Diabetic Retinopathy: 4 Stages, Symptoms, Treatments
Understand diabetic retinopathy: causes, symptoms, stages, screening, and treatments to protect your vision effectively.
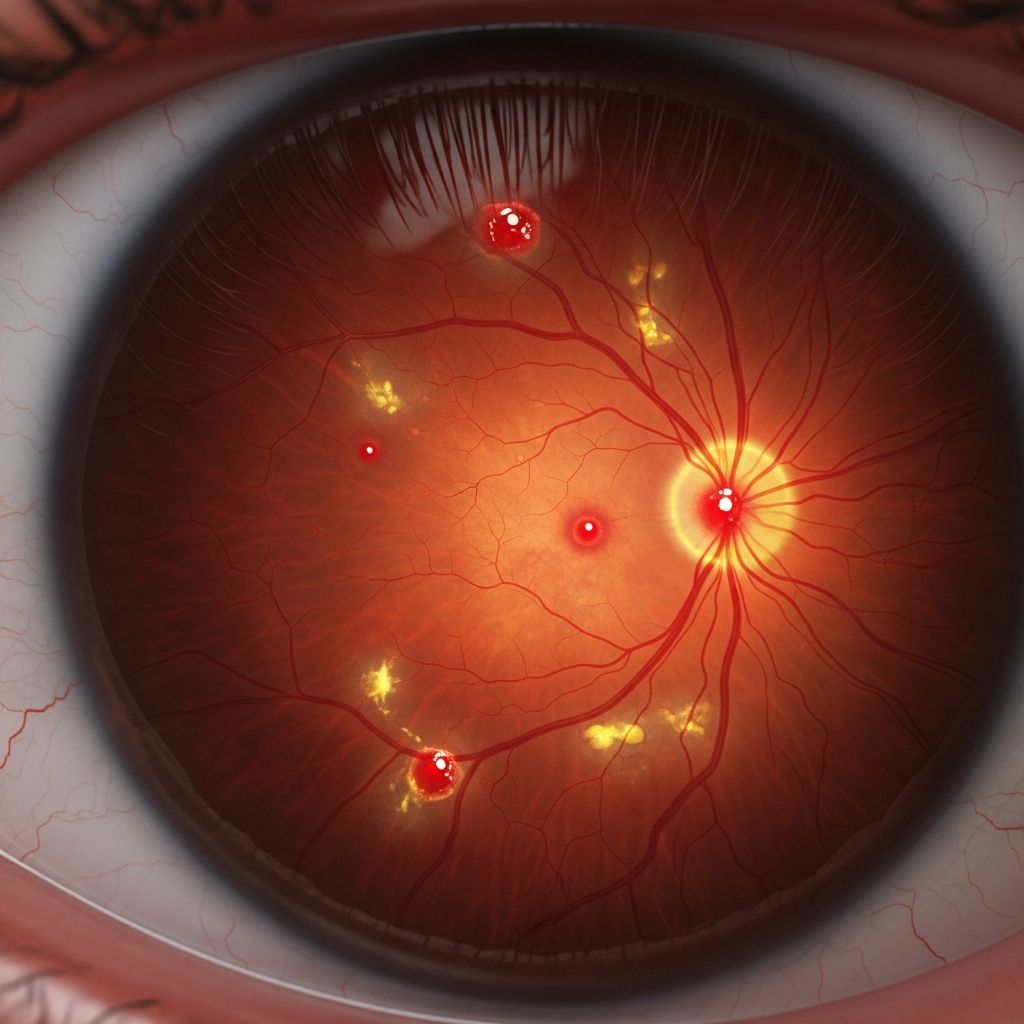
Diabetic retinopathy is a diabetes-related eye condition that affects the blood vessels in the retina, the light-sensitive layer at the back of the eye responsible for vision. If left untreated, it can progress to cause blurred vision, partial sight loss, or even total blindness in severe cases. Good control of blood sugar (glucose) and blood pressure significantly slows its progression, while early treatments like laser therapy can often prevent vision loss.
