Diverticulitis: Symptoms, Causes, Treatment Guide
Understand diverticulitis symptoms, causes, dietary management, and treatment options for better digestive health.
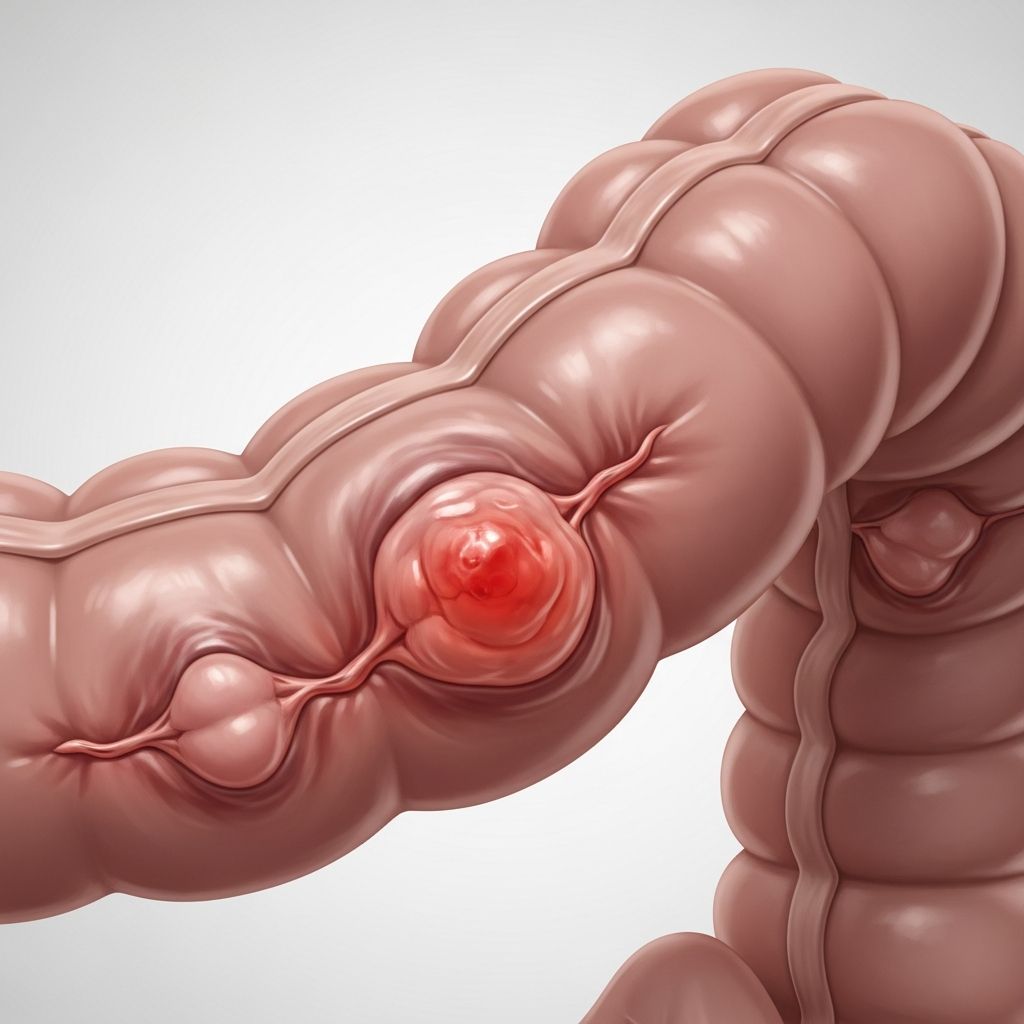
Diverticulitis
Diverticulitis is the inflammation or infection of small pouches called diverticula that develop in the lining of the colon, often causing sudden abdominal pain, fever, and changes in bowel habits. While many people have diverticulosis—the presence of these pouches—without symptoms, diverticulitis occurs when they become inflamed, typically due to bacterial trapping or blockage. This condition affects millions, particularly those over 40, and is linked to low-fiber diets prevalent in Western societies. Early recognition and management are crucial to prevent complications like abscesses or perforations.
What is Diverticulitis?
Diverticula are tiny, balloon-like sacs that protrude from the colon wall, most commonly in the sigmoid colon (lower left side). Diverticulosis refers to their presence without inflammation, affecting about half of Americans over 60. Diverticulitis develops when these pouches get infected or inflamed, often from stool or bacteria becoming trapped inside. Uncomplicated cases involve mild inflammation treatable at home, while complicated ones may lead to abscesses, fistulas, blockages, or perforations requiring hospitalization. Symptoms typically include persistent lower left abdominal pain, tenderness, fever, chills, nausea, vomiting, bloating, and altered bowel habits like constipation or diarrhea.
Risk increases with age as colon walls weaken, but lifestyle plays a major role. In right-sided (ascending) colon cases, pain may localize differently, though left-sided is more common. Prompt diagnosis via CT scans or blood tests helps distinguish it from other conditions like appendicitis or IBS.
Signs & Symptoms of Diverticulitis
- Sudden, severe abdominal pain: Usually lower left side, constant or cramping, worsened by movement.
- Fever and chills: Indicate infection, often above 100.4°F.
- Nausea and vomiting: Due to gut irritation.
- Bowel changes: Constipation, diarrhea, or bloating.
- Blood in stool or urinary issues: Signals complications like fistulas.
