Ear Infection Overview: Causes, Symptoms, and Treatment
Complete guide to understanding ear infections, their causes, symptoms, and effective treatment options.
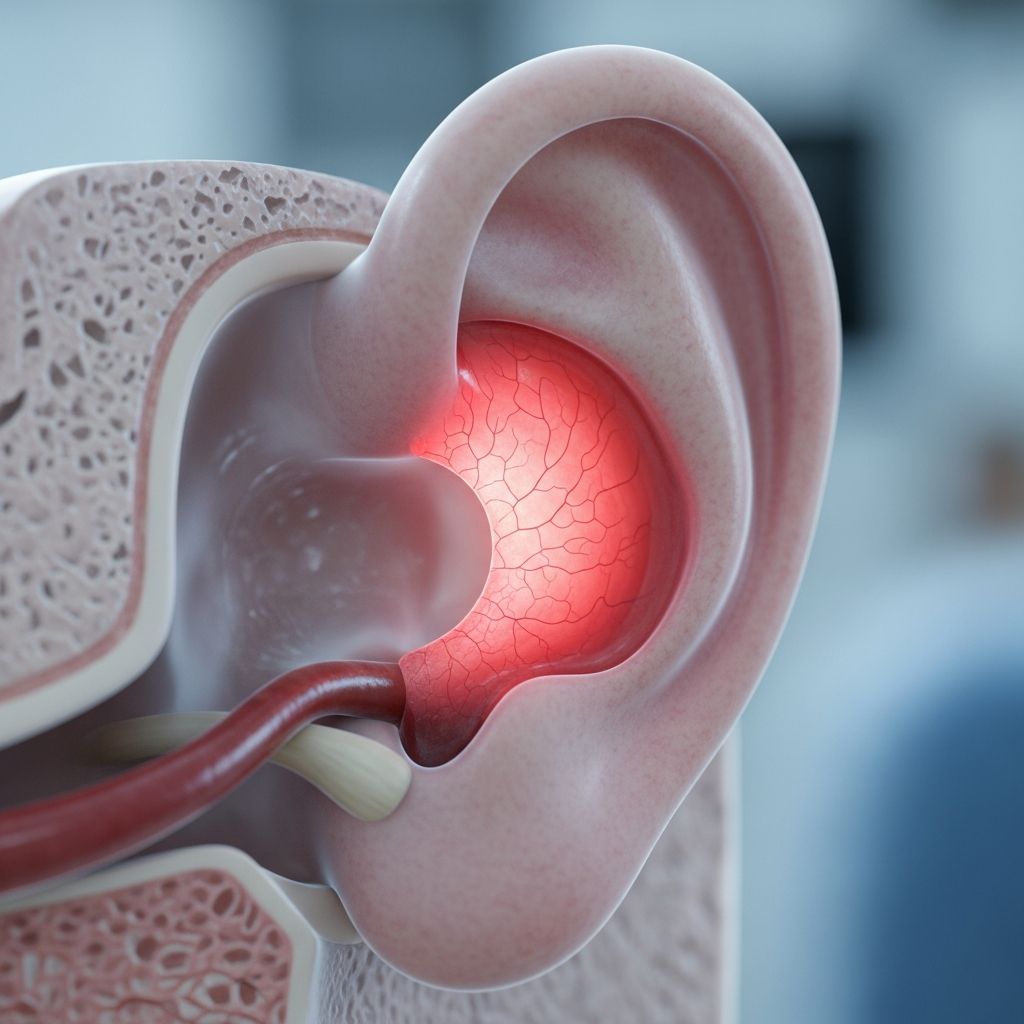
Ear infections are among the most common health conditions affecting children worldwide, and they represent one of the primary reasons parents seek medical care for their young children. An ear infection occurs when bacteria or viruses infect the small space behind the eardrum, known as the middle ear, a condition medically referred to as otitis media. Understanding the causes, symptoms, and treatment options for ear infections is essential for parents and adults to recognize when professional medical attention is needed and how to manage symptoms effectively at home.
What Is an Ear Infection?
An ear infection develops when bacteria or viruses infect the middle ear, the small chamber located just behind the eardrum. This space is normally filled with air and contains three tiny bones (the ossicles) that transmit sound vibrations to help us hear. The middle ear is connected to the back of the nose and throat through a narrow passageway called the eustachian tube, which plays a critical role in maintaining normal ear function.
When the eustachian tube becomes blocked, usually due to a cold, allergies, or other upper respiratory conditions, fluid can accumulate in the middle ear. This fluid buildup creates an ideal environment for bacteria and viruses to multiply, leading to infection and inflammation. The infection causes pressure to build up against the eardrum, resulting in pain and hearing difficulties.
Acute ear infections typically develop suddenly and are painful, while chronic ear infections last for extended periods or come and go repeatedly. Most acute middle ear infections resolve within two to three days, though some may persist longer.