What is diabetic retinopathy?
Diabetic retinopathy is a complication of diabetes that damages the tiny blood vessels (microvasculature) in the retina. Prolonged high blood glucose levels associated with diabetes weaken these vessels, causing them to leak fluid, swell, or form abnormal new ones (neovascularization). This chronic progressive disease is the leading cause of severe sight impairment in working-age adults in the UK and a major cause of blindness in the US.
People with diabetes also face higher risks of other eye issues, such as cataracts and glaucoma. Retinopathy can develop in both type 1 and type 2 diabetes, with risk increasing the longer diabetes is unmanaged. Damage begins subtly when glucose blocks retinal blood vessels, leading to poor circulation, fluid leaks (microaneurysms), and eventual scar tissue or retinal detachment if untreated.
Diabetic retinopathy symptoms
In the early stages, diabetic retinopathy often produces no noticeable symptoms, making regular screening essential. As it advances, common symptoms include:
- Blurred or fluctuating vision.
- Seeing floaters (dark spots or strings) or flashes of light.
- Sudden vision loss in one or both eyes.
- Double vision or distorted vision.
- Pain, pressure, or problems with peripheral (side) vision in advanced cases.
Without treatment, progression can lead to irreversible blindness, particularly if new vessels bleed into the eye’s vitreous humor or cause retinal detachment. Early detection through annual dilated eye exams is crucial, as symptoms may appear only after significant damage.
Diabetic retinopathy stages
Diabetic retinopathy develops gradually over years, classified into stages based on severity. Progression varies between eyes and accelerates with poor diabetes control or co-existing hypertension.
Stage 1: Background retinopathy (non-proliferative diabetic retinopathy, mild)
This initial stage features tiny leaks of fluid (exudates) and microaneurysms (small bleeds) visible as dots or blots on retinal exam. Vision remains unaffected, but these changes indicate early vessel damage. With good blood sugar and pressure control, it may not progress.
Stage 2: Pre-proliferative retinopathy (non-proliferative, moderate to severe)
Vessels become more dilated and irregular, with larger areas of poor blood flow (ischemia), hemorrhages, and cotton wool spots (nerve fiber damage). Vision may still be normal, but this signals higher risk of progression. Immediate referral to an ophthalmologist is often needed.
Stage 3: Maculopathy
The macula (central retina for sharp vision) swells due to fluid leakage (macular edema), causing central vision blur. This can occur at any stage but is common in moderate cases. It’s a leading cause of vision loss in diabetic retinopathy and requires urgent treatment.
Stage 4: Proliferative retinopathy (proliferative diabetic retinopathy, PDR)
Advanced stage where new, fragile vessels grow (neovascularization) on the retina or iris, leading to bleeding (vitreous hemorrhage), scar tissue, tractional retinal detachment, or neovascular glaucoma. This can cause severe, sudden vision loss or pain.
Key Progression Factors: Longer diabetes duration (especially >10 years), poor glycemic control (HbA1c >7%), hypertension, high cholesterol, pregnancy, and smoking accelerate stages.
Who develops diabetic retinopathy?
Retinopathy affects over half of people with diabetes after 10-15 years, more commonly in type 1 but increasingly in type 2 with rising prevalence. It’s the top cause of blindness in working-age adults. Risk factors include:
- Duration of diabetes (nearly all type 1 patients after 20 years).
- Poor blood glucose control.
- High blood pressure or kidney disease.
- Pregnancy (gestational changes worsen it rapidly).
- Ethnicity (higher in South Asian, African-Caribbean groups in UK).
Not everyone develops it; tight control can prevent or delay onset.
Diabetic eye screening
National programs like the UK’s Diabetic Eye Screening Programme offer free annual digital retinal photography for all with diabetes over age 12. A trained photographer dilates pupils and images the retina; AI-assisted grading detects changes.
