Ear Infection (Otitis Media): Symptoms, Causes & Treatment
Understanding ear infections: Learn about otitis media symptoms, causes, and effective treatment options.
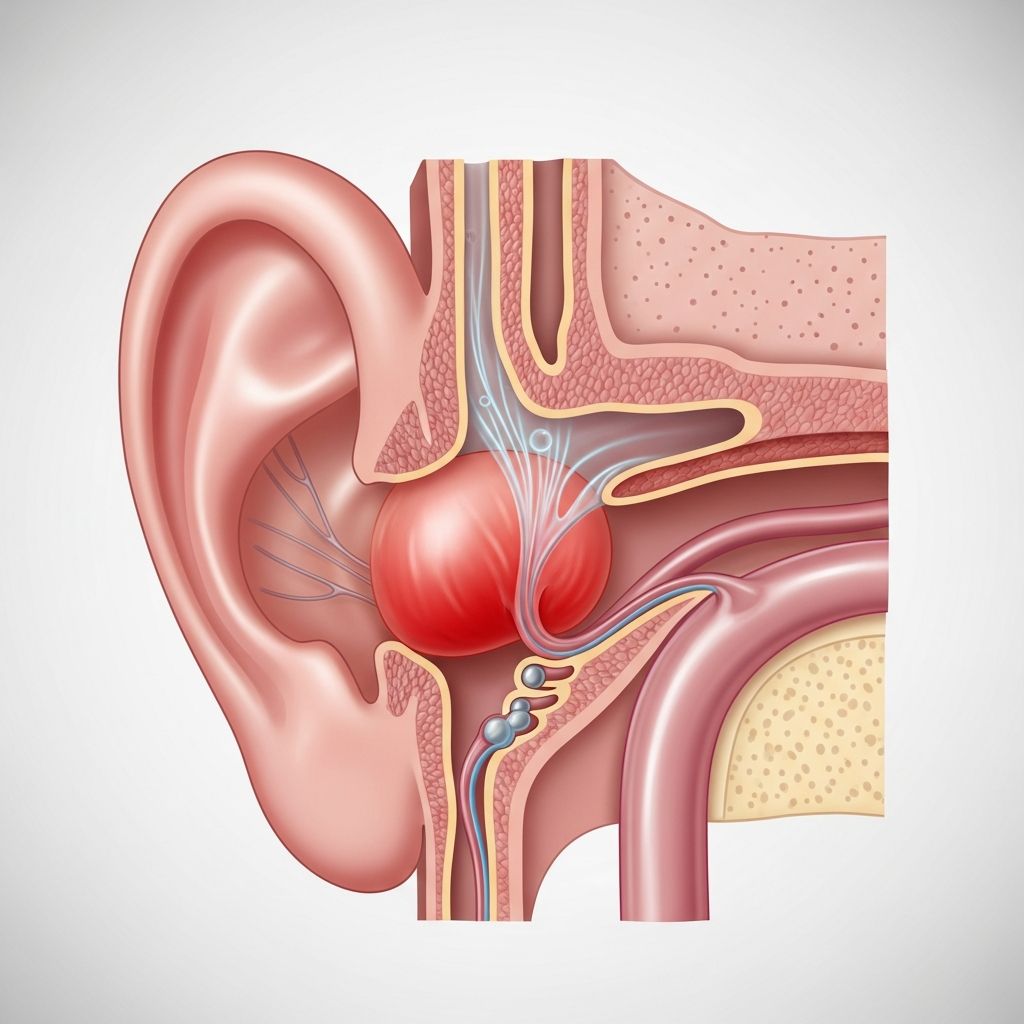
Ear infections, medically known as acute otitis media (AOM), are among the most common infections affecting children and adults alike. An ear infection occurs when a virus or bacteria infects the middle ear, the air-filled space located directly behind the eardrum. This condition can cause significant discomfort and, if left untreated, may lead to complications affecting hearing and overall ear health. Understanding the symptoms, causes, and appropriate treatment options is essential for managing this condition effectively.
What Is Otitis Media?
Otitis media is defined as the recent, abrupt onset of middle ear effusion accompanied by signs or symptoms of inflammation of the middle ear. The diagnosis requires three essential criteria: recent, abrupt onset (within 48 hours), presence of middle ear effusion (fluid), and evidence of middle ear inflammation. Middle ear effusion is critical to the diagnosis—without it, the condition cannot be classified as acute otitis media. A simple red tympanic membrane alone is insufficient for diagnosis; the presence of fluid buildup is necessary to confirm the condition.
Types of Ear Infections
While otitis media is the most common type of ear infection, understanding the different types helps clarify which part of the ear is affected and how treatment may differ.
Middle Ear Infections (Otitis Media): The middle ear is the air-filled space behind the eardrum that plays a crucial role in hearing. Middle ear infections typically result from a cold or other upper respiratory infection. Occasionally, allergies or chronic sinus infections can also trigger middle ear infections. During these respiratory infections, bacteria or viruses travel through the eustachian tubes, causing them to become inflamed and swollen. As the tubes swell, they become blocked and fill with fluid, creating an ideal breeding ground for bacterial growth.