Why Are Ear Infections Common in Children?
Ear infections are significantly more common in children than in adults, with most children experiencing at least one ear infection by age three. This higher prevalence in the pediatric population is due to several anatomical and developmental factors:
- The eustachian tube in infants and toddlers is narrower and shorter than in adults, making it easier for germs from the upper throat to spread to the middle ear.
- The immune system in young children is still developing, making them more susceptible to infections.
- Children have more frequent exposure to viruses and bacteria through daily contact with peers in schools and childcare settings.
- After age seven, ear infections become less common as the eustachian tube and immune system mature and develop.
Causes and Risk Factors
Acute middle ear infections typically develop as a secondary infection following a cold, flu, sore throat, or similar respiratory illness. When viruses or bacteria infect the throat, the mucous membranes become inflamed and produce excess fluid. This inflammation extends to the eustachian tube and the membranes lining the middle ear, causing them to swell and preventing proper fluid drainage.
Common Triggers for Ear Infections
Several specific situations and conditions increase the likelihood of developing an ear infection:
- Cold, flu, or allergy symptoms: These conditions cause congestion and inflammation that block the eustachian tube, allowing fluid to accumulate in the middle ear.
- Exposure to germs: Daily contact with infectious agents in childcare centers, schools, and other group settings increases the risk of respiratory infections that lead to ear infections.
- Bottle feeding position: Infants who drink from a bottle while lying down, especially during naps or overnight, have an increased risk of ear infections.
- Adenoid enlargement: Enlarged adenoids (lymph tissue in the upper throat) can block the eustachian tube, increasing infection risk.
- Allergies: Allergic reactions cause inflammation and swelling of the eustachian tube.
- Sinus infections: Infections of the sinuses can lead to eustachian tube swelling and middle ear inflammation.
- Tobacco smoke exposure: Environmental smoke irritates the respiratory tract and increases infection risk.
- Excess mucus production: Teething can produce excess saliva and mucus that contributes to fluid buildup.
Symptoms of Ear Infections
Ear infection symptoms vary depending on the severity of the infection and the age of the patient. In young children, recognizing ear infection symptoms can be challenging because they cannot always clearly communicate where they hurt.
Common Symptoms in Children
Children with acute middle ear infections typically experience:
- Severe earache and ear pain
- Fever over 100.4°F (38°C)
- Poor hearing and difficulty understanding speech
- Sleep disturbances and difficulty sleeping through the night
- Excessive crying and irritability
- General weakness and feeling unwell
- Vomiting or nausea
- Diarrhea
- Loss of appetite
- Head shaking and ear rubbing (nonverbal signs of ear pain)
Young children who cannot localize pain may complain of a stomach ache when the actual problem is an ear infection, making diagnosis more difficult for parents.
Symptoms in Older Children and Adults
Older children and adults with ear infections typically report:
- Ear pain and fullness in the affected ear
- Hearing loss in the affected ear
- Nasal congestion and cough
- Lethargy and fatigue
- Fluid drainage from the ear (indicating possible eardrum rupture)
An important warning sign is sudden drainage of yellow or green fluid from the ear, which may indicate that the eardrum has ruptured.
Diagnosis of Ear Infections
Healthcare providers diagnose ear infections through a combination of medical history, symptom assessment, and physical examination. During an examination, the provider uses an otoscope, a lighted instrument that allows visualization of the inner ear.
The otoscopic examination may reveal:
- Areas of marked redness inside the ear canal or on the eardrum
- Bulging of the tympanic membrane (eardrum), indicating fluid pressure behind it
- Discharge or drainage from the ear
- Air bubbles or visible fluid level behind the eardrum
- A perforation or hole in the eardrum
Diagnosis can sometimes be difficult, and providers may recommend additional hearing tests if a child has a history of recurrent ear infections.
Treatment Options
Most acute middle ear infections resolve on their own within two to three days without requiring antibiotics. The primary focus of treatment is symptom relief and comfort care while the body’s immune system fights the infection.
Pain Management and Home Care
The main treatment approach for acute ear infections involves providing pain relief and comfort:
- Painkillers: Over-the-counter pain relievers such as acetaminophen or ibuprofen can reduce ear pain and fever. Always follow age-appropriate dosing guidelines.
- Warm compress: Applying a warm (not hot) compress to the affected ear can provide comfort.
- Rest: Adequate rest and sleep support the immune system in fighting the infection.
- Elevation: Keeping the head elevated while sleeping can reduce ear discomfort.
- Avoiding irritants: Keep secondhand smoke and other respiratory irritants away from the child.
Antibiotic Use
Antibiotics are not routinely prescribed for all ear infections because most are caused by viruses, which do not respond to antibiotic treatment. However, antibiotics are recommended in specific situations:
- All children younger than six months with an ear infection receive antibiotic treatment.