Results:
- No retinopathy: Annual rescreen.
- Background: 6-12 month follow-up.
- Observable retinopathy: Fast-track to ophthalmologist.
- Referable (pre-proliferative, maculopathy, PDR): Same-day specialist referral.
In the US, annual comprehensive dilated exams are recommended by the American Diabetes Association. Early detection halves vision loss risk.
Preventing diabetic retinopathy
Strict diabetes management is key:
- Maintain HbA1c <7% (individualized).
- Control blood pressure (<130/80 mmHg).
- Manage cholesterol; quit smoking.
- Healthy diet, exercise, annual eye exams.
- Pregnant women: more frequent screening.
Studies like the Diabetes Control and Complications Trial show intensive control reduces retinopathy risk by 76%.
Treatment of diabetic retinopathy
Treatments stabilize or improve vision, not cure. Choice depends on stage.
Laser treatment (photocoagulation)
Gold standard for PDR: Argon laser seals leaks and destroys ischemia-driven new vessels. Focal laser treats macular edema; panretinal for PDR (500-2000 spots). Side effects: reduced night vision, color perception. Success: prevents severe loss in 90%.
Anti-VEGF injections
Intravitreal injections (e.g., ranibizumab, aflibercept) block vessel growth factors, shrinking new vessels and reducing macular edema. Monthly initially, then as-needed. Highly effective for edema; fewer side effects than steroids.
Steroid implants/injections
For persistent edema (e.g., dexamethasone implant). Risks: cataracts, glaucoma.
Vitrectomy
Surgical removal of vitreous blood/scar tissue in advanced PDR with hemorrhage or detachment. Improves vision in 80-90%.
| Stage | Primary Treatment | Expected Outcome |
|---|---|---|
| Background | Observation + control | Stable vision |
| Maculopathy | Anti-VEGF/laser | Reduced edema |
| PDR | Laser + anti-VEGF | Regression of vessels |
| Advanced | Vitrectomy | Restored vision |
Prognosis
With screening and treatment, most retain good vision. Untreated PDR causes blindness in >50%. Post-treatment, lifelong monitoring and diabetes control are vital to prevent recurrence.
Frequently Asked Questions (FAQs)
Q: How often should I get eye screening if I have diabetes?
A: Annually via national programs or comprehensive dilated exams. More frequent if changes detected or during pregnancy.
Q: Can diabetic retinopathy be reversed?
A: Early stages stabilize; advanced damage is irreversible, but treatments prevent worsening.
Q: Does type 2 diabetes cause retinopathy?
A: Yes, equally as type 1, especially after 5-10 years.
Q: What if I have no symptoms?
A: Screening detects silent damage; don’t wait for symptoms.
Q: Can lifestyle changes prevent it?
A: Yes, tight glucose/BP control reduces risk by up to 76%.
References
- Diabetic Retinopathy: Causes, Symptoms, and Treatment — Patient.info. 2023. https://patient.info/diabetes/diabetic-retinopathy
- Diabetic Retinopathy — National Eye Institute (NIH). 2024-01-15. https://www.nei.nih.gov/eye-health-information/eye-conditions-and-diseases/diabetic-retinopathy
- Diabetic Retinopathy and Diabetic Eye Problems — Patient.info (Doctor). 2023. https://patient.info/doctor/endocrine-disorders/diabetic-retinopathy-and-diabetic-eye-problems
- Diabetic Retinopathy — Mayo Clinic. 2024-08-20. https://www.mayoclinic.org/diseases-conditions/diabetic-retinopathy/symptoms-causes/syc-20371611
- Diabetic Retinopathy — American Society of Retina Specialists. 2023. https://www.asrs.org/diabeticretinopathy
- Diabetes-Related Retinopathy — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/8591-diabetic-retinopathy
Read full bio of Sneha Tete