Symptoms can mimic other GI issues, so medical evaluation is essential, especially if pain persists beyond 24-48 hours or worsens. In severe cases, signs of peritonitis (rigid abdomen, high fever) demand emergency care.
Causes
The precise cause remains unclear, but low-fiber diets lead to hard stools, straining, and increased colon pressure, promoting diverticula formation. Aging weakens colon muscles, while obesity, smoking, inactivity, and genetics heighten risk. Bacteria or fecal matter trapped in pouches triggers inflammation. Unlike past myths, nuts, seeds, or popcorn do not cause attacks. Chronic constipation from processed foods exacerbates pressure in the sigmoid colon.
Diagnosis
Doctors start with history and physical exam, checking for abdominal tenderness. Blood tests detect infection (high white cells), while stool tests rule out blood or other issues. CT scans are gold standard, revealing inflamed diverticula, abscesses, or perforations with 97% accuracy. Colonoscopy is avoided during acute flares but used later to exclude cancer. Ultrasound or MRI may supplement in select cases. Early imaging prevents complications.
Diverticulitis Treatment
Treatment varies by severity. Mild, uncomplicated cases (no fever >101°F, no peritonitis) are managed outpatient.
- Rest and diet: Clear liquids 2-3 days (broth, gelatin, tea), then low-fiber solids, advancing to high-fiber.
- Antibiotics: Oral like ciprofloxacin + metronidazole for 7-10 days.
- Pain relief: Acetaminophen; avoid NSAIDs/steroids as they risk bleeding/perforation.
- Hospitalization for severe cases: IV antibiotics, fluids, NG tube if vomiting; drainage for abscesses.
Surgery (colectomy) is for recurrent, complicated, or non-responding cases, often laparoscopic. Post-flare, high-fiber diet prevents recurrence.
Eating Right with Diverticulitis & Diverticulosis
Diet is cornerstone. For active diverticulitis, liquid diet rests the bowel. Recovery emphasizes gradual fiber increase to 25-30g/day to soften stools and reduce pressure.
High-Fiber Foods:
- Fruits: Apples (with skin), pears, berries (5-8g/serving).
- Vegetables: Broccoli, carrots, Brussels sprouts (4-6g/cup).
- Whole grains: Oats, brown rice, quinoa (3-6g/serving).
- Legumes: Beans, lentils (7-15g/cup).
Start slow to avoid gas; drink 64+ oz water daily. Fiber supplements like psyllium (Metamucil) aid if diet insufficient. Probiotics may support gut bacteria. Avoid low-fiber during flares but long-term high-fiber cuts recurrence 40%.
| Food Type | Examples | Fiber per Serving |
|---|---|---|
| Fruits | Raspberries (1 cup) | 8g |
| Vegetables | Broccoli (1 cup) | 5g |
| Grains | Oatmeal (1 cup) | 4g |
| Legumes | Black beans (1/2 cup) | 7.5g |
Soluble fiber (oats, apples) binds water; insoluble (veggies, grains) adds bulk.
Complications of Diverticulitis
- Abscess: Pus pocket; drained percutaneously.
- Perforation: Pouch rupture causes peritonitis.
- Fistula: Abnormal connections to bladder/bowel.
- Obstruction: Scarring blocks colon.
- Sepsis: Life-threatening infection spread.
Complications occur in 4% uncomplicated cases but rise with delays.
When to See a Doctor
Seek care for new/worsening abdominal pain, fever >100.4°F, bloody stool, vomiting preventing fluids, or symptoms >48 hours. ER for severe pain, distension, or shock signs.
Prevention Tips
- Maintain 25-35g fiber daily.
- Exercise 150 min/week.
- Stay hydrated.
- Quit smoking, manage weight.
- Mesalazine or rifaximin for symptom-prone diverticulosis.
These reduce recurrence by 50%.
Frequently Asked Questions
Can diverticulitis be cured?
Acute episodes resolve with treatment; prevention manages chronic risk. Surgery cures recurrent cases.
Is a high-fiber diet safe during remission?
Yes, essential to prevent flares; increase gradually.
Do nuts/seeds cause diverticulitis?
No, myth debunked; safe in moderation.
How long does recovery take?
3-7 days for mild; weeks for complicated.
Is surgery always needed?
No, only 20% recurrent cases.
References
- Diverticulitis: Symptoms, Causes and Treatment — Phoenix Unified Surgeons. 2023. https://phoenixunified.com/diverticulitis-treatment
- Diverticulitis: Causes, Symptoms, and Treatment Options — Vegas Digestive Health Center. 2023. https://www.vegasdhc.com/blog/1314029-diverticulitis-causes-symptoms-and-treatment-options-from-a-gastroenterologist/
- How to Relieve Diverticulitis Pain Fast — Houston Methodist. 2025-06-01. https://www.houstonmethodist.org/blog/articles/2025/jun/how-to-relieve-diverticulitis-pain-fast/
- Diverticulitis — UCSF Department of Surgery. 2023. https://surgery.ucsf.edu/condition/diverticulitis
- Diverticulitis: Symptoms, Causes & Treatment — Cleveland Clinic. 2023. https://my.clevelandclinic.org/health/diseases/10352-diverticulitis
- Diverticular Disease — NIDDK (NIH). 2023. https://www.niddk.nih.gov/health-information/digestive-diseases/diverticulosis-diverticulitis
Read full bio of Sneha Tete