- Children with severe symptoms or those who show no improvement after 48 to 72 hours may require antibiotics.
- Patients with signs of complications may need antibiotic therapy.
If symptoms persist or worsen beyond the typical recovery period, parents should schedule an appointment with their healthcare provider to determine whether antibiotics are necessary.
Potential Complications
While most ear infections resolve without complications, several serious conditions can develop if the infection spreads or persists:
- Ruptured eardrum: If fluid pressure behind the eardrum becomes too great, the eardrum can tear or perforate. Thick, sticky fluid mixed with pus and blood may drain into the ear canal, and pain may temporarily improve. Most small perforations heal on their own within days or weeks.
- Chronic otitis media: If infection continues for several weeks, the condition becomes chronic. While the acute pain and fever subside, fluid remains in the middle ear and may continue draining, potentially causing permanent hearing loss.
- Mastoiditis: Bacterial infection can spread to the mastoid bone behind the ear, causing pain, swelling, and fever. This condition requires antibiotic treatment to prevent further complications.
- Meningitis: In rare cases, infection can spread to the membranes covering the brain and spinal cord.
- Inner ear damage: Persistent infections can damage the inner ear nerves, potentially leading to permanent hearing loss.
- Brain abscess: Pus collection in or around the brain is a rare but serious complication.
Hearing Loss and Long-Term Effects
Most children experience temporary hearing loss during and immediately after an ear infection due to fluid accumulation in the middle ear. This fluid may persist for weeks or even months after the infection has cleared, but hearing typically returns to normal.
Speech and language delay is uncommon and usually only occurs in children who experience lasting hearing loss from multiple recurrent ear infections. However, parents should monitor their child’s hearing and discuss concerns with their healthcare provider during follow-up visits.
Prevention Strategies
While not all ear infections can be prevented, several strategies can reduce the risk:
- Vaccination: Keeping children current with pneumococcal and influenza vaccines reduces the risk of infections that lead to ear infections.
- Proper bottle feeding: Hold infants upright while bottle feeding and avoid propping bottles during naps or overnight.
- Smoke avoidance: Protect children from secondhand smoke exposure.
- Hygiene practices: Encourage frequent handwashing and minimize exposure to children with respiratory infections when possible.
- Allergy management: Address allergies promptly to prevent eustachian tube swelling.
- Breastfeeding: When possible, breastfeeding provides immune protection against infections.
When to Seek Medical Care
Parents should contact a healthcare provider if their child:
- Has severe ear pain that does not improve with pain medication
- Develops a high fever (over 102°F or 39°C)
- Shows signs of spreading infection, such as swelling behind the ear or stiff neck
- Has drainage of pus or blood from the ear
- Experiences symptoms lasting longer than three days without improvement
- Has recurrent ear infections (three or more within six months)
- Shows signs of hearing loss
Prognosis and Recovery
The outlook for most ear infections is excellent. With appropriate symptom management and comfort care, the majority of acute middle ear infections resolve completely without lasting effects. However, recurrent ear infections may occur in the future, and some children experience multiple infections throughout childhood.
Frequently Asked Questions (FAQs)
Q: How long does an ear infection last?
A: Most acute ear infections resolve within two to three days. However, fluid may remain in the middle ear for weeks or months after the infection clears.
Q: Do all ear infections need antibiotics?
A: No, most ear infections are caused by viruses and do not respond to antibiotics. Antibiotics are typically reserved for children under six months old or those with severe symptoms that don’t improve within 48 to 72 hours.
Q: Can ear infections cause permanent hearing loss?
A: Temporary hearing loss during infection is common, but permanent loss is rare and typically only occurs with chronic, recurrent infections left untreated.
Q: Are ear infections contagious?
A: Ear infections themselves are not contagious, but the respiratory infections that cause them (colds, flu) can be spread to others.
Q: What can I do at home to help my child?
A: Provide pain relief with age-appropriate medications, apply warm compresses, ensure adequate rest, maintain proper hydration, and monitor for signs of worsening symptoms or complications.
Q: When should I see a doctor for an ear infection?
A: Seek medical care if your child has severe pain, high fever, signs of spreading infection, drainage from the ear, symptoms lasting more than three days, or recurrent infections.
References
- Ear Infection Information — American Academy of Pediatrics (Healthy Children). Accessed January 2026. https://www.healthychildren.org/English/health-issues/conditions/ear-nose-throat/Pages/Ear-Infection-Information.aspx
- Overview: Middle Ear Infection — NCBI Bookshelf (InformedHealth.org). Published by the National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK279381/
- Ear Infection – Acute — MedlinePlus Medical Encyclopedia, U.S. National Library of Medicine. https://medlineplus.gov/ency/article/000638.htm
Read full bio of Sneha Tete











