Ear Infection Symptoms: 6 Key Signs To Spot Early
Recognize ear infection symptoms early in adults and children to seek timely treatment and prevent complications.
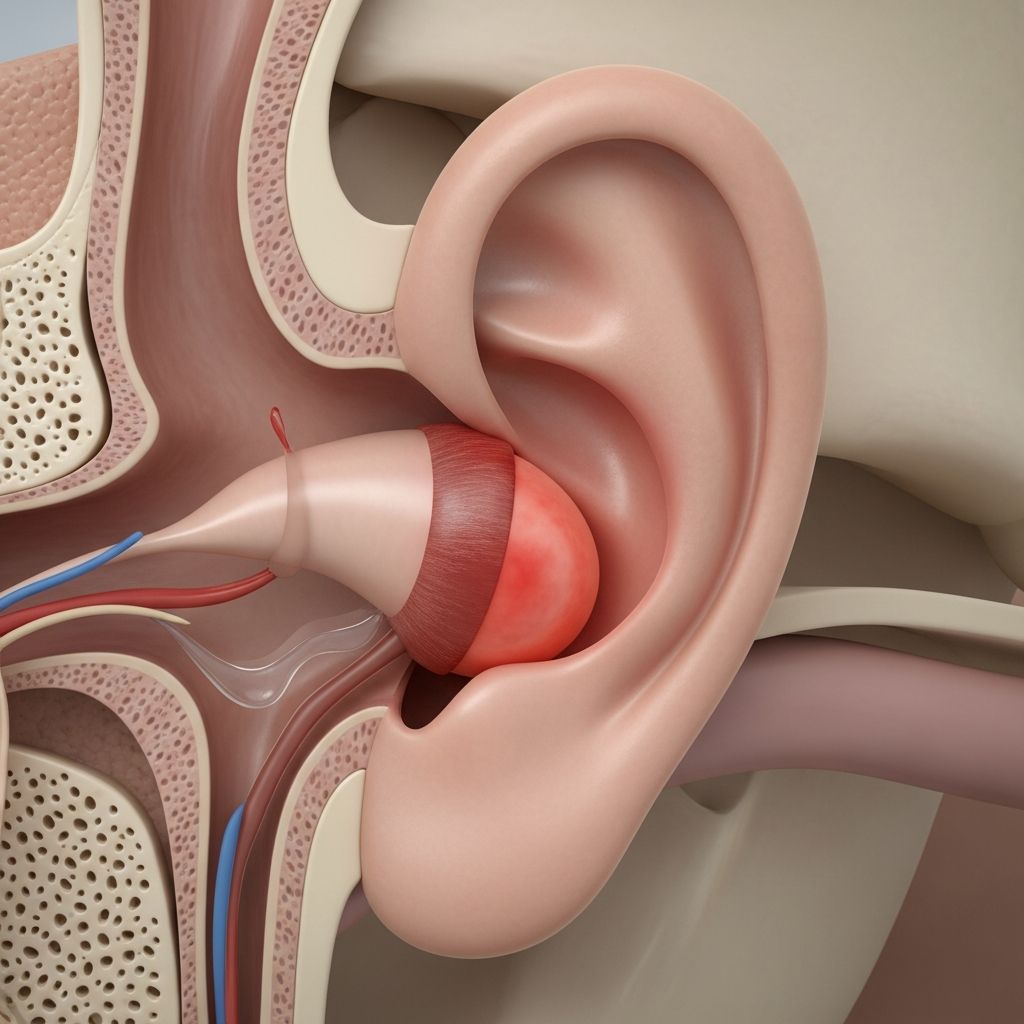
Ear Infection Symptoms
Ear infections, medically known as otitis, are common conditions affecting the ear’s structures and causing discomfort, pain, and potential complications if untreated. They primarily impact children but can occur in adults too, often following colds or respiratory issues. Recognizing
ear infection symptoms
early is crucial for prompt treatment and preventing issues like hearing loss or chronic infections.What Is an Ear Infection?
An ear infection involves inflammation and fluid buildup in the ear, typically due to bacterial or viral pathogens entering after a blockage in the Eustachian tube, which connects the middle ear to the throat. Acute infections develop quickly and are painful, while chronic ones persist or recur. The middle ear, behind the eardrum, is most commonly affected in otitis media, the prevalent type.
In children, shorter and more horizontal Eustachian tubes make them prone to fluid trapping, especially during colds, allergies, or teething. Adults experience them less frequently but may suffer from similar triggers like sinus infections or smoke exposure. According to the National Institute on Deafness and Other Communication Disorders (NIDCD), ear infections are a leading reason for pediatric doctor visits.
Types of Ear Infections
Ear infections are categorized by the affected area: outer, middle, or inner ear. Each type presents distinct
symptoms
and causes.- Outer Ear Infection (Otitis Externa): Affects the ear canal, often from irritation like water exposure (swimmer’s ear), eczema, or bacteria/fungi. Symptoms include itching, redness, and pain when touching the ear.
- Middle Ear Infection (Otitis Media): The most common, involving swelling and fluid behind the eardrum. Subtypes include acute otitis media (AOM) with pain and fever, otitis media with effusion (OME) with persistent fluid sans infection, and chronic otitis media with effusion (COME).
