Diverticulosis Vs Diverticulitis: Key Differences To Know
Understand the key differences between diverticulosis and diverticulitis, their symptoms, causes, treatments, and prevention strategies for better digestive health.
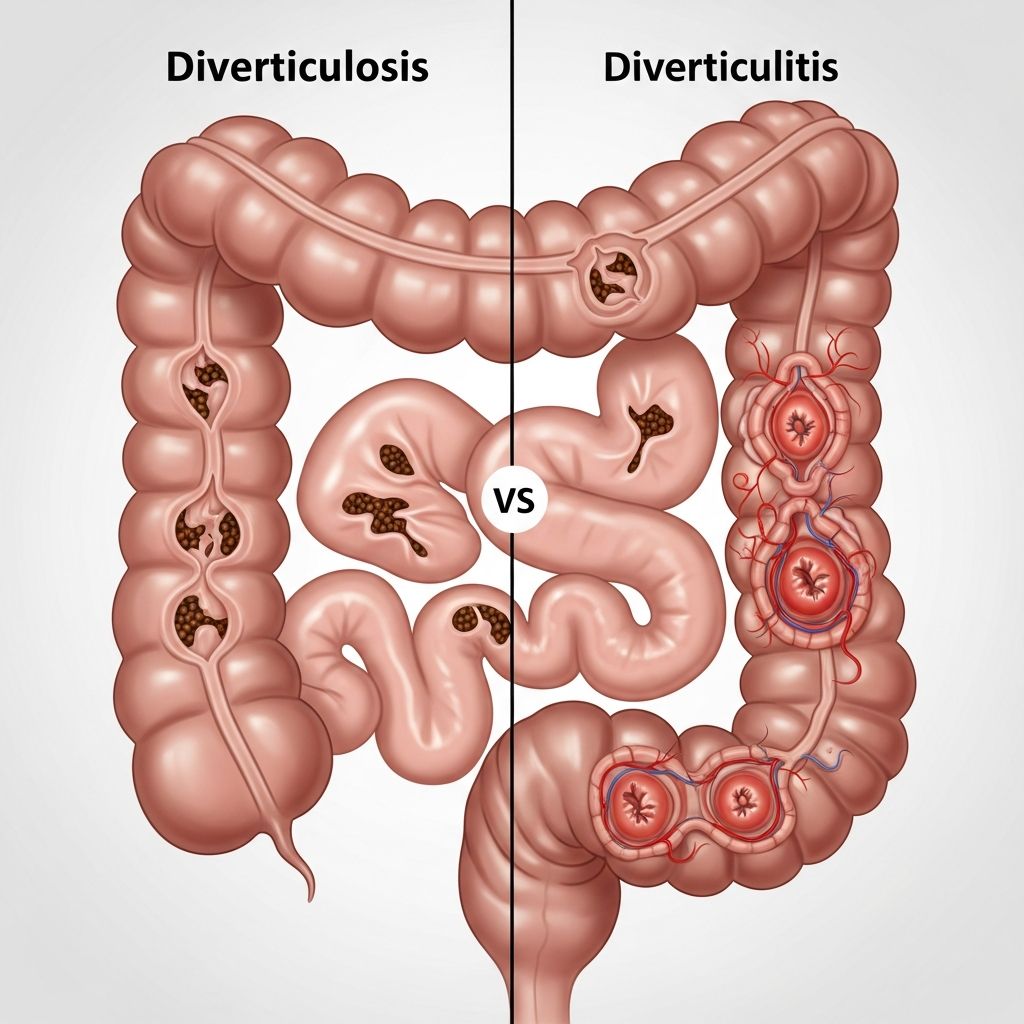
Diverticulosis vs. Diverticulitis: What’s the Difference?
Diverticulosis and diverticulitis are related conditions affecting the colon, but they differ significantly in symptoms, severity, and treatment. Diverticulosis refers to the formation of small pouches (diverticula) in the colon wall, often without symptoms, while diverticulitis occurs when these pouches become inflamed or infected, leading to pain and potential complications.
What Is Diverticulosis?
Diverticulosis is a common condition where small, bulging pouches called
diverticula
form in the lining of the digestive tract, particularly in the lower part of the large intestine (sigmoid colon). These pouches develop when weak spots in the colon wall give way under pressure, allowing the inner lining to push through. It affects about 50% of people over age 60 in Western countries and often goes unnoticed because it produces no symptoms.Diverticula are typically 5-10 millimeters in diameter but can grow larger. They form due to increased pressure in the colon from hard stool, often linked to low-fiber diets. While usually harmless, symptomatic diverticulosis can cause mild issues like bloating or irregular bowel habits.
What Is Diverticulitis?
**Diverticulitis** develops when one or more diverticula become inflamed or infected, often due to trapped stool or bacteria. This leads to sudden, severe symptoms, distinguishing it from asymptomatic diverticulosis. Diverticulitis accounts for only 4-5% of cases where diverticulosis progresses, but it requires prompt medical attention.
There are two main types: uncomplicated diverticulitis (about 80% of cases), involving inflammation without severe issues, and complicated diverticulitis (20%), which involves serious problems like abscesses or perforations.
Diverticulosis vs. Diverticulitis: Key Differences
| Aspect | Diverticulosis | Diverticulitis |
|---|---|---|
| Definition | Presence of pouches in colon wall | Inflammation/infection of pouches |
| Symptoms | Often none; mild bloating/cramping | Severe abdominal pain, fever, nausea |
| Prevalence | Common in older adults | Less common, 4-5% of diverticulosis cases |
| Treatment | Diet/lifestyle changes | Antibiotics, hospitalization if severe |
This table highlights the core distinctions, with diverticulosis as a structural change and diverticulitis as an acute inflammatory event.
