Diverticulitis: Symptoms, Causes, Treatment Guide
Comprehensive guide to diverticulitis: symptoms, causes, diagnosis, treatment, and prevention strategies for better digestive health.
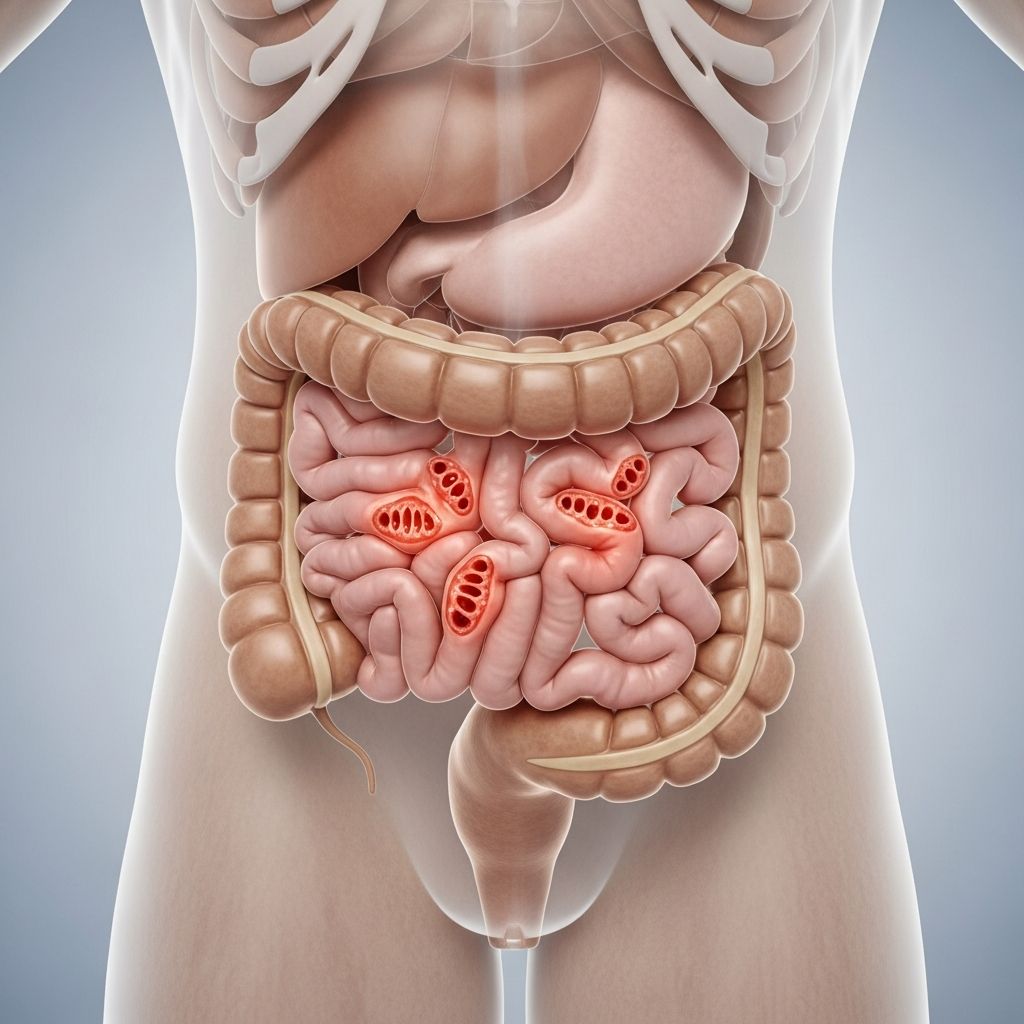
Diverticulitis Overview
Diverticulitis is a common digestive condition characterized by inflammation of small pouches called diverticula that form in the wall of the large intestine, primarily the colon. While many people have diverticulosis—the presence of these pouches—without symptoms, inflammation leads to diverticulitis, causing pain and potential complications. In the US, the annual incidence is about 180 per 100,000 people, leading to around 200,000 hospital admissions and over $6.3 billion in healthcare costs yearly.
What Is Diverticulitis?
Diverticula are small, bulging pouches that develop in weakened areas of the colon wall, often due to increased pressure from straining during bowel movements. Diverticulosis refers to the presence of these pouches, which affects up to 50% of people over 60 in Western countries. Diverticulitis occurs when these pouches become inflamed or infected, typically from trapped fecal matter or bacteria.
Acute diverticulitis presents suddenly with left lower quadrant pain, while chronic forms involve persistent symptoms. Uncomplicated cases (80% of instances) resolve with conservative care, but complicated ones may involve abscesses, perforations, or fistulas.
Symptoms of Diverticulitis
The hallmark symptom is
sudden, intense pain
in the lower left abdomen, though it can vary in intensity and may radiate to the back or pelvis. Pain often worsens gradually and is accompanied by tenderness when touched.Other common symptoms include:
- **Fever** and chills, indicating infection.