- Inner Ear Infection: Impacts the labyrinth or vestibular system, leading to labyrinthitis. Often viral, it causes dizziness, vertigo, and balance issues alongside hearing problems.
Understanding these distinctions aids in identifying the right treatment approach.
Symptoms of an Ear Infection
**Ear infection symptoms** vary by age, type, and severity but typically onset rapidly. Common signs include:
- Ear pain (earache): Sharp or throbbing, worsening when lying down.
- Fever or high temperature: Especially in young children.
- Hearing difficulties: Muffled sounds or temporary loss due to fluid.
- Ear discharge: Clear, pus-like, or bloody fluid if the eardrum ruptures.
- Feeling of fullness or pressure: In the affected ear.
- Itching and irritation: Common in outer ear infections.
In
adults
, additional symptoms may involve nasal congestion, cough, lethargy, vomiting, diarrhea, or loss of appetite.Symptoms in Children and Babies
Infants and toddlers can’t verbalize pain, so watch for nonverbal cues:
- Rubbing or pulling at the ear
- Irritability, restlessness, or fussiness
- Trouble sleeping or responding to sounds
- Fever, clumsiness, or balance problems
- Loss of appetite or fluid drainage
- Not reacting to quiet sounds
These signs often follow a cold, with fluid buildup causing pressure. Tugging the ear isn’t definitive but common.
Causes and Risk Factors
Ear infections stem from Eustachian tube dysfunction, preventing drainage and allowing bacteria or viruses to thrive. Primary causes include:
| Cause | Description |
|---|---|
| Colds/Upper Respiratory Infections | Viral illnesses like flu lead to secondary bacterial invasion |
| Allergies/Sinus Issues | Swelling blocks the tube |
| Teething | Excess mucus and saliva |
| Adenoid Problems | Infected or enlarged tissue |
| Tobacco Smoke | Irritates and inflames airways |
Risk factors heighten susceptibility: young age (under 3), daycare attendance, bottle-feeding while lying down, or seasonal allergies. Genetic predisposition or pacifier use also contributes.
Diagnosis of Ear Infections
Diagnosis begins with a medical history review, focusing on recent illnesses or symptoms. Providers use an
otoscope
—a lighted instrument—to examine the ear canal and eardrum for:- Redness or bulging eardrum
- Fluid, air bubbles, or discharge
- Perforation (hole) in the eardrum
Some otoscopes puff air to test eardrum mobility, indicating blockages. Tympanometry measures middle ear pressure, while hearing tests assess impacts from recurrent infections. Home fluid monitors exist but require professional confirmation.
Treatment Options
Many ear infections resolve within 3 days to a week without intervention, but symptom management is key.
- Pain Relief: Over-the-counter acetaminophen or ibuprofen for fever and pain. Avoid aspirin in children due to Reye’s syndrome risk.
- Antibiotics: Prescribed for bacterial cases (e.g., amoxicillin for 7-10 days) if severe or persistent.
- Eardrops: For outer infections or pain.
- Warm Compress: Soothes earache.
For chronic cases or effusions, options include ear tube insertion to drain fluid and restore hearing. Watchful waiting is common for mild AOM in children over 6 months.
When to See a Doctor
Seek immediate care if:
- Symptoms worsen or persist beyond 3 days
- High fever (>102°F in children under 2), severe pain, or swelling
- Discharge, dizziness, vomiting, or hearing changes
- Infant under 6 months has fever
- Sudden pain relief (possible rupture) or neurological signs like facial twitching
Early intervention prevents complications like mastoiditis, meningitis, or permanent hearing loss.
Complications and Prognosis
Most infections heal fully, but fluid may linger weeks, causing temporary hearing issues. Rare complications include eardrum tears, chronic otitis media, or spread to nearby structures like the brain (abscess/meningitis). Recurrent infections risk speech delays in children. Prognosis is excellent with treatment; prevention via vaccinations (pneumococcal, flu) and avoiding smoke helps.
Prevention Tips
Reduce risk by:
- Breastfeeding infants
- Avoiding secondhand smoke
- Limiting pacifier use
- Ensuring up-to-date vaccinations
- Practicing hand hygiene during cold season
- Drying ears after swimming
Frequently Asked Questions (FAQs)
What are the first signs of an ear infection?
Initial signs include ear pain, fever, tugging at the ear in children, and hearing difficulties.
How long do ear infection symptoms last?
Most clear in 3 days, up to a week; seek care if longer.
Can adults get ear infections?
Yes, though less common, often from colds or allergies.
Do ear infections go away on their own?
Many do, but antibiotics may be needed for bacterial cases.
Is ear tugging always an ear infection sign?
No, but common in infants; confirm with a doctor.
This comprehensive guide equips you to identify and manage ear infections effectively, promoting better ear health.
References
- Ear infections – NHS — NHS. 2023-10-12. https://www.nhs.uk/conditions/ear-infections/
- Ear infection – acute: MedlinePlus Medical Encyclopedia — MedlinePlus. 2024-05-01. https://medlineplus.gov/ency/article/000638.htm
- Ear Infections in Children, Babies & Toddlers | NIDCD — National Institute on Deafness and Other Communication Disorders, NIH. 2023-11-15. https://www.nidcd.nih.gov/health/ear-infections-children
Read full bio of Sneha Tete