Symptoms of Diverticulosis
Most people with diverticulosis experience no symptoms, discovering it incidentally during colonoscopies or imaging. When symptoms occur, they include:
- Mild abdominal pain or cramping
- Bloating and gas
- Changes in bowel habits (constipation or diarrhea)
- Blood in stool (rare, painless bleeding)
These mimic other GI issues, so routine screening is key for early detection.
Symptoms of Diverticulitis
Diverticulitis symptoms are more intense and sudden, often starting in the lower left abdomen:
- Persistent, severe pain worsening over days
- Fever and chills
- Nausea, vomiting
- Bloating, constipation, or diarrhea
- Blood in stool or inability to pass gas/stool
In right-sided diverticulitis (less common), pain may be in the lower right abdomen. Seek immediate care for high fever (>100.4°F), sharp pain, or distended abdomen.
Causes and Risk Factors
Causes: Diverticula form from high intraluminal pressure straining weak colon walls, exacerbated by low-fiber diets causing hard stools. In diverticulitis, fecal matter traps in pouches, leading to bacterial overgrowth and inflammation.
Risk Factors:
- Age over 50
- Low-fiber diet
- Obesity
- Smoking
- Lack of exercise
- NSAID use
- Genetics
Western diets high in processed foods increase risk compared to high-fiber Asian diets.
Complications of Diverticulitis
Untreated diverticulitis can lead to serious issues in 20% of cases:
- Abscess: Pus-filled swelling requiring drainage
- Fistula: Abnormal connection to bladder/vagina
- Obstruction: Blockage from scarring
- Perforation: Hole in colon wall
- Peritonitis: Life-threatening abdominal infection
- Bleeding: From eroded vessels
Complicated cases may need surgery.
Diverticulitis vs. IBS: How to Tell Them Apart
Both cause abdominal pain and bowel changes, but IBS is functional (no structural damage), while diverticulitis is inflammatory. IBS pain is crampy, relieved by defecation, and stress-triggered; diverticulitis pain is constant, fever-associated, and localized. Diagnosis via imaging confirms diverticulitis.
Diagnosis
Diagnosis starts with history and physical exam. Tests include:
- CT scan: Gold standard for diverticulitis, showing inflammation/thickening
- Blood tests: For infection/inflammation markers
- Colonoscopy: For diverticulosis, avoided in acute diverticulitis
- Stool tests: Rule out infection/bleeding
Ultrasound or MRI may be used in some cases.
Treatment Options
Treating Diverticulosis
Focuses on prevention:
- High-fiber diet (25-30g/day): fruits, veggies, whole grains
- Plenty of fluids
- Exercise
- Avoid nuts/seeds if symptomatic (debated)
Fiber supplements like psyllium help soften stool.
Treating Diverticulitis
Mild/uncomplicated: Oral antibiotics (e.g., ciprofloxacin + metronidazole), clear liquids, pain relievers.
Severe/complicated: Hospitalization, IV antibiotics, fluids, bowel rest. Surgery for abscess drainage, resection, or colostomy in emergencies.
Most recover in 7-10 days with treatment.
Prevention Tips
Lifestyle changes reduce risk:
- Eat high-fiber foods
- Stay hydrated (8+ glasses water/day)
- Exercise 30 min/day
- Maintain healthy weight
- Quit smoking
- Limit red meat/processed foods
Regular screenings catch diverticulosis early.
When to See a Doctor
Consult for new abdominal pain, blood in stool, persistent bowel changes, or fever. Emergencies include severe pain, vomiting, or inability to pass stool/gas.
Frequently Asked Questions (FAQs)
Can diverticulosis turn into diverticulitis?
Yes, in 4-5% of cases, but high-fiber diets lower risk.
Is diverticulitis curable?
Mild cases resolve with treatment; recurrent or complicated may need surgery.
What foods trigger diverticulitis?
Low-fiber diets contribute; during flares, avoid solids initially.
Does diverticulosis cause cancer?
No direct link, but screening rules out cancer.
How is diverticular disease different?
It encompasses symptomatic diverticulosis and diverticulitis.
References
- Diverticulosis Vs. Diverticulitis: What’s The Difference? — Temple Health. 2023. https://www.templehealth.org/about/blog/diverticulosis-vs-diverticulitis-what-is-the-difference
- Diverticulosis vs Diverticulitis Guide — Colon Digestive. 2024. https://colondigestive.com/diverticulosis-vs-diverticulitis-guide/
- Diverticulosis vs. diverticulitis: How do they differ? — Oshi Health. 2024. https://oshihealth.com/diverticulosis-vs-diverticulitis/
- Diverticulosis vs. diverticulitis: What’s the difference? — HealthPartners. 2023-10-13. https://www.healthpartners.com/blog/diverticulosis-vs-diverticulitis/
- Diverticulosis and diverticulitis — Better Health Channel (Victorian Government). 2023. https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/diverticulosis-and-diverticulitis
- Diverticulosis: What It Is, Symptoms, Causes & Treatment — Cleveland Clinic. 2023-07-05. https://my.clevelandclinic.org/health/diseases/24883-diverticulosis
Read full bio of Sneha Tete