- **Nausea and vomiting**.
- **Changes in bowel habits**, such as diarrhea, constipation, or bloating.
- **Leukocytosis** (elevated white blood cell count) and systemic signs like fatigue.
In Asian populations, symptoms may localize to the right upper quadrant due to diverticula prevalence there. Chronic diverticulitis features ongoing pain for months, potentially leading to obstruction from fibrosis. Seek immediate care if pain is severe, accompanied by high fever, or signs of peritonitis like rigid abdomen.
Causes and Risk Factors
Diverticula form from high intraluminal pressure in the colon, often linked to low-fiber diets causing hard stools and straining. Inflammation arises from microperforations allowing bacteria entry, or obstruction by stool.
Key risk factors include:
| Risk Factor | Description |
|---|---|
| Age | Most common over 40; prevalence rises with age. |
| Diet | Low fiber (<25g/day) increases risk; high red meat intake implicated. |
| Obesity | BMI >30 doubles risk via inflammation. |
| Smoking | Increases complication rates. |
| Genetics/Lifestyle | Sedentary habits, NSAIDs use, steroids elevate susceptibility. |
Approximately 1-4% of those with diverticulosis develop diverticulitis lifetime. Theories include trapped feces breeding bacteria or viral triggers like cytomegalovirus.
Diagnosis of Diverticulitis
Diagnosis starts with history and physical exam focusing on abdominal tenderness.
Contrast-enhanced CT scan
is gold standard, with 98-99% sensitivity and near 100% specificity, revealing wall thickening, fat stranding, and complications like abscesses.Additional tests:
- Blood tests: Elevated CRP, WBC for inflammation.
- Stool tests: Rule out infection or blood.
- Colonoscopy: Deferred acutely; used post-resolution to exclude cancer.
Differential includes appendicitis, IBD, or malignancy; long-segment involvement (>10cm) favors diverticulitis.
Diverticulitis Treatment
Treatment varies by severity.
Uncomplicated diverticulitis
(Hinchey I) uses outpatient management: clear liquids, pain control (acetaminophen), and observation. Antibiotics (e.g., ciprofloxacin + metronidazole) for persistent fever, immunocompromised, or elderly.**Complicated cases** require hospitalization:
- IV antibiotics: Ceftriaxone + metronidazole or piperacillin-tazobactam.
- Abscess (<4cm): Antibiotics; larger: Percutaneous drainage.
- Perforation/Obstruction: Surgery (resection, colostomy if needed).
Chronic/recurrent: Elective surgery like sigmoid colectomy after 2 episodes. Recovery involves gradual diet advancement.
Complications of Diverticulitis
While 80% uncomplicated, risks include:
- **Abscess**: Pus collection; drained percutaneously.
- **Perforation**: Free leak causing peritonitis.
- **Fistula**: Abnormal connections (e.g., colovesical, causing pneumaturia).
- **Obstruction**: From strictures.
- **Pylephlebitis**: Rare portal vein thrombosis.
Mortality low (1-4%) but rises with sepsis.
Prevention and Management
High-fiber diet (25-30g/day: fruits, veggies, whole grains) softens stool, reducing pressure. Hydration (8+ cups/day), exercise (150min/week), weight control, and quitting smoking prevent flares.
Avoid nuts/seeds/corn myth debunked; no evidence increases risk. Probiotics under study. Regular screenings for high-risk.
When to See a Doctor
Consult for persistent abdominal pain, fever >100.4°F, blood in stool, or unexplained weight loss. Emergency for severe pain, vomiting preventing fluids, or shock signs.
Frequently Asked Questions (FAQs)
What foods trigger diverticulitis?
No specific triggers proven; low-fiber diets contribute long-term. During flares, stick to low-residue.
Can diverticulitis be cured?
Uncomplicated resolves with treatment; recurrent may need surgery. Lifestyle prevents.
Is diverticulitis life-threatening?
Rarely; complications like perforation raise risks but treatable promptly.
How long does a flare-up last?
7-10 days with treatment; chronic varies.
Does alcohol worsen diverticulitis?
Moderate ok; excess via dehydration/smoking risks indirectly.
This comprehensive overview equips you with knowledge on managing diverticulitis effectively. Always consult healthcare providers for personalized advice.
References
- Diverticulitis: A Review — JAMA Network. 2024. https://jamanetwork.com/journals/jama/article-abstract/2836826
- Diverticulitis: a comprehensive review with usual and unusual — PMC (NCBI). 2017-02-17. https://pmc.ncbi.nlm.nih.gov/articles/PMC5265196/
- Diverticulitis – Symptoms and causes — Mayo Clinic. Accessed 2026. https://www.mayoclinic.org/diseases-conditions/diverticulitis/symptoms-causes/syc-20371758
- Diverticulitis: Symptoms, Causes & Treatment — Cleveland Clinic. Accessed 2026. https://my.clevelandclinic.org/health/diseases/10352-diverticulitis
Read full bio of Sneha Tete