Inner Ear Infections (Otitis Interna): Inner ear infections are most often caused by viral infections, including influenza or the virus responsible for shingles. These infections can also develop when a middle ear infection spreads to the inner ear. Inner ear infections are more prevalent in adults than in children.
Outer Ear Infections (Otitis Externa or Swimmer’s Ear): This type affects the ear canal, the pathway between the outer and middle ear. Swimmer’s ear typically develops following water exposure from swimming or bathing. Moisture in the ear canal creates an environment where bacteria and fungi can proliferate. Additionally, cuts or damage to the skin in the ear canal from cotton swabs or fingernails can increase infection risk.
Symptoms of Ear Infections
Recognizing the symptoms of an ear infection is crucial for early intervention and treatment. Symptoms can vary depending on the type and severity of the infection.
Common Symptoms in Children
In children, the most common and prominent symptom of an ear infection is ear pain. However, young children may express this discomfort in various ways, including:
– Pulling or tugging at the affected ear- Fever- Irritability and fussiness- Difficulty sleeping or restlessness- Drainage from the ear- Difficulty hearing or delayed response to sounds- Loss of appetite
It is important to note that pulling at the ear, while often associated with ear infections, is actually an unreliable indicator, as fewer than 10% of children who pull at their ears have an actual infection. Therefore, a comprehensive evaluation by a healthcare provider is necessary for accurate diagnosis.
Symptoms in Adults
Adults with ear infections may experience similar symptoms, with ear pain being the most prevalent complaint. Additional symptoms can include drainage from the ear, muffled hearing, and in some cases, a sensation of fullness in the affected ear.
Causes and Risk Factors
Infectious Agents
Ear infections result from bacterial or viral infections. Research shows that bacteria account for approximately 85% to 95% of middle ear infections, with the primary culprits being Streptococcus pneumoniae and Haemophilus influenzae type b, responsible for a significant portion of infections. Moraxella catarrhalis causes 5% to 10% of cases, while viruses serve as the sole infectious agent in approximately 5% to 15% of cases. In rare instances, no bacterial growth is detected, which may be attributed to purely viral infections or other factors.
Contributing Factors
Several factors increase the risk of developing an ear infection:
–
Upper Respiratory Infections:
Colds and flu often precede ear infections by 3 to 5 days. The viral infection can trigger inflammation and fluid accumulation in the middle ear.-Eustachian Tube Dysfunction:
When the eustachian tubes become blocked or inflamed, fluid cannot drain properly from the middle ear.-Allergies:
Chronic allergies can cause inflammation and congestion, increasing infection risk.-Environmental Factors:
Exposure to cigarette smoke or air pollution can irritate the eustachian tubes.-Age:
Young children, particularly those between 6 months and 3 years, have a higher incidence of ear infections due to their developing eustachian tubes and immune systems.-Attendance at Daycare:
Group settings increase exposure to viruses and bacteria.-Bottle Feeding in Supine Position:
Lying flat while bottle-feeding can allow fluid to enter the eustachian tubes.Diagnosis
Clinical Evaluation
A proper diagnosis of acute otitis media requires confirmation of a history of abrupt onset (within 48 hours) of middle ear effusion and inflammation. The condition can be suspected clinically when signs and symptoms of an upper respiratory tract infection are accompanied by ear pain, irritability, or other related symptoms. However, definitive diagnosis requires otoscopic examination by a healthcare provider.
Diagnostic Tools
Healthcare providers use an otoscope to examine the eardrum. They may also perform tympanometry, a test that measures how well the eardrum vibrates and moves, helping confirm the presence of fluid in the middle ear. For persistent cases or complications, audiometry may be recommended to assess hearing function.
Treatment Options
Observation and Watchful Waiting
Many ear infections resolve without treatment as the immune system fights the infection. However, observation has certain limitations and specific provisions that healthcare providers consider. If symptoms do not improve within 2 to 3 days, or if the infection worsens, medical intervention becomes necessary.
Pain Management
While the body works to clear the infection, healthcare providers recommend pain relievers to manage discomfort. Over-the-counter options include acetaminophen and ibuprofen, which help reduce ear pain and fever. These medications should be used according to age-appropriate dosing guidelines.
Antibiotic Treatment
Depending on a child’s age, symptoms, and the severity of the infection, antibiotics may be prescribed. Antibiotics are particularly important when bacterial infections are suspected. Common antibiotics used include amoxicillin and amoxicillin-clavulanate, though susceptibility varies. Notably, approximately 25% of pneumococcal strains show nonsusceptibility to penicillin, with some regions reporting nonsusceptibility rates as high as 60%. Patients should complete the full course of antibiotics, typically lasting 7 to 10 days, even if symptoms improve earlier.
