metalloproteinase excess. Infections often complicate existing ulcers due to impaired immunity.
What are the clinical features of diabetic foot ulcer?
DFUs present variably due to neuropathy masking symptoms. Common features include:
- Appearance: Open sores, often painless, with punched-out edges, surrounding callus, or fibrinous slough; neuropathic ulcers are typically on the forefoot, ischemic on toes/heels.
- Pain: Minimal or absent in neuropathic cases; severe in ischemic ulcers, worsened by weight-bearing.
- Swelling and erythema: Indicates edema or early infection; purulent discharge or foul odor suggests deeper involvement.
- Associated signs: Dry skin, fissures, deformities, hair loss, or cool skin in PAD.
Advanced cases may show cellulitis, abscesses, or gangrene. Classification systems like Wagner or University of Texas grade depth, infection, and ischemia for prognosis.
How is it diagnosed?
Diagnosis combines clinical assessment, history, and investigations:
- History and exam: Assess neuropathy (monofilament testing, vibration sense), vascular status (pulses, ankle-brachial index), and ulcer characteristics.
- Imaging: X-rays for osteomyelitis, MRI for soft tissue/bone infection, Doppler ultrasound for PAD.
- Labs: Wound swabs/cultures, HbA1c for glycemic control, inflammatory markers (CRP, ESR).
- Biopsy: Rarely, to rule out malignancy or confirm osteomyelitis.
Multidisciplinary input from podiatry, vascular surgery, and endocrinology optimizes diagnosis.
What is the treatment of a diabetic foot ulcer?
Treatment follows a structured approach: relieve pressure, restore perfusion, control infection, and promote healing.
Non-surgical management
- Offloading: Total contact casts, removable walkers, or half-shoes reduce plantar pressure by 50-90%; gold standard for neuropathic ulcers.
- Wound care: Sharp debridement removes necrotic tissue weekly; maintain moist environment with dressings.
- Glycemic control: Target HbA1c <7% enhances healing.
- Infection control: Oral antibiotics for mild cases (1-2 weeks), IV for severe; cover MRSA if prevalent.
Surgical management
For non-healing ulcers (>4-6 weeks) or deep infection:
- Debridement/excision of bone prominences.
- Vascular revascularization (angioplasty/bypass).
- Amputation (toe/ray/partial foot) if gangrene or uncontrolled infection.
| Grade | Description | Treatment Focus |
|---|---|---|
| 0 | Pre-ulcerative (callus) | Debridement, offloading |
| 1 | Superficial | Dressings, offloading |
| 2 | Deep to tendon/capsule | Debridement, antibiotics |
| 3 | Deep abscess/osteomyelitis | Surgery, IV antibiotics |
| 4 | Gangrene forefoot | Partial amputation |
(University of Texas Wound Classification System, adapted)
Complications
Untreated DFUs lead to cellulitis (50%), osteomyelitis (20-50%), gangrene, and amputation (15-20% within 1 year). Charcot neuroarthropathy causes destructive joint changes. Systemic sepsis is life-threatening.
How can diabetic foot ulcers be prevented?
Prevention emphasizes daily foot inspection, education, and risk reduction:
- Daily care: Wash, dry, moisturize feet; check for cuts/blisters; trim nails straight.
- Footwear: Custom orthotics, well-fitted shoes to offload pressure.
- Diabetes management: Tight glycemic control, smoking cessation, weight loss.
- Screening: Annual podiatry exams with monofilament testing.
- Education: Teach patients to recognize early signs and seek prompt care.
Multidisciplinary foot care clinics reduce amputation rates by 50-85%.
Related topics
- Charcot foot
- Diabetic neuropathy
- Peripheral artery disease
- Venous leg ulcer
- Wound dressings
Frequently asked questions
What causes the most diabetic foot ulcers?
The triad of neuropathy, trauma, and deformity accounts for 63% of cases.
Can diabetic foot ulcers heal on their own?
Rarely; most require intervention due to impaired healing.
How long do they take to heal?
Weeks to months; 20-50% persist beyond 12 weeks.
Does smoking worsen diabetic foot ulcers?
Yes, by exacerbating PAD and delaying healing.
When is amputation necessary?
In cases of extensive gangrene, uncontrolled infection, or non-healing despite optimal care.
References
- Diabetic Foot Ulcer: Causes, Prevention, and Treatment — Northern Ankle Foot. 2023. https://www.northernanklefoot.com/diabetic-foot-ulcer-causes-prevention-and-treatment/
- Diabetic Foot Ulceration and Complications – StatPearls — NCBI Bookshelf / NIH. 2023-10-01. https://www.ncbi.nlm.nih.gov/books/NBK499887/
- Diabetic Foot Ulcer – Causes, Treatment, and Prevention — Vohra Wound Care. 2023. https://vohrawoundcare.com/diabetic-foot-ulcer/
- Diabetic Foot Ulcers — UCSF Surgical Oncology. 2023. https://surgicaloncology.ucsf.edu/condition/diabetic-foot-ulcers
- Diabetic Foot Ulcer — University of Michigan Health. 2023. https://www.uofmhealth.org/our-care/specialties-services/diabetic-foot-ulcer
- Diabetic Foot Ulcers: Pathogenesis and Management — AAFP. 2002-11-01. https://www.aafp.org/pubs/afp/issues/2002/1101/p1655.html
- Diabetic Wound Care — APMA. 2023. https://www.apma.org/diabeticwoundcare/
Read full bio of Sneha Tete