Treatment for Different Ear Infection Types
Middle Ear Infections: Oral antibiotics are the standard treatment for middle ear infections caused by bacteria. Pain relievers and decongestants may provide additional symptom relief.
Outer Ear Infections (Swimmer’s Ear): Antibiotic or antifungal ear drops are the primary treatment for swimmer’s ear. It is crucial to understand that the treatment for swimmer’s ear differs significantly from that for middle ear infections, and treatments for one condition should not be used for the other. Healthcare providers may prescribe medicated drops containing antibiotics, corticosteroids, or both to eliminate the infection and reduce inflammation.
Inner Ear Infections: Treatment for inner ear infections may include antibiotics or antivirals, though most commonly healthcare providers use steroids to relieve inflammation. Antihistamines and anti-nausea medications may also be prescribed to manage associated symptoms like dizziness.
When to Seek Medical Care
Parents and caregivers should contact their child’s pediatrician if the child shows signs of an ear infection, particularly if the condition does not improve within 2 to 3 days. Seek immediate medical attention if:
– High fever accompanies the ear pain- Drainage from the ear is present- Hearing loss or muffled hearing develops- Symptoms worsen despite treatment- The child experiences balance problems or dizziness- Signs of infection spreading (severe headache, neck stiffness) appear
Prevention Strategies
While not all ear infections can be prevented, several measures reduce infection risk:
–
Maintain Good Hygiene:
Regular handwashing reduces the spread of viruses and bacteria that cause respiratory infections.-Vaccination:
Up-to-date immunizations, including pneumococcal and influenza vaccines, provide protection against common ear infection causes.-Avoid Smoke and Pollution:
Minimize exposure to secondhand smoke and air pollution.-Breastfeeding:
When possible, breastfeeding provides antibodies that protect against infections.-Proper Bottle Feeding:
Keep the child upright while bottle-feeding to prevent fluid from entering the eustachian tubes.-Manage Allergies:
Treat allergies appropriately to reduce eustachian tube inflammation.-Keep Ears Dry:
After swimming or bathing, dry ears thoroughly to prevent swimmer’s ear.-Avoid Inserting Objects:
Never insert cotton swabs, toys, or other objects into the ear canal.Complications
While most ear infections resolve without complications, untreated or severe infections can lead to serious problems. These include:
–
Hearing Loss:
Temporary or, in rare cases, permanent hearing impairment-Eardrum Perforation:
A hole or tear in the eardrum-Mastoiditis:
Infection spreading to the mastoid bone behind the ear-Meningitis:
In severe cases, infection can spread to the protective membranes around the brain and spinal cord-Cholesteatoma:
An abnormal skin growth in the middle ear resulting from repeated infectionsFrequently Asked Questions
Q: How long does it take for an ear infection to go away?
A: Many ear infections resolve within 7 to 10 days with or without treatment. However, some may take longer, and some require antibiotic treatment to clear the infection completely. If symptoms persist beyond 3 days, contact your healthcare provider.
Q: Can ear infections cause permanent hearing loss?
A: Most ear infections cause temporary hearing loss that resolves once the infection clears. However, repeated or severe infections, particularly during critical developmental years in children, may potentially lead to permanent hearing issues. This is why prompt treatment and follow-up care are important.
Q: Are ear infections contagious?
A: Ear infections themselves are not contagious, but the underlying viral or bacterial infections that cause them can spread from person to person. Good hygiene practices help prevent transmission of these underlying infections.
Q: Can I use home remedies to treat an ear infection?
A: While over-the-counter pain relievers can help manage discomfort, ear infections require proper medical evaluation and treatment. Home remedies alone cannot eliminate bacterial infections, and delaying proper treatment may lead to complications. Always consult with a healthcare provider for appropriate care.
Q: What is the difference between otitis media and swimmer’s ear?
A: Otitis media (middle ear infection) occurs behind the eardrum and is usually caused by upper respiratory infections. Swimmer’s ear (otitis externa) affects the ear canal and is typically caused by water exposure. These conditions require different treatments, so proper diagnosis is essential.
References
- Ear Infection (Otitis Media): Symptoms, Causes & Treatment — Cleveland Clinic. 2023-06-06. https://my.clevelandclinic.org/health/diseases/8613-ear-infection-otitis-media
- New guidelines on acute otitis media — Cleveland Clinic Journal of Medicine, 2006. https://www.ccjm.org/content/ccjom/71/6_suppl_4/S3.full.pdf
- How ear infections can affect hearing — University of Houston College of Optometry. https://www.uhchearing.com/resources/articles/article/ear-health/how-ear-infections-can-affect-hearing
- Treating Earache in Children: Remedies & Tips — Tylenol. https://www.tylenol.com/children-infants/pain-relief/earache-causes-symptoms-relief
- Swimmer’s Ear (Otitis Externa): Symptoms & Care — Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/8381-swimmers-ear-otitis-externa
Read full bio of Sneha Tete











